Skin Changes After 50

As we age, our organs change. In fact, skin changes after 50 are considered the main visible sign of aging (along with whitening hair). This is a natural consequence, one that can be greater or lesser according to different variables. Exposure to the sun, an unhealthy diet, bad habits, and genetic factors all play a role.
The skin is made up of three layers: The outer layer (the epidermis), the middle layer (the dermis), and the inner layer (subcutaneous). Skin changes after 50 affect each of these layers and not just the outer one. Such changes expose people to skin lesions, decreased sensitivity to touch, and delayed healing. Let’s see what scientists have to say.
The main skin changes after 50
Skin changes after 50 develop gradually. We notice them with the passing of the years, meaning that their manifestations don’t occur in just a matter of days.
The presence of underlying disorders can speed up the process. Indeed, people with diabetes, liver disease, heart disease, blood vessel disease, obesity, and stress can manifest much greater changes.
Apart from all this, the main catalyst for skin aging after the age of 50 is exposure to sunlight. In fact, and as the experts point out, photoaging can advance the manifestation of changes in the skin as a result of age. With these reflections as an introduction, we’ll leave you with the most common ones and their characteristics.
1. Dry itchy skin
The skin reduces oil production over time as it ages. The sebaceous glands are responsible for it, and it’s what helps the skin to stay hydrated. Oil reduction is gradual, although in women it accelerates immediately after menopause. In men, it’s much slower, as it doesn’t manifest itself until after the age of 70.
This is known as xeroderma or xerosis, and is almost always accompanied by itching. The appearance of the skin takes on a scaly texture in the absence of hydration.
As the researchers point out, this increases the chances of irritants and allergens entering the skin. It’s often a condition that’s ignored or at least not given the importance it deserves.
2. Wrinkles on the surface
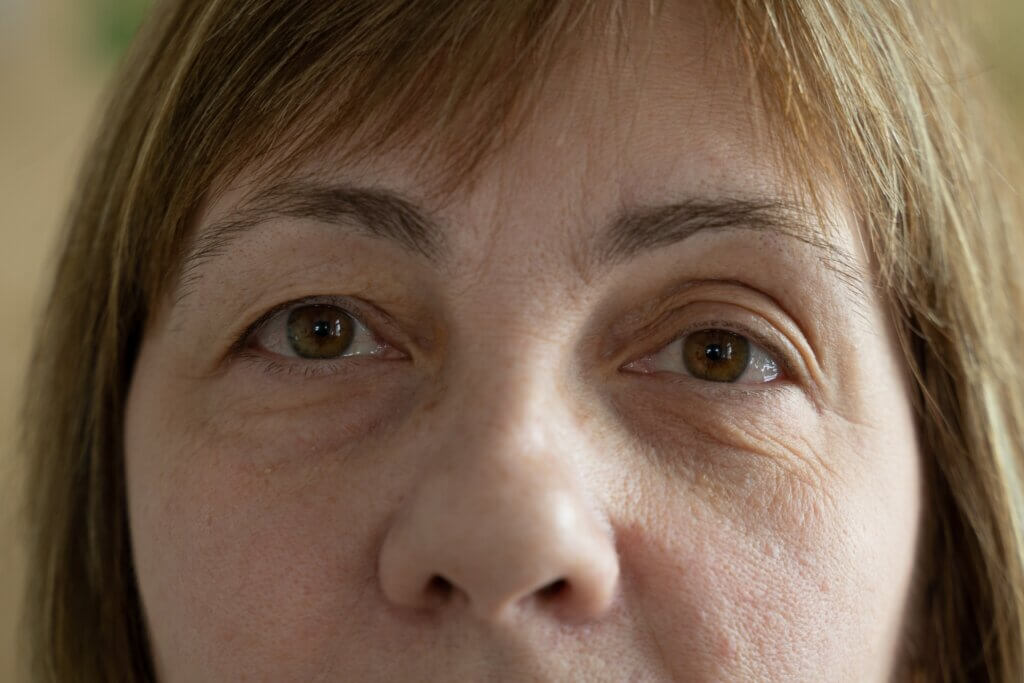
Undoubtedly one of the most feared changes in the skin after the age of 50 is the appearance of wrinkles on the surface. Specialists distinguish between two types: Fine wrinkles (less than 1 millimeter wide) and thick wrinkles (more than 1 millimeter wide). They occur on almost the entire surface of the skin, although they’re most common on the face, hands, and forearms.
