Thrombosis: Symptoms, Causes, Prevention and Treatment


Escrito y verificado por el biólogo Samuel Antonio Sánchez Amador
Thrombosis is the formation of a clot within a blood vessel. This medical condition is one of the main causes of myocardial infarction, which is why acute venous and arterial thromboses are considered the most common cause of death in high-income countries.
For example, ischemic heart disease is the leading cause of death in these regions – one in every four deaths worldwide and, in the United States, it causes more deaths than lung cancer, AIDS, and traffic accidents combined (about 300,000 deaths annually). Certainly the numbers make us sit up and take notice.
However, it should be noted that not all people have the same risk. For example, the prevalence of deep vein thrombosis (DVT) ranges from one case in every 10,000 young adults to 1 in every 1,000 older adults, depending on the population sector analyzed and socioeconomic status. If you want to know more about this condition, keep reading.
What is a thrombosis?
According to the Navarra University Clinic (CUN), thrombosis is an abnormal vascular situation in which a thrombus develops inside a blood vessel. This can happen in both veins and arteries and prevents proper blood flow to the different structures of the body, which results in sequelae and/or the death of the patient.
The ability of blood to flow properly in the body depends on a complex homeostatic relationship. In it, the blood bodies (leukocytes, erythrocytes and platelets), plasma proteins, coagulation factors, inflammatory factors and the nature of the endothelium, the inner cellular face of the duct, play essential roles.
Our body contains about 5 liters of blood. The heart pumps almost everything in a matter of a minute.
A matter of pressure
From here, a series of complex terms come into play that we must describe briefly. Osmolarity corresponds to the number of particles per liter of a given solution, measured in moles/liter (osm/l). Osmorality is similar, and it represents the concentration of solutes in a solution, in osmoles per kilogram.
In the internal fluids of the body, osmolality and osmolarity are practically interchangeable. As indicated by the Foundation for Health Training and Research of the Region of Murcia (FFIS), plasma osmolarity values can be calculated using the following formula:
OSMp = 2 [Na +] + [glucose] + [urea]
Normal = 290 ± 10 mOsm/kg H2O
Here the most common solutes in blood plasma are taken into account, which are sodium (Na), glucose, and urea. Normal values when applying this formula are 282 +/- 4 mosm/kilogram. This data is very interesting on its own, but it’s also essential to know what the normal situation is in the plasma of a healthy person.
Osmolarity and osmolality aren’t directly linked to other processes such as blood pressure, but they do condition them. The force exerted by blood on the artery walls as it’s pumped depends on many factors, including the concentration of solutes within the plasma and thus osmolality/osmolality (OSMp).
Epidemiology

The epidemiology of thrombosis depends on whether it’s venous or arterial, whether or not it has been caused by previous factors, and whether it’s the first episode or has already occurred in other cases. Based on these parameters, here are some figures of interest regarding thrombosis in the world:
- Venous thromboembolism (VTE) includes deep vein thrombosis (DVT) and pulmonary embolism (PE). Its incidence is 1 in every 100,000 children, 1 in every 10,000 adults of reproductive age, 1 in every 1,000 retired adults, and 1 in every 100 elderly people. With age, the risk increases.
- The incidence of a pulmonary embolism is 29 to 48 patients per 100,000 people per year. 6% of them may die, a value that increases to 30% if there is hemodynamic instability.
- Arterial thrombosis is estimated to be less common than venous thrombosis, especially in females. However, the risk increases exponentially with age as well.
The types of thrombosis
Once we have established the basis of what a thrombosis is and what the normal blood values are in a patient, we’re ready to dissect the types of thrombosis. These can be differentiated according to their location, degree of occlusion, and severity. Go for it.
According to your location
In this category, we differentiate thrombosis by precipitation, hyaline or by coagulation. Precipitation thrombosis, also known as “white thrombi”, is characterized by the appearance of a platelet thrombus. Platelets break off and adhere to collagen, releasing substances that promote the adherence of new platelets.
