Colon Cancer Diagnosis

Colon cancer is the third most common neoplastic condition in men worldwide. In general, this pathology originates from polyps that form inside the large intestine. Early diagnosis of colon cancer is key to offering a better prognosis and a higher quality of life for those affected.
Currently, the American Cancer Society suggests colon cancer screening starting at age 45 in people at average risk. The digital rectal examination, colonoscopy, and stool examination are the most used methods for the identification of the classic signs of this pathology.
Clinical examination
A comprehensive clinical approach is vital for the diagnosis of early-stage colon cancer. In this sense, the treating physician will initiate the detection protocol from the questioning of the symptoms afflicting the patient. Changes in stool consistency, urgency, rectal bleeding, fatigue, and abdominal discomfort often guide the clinical diagnosis.
Similarly, medical history and family history are very useful in the prognosis of the state of health, as well as in the detection of possible risk factors for this intestinal condition. In this sense, age over 50 years, family or personal history of polyps, colorectal neoplasms, ulcerative colitis, and Crohn’s disease increase the probability of developing colon cancer.
The specialist doctor will carry out an adequate physical examination in search of any signs or anomalies suggestive of this condition. Palpation of the abdomen allows the identification of masses, painful areas, and enlarged viscera that allow a differential diagnosis of colon cancer to be established.
In addition, the digital rectal examination is one of the most used tests for the identification of colorectal alterations. It consists of the introduction of a gloved and lubricated finger through the anal orifice in search of structural abnormalities, secretions, or proliferations in the rectal epithelium.
Lab tests
Laboratory tests are indicated by the treating physician in order to obtain a broader picture of the general condition of the patient. Among the most used tests for the identification of the signs of colon cancer and the definitive diagnosis are the following.
Stool examination
Studies of fecal samples provide information about the macroscopic and microscopic characteristics of the intestinal contents. Studies affirm that the detection of occult blood in feces is very useful in the investigation and initial diagnosis of the condition. The bleeding is usually the result of the rupture of the blood vessels near the polyps or tumor lesions.
The Fecal Immunochemical Test (FIT) can easily detect occult blood by reacting with the hemoglobin contained in fecal material. Similarly, the guaiac-based fecal occult blood test (gFOBT) uses a chemical reaction to identify red blood cells in the stool.
On the other hand, the multidirectional stool DNA test or MT-sDNA allows the identification of abnormal DNA from cancer cells that proliferate in the colon and rectum. It is recommended every 3 years in patients at high risk of colon cancer.
In case the samples are positive for occult blood in the stool, a confirmatory colonoscopy is necessary. This sign can be positive not only in colon cancer and polyps, but also in patients with ulcers and hemorrhoids, so the interior of the large intestine should be observed to identify the origin of the bleeding.
Blood test
The complete blood count provides detailed information on the red blood cell, white blood cell, and platelet count, as well as the size and concentration characteristics of the hemoglobin in the red blood cells.
Hypochromic microcytic anemia (ie, small, “pale” red blood cells) is common in people with colon cancer as a result of blood loss and destruction of red blood cells by the tumor.
On the other hand, white blood cells may be elevated, which is called leukocytosis, in response to necrosis (tissue death) and tumor invasion. Furthermore, liver metastasis and septic complications in affected people are also associated with this sign.
Tumor marker detection
In some cases, tumor cells are capable of producing and releasing certain substances or markers into the bloodstream that can be identified by serological tests. Studies confirm that carcinoembryonic antigen (CEA) is expressed in more than 90% of colorectal neoplasms. In fact, it is the most widely used biomarker in the diagnosis of colon cancer.
CEA generally remains below 2.5 nanograms per milliliter in nonsmoking patients. Colon adenocarcinoma is the main responsible for the elevation of this tumor marker. Similarly, it can be elevated in other types of colorectal neoplasms or in breast, gastrointestinal, lung, thyroid, and pancreatic cancer.
The carbohydrate antigen 19-9 (CA 19-9) is another of the substances linked to colon cancer, whose normal levels are below 37 units per milliliter. CA 19-9 values are related to CEA values in the follow-up of people diagnosed who are under treatment. In addition, they show great sensitivity in detecting metastasis to other organs.
Liver function test
Usually, late-stage colon neoplasms can spread to liver tissue. For this reason, the specialist may order a blood test to assess the status of the liver. In this sense, it’s common to show an alteration of total and fractionated proteins, especially in those who suffer from localized liver metastasis or recurrence.
