What Is an Antigen Test?

Escrito y verificado por el biólogo Samuel Antonio Sánchez Amador
Human beings are a reservoir of thousands of pathogens, so it isn’t surprising that 95% of the world’s population has some type of illness, disease, or health problem at any given time and place, as indicated by information sources. The detection of certain microorganisms within the body is vital for the treatment of infections, and the antigen test is a very effective method.
Today, the words “antigens”, “antibodies”, “herd immunity” and many more have become familiar to us due to the pandemic that started in 2020. However, few people really know what all these terms mean.
When we speak of an “antigen test” we’re referring, of course, to a rapid medical test that detects the presence of a pathogen in the body of a human.. Let’s take a closer look at how it’s done and what implications it has.
An overview of human immunity
Before explaining in detail what an antigen test is, we must lay a certain foundation regarding the immune system. The National Cancer Institute (NCI) defines this mechanism as “a complex network of cells, tissues, organs and substances that help protect the body from pathogens ( exogenous factors) and internal failures, such as cancer (endogenous)”.
Human immunity is divided into 2 mechanisms: innate and acquired. The first responds nonspecifically to the presence of threats, while the second is responsible for attacking in a specialized way the causative pathogen of the disease and “remembering” it for a variable period of time.
- The innate immune system activates the acquired one in the presence of infections. For example, macrophages engulf the pathogen and present it to lymphocytes, which elicit a specialized response.
- The acquired immune system uses innate mechanisms to fight infection.
Antigens and antibodies
One of the basic molecules when talking about the acquired immune system is the antibody. This term represents a series of proteins produced by B lymphocytes when they differentiate into plasma cells. Antibodies have variable regions that bind to specific compounds of the pathogen, recognizing and attacking it exclusively.
This molecule that binds to the antibody is known as an antigen. Thus, an “antigen” is any substance that causes an immune reaction when entering the body. This isn’t always of infectious origin, since it can be an allergen in pollen, for example.
The antigens of the harmful microorganism bind to the antibodies, thus remaining marked. In this way, the lymphocytes know which molecules in the body to attack.
What is an antigen test?
Now that we are clear about the basics of the immune system, understanding this term is much easier. Briefly stated, an antigen test is a quick and easy way to demonstrate the presence or absence of a specific antigen (a sign of infection) in a sample provided by a suspected patient.
Also called rapid antigen detection tests (RATs), these procedures stand out from the rest because they look for a specific protein of the microorganism in the sample. On the other hand, antibody tests try to locate specific antibodies in the patient’s blood, while PCRs (polymerase chain reaction) try to find genetic information about the pathogen.
Antigen tests are much faster than a PCR or an antibody test.
General mechanism of action
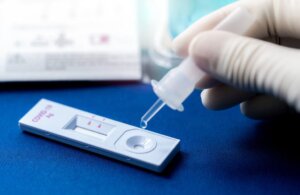
Using an antigen test is quite similar to a pregnancy test. In a healthcare setting, the professional obtains a sample from the patient and it is placed in a device that separates the compound of interest using immunoaffinity chromatography.
In the following list, we’ll show you how an antigen test works:
- A sample is collected from the patient (eg, from the nasopharyngeal tract with a swab) and placed into the specialized device.
- The sample is absorbed by capillary action and progresses through the device. At this point, it mixes with a conjugate flowing through a membrane.
- The conjugate is a mixture of substances, but it contains antibodies specific to the antigen to be localized. For example, if the antigen is “A”, there are “anti-A antibodies” in the contraption.
- If the result is positive, a colored band appears on the device. This indicates that the antigen and antibody have bound, thus confirming the presence of the pathogen of interest in the sample.
- If the band is not colored in the indicated place on the device, the test result is negative. However, a possible infection cannot be completely ruled out.
If the antigen-antibody complex is produced, a colored band forms on the test device, and infection is confirmed. The results are visible to the naked eye, so it’s simply interpreted as a “yes” or “no” to the question of whether there’s an infection.
