Latex Allergy: Everything You Need to Know

According to the World Allergy Organization, it’s estimated that there are more than 13 million people worldwide with a latex allergy. The number could be even higher, because the compound is used less and less in first-world countries, and reported cases have dropped considerably.
Although it’s less common than other types of allergies (such as pollen allergy), in reality this condition is associated with a greater number of complications. For example, patients may more easily develop anaphylaxis or asthma. Today we’ll tell you everything that we know about these reactions, especially about what you can do to prevent them.
What is a latex allergy?

Latex is a milky liquid that’s extracted from the rubber tree in the forests of South America and Central America. It’s used as a liner for surgical gloves, condoms, balloons, erasers, toys, bottles, some clothing items, paint, shoe soles, and many other objects. When a person who is sensitive to this compound comes into contact with any of them, they develop an allergic reaction.
As the American Academy of Allergy, Asthma & Immunology reminds us, latex allergy was relatively rare until the late 1980s, with only a couple of thousand cases previously reported worldwide. Since becoming aware of the possibility of allergic reactions, synthetic variants have been chosen, and so reactions of this type have clearly diminished.
Patients can develop reactions from any type of contact with the substance. Here are some examples:
- After tasting food prepared by a person who wore latex gloves.
- By inhaling the dust that covers many of the products coated with the substance.
- Through intravenous injection lines or surgical procedures (when such materials are used).
- By having sex with condoms or diaphragms made of latex.
- Absorption of the substance through wounds or trauma to the skin.
- An interaction with any type of product that has used it as a coating.
In addition to this, reactions can be produced when food that contains the same proteins as the natural substance is ingested. For example, bananas, avocados, and chestnuts. These are the most important groups, although others such as kiwis, peaches, apples, carrots, tomatoes, and melons, among others, can trigger reactions by having similar proteins.
According to the Australasian Society of Clinical Immunology and Allergy (ASCIA), most cases are reported in people who have been in contact with the compound for a long period of time. Doctors, nurses, dentists, and patients who have had several operations are the main focuses. Also, those with a history of allergic reactions, hay fever, hives, or dermatitis.
Symptoms of latex allergy
Patients show many symptoms due to contact with the substance. These depend on the degree of sensitivity and the amount of latex to which they have been exposed. It can develop in a focal or generalized manner, and manifestations usually occur in the vicinity of the contact surface.
Following the information provided by the Asthma and Allergy Foundation for America (AAFA), we highlight the following examples of the symptoms you can develop from latex allergy:
