Skin Allergies: Everything You Need to Know
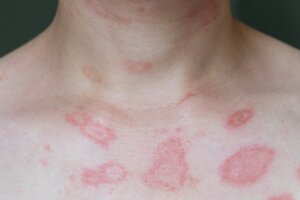
Skin allergies affect thousands of patients each year. This category includes dozens of skin conditions that are caused by an external trigger. They can be easily confused with an infection and their symptoms cause discomfort, low self-esteem and embarrassment among those who suffer from them. Although they’re more common in children, they can occur at any age.
Manifestations of this type are usually chronic and people have to deal with them for years.
Despite this, there are many treatment options, so seek medical assistance to find a solution to flare-ups. In the next few lines, we’ll show you everything you should know about skin allergies.
What are the causes of skin allergies?
There is no single cause of skin allergies. In general, these types of conditions are considered multifactorial, in which genetic predisposition and external triggers play a leading role.
The most common catalysts, according to the Asthma and Allergy Foundation of America, are the following:
- Water
- Pollen
- Mites
- Stings or contact with insects
- Intake of certain foods
- Sunlight
- Drug intake
- Changes in temperature (hot or cold)
- Pet dander
- Interaction with some plants (such as poison ivy)
- Contact with latex
Skin symptoms can also occur, as the American College of Allergy, Asthma and Immunology reminds us, with diseases such as measles or chickenpox. However, these episodes are considered infectious and non-allergic.
Although it varies with each type, reactions happen when the body overreacts to triggers. That is, an excessive reaction is generated. Because of this, patients manifest skin symptoms.
Types of skin allergies
There are many types of skin allergies. The severity of the symptoms, their evolution, and prognosis differ with each case. The American Academy of Asthma, Allergy & Immunology highlights the following 4 manifestations as the most frequent.
Eczema
Also known as eczema or atopic dermatitis, researchers estimate that it affects 20% of children and 3% of adults. It is the most common type of dermatitis and is accompanied by other allergic disorders (such as asthma and rhinitis). Symptoms manifest in flare-ups, also called episodes or exacerbations.
The Australasian Society of Clinical Immunology and Allergy indicates that patients with this type of skin allergy have difficulty retaining moisture. This makes your epidermis dry very easily, allowing allergens to penetrate a particularly sensitive area.
The following clinical manifestations are the most common:
- Rashes that are concentrated on the arms and behind the knees (in children it is more common on the face, elbows, and knees).
- Flaky or dehydrated skin
- Flaking
- Itching in the affected area
- Thick or very sensitive skin
- Spots that ooze fluid (in case infection is added)
Patients should resist the temptation to rub the affected areas, as these can become infected and further itch. This type of condition is not infectious, so it cannot be spread to people it comes in contact with.

Urticaria
Hives is a disorder that occurs when the body releases histamine and bradykinin, among other hormones. The evidence indicates that the classic manifestations are between 1 to 2 centimeters big and can appear anywhere on the body.
Lesions develop in a matter of minutes and disappear after 24 hours. This, of course, occurs only in benign cases. When they grow, they join with others creating larger patterns on the skin. In addition, it is accompanied by the following symptoms:
- Itching (medium or severe)
- Slight inflammation in the affected areas
- Intermittent episodes, appearing and disappearing according to exposure to the trigger
Like all cases of skin allergies, hives are not contagious. Its chronic manifestation can last several weeks and is not always related to a catalyst. It isn’t uncommon for allergy tests to come back negative.
Contact dermatitis
Contact dermatitis is triggered, as the name implies, when the skin comes into direct contact with the allergen. This causes an irritating reaction that is manifested only in the area where the friction has occurred. Based on information from the American Academy of Dermatology (AAD), we present a selection of irritants:
- Household detergents
- Some plants (such as poison ivy)
- Disinfectants
- Petroleum products (gasoline and diesel, for example)
- Bath soaps
- Fertilizers and pesticides
- Jewels
- Some types of fragrances
- Latex
As evidence points out, nickel allergy explains many of the cases of contact dermatitis. Unfortunately, this allergen is frequently used in rings, earrings, cell phones, and e-cigarettes.
Angioedema
Angioedema is the inflammation of the deep layers of the skin. Evidence indicates that most cases clear up within 72 hours, although if you have the chronic variant, you may have to deal with it for longer.
Typically, it concentrates on the soft tissues of the skin, such as the eyelids, mouth, and genitals. It consists of an excessive inflammation that may or may not be accompanied by hives. Generally, it isn’t dangerous, although if it occupies part of the throat or tongue it can block the airways.
It has a couple of variants; among them, hereditary angioedema. It is a rare genetic disorder characterized by inflammation of various parts of the body. Given that it offers greater resistance to conventional therapy, it is important that patients with this type seek a specialist.
