What Is Dyspepsia?

Dyspepsia is one of the most frequent reasons for an appointment with a gastroenterologist. Its a set of symptoms characterized by gastrointestinal discomfort, usually associated with the consumption of food.
Despite its high prevalence, in very few cases do doctors reach a specific diagnosis to explain the cause. If you’re interested in knowing the reasons for this, we have prepared the following article on the most important characteristics of this condition. Keep reading!
Dyspepsia: symptom or disease?

It is a set of diverse and nonspecific gastrointestinal symptoms that sometimes occur as a consequence of a pre-existing disease. For this reason, dyspepsia can’t be considered a disease, but, rather, the result of various pathophysiological alterations.
From a clinical point of view, it usually affects the central and upper region of the abdomen, known as the epigastrium. The sensations can be multiple, including pain and burning. Some general symptoms such as bloating, nausea, vomiting, and fullness after eating small amounts of food are also common.
According to this scientific review article (2014), dyspepsia can reach prevalence figures of up to 24%, despite the fact that many patients avoid medical consultation and prefer self-medication with over-the-counter drugs. Therefore, these latter cases are not recorded.
Classification of dyspepsia
This can be divided into two types: functional and organic. The first occurs in the absence of an illness, while in the second there is an obvious cause. Next, we’ll describe the particularities of each one.
Functional
This type of dyspepsia is one that isn’t related to important organic pathologies, such as peptic ulcers. To reach the diagnosis, the doctor could resort to several complementary studies that we’ll talk about later.
Although the exhaustive search for diseases doesn’t give any results in functional dyspepsia, it’s logical to think that there’s some pathophysiological cause behind the symptoms. For years, this seemed to be a mystery, until this meta-analysis (2018) was published.
To carry out this study, the authors reviewed 37 high-quality publications in which some microscopic findings were published in the gastric and duodenal mucosa of patients with functional dyspepsia.
Through various statistical methods, they came to the conclusion that the mechanism involved is the appearance of micro-inflammatory phenomena, with an abundance of eosinophils and mast cells.
For practical and economic reasons, these types of procedures aren’t performed routinely. Doctors, once they rule out the presence of important pathologies, usually indicate prolonged treatment to reduce or eliminate symptoms.
Organic