Biopsy
This test consists of the extraction of a sample of the affected tissue for its subsequent microscopic and histopathological study. Research affirms that the biopsy is the standard confirmatory test in the diagnosis of colon cancer. It is requested when there is clinical suspicion or when there is evidence by an imaging study of an abnormal mass in the large intestine.
On the other hand, it’s very useful in the classification of colon neoplasms based on the cellular characteristics and the degree of differentiation of the tissue. It also makes it possible to determine the severity of the disease, deduce the patient’s prognosis, and implement the most effective treatment.
Imaging tests
Imaging studies allow a more detailed view of the general state of internal organs to be obtained. They are used in patients with suspected colon cancer in search of abnormal lesions or proliferations suggestive of malignancy. Some of the imaging tests used are the following:
Colonoscopy
Colonoscopy is one of the most widely used imaging methods in the early diagnosis of colon cancer. It consists of the introduction of a thin and flexible tube with a camera at its end through the anal opening. In this way, it is possible to explore the inside of the rectum and anus in its entirety, verifying if there are tumors or polyps that could evolve into cancer.
In addition, this procedure allows the introduction of special instruments for taking the biopsy sample. It also offers the possibility of removing any small lesions with potential malignancy if necessary.
CT colonography
Computed tomography (CT) colonography allows the colonic structure to be visualized through special cuts made by an X-ray machine. During this test, a small tube is inserted through the anal opening, which will be inflated with gas to obtain a more detailed image of the rectum and colon.
Flexible sigmoidoscopy
Sigmoidoscopy is an endoscopic method that allows exploration of the inside of the rectum and sigmoid colon. This test generally requires less preparation, and, in some people, anesthesia is not necessary. In case of polyps or any other lesion suggestive of cancer, a colonoscopy will be indicated to evaluate the rest of the large intestine.
Magnetic resonance
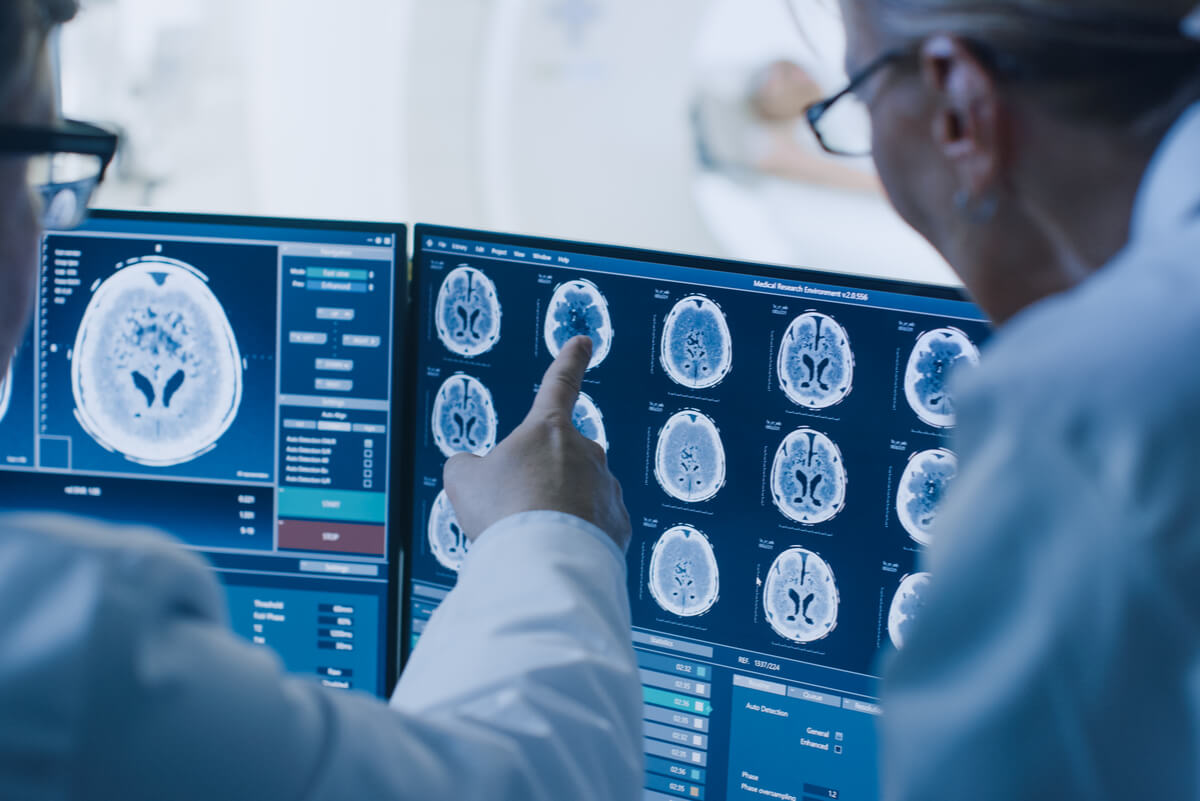
Magnetic resonance imaging (MRI) is useful in the non-invasive assessment of soft tissues and in the detection of tumor processes. In some cases, a contrast medium may be administered parenterally before starting the procedure. It facilitates the detection of metastatic spread of cancer to the liver, brain, and spinal cord.
