All About the Diagnosis of Ulcerative Colitis

The diagnosis of ulcerative colitis is carried out using different conclusions based on laboratory and other tests. There’s no single and 100 percent effective test for its detection, but the sum of several elements allows the specialist to give a sure diagnosis. Since its symptoms are general, other gastrointestinal conditions are ruled out during the process.
An early diagnosis is very important. Ulcerative colitis is a chronic disorder that worsens over time. If it isn’t treated properly, then it can cause considerable complications in patients. Today, we’ll show you the protocol used to determine its presence.
Laboratory tests for the diagnosis of ulcerative colitis
The first step in the diagnosis of ulcerative colitis is to carry out a general assessment of the patient, as Crohn’s & Colitis Foundation reminds us. The doctor will take into account your experience in recent months, symptoms, habits, medical history, and family history, among other things.
They will also carry out an evaluation for abdominal swelling, mouth ulcers, and other extraintestinal manifestations. Based on this, you can rule out various hypotheses. For added security, a doctor will proceed with the following laboratory tests:
Stool analysis
Although it cannot diagnose ulcerative colitis, it is very useful in ruling out bacterial or viral explanations. According to Crohn’s & Colitis UK, it’s less effective in those under 18 and over 60. In this way, it’s a more useful test to carry out between 20 and 50 years of age.
Researchers agree that fecal calprotectin, lactoferrin, elastase, and S100A12 are the best candidates for detecting inflammation in the large intestine. These markers will alert doctors that the colon has been affected and will be the starting point before performing a colonoscopy (see below).
Blood test
As in the previous case, this isn’t capable of diagnosing ulcerative colitis on its own. Its goal is to find some common markers in the disease. For example, the inflammatory process in the colon usually unbalances the absorption of nutrients. This can lead to iron deficiency anemia and other similar types of decompensation.
Evidence also suggests that C-reactive protein levels and erythrocyte sedimentation can be used as markers. At the same time, blood tests will help to rule out other conditions.
Special research for the diagnosis of ulcerative colitis
The tests we’ve already mentioned are the starting point. The next thing is to confirm the suspicions with the help of more specific tests. Those preferred by specialists are the following:
Colonoscopy
As Stanford Health Care points out, colonoscopy is the gold standard during the diagnosis of ulcerative colitis. With its help, the professional can see the state of the walls of the large intestine, examining its entire length to check the level of deterioration.
They will look for evidence of inflammation and ulcers at the edges. Dead tissue is also likely to be removed for laboratory testing (biopsy). The process is carried out under sedation, so you shouldn’t experience any discomfort during it.
Sigmoidoscopy
This is similar to the previous one, only less invasive. Sigmoidoscopy allows you to visualize the state of the rectum and the part of the colon closest to it (sigmoid). Most episodes of ulcerative colitis begin in the rectum (proctitis) before spreading to the left side of the colon (proctosigmoiditis), and will eventually encompass the entire large intestine (pancolitis).