In this case, the symptoms are the result of a certain health condition. Each has its own diagnostic methods, and the most important causes are the following:
- Peptic ulcer: This is a condition characterized by the appearance of excavated lesions in the gastric or duodenal mucosa. It usually causes intense pain and burning. In some patients, it may be the cause of gastrointestinal bleeding.
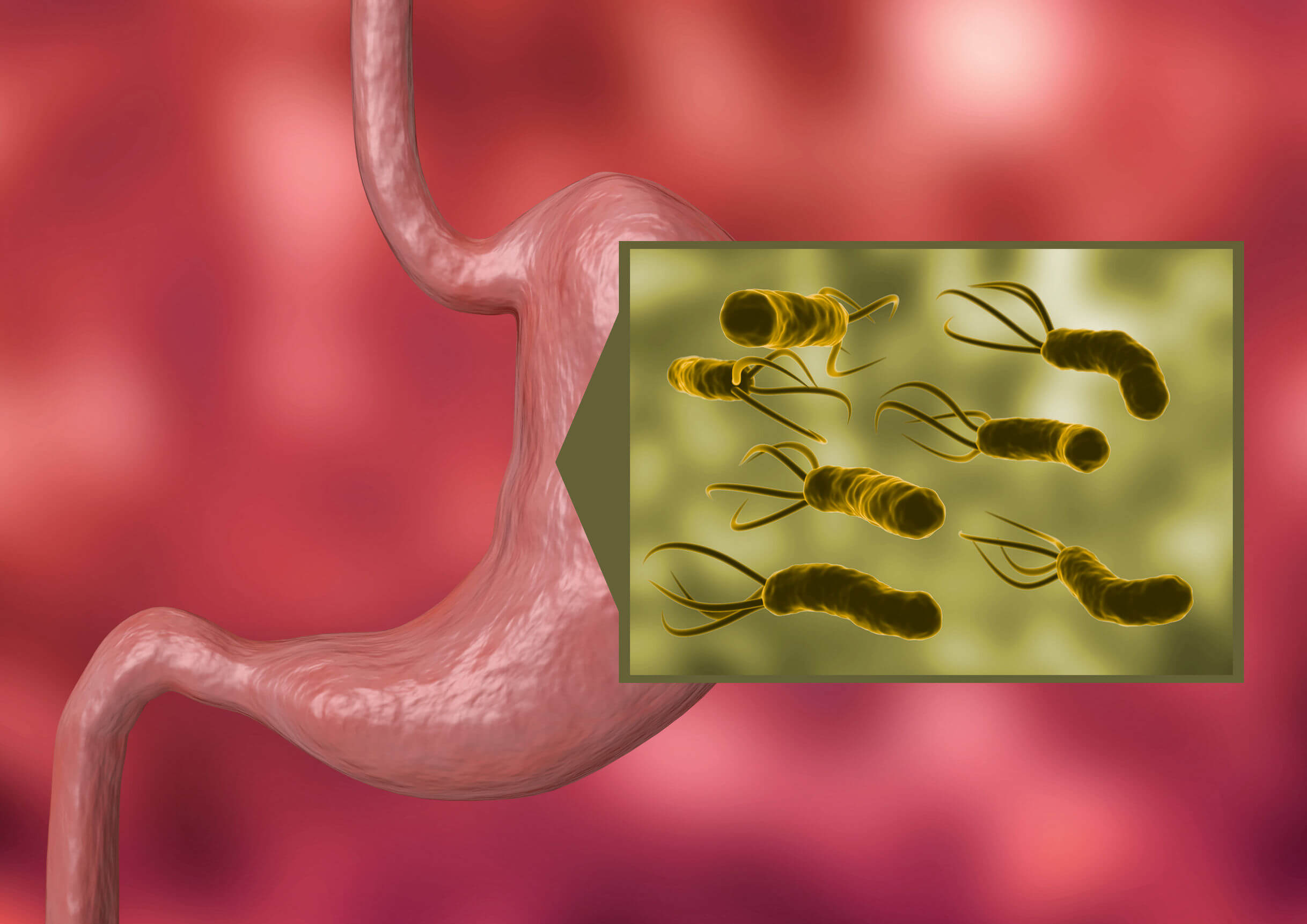
- Helicobacter pylori infection: This bacterium is responsible for many cases of chronic gastritis. Although in most cases the clinical picture is limited to dyspepsia, in some patients it could evolve to produce gastric cancer.
- Gallstones: This is a very common condition in which there’s an accumulation of hardened substances within the lumen of the gallbladder or bile ducts. When an associated infection occurs, it’s called cholecystitis or cholangitis.
- Pancreatic or gastric cancer: Both conditions have a poor prognosis, especially because their diagnosis is usually late. Some warning symptoms are digestive bleeding and unexplained weight loss.
Other much less common causes include chronic pancreatitis, some metabolic disorders, and poorly controlled diabetes mellitus. In the latter case, dyspepsia is a consequence of nerve damage due to persistent elevation of blood glucose (diabetic neuropathy).
Diagnosis
As we mentioned before, dyspepsia isn’t a disease. Therefore, at first, the diagnosis seems obvious. However, the real importance of going to the doctor lies in determining the origin of the symptoms.
For this reason, the goal of the gastroenterologist is to determine if it’s a case of functional or organic dyspepsia. For this reason, patients are usually differentiated according to the probability that they have functional dyspepsia. The use of clinical rating scales allows specialists to determine this probability.
If the doctor suspects the existence of a previous pathology that explains the symptoms, he could resort to several different studies to make the diagnosis.
Complementary studies
The most effective method is an upper gastrointestinal endoscopy. This technique is based on the introduction of a flexible tube connected to a high-resolution camera, which can be introduced (after sedation) through the patient’s mouth.
This allows the correct visualization of gastrointestinal structures, in addition to allowing the specialists to perform biopsies in places of interest.
There are less specific methods but ones that still help when making the diagnosis, such as the following:
- A complete blood count
- Abdominal echography
- Detection of H. pylori through serological studies and the determination of antigens in feces, among other tests.