On the other hand, endorectal MRI is used in the diagnosis of colon cancer spread to adjacent organs or tissues. Unlike traditional MRI, this uses a small probe that will remain in the rectum during the study. In addition, it is used in the planning of surgical or chemotherapy treatment of affected people.
Colon cancer staging
The large intestine is lined by an inner layer or mucosa, which is the area where most cancerous lesions usually start. Similarly, it has a submucosal layer and a muscular layer just below the mucosa. On the other hand, the subserous and serous layers cover the external face of most of the colon, with the exception of the rectal tissue.
How is staging done?
Currently, the staging of colorectal neoplasms is based on the system established by the American Joint Committee on Cancer (AJCC). It considers the extent and size of the tumor, spread to lymph nodes, and spread to other contiguous or distant organs. In this sense, the stages of colon cancer are the following:
- Stage 0: This is known as carcinoma in situ and is one in which the cancer has not spread beyond the inner mucous layer of the colon.
- Stage 1: The tumor process has penetrated into the submucosal layer or the muscle layer. However, it has not spread to nearby lymph nodes or tissues.
- Stage 2: The cancer has spread to the outermost layers of the colon. If it spreads without penetrating, it is called stage IIA, while if it perforates the colonic wall, it is considered stage IIB. On the other hand, stage IIC is when the lesion is fixed and grows in the adjacent tissues.
- Stage 3: Defined by the involvement of 1 to 7 lymph nodes contiguous to the affected tissue. In stage IIIA there is penetration of the submucosa and the muscle layer. On the other hand, stage IIIB is described by proliferation towards the outer layer, with or without penetration of the peritoneum, and stage IIIC is the result of growth in adjacent organs.
- Stage 4: The neoplastic lesion has spread to distant organs such as the liver and lung.
Differential diagnosis
The clinical manifestations of colon cancer, such as rectal bleeding, urgency, and changes in bowel habits can be caused by multiple diseases. For this reason, the treating physician must perform a correct examination supported by laboratory and imaging tests to rule out other conditions. Some of the differential diagnoses of colon cancer are as follows:
- Hemorrhoids
- Inflammatory bowel disease
- Appendicitis
- Irritable bowel syndrome
- Diverticulitis
- Infectious colitis
- Nephrolithiasis
Early cancer diagnosis increases survival rate
Colorectal neoplasms are common diseases in men over 50 years of age. However, the diagnosis of colon cancer in the early stages offers quite high expectations for a cure. In this sense, it’s recommended to carry out annual medical follow-up tests in people over 45 years of age, especially in those with risk factors.
Similarly, if you have abnormal bowel symptoms, bloody bowel movements, and fatigue, do not hesitate to seek medical attention as soon as possible. Specialist doctors are trained to take care of your condition and provide you with the best treatment options.
Colon cancer is the third most common neoplastic condition in men worldwide. In general, this pathology originates from polyps that form inside the large intestine. Early diagnosis of colon cancer is key to offering a better prognosis and a higher quality of life for those affected.
Currently, the American Cancer Society suggests colon cancer screening starting at age 45 in people at average risk. The digital rectal examination, colonoscopy, and stool examination are the most used methods for the identification of the classic signs of this pathology.
Clinical examination
A comprehensive clinical approach is vital for the diagnosis of early-stage colon cancer. In this sense, the treating physician will initiate the detection protocol from the questioning of the symptoms afflicting the patient. Changes in stool consistency, urgency, rectal bleeding, fatigue, and abdominal discomfort often guide the clinical diagnosis.
Similarly, medical history and family history are very useful in the prognosis of the state of health, as well as in the detection of possible risk factors for this intestinal condition. In this sense, age over 50 years, family or personal history of polyps, colorectal neoplasms, ulcerative colitis, and Crohn’s disease increase the probability of developing colon cancer.
The specialist doctor will carry out an adequate physical examination in search of any signs or anomalies suggestive of this condition. Palpation of the abdomen allows the identification of masses, painful areas, and enlarged viscera that allow a differential diagnosis of colon cancer to be established.