These tests report results in about 15-30 minutes, so the patient can go home with a confirmed diagnosis if they have tested positive for the disease.
Sensitivity and specificity of the antigen test
The term sensitivity refers to the number of sick patients who have received a positive result when using a specific test. On the other hand, specificity designates the percentage of healthy people who have obtained a negative diagnosis. In other words, the perfect test must rule out 100% non-diseased inhabitants and collect all those infected.
As the antigen test can be seen with the naked eye and is a bit rudimentary, it reports a sensitivity and specificity that are relatively low. Therefore, the absence of the colored band on the device doesn’t always indicate an absence of infection, and the patient sample should undergo a PCR test to refine the diagnosis.
In the polymerase chain reaction (PCR), the RNA or DNA of the pathogen is extracted from the patient sample and amplified using thermal cyclers. Using chromatography, electrophoresis, and other techniques, “bands” can be visualized in the analyzes that indicate the presence of the genome of the virus or bacterium that is being searched for. This technique is far more effective.
PCR is vastly more efficient than an antigen test, but it’s also more expensive and results take significantly longer to arrive.
Types of antigen test
Although, due to the pandemic, we usually only think about one type of antigen test, the reality is that there are many more. We’ll take a look at all of them, leaving the most familiar one to the end. Don’t miss it.
1. Rapid test for the detection of streptococcus antigens
Known as the rapid strep test (RST), this detection method is used to confirm the diagnosis in people with pharyngitis caused by group A strep bacteria. There are many subtypes of tests within this group, but they all have something in common – they respond to a Streptococcus-A specific antigen in a patient sample.
According to the Kids Health portal, this rapid test is used mainly in young children in the following scenarios:
- The patient has symptoms of a streptococcal infection in the throat and this cannot be attributed to a virus.
- The child has a sore throat and has previously been in contact with a positive strep infection.
The premise is very similar to the general mechanism cited above – the child’s mucus is exposed to a reagent containing antibodies that specifically bind to Streptococcus A antigens. If the test is positive, a colored band appears on the device used.
The average specificity of this type of test is 95%, but the sensitivity is between 65-80%. A negative result cannot be used to rule out a Strep A infection, but it can help the medical professional to continue with the diagnosis on the right path.
Sometimes it is necessary to do a culture of the bacteria to confirm the diagnosis, as this test is not reliable in 100% of cases.
2. Rapid diagnostic test for malaria
Malaria is a disease of great significance throughout the world. As indicated by the World Health Organization (WHO), more than 220 million global cases are estimated and 400,000 patients lose their lives each year fighting this disease. The African region is the one that is most impacted, as 94% of cases around the world occurred there in 2019.
Due to the epidemiological burden of parasites of the genus Plasmodium, at least 20 types of rapid diagnostic tests have been developed to detect the disease. A laboratory analysis is not needed to confirm positive cases, and on these occasions the sample collected is blood, not from the patient’s mucosa.
The sensitivity of these tests is around 99.7%, so they can be used as the sole diagnostic method of infection.
3. Rapid influenza diagnostic test
Flu or influenza viruses are very familiar to us all. Although they don’t cause serious effects in the general population, it mustn’t be forgotten that these viral clusters affect 10% of adults and 30% of children each year, causing up to 650,000 deaths per year from respiratory failure. Therefore, it’s necessary to detect them quickly.
As you can imagine, the operation of this test is the same as that of Streptococcus A. A sample of the patient’s mucosa is obtained, the presence of the antigen is analyzed and, if it’s positive, a colored band appears on the device. However, the results aren’t as promising as in the other models; some tests report false negatives in 49% of cases.
We go further, since scientific studies have shown that some brands report false negatives in 88.9% of cases, correctly reflecting the H1N1 infection in only the remaining 11.1%. For this reason, it’s unusual for a rapid flu diagnostic test to be performed to confirm infection.