Diagnosis of skin allergies
Diagnosis of skin allergies is made by an allergist or a dermatologist. The standard procedure is to subject the body to allergens to assess which of these causes the reaction.
For this, some of the following options are used:
- Patch test: this consists of applying a patch directly to the skin and assessing the results of the exposure between 24 and 48 hours later. The patch contains specific allergens, so the area under and around it will show signs of allergy. It is a safe, painless and very useful procedure for contact dermatitis.
- Skin prick test: In this case a needle is used to make a superficial puncture in the skin to detect about 50 triggers of skin allergies. It is useful for determining episodes caused by pollen, mold, mites and dust. Although it may be uncomfortable, it is a painless test.
- Skin injection test: Similar to above, only this time the allergen goes a little deeper into the skin. It is useful to assess the possible reaction to drugs or insect venom (bees, for example).
The specialist may also opt for an exposure test. In it, the person is directly exposed to the allergen, usually pollen or food, to assess their reaction. The risks of this examination are greater, so it must be carried out in a controlled environment and in the presence of professionals.
It isn’t uncommon for blood tests to be performed to find some indicators of allergies. Although home tests can be helpful in taking a first step toward screening, the above are currently the standard.

Treatment of skin allergies
The treatment of skin allergies varies according to the manifestation, although they are generally based on the application of hydrocortisone creams and the intake of antihistamines. Researchers also approve the use of biologics to relieve symptoms. Corticosteroids, in their various forms, are a highly prescribed option.
But these are not the only therapies available for skin allergies. Here are a selection of tips for you to reduce the duration of episodes and avoid exacerbations:
- Apply cold or damp cloth compresses directly to the affected area
- Always keep your skin hydrated with neutral products
- During episodes, avoid bathing in hot water
- Try not to wear tight clothing that creates friction
- Buy lotions, soaps, and detergents that are not scented strongly
- Take oatmeal baths a few times a week
If you take these principles into account and apply the treatment indicated by the specialist, then you will be able to control the regularity of the outbreaks. If these are very common, it’s a sign that the condition isn’t being treated properly. Talk to your specialist about drug alternatives that you can use as therapy.
Skin allergies affect thousands of patients each year. This category includes dozens of skin conditions that are caused by an external trigger. They can be easily confused with an infection and their symptoms cause discomfort, low self-esteem and embarrassment among those who suffer from them. Although they’re more common in children, they can occur at any age.
Manifestations of this type are usually chronic and people have to deal with them for years.
Despite this, there are many treatment options, so seek medical assistance to find a solution to flare-ups. In the next few lines, we’ll show you everything you should know about skin allergies.
What are the causes of skin allergies?
There is no single cause of skin allergies. In general, these types of conditions are considered multifactorial, in which genetic predisposition and external triggers play a leading role.
The most common catalysts, according to the Asthma and Allergy Foundation of America, are the following:
- Water
- Pollen
- Mites
- Stings or contact with insects
- Intake of certain foods
- Sunlight
- Drug intake
- Changes in temperature (hot or cold)
- Pet dander
- Interaction with some plants (such as poison ivy)
- Contact with latex
Skin symptoms can also occur, as the American College of Allergy, Asthma and Immunology reminds us, with diseases such as measles or chickenpox. However, these episodes are considered infectious and non-allergic.
Although it varies with each type, reactions happen when the body overreacts to triggers. That is, an excessive reaction is generated. Because of this, patients manifest skin symptoms.
Types of skin allergies
There are many types of skin allergies. The severity of the symptoms, their evolution, and prognosis differ with each case. The American Academy of Asthma, Allergy & Immunology highlights the following 4 manifestations as the most frequent.
Eczema
Also known as eczema or atopic dermatitis, researchers estimate that it affects 20% of children and 3% of adults. It is the most common type of dermatitis and is accompanied by other allergic disorders (such as asthma and rhinitis). Symptoms manifest in flare-ups, also called episodes or exacerbations.
The Australasian Society of Clinical Immunology and Allergy indicates that patients with this type of skin allergy have difficulty retaining moisture. This makes your epidermis dry very easily, allowing allergens to penetrate a particularly sensitive area.
The following clinical manifestations are the most common:
- Rashes that are concentrated on the arms and behind the knees (in children it is more common on the face, elbows, and knees).
- Flaky or dehydrated skin
- Flaking
- Itching in the affected area
- Thick or very sensitive skin
- Spots that ooze fluid (in case infection is added)
Patients should resist the temptation to rub the affected areas, as these can become infected and further itch. This type of condition is not infectious, so it cannot be spread to people it comes in contact with.

Urticaria
Hives is a disorder that occurs when the body releases histamine and bradykinin, among other hormones. The evidence indicates that the classic manifestations are between 1 to 2 centimeters big and can appear anywhere on the body.