- Swelling of the lips after inflating a balloon.
- Swelling or itching in the mouth after going to the dentist (if the dentist has used latex gloves).
- Itching and swelling in the genitals after using latex condoms.
- Red, itchy skin, rashes, and hives after wearing a latex-coated bandage.
- Runny nose, sneezing, watery eyes, and other classic allergy symptoms.
People can also develop an anaphylactic reaction, most often if the dust enters their mucous membranes and travels to some point in their airways. These cases are potentially dangerous and require rapid intervention with epinephrine to control them.
How is a latex allergy diagnosed?
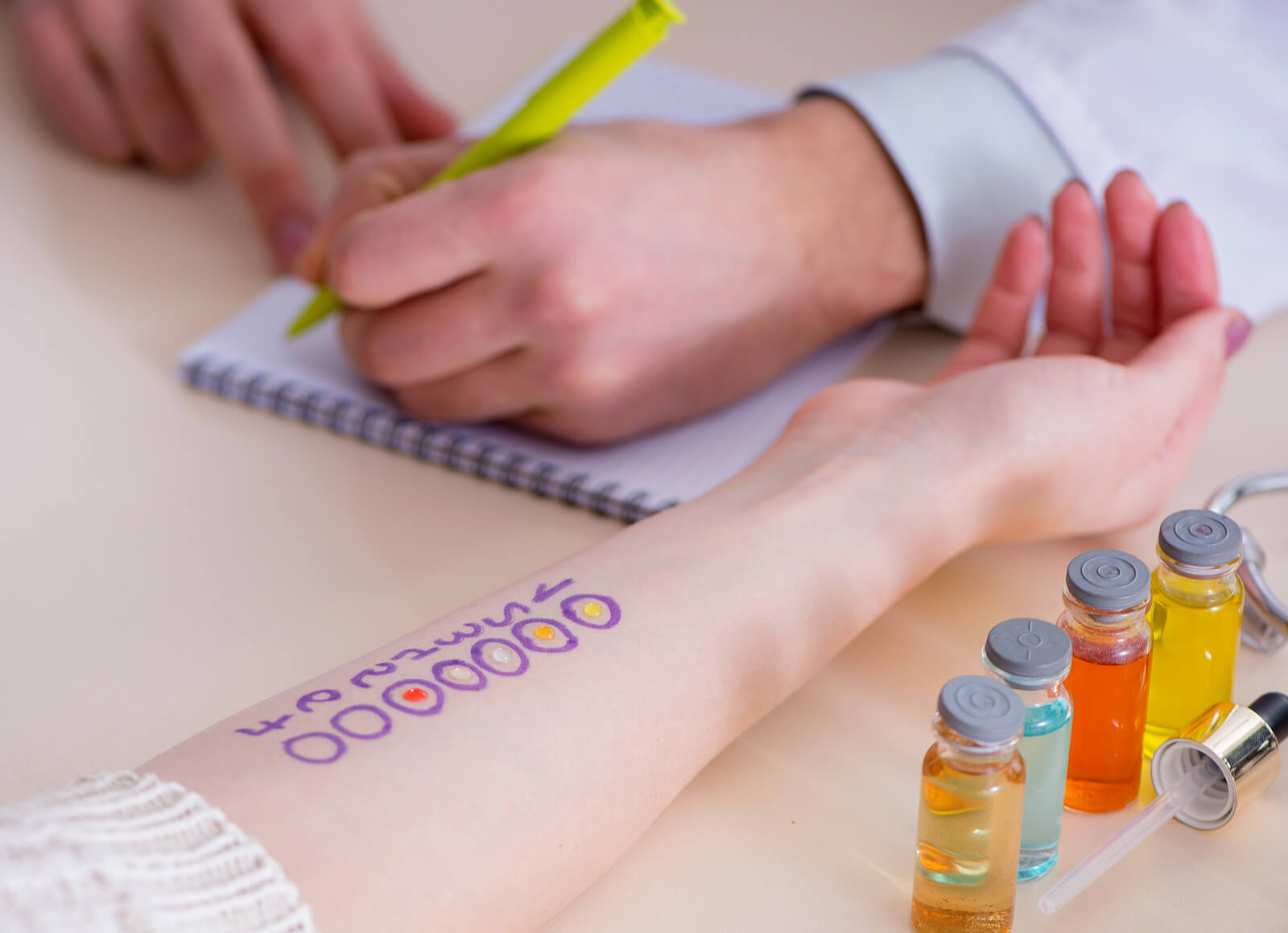
Since the reaction is triggered at specific times, the diagnosis of latex allergy shouldn’t be too complicated. The process begins when the patient discovers reactions of inflammation and itching when in contact with gloves, bandages, and other things, and so they turn to a specialist to confirm the allergy.
Researchers suggest three tests for accurate detection: a positive latex radioallergosorbent test (RAST), a skin prick test, and a challenge test. In the latter, patients are directly exposed to a controlled environment and their reaction is assessed during the next few minutes.
Treatment options available
There’s no cure for latex allergy, but, fortunately, it’s a condition that can be treated very efficiently. The American College of Allergy, Asthma & Immunology recommends that patients who develop severe reactions carry an allergy tag and an injection of epinephrine with them at all times.
It’s also recommended that you opt for synthetic latex-coated alternatives, which are common in today’s market. Inform your dentist before going to an appointment that you suffer from this allergy, as well as any medical specialist you have to visit. Also, avoid takeaway food, as you do not know whether the people who prepared it have used latex gloves.
In the long term, researchers endorse the use of immunotherapy, although this should be carried out with caution because the adverse effects are higher than with other types of allergies. Evidence suggests that antihistamine and corticosteroid therapy is helpful in treating current reactions.
Whatever the case, the important thing is to avoid exposure. Consider removing all latex products from your home, including toys, rugs, and some types of sprays. Go to the specialist if you can’t control the reactions, and they’ll give you more personalized guidance.
According to the World Allergy Organization, it’s estimated that there are more than 13 million people worldwide with a latex allergy. The number could be even higher, because the compound is used less and less in first-world countries, and reported cases have dropped considerably.
Although it’s less common than other types of allergies (such as pollen allergy), in reality this condition is associated with a greater number of complications. For example, patients may more easily develop anaphylaxis or asthma. Today we’ll tell you everything that we know about these reactions, especially about what you can do to prevent them.
What is a latex allergy?

