Colorectal Polyps: Everything You Need to Know
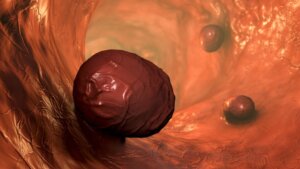
Polyps are small raised lesions that arise in the mucosa and project into the lumen of a hollow viscus. In general, these proliferations originate in the intestine and have a benign course. However, some can evolve into cancerous lesions. Are you interested in learning about colorectal polyps? Here we’ll tell you everything you need to know.
The colon and rectum are susceptible to polyps in elderly patients. Similarly, they can be congenital or acquired, and are classified according to their nature as neoplastic and non-neoplastic. Studies affirm that more than 5% of polyps progress to colorectal cancer.
Symptoms

In most people, colon and rectal polyps don’t cause any symptoms. They can easily go unnoticed, being diagnosed during routine evaluations or screening tests. In some cases, these lesions can ulcerate and cause rectal bleeding. Similarly, some people may develop the following symptoms:
- Colic and abdominal discomfort
- Dark or blackish stools
- Constipation
- Rectal occupation sensation
- Diarrhea
On the other hand, continuous intestinal bleeding promoted by polyps can lead to long-term anemia. In this sense, blood loss leads to a deficiency in iron levels and in the formation of hemoglobin, leading to iron deficiency anemia. Also, some large polyps can become complicated, causing intussusception and intestinal obstruction.
You may be interested in: Colon Cancer in Children
Why do colorectal polyps occur?
All tissues are made up of cells that grow and multiply in an orderly fashion to shape organs. However, the alteration of the genetic material of these cells can lead to the proliferation of abnormal lesions in the body. Colorectal polyps are the result of an uncontrolled cell division anywhere in the mucosa of the large intestine.
Currently, polyps are classified as neoplastic and non-neoplastic based on their microscopic characteristics. In general, the lesions with carcinogenic potential originate from the ganglion cells that line the colorectal tissue, and cause the so-called adenomatous polyps. Some research (in Spanish) suggests that these polyps progress to cancer in 95% of cases.
Non-neoplastic conditions can result from hyperplastic, inflammatory, and lymphoid polyps, as well as hamartomas. Inflammatory polyposis commonly originates from inflammatory bowel diseases such as Crohn’s disease. On the other hand, hyperplastic lesions usually develop at the level of the rectum with a size of no greater than 5 millimeters.
Similarly, there are hereditary pathologies that promote the growth of polyps in the colon and rectum. Among the diseases associated with this condition are the following:
- Peutz-Jeghers syndrome
- MUTYH polyposis syndrome
- Familial adenomatous polyposis
- Lynch syndrome
- Gardner syndrome
Risk factors
The alteration of cellular genetic material that promotes the formation of polyps is influenced by various intrinsic and lifestyle variables. Some factors that increase the likelihood of suffering from this condition are the following:
- Being more than 50 years of age
- Being of African descent
- Uncontrolled type 2 diabetes
- Having suffered from ulcerative colitis or Crohn’s disease
- Tobacco use
- Excessive alcohol consumption
- Obesity
- A sedentary lifestyle and lack of physical exercise
A family history of colon and rectal cancer or polyps greatly increases the incidence of these pathologies, due to recurrences. Furthermore, the risk increases in proportion to the number of direct relatives affected. In this way, specialists recommend early detection tests in this type of patient.
Diagnosis
The identification of colorectal polyps is based on a comprehensive clinical examination supported by imaging studies and laboratory tests. The treating physician can palpate the lesions at the level of the rectal ampulla digitally. In addition, the clinical manifestations and family history offer data that can increase the diagnostic suspicion.
Studies (in Spanish) affirm that colonoscopy is the procedure of choice for the detection of polyps located along the colon or in the rectum. Similarly, flexible sigmoidoscopy, computerized axial tomography (CT), and magnetic resonance imaging (MRI) are other imaging studies that can be used within the diagnostic protocol.