In addition, the digital rectal examination is one of the most used tests for the identification of colorectal alterations. It consists of the introduction of a gloved and lubricated finger through the anal orifice in search of structural abnormalities, secretions, or proliferations in the rectal epithelium.
Lab tests

Laboratory tests are indicated by the treating physician in order to obtain a broader picture of the general condition of the patient. Among the most used tests for the identification of the signs of colon cancer and the definitive diagnosis are the following.
Stool examination
Studies of fecal samples provide information about the macroscopic and microscopic characteristics of the intestinal contents. Studies affirm that the detection of occult blood in feces is very useful in the investigation and initial diagnosis of the condition. The bleeding is usually the result of the rupture of the blood vessels near the polyps or tumor lesions.
The Fecal Immunochemical Test (FIT) can easily detect occult blood by reacting with the hemoglobin contained in fecal material. Similarly, the guaiac-based fecal occult blood test (gFOBT) uses a chemical reaction to identify red blood cells in the stool.
On the other hand, the multidirectional stool DNA test or MT-sDNA allows the identification of abnormal DNA from cancer cells that proliferate in the colon and rectum. It is recommended every 3 years in patients at high risk of colon cancer.
In case the samples are positive for occult blood in the stool, a confirmatory colonoscopy is necessary. This sign can be positive not only in colon cancer and polyps, but also in patients with ulcers and hemorrhoids, so the interior of the large intestine should be observed to identify the origin of the bleeding.
Blood test
The complete blood count provides detailed information on the red blood cell, white blood cell, and platelet count, as well as the size and concentration characteristics of the hemoglobin in the red blood cells.
Hypochromic microcytic anemia (ie, small, “pale” red blood cells) is common in people with colon cancer as a result of blood loss and destruction of red blood cells by the tumor.
On the other hand, white blood cells may be elevated, which is called leukocytosis, in response to necrosis (tissue death) and tumor invasion. Furthermore, liver metastasis and septic complications in affected people are also associated with this sign.
Tumor marker detection
In some cases, tumor cells are capable of producing and releasing certain substances or markers into the bloodstream that can be identified by serological tests. Studies confirm that carcinoembryonic antigen (CEA) is expressed in more than 90% of colorectal neoplasms. In fact, it is the most widely used biomarker in the diagnosis of colon cancer.
CEA generally remains below 2.5 nanograms per milliliter in nonsmoking patients. Colon adenocarcinoma is the main responsible for the elevation of this tumor marker. Similarly, it can be elevated in other types of colorectal neoplasms or in breast, gastrointestinal, lung, thyroid, and pancreatic cancer.
The carbohydrate antigen 19-9 (CA 19-9) is another of the substances linked to colon cancer, whose normal levels are below 37 units per milliliter. CA 19-9 values are related to CEA values in the follow-up of people diagnosed who are under treatment. In addition, they show great sensitivity in detecting metastasis to other organs.
Liver function test
Usually, late-stage colon neoplasms can spread to liver tissue. For this reason, the specialist may order a blood test to assess the status of the liver. In this sense, it’s common to show an alteration of total and fractionated proteins, especially in those who suffer from localized liver metastasis or recurrence.
Biopsy
This test consists of the extraction of a sample of the affected tissue for its subsequent microscopic and histopathological study. Research affirms that the biopsy is the standard confirmatory test in the diagnosis of colon cancer. It is requested when there is clinical suspicion or when there is evidence by an imaging study of an abnormal mass in the large intestine.
On the other hand, it’s very useful in the classification of colon neoplasms based on the cellular characteristics and the degree of differentiation of the tissue. It also makes it possible to determine the severity of the disease, deduce the patient’s prognosis, and implement the most effective treatment.
Imaging tests
Imaging studies allow a more detailed view of the general state of internal organs to be obtained. They are used in patients with suspected colon cancer in search of abnormal lesions or proliferations suggestive of malignancy. Some of the imaging tests used are the following:
Colonoscopy
Colonoscopy is one of the most widely used imaging methods in the early diagnosis of colon cancer. It consists of the introduction of a thin and flexible tube with a camera at its end through the anal opening. In this way, it is possible to explore the inside of the rectum and anus in its entirety, verifying if there are tumors or polyps that could evolve into cancer.
In addition, this procedure allows the introduction of special instruments for taking the biopsy sample. It also offers the possibility of removing any small lesions with potential malignancy if necessary.
CT colonography
Computed tomography (CT) colonography allows the colonic structure to be visualized through special cuts made by an X-ray machine. During this test, a small tube is inserted through the anal opening, which will be inflated with gas to obtain a more detailed image of the rectum and colon.