Latex is a milky liquid that’s extracted from the rubber tree in the forests of South America and Central America. It’s used as a liner for surgical gloves, condoms, balloons, erasers, toys, bottles, some clothing items, paint, shoe soles, and many other objects. When a person who is sensitive to this compound comes into contact with any of them, they develop an allergic reaction.
As the American Academy of Allergy, Asthma & Immunology reminds us, latex allergy was relatively rare until the late 1980s, with only a couple of thousand cases previously reported worldwide. Since becoming aware of the possibility of allergic reactions, synthetic variants have been chosen, and so reactions of this type have clearly diminished.
Patients can develop reactions from any type of contact with the substance. Here are some examples:
- After tasting food prepared by a person who wore latex gloves.
- By inhaling the dust that covers many of the products coated with the substance.
- Through intravenous injection lines or surgical procedures (when such materials are used).
- By having sex with condoms or diaphragms made of latex.
- Absorption of the substance through wounds or trauma to the skin.
- An interaction with any type of product that has used it as a coating.
In addition to this, reactions can be produced when food that contains the same proteins as the natural substance is ingested. For example, bananas, avocados, and chestnuts. These are the most important groups, although others such as kiwis, peaches, apples, carrots, tomatoes, and melons, among others, can trigger reactions by having similar proteins.
According to the Australasian Society of Clinical Immunology and Allergy (ASCIA), most cases are reported in people who have been in contact with the compound for a long period of time. Doctors, nurses, dentists, and patients who have had several operations are the main focuses. Also, those with a history of allergic reactions, hay fever, hives, or dermatitis.
Symptoms of latex allergy
Patients show many symptoms due to contact with the substance. These depend on the degree of sensitivity and the amount of latex to which they have been exposed. It can develop in a focal or generalized manner, and manifestations usually occur in the vicinity of the contact surface.
Following the information provided by the Asthma and Allergy Foundation for America (AAFA), we highlight the following examples of the symptoms you can develop from latex allergy:
- Swelling of the lips after inflating a balloon.
- Swelling or itching in the mouth after going to the dentist (if the dentist has used latex gloves).
- Itching and swelling in the genitals after using latex condoms.
- Red, itchy skin, rashes, and hives after wearing a latex-coated bandage.
- Runny nose, sneezing, watery eyes, and other classic allergy symptoms.
People can also develop an anaphylactic reaction, most often if the dust enters their mucous membranes and travels to some point in their airways. These cases are potentially dangerous and require rapid intervention with epinephrine to control them.
How is a latex allergy diagnosed?

Since the reaction is triggered at specific times, the diagnosis of latex allergy shouldn’t be too complicated. The process begins when the patient discovers reactions of inflammation and itching when in contact with gloves, bandages, and other things, and so they turn to a specialist to confirm the allergy.
Researchers suggest three tests for accurate detection: a positive latex radioallergosorbent test (RAST), a skin prick test, and a challenge test. In the latter, patients are directly exposed to a controlled environment and their reaction is assessed during the next few minutes.
Treatment options available
There’s no cure for latex allergy, but, fortunately, it’s a condition that can be treated very efficiently. The American College of Allergy, Asthma & Immunology recommends that patients who develop severe reactions carry an allergy tag and an injection of epinephrine with them at all times.
It’s also recommended that you opt for synthetic latex-coated alternatives, which are common in today’s market. Inform your dentist before going to an appointment that you suffer from this allergy, as well as any medical specialist you have to visit. Also, avoid takeaway food, as you do not know whether the people who prepared it have used latex gloves.
In the long term, researchers endorse the use of immunotherapy, although this should be carried out with caution because the adverse effects are higher than with other types of allergies. Evidence suggests that antihistamine and corticosteroid therapy is helpful in treating current reactions.
Whatever the case, the important thing is to avoid exposure. Consider removing all latex products from your home, including toys, rugs, and some types of sprays. Go to the specialist if you can’t control the reactions, and they’ll give you more personalized guidance.
- Patriarca G, Nucera E, Buonomo A, Roncallo C, De Pasquale T, Pollastrini E, Schiavino D. New insights on latex allergy diagnosis and treatment. J Investig Allergol Clin Immunol. 2002;12(3):169-76.
- Rolland JM, O’Hehir RE. Latex allergy: a model for therapy. Clin Exp Allergy. 2008 Jun;38(6):898-912.
- Taylor JS, Erkek E. Latex allergy: diagnosis and management. Dermatol Ther. 2004;17(4):289-301.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