4. COVID-19 antigen test

Without a doubt, the COVID-19 antigen test is the most famous and the one that has monopolized the media in recent times. Millions of people around the world have already undergone this test due to the suspicion of infection by the SARS-CoV-2 virus.
Due to the medical urgency of this pathogen, COVID-19 antigen tests have been sold very cheaply and have been made available to the entire population. In this case, a sample is obtained from the patient’s nasal cavity with a swab and is subjected to the aforementioned mechanism. Results are obtained in about 15-30 minutes.
This type of test reports a sensitivity of 98.2% and a specificity greater than 99% in symptomatic patients with 5 or less days of evolution. Unfortunately, the sensitivity is much lower in asymptomatic people (45.5%), which indicates that detecting the virus in a sick person without clinical symptoms is much more difficult than ruling out its presence in an uninfected person.
The specificity and sensitivity of this test in asymptomatic patients is low. Unfortunately, they carry the virus and can continue to spread it even if they have tested negative.
Antigen tests are useful, but they have their limitations
As you have seen, the antigen test is very useful to detect the presence of a pathogen. The operation is quite simple – if the antibodies in the device bind to the antigens in the sample, a color change can be observed, indicating the presence of infection.
However, we emphasize that these detection methods are not perfect, since they can report false positives or negatives in some cases. This is further complicated in asymptomatic patients, since the sensitivity and specificity in general is much lower for them. If in doubt, PCR is always the way to go.
Human beings are a reservoir of thousands of pathogens, so it isn’t surprising that 95% of the world’s population has some type of illness, disease, or health problem at any given time and place, as indicated by information sources. The detection of certain microorganisms within the body is vital for the treatment of infections, and the antigen test is a very effective method.
Today, the words “antigens”, “antibodies”, “herd immunity” and many more have become familiar to us due to the pandemic that started in 2020. However, few people really know what all these terms mean.
When we speak of an “antigen test” we’re referring, of course, to a rapid medical test that detects the presence of a pathogen in the body of a human.. Let’s take a closer look at how it’s done and what implications it has.
An overview of human immunity
Before explaining in detail what an antigen test is, we must lay a certain foundation regarding the immune system. The National Cancer Institute (NCI) defines this mechanism as “a complex network of cells, tissues, organs and substances that help protect the body from pathogens ( exogenous factors) and internal failures, such as cancer (endogenous)”.
Human immunity is divided into 2 mechanisms: innate and acquired. The first responds nonspecifically to the presence of threats, while the second is responsible for attacking in a specialized way the causative pathogen of the disease and “remembering” it for a variable period of time.
- The innate immune system activates the acquired one in the presence of infections. For example, macrophages engulf the pathogen and present it to lymphocytes, which elicit a specialized response.
- The acquired immune system uses innate mechanisms to fight infection.
Antigens and antibodies

One of the basic molecules when talking about the acquired immune system is the antibody. This term represents a series of proteins produced by B lymphocytes when they differentiate into plasma cells. Antibodies have variable regions that bind to specific compounds of the pathogen, recognizing and attacking it exclusively.
This molecule that binds to the antibody is known as an antigen. Thus, an “antigen” is any substance that causes an immune reaction when entering the body. This isn’t always of infectious origin, since it can be an allergen in pollen, for example.
The antigens of the harmful microorganism bind to the antibodies, thus remaining marked. In this way, the lymphocytes know which molecules in the body to attack.
What is an antigen test?
Now that we are clear about the basics of the immune system, understanding this term is much easier. Briefly stated, an antigen test is a quick and easy way to demonstrate the presence or absence of a specific antigen (a sign of infection) in a sample provided by a suspected patient.
Also called rapid antigen detection tests (RATs), these procedures stand out from the rest because they look for a specific protein of the microorganism in the sample. On the other hand, antibody tests try to locate specific antibodies in the patient’s blood, while PCRs (polymerase chain reaction) try to find genetic information about the pathogen.
Antigen tests are much faster than a PCR or an antibody test.