The precipitation variant is typical of the arteries and the heart. On the other hand, hyaline thrombosis is also produced by the detachment of fibrin and platelets, but, in this case, in venules or capillaries. Ultimately, clotting thromboses (red thrombi) occur in the veins, and this is the most common of all.
According to the degree of occlusion
Depending on how much blood flow is stopped in the affected structure, a thrombosis can be occluding or mural. In the occluding variant, the vessel is completely plugged, whereas in a mural thrombosis, the result is a partial obstruction.
There are many more types of thrombosis depending on the site of involvement: jugular, renal, portal, cerebral, cavernous sinus, and more.
Pathophysiology and causes of thrombosis
As indicated by the Stat Pearls medical portal, thrombosis is a clinical condition of multifactorial etiology. As previously mentioned, this condition occurs when there’s an endogenous imbalance in the body’s coagulation mechanism, which is also accompanied by a blood homeostatic imbalance (osmolarity and other things).
Historically, three common factors have been associated with the appearance of a thrombus, known as Virchow’s triad, named after the German pathologist who described them. They are as follows:
- Damage to the endothelial cells that line the blood vessels on the inside: This can happen due to the wrong insertion of a catheter, a direct injury, or a surgical procedure, among other things.
- Hypercoagulable state: Conditions that increase the risk of excessive and/or inappropriate clot formation in the patient’s blood.
- Venous or arterial stasis: Slow venous or arterial blood circulation. This is common, especially in the deep veins of the legs. This specific case is called deep vein thrombosis (DVT).
Hypercoagulability is intrinsic to thrombosis, as this concept describes a set of clinical entities that promote a thrombogenic state, due to the accumulation of prothrombotic compounds in the blood.
This alteration in the clotting rhythm may be due to the presence of inflammatory factors, a high blood viscosity, a higher amount of cytokines, an increase in prothrombin in the blood, or deficiencies in endogenous anticoagulant factors, among others.
This condition can be inherited or acquired, with antithrombin III deficiency being the most famous congenital variant.
The importance of acquired hypercoagulability
As the Medigraphic portal indicates, a clot and a thrombus are formed in the same way. A clot is a homeostatic response of very high biological value (it prevents the death of the individual due to hemorrhage after an injury), while thrombosis is considered pathological in all cases.
This fatal medical condition is almost always caused by acquired hypercoagulability, since inherited variants are very rare in the general population. This can be the result of the action of certain medications, acute inflammatory events (pregnancies, injuries or surgeries), infections and chronic inflammatory pathologies.
We understand chronic inflammatory diseases as morbid obesity, ulcerative colitis, extreme smoking and serious rheumatological diseases.
However, it should be noted that the initiation mechanism is different for arterial and venous thrombosis. In the first case, the trigger is atherosclerosis, accumulation of fat, cholesterol and other substances in and on the walls of the arteries. On the other hand, venous thrombosis usually begins with damage to the endothelium that covers it.
Treatment of thrombosis
As the scientific article Triggers, targets and treatments for thrombosis indicates, a venous thrombosis requires a very different treatment to an arterial one. Based on this premise, we carry out the medical approaches separately.