Treatment
Like many other gastrointestinal disorders, dyspepsia can be treated by changing some eating and behavioral patterns. When necessary, the use of drugs is also possible.
Diet and lifestyle changes
This is usually the first recommendation that doctors make. According to a publication from the Mayo Clinic, the main recommendations are the following:
- Avoid skipping meals
- Reduce the consumption of tobacco, coffee, and alcohol.
- Do not eat large meals
- Decrease the amount of food and increase the frequency of meals
- Chew and swallow slowly and deliberately
Although these changes can provide symptomatic relief, there are frequent cases where you won’t get complete relief. In these patients, pharmacological treatment is recommended.
Drugs
If it is a case of secondary or organic dyspepsia, treatment is directed to the cause of the symptoms. For example, to achieve the elimination of H. pylori, doctors often prescribe omeprazole, clarithromycin, and amoxicillin.
In cases of functional dyspepsia, one of the following drugs may be recommended:
- Proton pump inhibitors: These decrease gastric acid secretion, and an example is omeprazole.
- Prokinetics: Promotes gastric emptying and prevents gastroesophageal reflux. This group includes metoclopramide, domperidone, and cinitapride.
- Psychopharmaceuticals: These are useful only when there is an associated psychiatric component.
Living with dyspepsia: when do you need to go to the doctor?
When symptoms are severe or recur too frequently, it’s advisable to go to the gastroenterologist. Depending on the context, they could request more studies to determine the origin of the dyspepsia, although in many cases there’s no clear illness.
Dyspepsia is one of the most frequent reasons for an appointment with a gastroenterologist. Its a set of symptoms characterized by gastrointestinal discomfort, usually associated with the consumption of food.
Despite its high prevalence, in very few cases do doctors reach a specific diagnosis to explain the cause. If you’re interested in knowing the reasons for this, we have prepared the following article on the most important characteristics of this condition. Keep reading!
Dyspepsia: symptom or disease?

It is a set of diverse and nonspecific gastrointestinal symptoms that sometimes occur as a consequence of a pre-existing disease. For this reason, dyspepsia can’t be considered a disease, but, rather, the result of various pathophysiological alterations.
From a clinical point of view, it usually affects the central and upper region of the abdomen, known as the epigastrium. The sensations can be multiple, including pain and burning. Some general symptoms such as bloating, nausea, vomiting, and fullness after eating small amounts of food are also common.
According to this scientific review article (2014), dyspepsia can reach prevalence figures of up to 24%, despite the fact that many patients avoid medical consultation and prefer self-medication with over-the-counter drugs. Therefore, these latter cases are not recorded.
Classification of dyspepsia
This can be divided into two types: functional and organic. The first occurs in the absence of an illness, while in the second there is an obvious cause. Next, we’ll describe the particularities of each one.
Functional
This type of dyspepsia is one that isn’t related to important organic pathologies, such as peptic ulcers. To reach the diagnosis, the doctor could resort to several complementary studies that we’ll talk about later.
Although the exhaustive search for diseases doesn’t give any results in functional dyspepsia, it’s logical to think that there’s some pathophysiological cause behind the symptoms. For years, this seemed to be a mystery, until this meta-analysis (2018) was published.
To carry out this study, the authors reviewed 37 high-quality publications in which some microscopic findings were published in the gastric and duodenal mucosa of patients with functional dyspepsia.
Through various statistical methods, they came to the conclusion that the mechanism involved is the appearance of micro-inflammatory phenomena, with an abundance of eosinophils and mast cells.
For practical and economic reasons, these types of procedures aren’t performed routinely. Doctors, once they rule out the presence of important pathologies, usually indicate prolonged treatment to reduce or eliminate symptoms.
Organic

In this case, the symptoms are the result of a certain health condition. Each has its own diagnostic methods, and the most important causes are the following:
- Peptic ulcer: This is a condition characterized by the appearance of excavated lesions in the gastric or duodenal mucosa. It usually causes intense pain and burning. In some patients, it may be the cause of gastrointestinal bleeding.
- Helicobacter pylori infection: This bacterium is responsible for many cases of chronic gastritis. Although in most cases the clinical picture is limited to dyspepsia, in some patients it could evolve to produce gastric cancer.