Lesions develop in a matter of minutes and disappear after 24 hours. This, of course, occurs only in benign cases. When they grow, they join with others creating larger patterns on the skin. In addition, it is accompanied by the following symptoms:
- Itching (medium or severe)
- Slight inflammation in the affected areas
- Intermittent episodes, appearing and disappearing according to exposure to the trigger
Like all cases of skin allergies, hives are not contagious. Its chronic manifestation can last several weeks and is not always related to a catalyst. It isn’t uncommon for allergy tests to come back negative.
Contact dermatitis
Contact dermatitis is triggered, as the name implies, when the skin comes into direct contact with the allergen. This causes an irritating reaction that is manifested only in the area where the friction has occurred. Based on information from the American Academy of Dermatology (AAD), we present a selection of irritants:
- Household detergents
- Some plants (such as poison ivy)
- Disinfectants
- Petroleum products (gasoline and diesel, for example)
- Bath soaps
- Fertilizers and pesticides
- Jewels
- Some types of fragrances
- Latex
As evidence points out, nickel allergy explains many of the cases of contact dermatitis. Unfortunately, this allergen is frequently used in rings, earrings, cell phones, and e-cigarettes.
Angioedema
Angioedema is the inflammation of the deep layers of the skin. Evidence indicates that most cases clear up within 72 hours, although if you have the chronic variant, you may have to deal with it for longer.
Typically, it concentrates on the soft tissues of the skin, such as the eyelids, mouth, and genitals. It consists of an excessive inflammation that may or may not be accompanied by hives. Generally, it isn’t dangerous, although if it occupies part of the throat or tongue it can block the airways.
It has a couple of variants; among them, hereditary angioedema. It is a rare genetic disorder characterized by inflammation of various parts of the body. Given that it offers greater resistance to conventional therapy, it is important that patients with this type seek a specialist.
Diagnosis of skin allergies
Diagnosis of skin allergies is made by an allergist or a dermatologist. The standard procedure is to subject the body to allergens to assess which of these causes the reaction.
For this, some of the following options are used:
- Patch test: this consists of applying a patch directly to the skin and assessing the results of the exposure between 24 and 48 hours later. The patch contains specific allergens, so the area under and around it will show signs of allergy. It is a safe, painless and very useful procedure for contact dermatitis.
- Skin prick test: In this case a needle is used to make a superficial puncture in the skin to detect about 50 triggers of skin allergies. It is useful for determining episodes caused by pollen, mold, mites and dust. Although it may be uncomfortable, it is a painless test.
- Skin injection test: Similar to above, only this time the allergen goes a little deeper into the skin. It is useful to assess the possible reaction to drugs or insect venom (bees, for example).
The specialist may also opt for an exposure test. In it, the person is directly exposed to the allergen, usually pollen or food, to assess their reaction. The risks of this examination are greater, so it must be carried out in a controlled environment and in the presence of professionals.
It isn’t uncommon for blood tests to be performed to find some indicators of allergies. Although home tests can be helpful in taking a first step toward screening, the above are currently the standard.

Treatment of skin allergies
The treatment of skin allergies varies according to the manifestation, although they are generally based on the application of hydrocortisone creams and the intake of antihistamines. Researchers also approve the use of biologics to relieve symptoms. Corticosteroids, in their various forms, are a highly prescribed option.
But these are not the only therapies available for skin allergies. Here are a selection of tips for you to reduce the duration of episodes and avoid exacerbations:
- Apply cold or damp cloth compresses directly to the affected area
- Always keep your skin hydrated with neutral products
- During episodes, avoid bathing in hot water
- Try not to wear tight clothing that creates friction
- Buy lotions, soaps, and detergents that are not scented strongly
- Take oatmeal baths a few times a week
If you take these principles into account and apply the treatment indicated by the specialist, then you will be able to control the regularity of the outbreaks. If these are very common, it’s a sign that the condition isn’t being treated properly. Talk to your specialist about drug alternatives that you can use as therapy.
- Ahlström MG, Thyssen JP, Wennervaldt M, Menné T, Johansen JD. Nickel allergy and allergic contact dermatitis: A clinical review of immunology, epidemiology, exposure, and treatment. Contact Dermatitis. 2019 Oct;81(4):227-241.
- Eyerich S, Metz M, Bossios A, Eyerich K. New biological treatments for asthma and skin allergies. Allergy. 2020 Mar;75(3):546-560.
- Holguín-Gómez, L. M., Vásquez-Ochoa, L. A., & Cardona, R. (2016). Revista Alergia México. 2016; 63(4): 373-384.
- Nutten S. Atopic dermatitis: global epidemiology and risk factors. Ann Nutr Metab. 2015;66 Suppl 1:8-16. doi: 10.1159/000370220. Epub 2015 Apr 24. PMID: 25925336.
- Schaefer P. Urticaria: evaluation and treatment. Am Fam Physician. 2011 May 1;83(9):1078-84.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