Arterial thrombosis
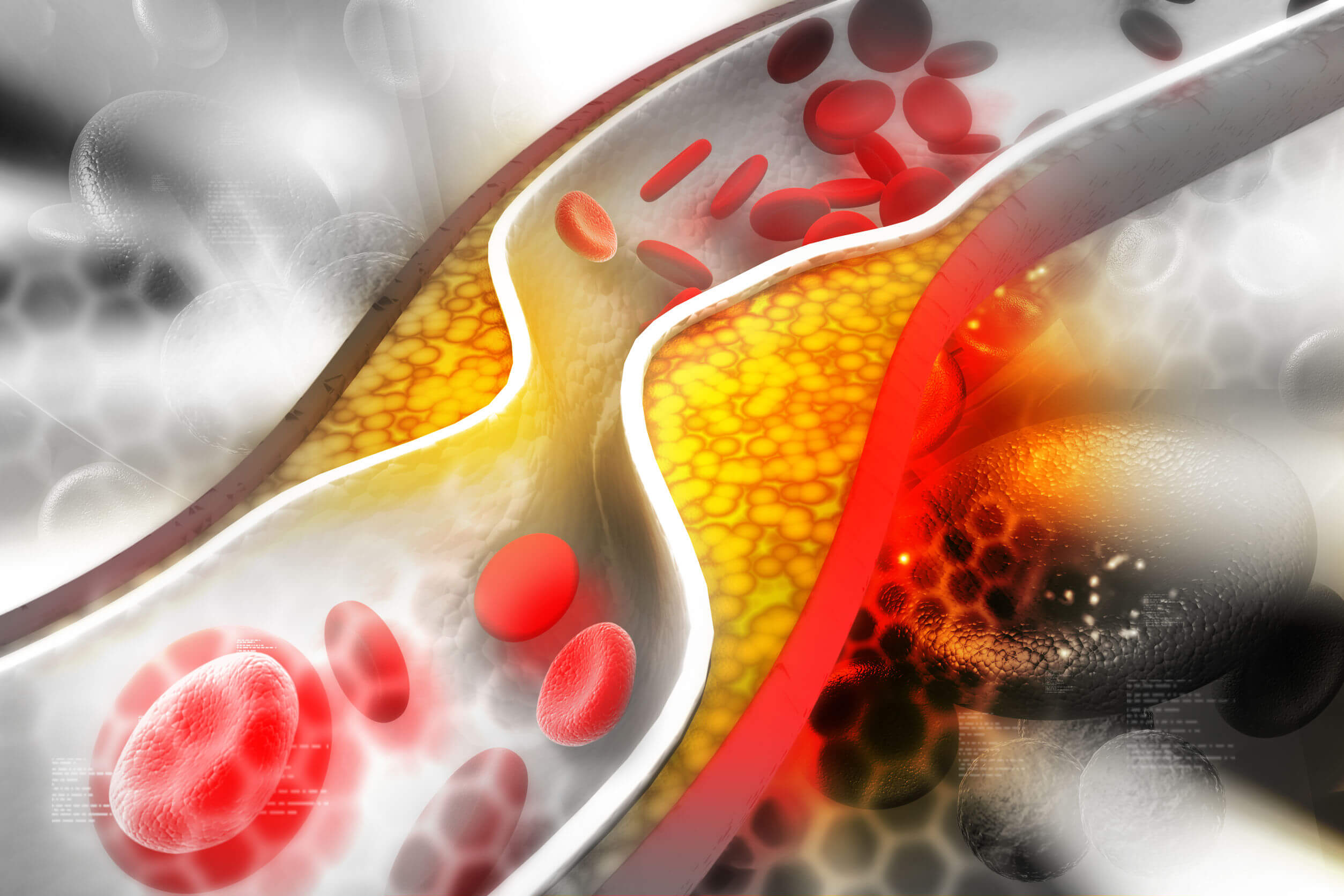
The primary trigger for arterial thrombosis is the rupture of an atherosclerotic plaque. When lipids accumulate in the wall of an artery, it favors the rupture of the modified endothelium, which causes the transport and action of platelets to the affected place. Platelet growth in the lesion promotes thrombus formation.
To avoid this situation and to manage an acute condition, the use of antiplatelet drugs is used. As indicated by the United States National Library of Medicine, P2Y12 inhibitors are prescribed to patients with peripheral arterial disease (PAD) to prevent thrombosis and thus potential death.
There are also other drugs, such as integrin inhibitors, protease inhibitors (PAR1), and others.
Venous thrombosis
Deep vein thrombosis (DVT) and pulmonary embolism (PE) are the third leading cause of death worldwide associated with a cardiovascular event, only surpassed by myocardial infarction and cerebrovascular accident (CVA). Arterial thrombi are rich in platelets (white), while venous thrombi have trapped red blood cells (red).
Venous thromboses occur as a result of changes in the blood, such as variations in the thickness of the plasma or damage to the endothelium that lines the veins. In this case, the first-line drugs are anticoagulants, more specifically enoxaparin (Lovenox) and fondaparinux (Arixtra), as indicated by the Mayo Clinic.