If symptoms are very recent or previous laboratory tests indicate minor damage, the specialist may opt for sigmoidoscopy alone. Despite this, it isn’t considered the standard test, as thus the disorder can sometimes develop in other parts of the large intestine. This is why colonoscopy is the best option.
Endoscopy
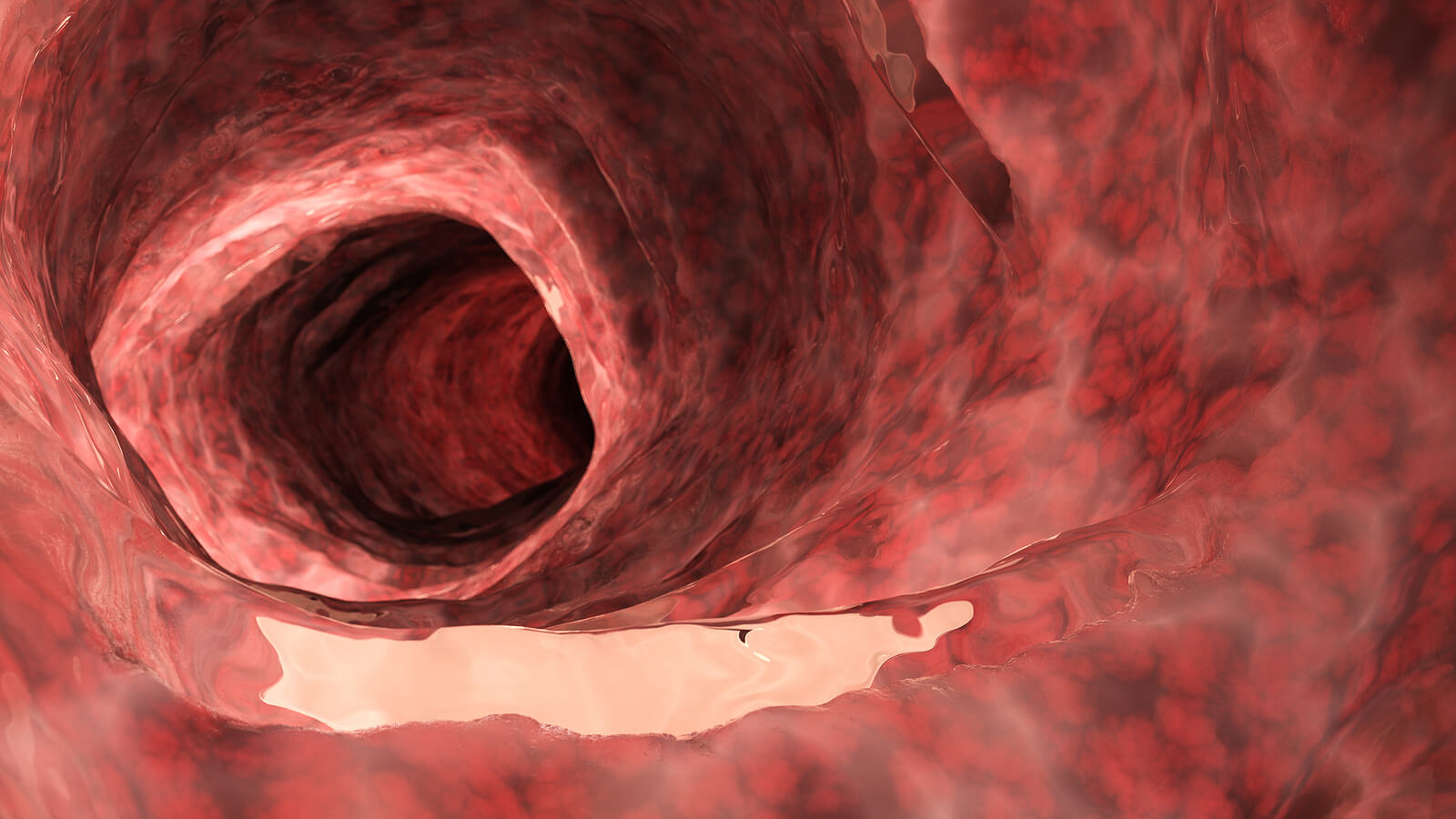
If the specialist hasn’t found signs that point to ulcerative colitis, they can perform an endoscopy. It isn’t useful in detecting the disease itself, but it’s used to rule out other gastrointestinal complications that are causing the symptoms. Sometimes tissue can be removed for laboratory testing (biopsy).
In some settings, other imaging tests are necessary. The researchers suggest using x-rays to rule out toxic megacolon. Barium enema, enterography, and capsule endoscopy are also available.
Differential diagnosis of ulcerative colitis
Dozens of complications and diseases can explain the appearance of symptoms, apart from ulcerative colitis. Stanford Medicine recommends ruling out bacterial, fungal, and parasitic infections first. Other differential diagnoses of ulcerative colitis include the following:
- Crohn’s disease: Crohn’s disease is very similar to this disorder; in fact, both are the two possible manifestations of inflammatory bowel disease (IBD). It’s more common in young people than in adults.
- Ischemic colitis: This occurs when the blood flow that radiates to the large intestine is reduced. It usually develops the same symptoms as ulcerative colitis, although this time its prevalence is higher in adults over 60 years of age.
- Microscopic colitis: This is a variant that develops after the age of 50. It’s characterized by the same signs and symptoms, except for the presence of blood in the stools.
Although these manifestations have a very similar clinical picture, in reality their treatment is different. This is why it’s so important to rule it out during the diagnosis of ulcerative colitis, thus avoiding starting a treatment that won’t be effective in counteracting the real cause.
Remember that the disorder has no cure, but it can be controlled with the help of pharmacological therapies. If you have an autoimmune disease, a history of the condition in your family or have experienced its symptoms, don’t hesitate to seek medical assistance.
The diagnosis of ulcerative colitis is carried out using different conclusions based on laboratory and other tests. There’s no single and 100 percent effective test for its detection, but the sum of several elements allows the specialist to give a sure diagnosis. Since its symptoms are general, other gastrointestinal conditions are ruled out during the process.
An early diagnosis is very important. Ulcerative colitis is a chronic disorder that worsens over time. If it isn’t treated properly, then it can cause considerable complications in patients. Today, we’ll show you the protocol used to determine its presence.
Laboratory tests for the diagnosis of ulcerative colitis
The first step in the diagnosis of ulcerative colitis is to carry out a general assessment of the patient, as Crohn’s & Colitis Foundation reminds us. The doctor will take into account your experience in recent months, symptoms, habits, medical history, and family history, among other things.