- Gallstones: This is a very common condition in which there’s an accumulation of hardened substances within the lumen of the gallbladder or bile ducts. When an associated infection occurs, it’s called cholecystitis or cholangitis.
- Pancreatic or gastric cancer: Both conditions have a poor prognosis, especially because their diagnosis is usually late. Some warning symptoms are digestive bleeding and unexplained weight loss.
Other much less common causes include chronic pancreatitis, some metabolic disorders, and poorly controlled diabetes mellitus. In the latter case, dyspepsia is a consequence of nerve damage due to persistent elevation of blood glucose (diabetic neuropathy).
Diagnosis
As we mentioned before, dyspepsia isn’t a disease. Therefore, at first, the diagnosis seems obvious. However, the real importance of going to the doctor lies in determining the origin of the symptoms.
For this reason, the goal of the gastroenterologist is to determine if it’s a case of functional or organic dyspepsia. For this reason, patients are usually differentiated according to the probability that they have functional dyspepsia. The use of clinical rating scales allows specialists to determine this probability.
If the doctor suspects the existence of a previous pathology that explains the symptoms, he could resort to several different studies to make the diagnosis.
Complementary studies
The most effective method is an upper gastrointestinal endoscopy. This technique is based on the introduction of a flexible tube connected to a high-resolution camera, which can be introduced (after sedation) through the patient’s mouth.
This allows the correct visualization of gastrointestinal structures, in addition to allowing the specialists to perform biopsies in places of interest.
There are less specific methods but ones that still help when making the diagnosis, such as the following:
- A complete blood count
- Abdominal echography
- Detection of H. pylori through serological studies and the determination of antigens in feces, among other tests.
Treatment
Like many other gastrointestinal disorders, dyspepsia can be treated by changing some eating and behavioral patterns. When necessary, the use of drugs is also possible.
Diet and lifestyle changes
This is usually the first recommendation that doctors make. According to a publication from the Mayo Clinic, the main recommendations are the following:
- Avoid skipping meals
- Reduce the consumption of tobacco, coffee, and alcohol.
- Do not eat large meals
- Decrease the amount of food and increase the frequency of meals
- Chew and swallow slowly and deliberately
Although these changes can provide symptomatic relief, there are frequent cases where you won’t get complete relief. In these patients, pharmacological treatment is recommended.
Drugs
If it is a case of secondary or organic dyspepsia, treatment is directed to the cause of the symptoms. For example, to achieve the elimination of H. pylori, doctors often prescribe omeprazole, clarithromycin, and amoxicillin.
In cases of functional dyspepsia, one of the following drugs may be recommended:
- Proton pump inhibitors: These decrease gastric acid secretion, and an example is omeprazole.
- Prokinetics: Promotes gastric emptying and prevents gastroesophageal reflux. This group includes metoclopramide, domperidone, and cinitapride.
- Psychopharmaceuticals: These are useful only when there is an associated psychiatric component.
Living with dyspepsia: when do you need to go to the doctor?
When symptoms are severe or recur too frequently, it’s advisable to go to the gastroenterologist. Depending on the context, they could request more studies to determine the origin of the dyspepsia, although in many cases there’s no clear illness.
- Longstreth GF, Thompson WG, Chey WD, et al. Functional bowel disorders. Gastroenterology 2006;130:1480-1491.
-
Mearin F, et al. Definiendo la dispepsia funcional. Rev Esp Enferm Dig (Madrid) 2011;103(11):640-647.
-
Mearin F. Dispepsia funcional. Revista de Gastroenterología de México 2010;Supl. 2(75):19-24.
-
Moayyedi P, Mason J. Clinical and economic consequences of dyspepsia in the community. Gut 2002;Supl 4:10-2.
-
Tack J, Talley NJ, Camilleri M, et al. Functional gastroduodenal disorders: a working team report for the Rome III consensus on functional gastrointestinal disorders. Gastroenterology 2006;130:1466-1479.
-
Talley NJ. Functional gastrointestinal disorders as a public health problem. Neurogastroenterol Motil 2008;(Supl. 1):121-9.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