Beyond this, you can also resort to thrombolytics (clot solvents), a filter in the vena cava (if other treatments are impossible, to avoid the migration of the thrombus to the lung) or compression stockings, which prevent blood clotting in the affected area.
Prevention and risks
As indicated by the Trombo.info portal, in half of the cases of deep vein thrombosis and pulmonary embolism, the cause that led to them is unknown. In any case, medical-scientific advances have managed to elucidate certain risk factors for its appearance, among we find the following:
- Surgery or trauma: As we’ve said, damage to the venous endothelium causes a thrombus to occur.
- Prolonged rest: People who are immobile for a long time are more prone to thrombosis. Not only that, but they’re also much more susceptible to ulcers.
- Hormonal treatment: Some oral contraceptives have been associated with the risk of venous thrombosis.
- Genetic predisposition: Some coagulopathies are genetic, while others are acquired.
Despite the fact that in many cases knowing the origin of a thrombus is impossible, we have said that chronic inflammatory conditions, such as morbid obesity, smoking, and alcoholism can promote its appearance. Obesity leads to stagnation or stasis in the venous flow, which greatly favors the formation of clots.
For all these reasons, what we can recommend most of all to every reader is that they lead a healthy, active lifestyle. It’s very unlikely for a young person to suffer a thrombus if they take care of themselves, but, unfortunately, in old age, this medical condition is very common (1 in 100 inhabitants). The only thing we can do is to try to look after ourselves as much as possible.
Thrombosis is the formation of a clot within a blood vessel. This medical condition is one of the main causes of myocardial infarction, which is why acute venous and arterial thromboses are considered the most common cause of death in high-income countries.
For example, ischemic heart disease is the leading cause of death in these regions – one in every four deaths worldwide and, in the United States, it causes more deaths than lung cancer, AIDS, and traffic accidents combined (about 300,000 deaths annually). Certainly the numbers make us sit up and take notice.
However, it should be noted that not all people have the same risk. For example, the prevalence of deep vein thrombosis (DVT) ranges from one case in every 10,000 young adults to 1 in every 1,000 older adults, depending on the population sector analyzed and socioeconomic status. If you want to know more about this condition, keep reading.
What is a thrombosis?
According to the Navarra University Clinic (CUN), thrombosis is an abnormal vascular situation in which a thrombus develops inside a blood vessel. This can happen in both veins and arteries and prevents proper blood flow to the different structures of the body, which results in sequelae and/or the death of the patient.
The ability of blood to flow properly in the body depends on a complex homeostatic relationship. In it, the blood bodies (leukocytes, erythrocytes and platelets), plasma proteins, coagulation factors, inflammatory factors and the nature of the endothelium, the inner cellular face of the duct, play essential roles.
Our body contains about 5 liters of blood. The heart pumps almost everything in a matter of a minute.
A matter of pressure
From here, a series of complex terms come into play that we must describe briefly. Osmolarity corresponds to the number of particles per liter of a given solution, measured in moles/liter (osm/l). Osmorality is similar, and it represents the concentration of solutes in a solution, in osmoles per kilogram.
In the internal fluids of the body, osmolality and osmolarity are practically interchangeable. As indicated by the Foundation for Health Training and Research of the Region of Murcia (FFIS), plasma osmolarity values can be calculated using the following formula:
OSMp = 2 [Na +] + [glucose] + [urea]
Normal = 290 ± 10 mOsm/kg H2O
Here the most common solutes in blood plasma are taken into account, which are sodium (Na), glucose, and urea. Normal values when applying this formula are 282 +/- 4 mosm/kilogram. This data is very interesting on its own, but it’s also essential to know what the normal situation is in the plasma of a healthy person.
Osmolarity and osmolality aren’t directly linked to other processes such as blood pressure, but they do condition them. The force exerted by blood on the artery walls as it’s pumped depends on many factors, including the concentration of solutes within the plasma and thus osmolality/osmolality (OSMp).