They will also carry out an evaluation for abdominal swelling, mouth ulcers, and other extraintestinal manifestations. Based on this, you can rule out various hypotheses. For added security, a doctor will proceed with the following laboratory tests:
Stool analysis

Although it cannot diagnose ulcerative colitis, it is very useful in ruling out bacterial or viral explanations. According to Crohn’s & Colitis UK, it’s less effective in those under 18 and over 60. In this way, it’s a more useful test to carry out between 20 and 50 years of age.
Researchers agree that fecal calprotectin, lactoferrin, elastase, and S100A12 are the best candidates for detecting inflammation in the large intestine. These markers will alert doctors that the colon has been affected and will be the starting point before performing a colonoscopy (see below).
Blood test
As in the previous case, this isn’t capable of diagnosing ulcerative colitis on its own. Its goal is to find some common markers in the disease. For example, the inflammatory process in the colon usually unbalances the absorption of nutrients. This can lead to iron deficiency anemia and other similar types of decompensation.
Evidence also suggests that C-reactive protein levels and erythrocyte sedimentation can be used as markers. At the same time, blood tests will help to rule out other conditions.
Special research for the diagnosis of ulcerative colitis
The tests we’ve already mentioned are the starting point. The next thing is to confirm the suspicions with the help of more specific tests. Those preferred by specialists are the following:
Colonoscopy
As Stanford Health Care points out, colonoscopy is the gold standard during the diagnosis of ulcerative colitis. With its help, the professional can see the state of the walls of the large intestine, examining its entire length to check the level of deterioration.
They will look for evidence of inflammation and ulcers at the edges. Dead tissue is also likely to be removed for laboratory testing (biopsy). The process is carried out under sedation, so you shouldn’t experience any discomfort during it.
Sigmoidoscopy
This is similar to the previous one, only less invasive. Sigmoidoscopy allows you to visualize the state of the rectum and the part of the colon closest to it (sigmoid). Most episodes of ulcerative colitis begin in the rectum (proctitis) before spreading to the left side of the colon (proctosigmoiditis), and will eventually encompass the entire large intestine (pancolitis).
If symptoms are very recent or previous laboratory tests indicate minor damage, the specialist may opt for sigmoidoscopy alone. Despite this, it isn’t considered the standard test, as thus the disorder can sometimes develop in other parts of the large intestine. This is why colonoscopy is the best option.
Endoscopy

If the specialist hasn’t found signs that point to ulcerative colitis, they can perform an endoscopy. It isn’t useful in detecting the disease itself, but it’s used to rule out other gastrointestinal complications that are causing the symptoms. Sometimes tissue can be removed for laboratory testing (biopsy).
In some settings, other imaging tests are necessary. The researchers suggest using x-rays to rule out toxic megacolon. Barium enema, enterography, and capsule endoscopy are also available.
Differential diagnosis of ulcerative colitis
Dozens of complications and diseases can explain the appearance of symptoms, apart from ulcerative colitis. Stanford Medicine recommends ruling out bacterial, fungal, and parasitic infections first. Other differential diagnoses of ulcerative colitis include the following:
- Crohn’s disease: Crohn’s disease is very similar to this disorder; in fact, both are the two possible manifestations of inflammatory bowel disease (IBD). It’s more common in young people than in adults.
- Ischemic colitis: This occurs when the blood flow that radiates to the large intestine is reduced. It usually develops the same symptoms as ulcerative colitis, although this time its prevalence is higher in adults over 60 years of age.
- Microscopic colitis: This is a variant that develops after the age of 50. It’s characterized by the same signs and symptoms, except for the presence of blood in the stools.
Although these manifestations have a very similar clinical picture, in reality their treatment is different. This is why it’s so important to rule it out during the diagnosis of ulcerative colitis, thus avoiding starting a treatment that won’t be effective in counteracting the real cause.
Remember that the disorder has no cure, but it can be controlled with the help of pharmacological therapies. If you have an autoimmune disease, a history of the condition in your family or have experienced its symptoms, don’t hesitate to seek medical assistance.
- Collins, P., & Rhodes, J. Ulcerative colitis: diagnosis and management. Bmj. 2006; 333(7563): 340-343.
- Dignass A, Eliakim R, Magro F, Maaser C, Chowers Y, Geboes K, Mantzaris G, Reinisch W, Colombel JF, Vermeire S, Travis S, Lindsay JO, Van Assche G. Second European evidence-based consensus on the diagnosis and management of ulcerative colitis part 1: definitions and diagnosis. J Crohns Colitis. 2012 Dec;6(10):965-90.
- Turner D, Mack DR, Hyams J, LeLeiko N, Otley A, Markowitz J, Kasirer Y, Muise A, Seow CH, Silverberg MS, Crandall W, Griffiths AM. C-reactive protein (CRP), erythrocyte sedimentation rate (ESR) or both? A systematic evaluation in pediatric ulcerative colitis. J Crohns Colitis. 2011 Oct;5(5):423-9.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