3. Age spots
These are also known as liver spots, lentigo seniles, or solar lentigo. They’re light brown or black pigmented lesions of various sizes. They can be as small as a few millimeters or as long as several centimeters, and are most common on the surface of skin that’s regularly exposed to the sun (the face, arms, and neck, for example).
As the researchers warn, its etiology is still not fully understood, although we know that hyperactive pigment cells are behind it. Sometimes age spots can group together, giving the impression that it’s a single or very large spot. They’re more noticeable in people with very white skin.
4. Thinning of the skin
Although the number of cell layers doesn’t change over time, the first layer of the skin (the epidermis) suffers from thinning. As a consequence, the number of pigment-containing cells is reduced, giving the sensation of translucent, clear, and pale skin. This is one of the most noticeable skin changes after 50, and one that’s more common in women.
This is because a good part of its manifestation has a hormonal basis, meaning that women develop it more intensely as a result of menopause. In these cases, and following the evidence, hormone replacement therapy can help to recover the thickness of the skin. Being the thinnest skin, it can break more easily against friction with objects.
5. Loss of fat under the skin
As the researchers point out, the thickness of the skin decreases an average of 6.4% per decade. Much of the reduction in this thickness has to do with the loss of fat that surrounds its layers.
As a person ages, their muscle mass also decreases, which also has a direct impact on the appearance of the skin after the age of 50. This can look less smooth, and more malleable and loose.
6. The development of benign tumors
This is the case of seborrheic keratoses. Experts agree that they’re the most common benign skin tumor worldwide, and that their incidence increases with age and sun exposure. They’re more common on the face (on the forehead, in particular) and on the trunk of the body. Their size varies, although in no case do they exceed 4 centimeters.
7. Bruises and prolonged scarring
Lastly, and as the National Institute on Aging reminds us, bruises and prolonged scarring are a frequent skin manifestation after the age of 50.
The presence of bruises from blows is maximized, and wounds can take up to four times longer to heal. As we’ve already warned, certain underlying diseases can enhance this and other changes.
All of these consequences are natural, and in practice, you can do very little to avoid them. Reducing prolonged sun exposure, maintaining a healthy diet, drinking plenty of water, getting regular exercise, and managing diagnosed illnesses can make a big difference. If you’re concerned about any manifestation, be sure to consult a dermatologist.
As we age, our organs change. In fact, skin changes after 50 are considered the main visible sign of aging (along with whitening hair). This is a natural consequence, one that can be greater or lesser according to different variables. Exposure to the sun, an unhealthy diet, bad habits, and genetic factors all play a role.
The skin is made up of three layers: The outer layer (the epidermis), the middle layer (the dermis), and the inner layer (subcutaneous). Skin changes after 50 affect each of these layers and not just the outer one. Such changes expose people to skin lesions, decreased sensitivity to touch, and delayed healing. Let’s see what scientists have to say.
The main skin changes after 50
Skin changes after 50 develop gradually. We notice them with the passing of the years, meaning that their manifestations don’t occur in just a matter of days.
The presence of underlying disorders can speed up the process. Indeed, people with diabetes, liver disease, heart disease, blood vessel disease, obesity, and stress can manifest much greater changes.
Apart from all this, the main catalyst for skin aging after the age of 50 is exposure to sunlight. In fact, and as the experts point out, photoaging can advance the manifestation of changes in the skin as a result of age. With these reflections as an introduction, we’ll leave you with the most common ones and their characteristics.
1. Dry itchy skin
The skin reduces oil production over time as it ages. The sebaceous glands are responsible for it, and it’s what helps the skin to stay hydrated. Oil reduction is gradual, although in women it accelerates immediately after menopause. In men, it’s much slower, as it doesn’t manifest itself until after the age of 70.
This is known as xeroderma or xerosis, and is almost always accompanied by itching. The appearance of the skin takes on a scaly texture in the absence of hydration.