Epidemiology

The epidemiology of thrombosis depends on whether it’s venous or arterial, whether or not it has been caused by previous factors, and whether it’s the first episode or has already occurred in other cases. Based on these parameters, here are some figures of interest regarding thrombosis in the world:
- Venous thromboembolism (VTE) includes deep vein thrombosis (DVT) and pulmonary embolism (PE). Its incidence is 1 in every 100,000 children, 1 in every 10,000 adults of reproductive age, 1 in every 1,000 retired adults, and 1 in every 100 elderly people. With age, the risk increases.
- The incidence of a pulmonary embolism is 29 to 48 patients per 100,000 people per year. 6% of them may die, a value that increases to 30% if there is hemodynamic instability.
- Arterial thrombosis is estimated to be less common than venous thrombosis, especially in females. However, the risk increases exponentially with age as well.
The types of thrombosis
Once we have established the basis of what a thrombosis is and what the normal blood values are in a patient, we’re ready to dissect the types of thrombosis. These can be differentiated according to their location, degree of occlusion, and severity. Go for it.
According to your location
In this category, we differentiate thrombosis by precipitation, hyaline or by coagulation. Precipitation thrombosis, also known as “white thrombi”, is characterized by the appearance of a platelet thrombus. Platelets break off and adhere to collagen, releasing substances that promote the adherence of new platelets.
The precipitation variant is typical of the arteries and the heart. On the other hand, hyaline thrombosis is also produced by the detachment of fibrin and platelets, but, in this case, in venules or capillaries. Ultimately, clotting thromboses (red thrombi) occur in the veins, and this is the most common of all.
According to the degree of occlusion
Depending on how much blood flow is stopped in the affected structure, a thrombosis can be occluding or mural. In the occluding variant, the vessel is completely plugged, whereas in a mural thrombosis, the result is a partial obstruction.
There are many more types of thrombosis depending on the site of involvement: jugular, renal, portal, cerebral, cavernous sinus, and more.
Pathophysiology and causes of thrombosis
As indicated by the Stat Pearls medical portal, thrombosis is a clinical condition of multifactorial etiology. As previously mentioned, this condition occurs when there’s an endogenous imbalance in the body’s coagulation mechanism, which is also accompanied by a blood homeostatic imbalance (osmolarity and other things).
Historically, three common factors have been associated with the appearance of a thrombus, known as Virchow’s triad, named after the German pathologist who described them. They are as follows:
- Damage to the endothelial cells that line the blood vessels on the inside: This can happen due to the wrong insertion of a catheter, a direct injury, or a surgical procedure, among other things.
- Hypercoagulable state: Conditions that increase the risk of excessive and/or inappropriate clot formation in the patient’s blood.
- Venous or arterial stasis: Slow venous or arterial blood circulation. This is common, especially in the deep veins of the legs. This specific case is called deep vein thrombosis (DVT).
Hypercoagulability is intrinsic to thrombosis, as this concept describes a set of clinical entities that promote a thrombogenic state, due to the accumulation of prothrombotic compounds in the blood.
This alteration in the clotting rhythm may be due to the presence of inflammatory factors, a high blood viscosity, a higher amount of cytokines, an increase in prothrombin in the blood, or deficiencies in endogenous anticoagulant factors, among others.
This condition can be inherited or acquired, with antithrombin III deficiency being the most famous congenital variant.
The importance of acquired hypercoagulability
As the Medigraphic portal indicates, a clot and a thrombus are formed in the same way. A clot is a homeostatic response of very high biological value (it prevents the death of the individual due to hemorrhage after an injury), while thrombosis is considered pathological in all cases.
This fatal medical condition is almost always caused by acquired hypercoagulability, since inherited variants are very rare in the general population. This can be the result of the action of certain medications, acute inflammatory events (pregnancies, injuries or surgeries), infections and chronic inflammatory pathologies.
We understand chronic inflammatory diseases as morbid obesity, ulcerative colitis, extreme smoking and serious rheumatological diseases.
However, it should be noted that the initiation mechanism is different for arterial and venous thrombosis. In the first case, the trigger is atherosclerosis, accumulation of fat, cholesterol and other substances in and on the walls of the arteries. On the other hand, venous thrombosis usually begins with damage to the endothelium that covers it.