Flexible sigmoidoscopy
Sigmoidoscopy is an endoscopic method that allows exploration of the inside of the rectum and sigmoid colon. This test generally requires less preparation, and, in some people, anesthesia is not necessary. In case of polyps or any other lesion suggestive of cancer, a colonoscopy will be indicated to evaluate the rest of the large intestine.
Magnetic resonance
Magnetic resonance imaging (MRI) is useful in the non-invasive assessment of soft tissues and in the detection of tumor processes. In some cases, a contrast medium may be administered parenterally before starting the procedure. It facilitates the detection of metastatic spread of cancer to the liver, brain, and spinal cord.
On the other hand, endorectal MRI is used in the diagnosis of colon cancer spread to adjacent organs or tissues. Unlike traditional MRI, this uses a small probe that will remain in the rectum during the study. In addition, it is used in the planning of surgical or chemotherapy treatment of affected people.
Colon cancer staging

The large intestine is lined by an inner layer or mucosa, which is the area where most cancerous lesions usually start. Similarly, it has a submucosal layer and a muscular layer just below the mucosa. On the other hand, the subserous and serous layers cover the external face of most of the colon, with the exception of the rectal tissue.
How is staging done?
Currently, the staging of colorectal neoplasms is based on the system established by the American Joint Committee on Cancer (AJCC). It considers the extent and size of the tumor, spread to lymph nodes, and spread to other contiguous or distant organs. In this sense, the stages of colon cancer are the following:
- Stage 0: This is known as carcinoma in situ and is one in which the cancer has not spread beyond the inner mucous layer of the colon.
- Stage 1: The tumor process has penetrated into the submucosal layer or the muscle layer. However, it has not spread to nearby lymph nodes or tissues.
- Stage 2: The cancer has spread to the outermost layers of the colon. If it spreads without penetrating, it is called stage IIA, while if it perforates the colonic wall, it is considered stage IIB. On the other hand, stage IIC is when the lesion is fixed and grows in the adjacent tissues.
- Stage 3: Defined by the involvement of 1 to 7 lymph nodes contiguous to the affected tissue. In stage IIIA there is penetration of the submucosa and the muscle layer. On the other hand, stage IIIB is described by proliferation towards the outer layer, with or without penetration of the peritoneum, and stage IIIC is the result of growth in adjacent organs.
- Stage 4: The neoplastic lesion has spread to distant organs such as the liver and lung.
Differential diagnosis
The clinical manifestations of colon cancer, such as rectal bleeding, urgency, and changes in bowel habits can be caused by multiple diseases. For this reason, the treating physician must perform a correct examination supported by laboratory and imaging tests to rule out other conditions. Some of the differential diagnoses of colon cancer are as follows:
- Hemorrhoids
- Inflammatory bowel disease
- Appendicitis
- Irritable bowel syndrome
- Diverticulitis
- Infectious colitis
- Nephrolithiasis
Early cancer diagnosis increases survival rate
Colorectal neoplasms are common diseases in men over 50 years of age. However, the diagnosis of colon cancer in the early stages offers quite high expectations for a cure. In this sense, it’s recommended to carry out annual medical follow-up tests in people over 45 years of age, especially in those with risk factors.
Similarly, if you have abnormal bowel symptoms, bloody bowel movements, and fatigue, do not hesitate to seek medical attention as soon as possible. Specialist doctors are trained to take care of your condition and provide you with the best treatment options.
- Rodríguez Fernández Z, Jean-Louis B, Lozada Prado G, Joubert Álvarez G, Pineda Chacón J. Conocimientos vigentes acerca del cáncer de colon recurrente. MEDISAN. 2015; 19(6): 797-814.
- Recio-Boiles A, Cagir B. Cáncer de colon. En: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2021 enero-.
- Menéndez-Sánchez P, Villarejo-Campos P, Menéndez-Rubio J, Rodríguez-Montes J et al. Marcadores tumorales en el cáncer colorrectal. Cirugía y Cirujanos. 2013;81(2):169-175.
- Oh K, Han K, Kim E, Lee J et al. Colon Cancer After Acute Diverticulitis Treatment. Annals of Coloproctology. 2013;29(4):167.
- Dienstmann R, Mason M, Sinicrope F, Phipps A et al. Prediction of overall survival in stage II and III colon cancer beyond TNM system: a retrospective, pooled biomarker study. Annals of Oncology. 2017;28(5):1023-1031.
- Teng A, Nelson DW, Dehal A, Chang SC et al. Colon cancer as a subsequent malignant neoplasm in young adults. Cancer. 2019;125(21):3749-3754.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