On the other hand, stool samples can be tested for signs suggestive of this condition, such as occult blood in stools. Fecal studies are also useful in the detection of tumor DNA as part of the colorectal cancer screening tests associated with neoplastic polyps. In addition, genetic testing is possible for hereditary diseases.
Find out more: Alcohol and Digestive Diseases: What’s the Link?
Treatment of colorectal polyps
The treatment of colorectal polyps is based on the total resection of the lesion, seeking to prevent its abnormal growth and malignant evolution. Endoscopic polypectomy is the most widely used method in the therapeutic approach to these conditions. Surgeons usually remove all visible polyps in the colon and rectum when performing the procedure.
On the other hand, laparoscopic abdominal surgery is the procedure to be performed in case of large lesions. Some patients with hereditary familial polyposis may require the removal of the colon and rectum through a total proctocolectomy. Resected polyps should be evaluated by a biopsy to determine the need for anticancer treatment.
Prevention is vital in the prognosis of this condition
Colon and rectal polyps are associated with people over 50 with a family history of this condition. Today, it’s possible to reduce the risk of polyposis and its progression to colorectal cancer through small changes in lifestyle. In this sense, diets rich in fruits, vegetables, and fibers, as well as physical activity are the main prevention measures.
In the same way, people should maintain a routine check on their health status with their family doctor. The early detection of polyps and their timely management determine a better prognosis of the disease and a higher quality of life.
Polyps are small raised lesions that arise in the mucosa and project into the lumen of a hollow viscus. In general, these proliferations originate in the intestine and have a benign course. However, some can evolve into cancerous lesions. Are you interested in learning about colorectal polyps? Here we’ll tell you everything you need to know.
The colon and rectum are susceptible to polyps in elderly patients. Similarly, they can be congenital or acquired, and are classified according to their nature as neoplastic and non-neoplastic. Studies affirm that more than 5% of polyps progress to colorectal cancer.
Symptoms

In most people, colon and rectal polyps don’t cause any symptoms. They can easily go unnoticed, being diagnosed during routine evaluations or screening tests. In some cases, these lesions can ulcerate and cause rectal bleeding. Similarly, some people may develop the following symptoms:
- Colic and abdominal discomfort
- Dark or blackish stools
- Constipation
- Rectal occupation sensation
- Diarrhea
On the other hand, continuous intestinal bleeding promoted by polyps can lead to long-term anemia. In this sense, blood loss leads to a deficiency in iron levels and in the formation of hemoglobin, leading to iron deficiency anemia. Also, some large polyps can become complicated, causing intussusception and intestinal obstruction.
You may be interested in: Colon Cancer in Children
Why do colorectal polyps occur?
All tissues are made up of cells that grow and multiply in an orderly fashion to shape organs. However, the alteration of the genetic material of these cells can lead to the proliferation of abnormal lesions in the body. Colorectal polyps are the result of an uncontrolled cell division anywhere in the mucosa of the large intestine.
Currently, polyps are classified as neoplastic and non-neoplastic based on their microscopic characteristics. In general, the lesions with carcinogenic potential originate from the ganglion cells that line the colorectal tissue, and cause the so-called adenomatous polyps. Some research (in Spanish) suggests that these polyps progress to cancer in 95% of cases.
Non-neoplastic conditions can result from hyperplastic, inflammatory, and lymphoid polyps, as well as hamartomas. Inflammatory polyposis commonly originates from inflammatory bowel diseases such as Crohn’s disease. On the other hand, hyperplastic lesions usually develop at the level of the rectum with a size of no greater than 5 millimeters.