Treatment of thrombosis
As the scientific article Triggers, targets and treatments for thrombosis indicates, a venous thrombosis requires a very different treatment to an arterial one. Based on this premise, we carry out the medical approaches separately.
Arterial thrombosis

The primary trigger for arterial thrombosis is the rupture of an atherosclerotic plaque. When lipids accumulate in the wall of an artery, it favors the rupture of the modified endothelium, which causes the transport and action of platelets to the affected place. Platelet growth in the lesion promotes thrombus formation.
To avoid this situation and to manage an acute condition, the use of antiplatelet drugs is used. As indicated by the United States National Library of Medicine, P2Y12 inhibitors are prescribed to patients with peripheral arterial disease (PAD) to prevent thrombosis and thus potential death.
There are also other drugs, such as integrin inhibitors, protease inhibitors (PAR1), and others.
Venous thrombosis
Deep vein thrombosis (DVT) and pulmonary embolism (PE) are the third leading cause of death worldwide associated with a cardiovascular event, only surpassed by myocardial infarction and cerebrovascular accident (CVA). Arterial thrombi are rich in platelets (white), while venous thrombi have trapped red blood cells (red).
Venous thromboses occur as a result of changes in the blood, such as variations in the thickness of the plasma or damage to the endothelium that lines the veins. In this case, the first-line drugs are anticoagulants, more specifically enoxaparin (Lovenox) and fondaparinux (Arixtra), as indicated by the Mayo Clinic.
Beyond this, you can also resort to thrombolytics (clot solvents), a filter in the vena cava (if other treatments are impossible, to avoid the migration of the thrombus to the lung) or compression stockings, which prevent blood clotting in the affected area.
Prevention and risks
As indicated by the Trombo.info portal, in half of the cases of deep vein thrombosis and pulmonary embolism, the cause that led to them is unknown. In any case, medical-scientific advances have managed to elucidate certain risk factors for its appearance, among we find the following:
- Surgery or trauma: As we’ve said, damage to the venous endothelium causes a thrombus to occur.
- Prolonged rest: People who are immobile for a long time are more prone to thrombosis. Not only that, but they’re also much more susceptible to ulcers.
- Hormonal treatment: Some oral contraceptives have been associated with the risk of venous thrombosis.
- Genetic predisposition: Some coagulopathies are genetic, while others are acquired.
Despite the fact that in many cases knowing the origin of a thrombus is impossible, we have said that chronic inflammatory conditions, such as morbid obesity, smoking, and alcoholism can promote its appearance. Obesity leads to stagnation or stasis in the venous flow, which greatly favors the formation of clots.
For all these reasons, what we can recommend most of all to every reader is that they lead a healthy, active lifestyle. It’s very unlikely for a young person to suffer a thrombus if they take care of themselves, but, unfortunately, in old age, this medical condition is very common (1 in 100 inhabitants). The only thing we can do is to try to look after ourselves as much as possible.
- Trombosis, CUN. Recogido a 8 de abril en https://www.cun.es/diccionario-medico/terminos/trombosis
- Principios básicos de la ósmosis y la presión oncótica. Recogido a 8 de abril en http://www.ffis.es/volviendoalobasico/2principios_bsicos_de_la_smosis_y_la_presin_onctica_clculo_de_la_osmolalidad_plasmtica_osmp.html
- Ashorobi, D., & Fernandez, R. (2019). Thrombosis. StatPearls [Internet].
- Fisiopatología de la trombosis, medigraphic. Recogido a 8 de abril en https://www.medigraphic.com/pdfs/gaceta/gm-2007/gms071d.pdf
- Mackman, N. (2008). Triggers, targets and treatments for thrombosis. Nature, 451(7181), 914-918.
- Antiplaquetarios, medlineplus.gov. Recogido a 8 de abril en https://medlineplus.gov/spanish/ency/patientinstructions/000100.htm
- Factores de riesgo de la ETV, trombo.info. Recogido a 8 de abril en https://trombo.info/factores-de-riesgo/
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