As the researchers point out, this increases the chances of irritants and allergens entering the skin. It’s often a condition that’s ignored or at least not given the importance it deserves.
2. Wrinkles on the surface

Undoubtedly one of the most feared changes in the skin after the age of 50 is the appearance of wrinkles on the surface. Specialists distinguish between two types: Fine wrinkles (less than 1 millimeter wide) and thick wrinkles (more than 1 millimeter wide). They occur on almost the entire surface of the skin, although they’re most common on the face, hands, and forearms.
3. Age spots
These are also known as liver spots, lentigo seniles, or solar lentigo. They’re light brown or black pigmented lesions of various sizes. They can be as small as a few millimeters or as long as several centimeters, and are most common on the surface of skin that’s regularly exposed to the sun (the face, arms, and neck, for example).
As the researchers warn, its etiology is still not fully understood, although we know that hyperactive pigment cells are behind it. Sometimes age spots can group together, giving the impression that it’s a single or very large spot. They’re more noticeable in people with very white skin.
4. Thinning of the skin
Although the number of cell layers doesn’t change over time, the first layer of the skin (the epidermis) suffers from thinning. As a consequence, the number of pigment-containing cells is reduced, giving the sensation of translucent, clear, and pale skin. This is one of the most noticeable skin changes after 50, and one that’s more common in women.
This is because a good part of its manifestation has a hormonal basis, meaning that women develop it more intensely as a result of menopause. In these cases, and following the evidence, hormone replacement therapy can help to recover the thickness of the skin. Being the thinnest skin, it can break more easily against friction with objects.
5. Loss of fat under the skin

As the researchers point out, the thickness of the skin decreases an average of 6.4% per decade. Much of the reduction in this thickness has to do with the loss of fat that surrounds its layers.
As a person ages, their muscle mass also decreases, which also has a direct impact on the appearance of the skin after the age of 50. This can look less smooth, and more malleable and loose.
6. The development of benign tumors
This is the case of seborrheic keratoses. Experts agree that they’re the most common benign skin tumor worldwide, and that their incidence increases with age and sun exposure. They’re more common on the face (on the forehead, in particular) and on the trunk of the body. Their size varies, although in no case do they exceed 4 centimeters.
7. Bruises and prolonged scarring
Lastly, and as the National Institute on Aging reminds us, bruises and prolonged scarring are a frequent skin manifestation after the age of 50.
The presence of bruises from blows is maximized, and wounds can take up to four times longer to heal. As we’ve already warned, certain underlying diseases can enhance this and other changes.
All of these consequences are natural, and in practice, you can do very little to avoid them. Reducing prolonged sun exposure, maintaining a healthy diet, drinking plenty of water, getting regular exercise, and managing diagnosed illnesses can make a big difference. If you’re concerned about any manifestation, be sure to consult a dermatologist.
- Choi W, Yin L, Smuda C, Batzer J, Hearing VJ, Kolbe L. Molecular and histological characterization of age spots. Exp Dermatol. 2017;26(3):242-248.
- Farage MA, Miller KW, Elsner P, Maibach HI. Characteristics of the Aging Skin. Adv Wound Care (New Rochelle). 2013;2(1):5-10.
- Garibyan L, Chiou AS, Elmariah SB. Advanced aging skin and itch: addressing an unmet need. Dermatol Ther. 2013;26(2):92-103.
- Manríquez JJ, Cataldo K, Vera-Kellet C, Harz-Fresno I. Wrinkles. BMJ Clin Evid. 2014;2014:1711.
- Majidian M, Kolli H, Moy RL. Management of skin thinning and aging: review of therapies for neocollagenesis; hormones and energy devices. Int J Dermatol. 2021 Dec;60(12):1481-1487.
- Rittié L, Fisher GJ. Natural and sun-induced aging of human skin. Cold Spring Harb Perspect Med. 2015;5(1):a015370. Published 2015 Jan 5.
- Wollina U. Seborrheic Keratoses – The Most Common Benign Skin Tumor of Humans. Clinical presentation and an update on pathogenesis and treatment options. Open Access Maced J Med Sci. 2018;6(11):2270-2275.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