Similarly, there are hereditary pathologies that promote the growth of polyps in the colon and rectum. Among the diseases associated with this condition are the following:
- Peutz-Jeghers syndrome
- MUTYH polyposis syndrome
- Familial adenomatous polyposis
- Lynch syndrome
- Gardner syndrome
Risk factors
The alteration of cellular genetic material that promotes the formation of polyps is influenced by various intrinsic and lifestyle variables. Some factors that increase the likelihood of suffering from this condition are the following:
- Being more than 50 years of age
- Being of African descent
- Uncontrolled type 2 diabetes
- Having suffered from ulcerative colitis or Crohn’s disease
- Tobacco use
- Excessive alcohol consumption
- Obesity
- A sedentary lifestyle and lack of physical exercise
A family history of colon and rectal cancer or polyps greatly increases the incidence of these pathologies, due to recurrences. Furthermore, the risk increases in proportion to the number of direct relatives affected. In this way, specialists recommend early detection tests in this type of patient.
Diagnosis

The identification of colorectal polyps is based on a comprehensive clinical examination supported by imaging studies and laboratory tests. The treating physician can palpate the lesions at the level of the rectal ampulla digitally. In addition, the clinical manifestations and family history offer data that can increase the diagnostic suspicion.
Studies (in Spanish) affirm that colonoscopy is the procedure of choice for the detection of polyps located along the colon or in the rectum. Similarly, flexible sigmoidoscopy, computerized axial tomography (CT), and magnetic resonance imaging (MRI) are other imaging studies that can be used within the diagnostic protocol.
On the other hand, stool samples can be tested for signs suggestive of this condition, such as occult blood in stools. Fecal studies are also useful in the detection of tumor DNA as part of the colorectal cancer screening tests associated with neoplastic polyps. In addition, genetic testing is possible for hereditary diseases.
Find out more: Alcohol and Digestive Diseases: What’s the Link?
Treatment of colorectal polyps
The treatment of colorectal polyps is based on the total resection of the lesion, seeking to prevent its abnormal growth and malignant evolution. Endoscopic polypectomy is the most widely used method in the therapeutic approach to these conditions. Surgeons usually remove all visible polyps in the colon and rectum when performing the procedure.
On the other hand, laparoscopic abdominal surgery is the procedure to be performed in case of large lesions. Some patients with hereditary familial polyposis may require the removal of the colon and rectum through a total proctocolectomy. Resected polyps should be evaluated by a biopsy to determine the need for anticancer treatment.
Prevention is vital in the prognosis of this condition
Colon and rectal polyps are associated with people over 50 with a family history of this condition. Today, it’s possible to reduce the risk of polyposis and its progression to colorectal cancer through small changes in lifestyle. In this sense, diets rich in fruits, vegetables, and fibers, as well as physical activity are the main prevention measures.
In the same way, people should maintain a routine check on their health status with their family doctor. The early detection of polyps and their timely management determine a better prognosis of the disease and a higher quality of life.
- Garrido Botella A, Garrido Gómez E. Pólipos de colon. Rev. esp. enferm. dig. 2007; 99( 1 ): 48-48.
- Sihues E, Añez M, Lizarzabal M, Rangel R et al . Pólipos de colon: Una revisión de 1 año de experiencia en un centro de referencia. Gen. 2008; 62( 1 ): 60-63.
- Bastos N. Clasificación de los pólipos de la mucosa del colon y recto: uso del sistema de imágenes de banda angosta. Gen. 2011; 65( 1 ): 22-29.
- Rodríguez Fernández Z, Jean-Louis B, Lozada Prado G, Joubert Álvarez G, Pineda Chacón J. Conocimientos vigentes acerca del cáncer de colon recurrente. MEDISAN. 2015; 19( 6 ): 797-814.
- López Colombo A. Colon y recto. Pólipos colónicos [Colorectal diseases. Colon polyps]. Rev Gastroenterol Mex. 2010;75 Suppl 1:127-9.
- Gallo Reynoso S, Candelaria Hernández MG. Pólipos neoplásicos del colon [Neoplastic polyps of the colon]. Rev Gastroenterol Mex. 1992;57(1):27-31.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