General mechanism of action
Using an antigen test is quite similar to a pregnancy test. In a healthcare setting, the professional obtains a sample from the patient and it is placed in a device that separates the compound of interest using immunoaffinity chromatography.
In the following list, we’ll show you how an antigen test works:
- A sample is collected from the patient (eg, from the nasopharyngeal tract with a swab) and placed into the specialized device.
- The sample is absorbed by capillary action and progresses through the device. At this point, it mixes with a conjugate flowing through a membrane.
- The conjugate is a mixture of substances, but it contains antibodies specific to the antigen to be localized. For example, if the antigen is “A”, there are “anti-A antibodies” in the contraption.
- If the result is positive, a colored band appears on the device. This indicates that the antigen and antibody have bound, thus confirming the presence of the pathogen of interest in the sample.
- If the band is not colored in the indicated place on the device, the test result is negative. However, a possible infection cannot be completely ruled out.
If the antigen-antibody complex is produced, a colored band forms on the test device, and infection is confirmed. The results are visible to the naked eye, so it’s simply interpreted as a “yes” or “no” to the question of whether there’s an infection.
These tests report results in about 15-30 minutes, so the patient can go home with a confirmed diagnosis if they have tested positive for the disease.
Sensitivity and specificity of the antigen test
The term sensitivity refers to the number of sick patients who have received a positive result when using a specific test. On the other hand, specificity designates the percentage of healthy people who have obtained a negative diagnosis. In other words, the perfect test must rule out 100% non-diseased inhabitants and collect all those infected.
As the antigen test can be seen with the naked eye and is a bit rudimentary, it reports a sensitivity and specificity that are relatively low. Therefore, the absence of the colored band on the device doesn’t always indicate an absence of infection, and the patient sample should undergo a PCR test to refine the diagnosis.
In the polymerase chain reaction (PCR), the RNA or DNA of the pathogen is extracted from the patient sample and amplified using thermal cyclers. Using chromatography, electrophoresis, and other techniques, “bands” can be visualized in the analyzes that indicate the presence of the genome of the virus or bacterium that is being searched for. This technique is far more effective.
PCR is vastly more efficient than an antigen test, but it’s also more expensive and results take significantly longer to arrive.
Types of antigen test
Although, due to the pandemic, we usually only think about one type of antigen test, the reality is that there are many more. We’ll take a look at all of them, leaving the most familiar one to the end. Don’t miss it.
1. Rapid test for the detection of streptococcus antigens
Known as the rapid strep test (RST), this detection method is used to confirm the diagnosis in people with pharyngitis caused by group A strep bacteria. There are many subtypes of tests within this group, but they all have something in common – they respond to a Streptococcus-A specific antigen in a patient sample.
According to the Kids Health portal, this rapid test is used mainly in young children in the following scenarios:
- The patient has symptoms of a streptococcal infection in the throat and this cannot be attributed to a virus.
- The child has a sore throat and has previously been in contact with a positive strep infection.
The premise is very similar to the general mechanism cited above – the child’s mucus is exposed to a reagent containing antibodies that specifically bind to Streptococcus A antigens. If the test is positive, a colored band appears on the device used.
The average specificity of this type of test is 95%, but the sensitivity is between 65-80%. A negative result cannot be used to rule out a Strep A infection, but it can help the medical professional to continue with the diagnosis on the right path.
Sometimes it is necessary to do a culture of the bacteria to confirm the diagnosis, as this test is not reliable in 100% of cases.
2. Rapid diagnostic test for malaria
Malaria is a disease of great significance throughout the world. As indicated by the World Health Organization (WHO), more than 220 million global cases are estimated and 400,000 patients lose their lives each year fighting this disease. The African region is the one that is most impacted, as 94% of cases around the world occurred there in 2019.
Due to the epidemiological burden of parasites of the genus Plasmodium, at least 20 types of rapid diagnostic tests have been developed to detect the disease. A laboratory analysis is not needed to confirm positive cases, and on these occasions the sample collected is blood, not from the patient’s mucosa.
The sensitivity of these tests is around 99.7%, so they can be used as the sole diagnostic method of infection.
3. Rapid influenza diagnostic test
Flu or influenza viruses are very familiar to us all. Although they don’t cause serious effects in the general population, it mustn’t be forgotten that these viral clusters affect 10% of adults and 30% of children each year, causing up to 650,000 deaths per year from respiratory failure. Therefore, it’s necessary to detect them quickly.
As you can imagine, the operation of this test is the same as that of Streptococcus A. A sample of the patient’s mucosa is obtained, the presence of the antigen is analyzed and, if it’s positive, a colored band appears on the device. However, the results aren’t as promising as in the other models; some tests report false negatives in 49% of cases.
We go further, since scientific studies have shown that some brands report false negatives in 88.9% of cases, correctly reflecting the H1N1 infection in only the remaining 11.1%. For this reason, it’s unusual for a rapid flu diagnostic test to be performed to confirm infection.
4. COVID-19 antigen test

Without a doubt, the COVID-19 antigen test is the most famous and the one that has monopolized the media in recent times. Millions of people around the world have already undergone this test due to the suspicion of infection by the SARS-CoV-2 virus.
Due to the medical urgency of this pathogen, COVID-19 antigen tests have been sold very cheaply and have been made available to the entire population. In this case, a sample is obtained from the patient’s nasal cavity with a swab and is subjected to the aforementioned mechanism. Results are obtained in about 15-30 minutes.
This type of test reports a sensitivity of 98.2% and a specificity greater than 99% in symptomatic patients with 5 or less days of evolution. Unfortunately, the sensitivity is much lower in asymptomatic people (45.5%), which indicates that detecting the virus in a sick person without clinical symptoms is much more difficult than ruling out its presence in an uninfected person.
The specificity and sensitivity of this test in asymptomatic patients is low. Unfortunately, they carry the virus and can continue to spread it even if they have tested negative.
Antigen tests are useful, but they have their limitations
As you have seen, the antigen test is very useful to detect the presence of a pathogen. The operation is quite simple – if the antibodies in the device bind to the antigens in the sample, a color change can be observed, indicating the presence of infection.
However, we emphasize that these detection methods are not perfect, since they can report false positives or negatives in some cases. This is further complicated in asymptomatic patients, since the sensitivity and specificity in general is much lower for them. If in doubt, PCR is always the way to go.
- Todos (casi) enfermos: más del 95% de la población mundial tiene problemas de salud, 20 minutos Salud. Recogido a 3 de septiembre en https://www.20minutos.es/noticia/2483075/0/95-por-ciento-poblacion/mundo-tiene/problemas-salud/?autoref=true
- Definición de sistema inmunitario, Instituto Nacional del Cáncer (NIH). Recogido a 3 de septiembre en https://www.cancer.gov/espanol/publicaciones/diccionarios/diccionario-cancer/def/sistema-inmunitario
- Visión panorámica del sistema inmune, Elsevier. Recogido a 3 de septiembre en https://www.elsevier.es/es-revista-revista-medica-clinica-las-condes-202-articulo-vision-panoramica-del-sistema-inmune-S0716864012703358
- What is an antigen test and what does it consist of? Clinica Barcelona. Recogido a 3 de septiembre en https://www.clinicbarcelona.org/en/assistance/tests-and-procedures/antigen/what-is-an-antigen-test-and-what-does-it-consist-of
- Strep test: rapid, KidsHealth. Recogido a 3 de septiembre en https://kidshealth.org/en/parents/test-rapid-strep.html
- Paludismo, OMS. Recogido a 3 de septiembre en https://www.who.int/es/news-room/fact-sheets/detail/malaria
- Sensibilidad y especificidad de los test rápidos antigénicos en personas asintomáticas, Murcia Salud. Recogido a 3 de septiembre en https://www.murciasalud.es/preevid/23830#:~:text=La%20sensibilidad%20de%20la%20prueba,2%20a%2098%2C6%25).
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







