The Different Stages of Melanoma

Before talking about the stages of melanoma, we’d like to point out that we normally find several types of cells in the skin. These include basal cells, squamous cells, and melanocytes.
Melanocytes are cells that produce melanin, a pigment that protects against ultraviolet (UV) rays and colors the skin, hair, and eyes. The higher the number of melanocytes, the darker the skin, and it’s for this reason that white-skinned people are more likely to develop this type of tumor.
When benign tumors develop from melanocytes, they’re called nevi or moles. In contrast, the malignant tumor that arises from melanocytes is called melanoma.
Skin carcinomas originating from basal and squamous cells (basal cell and squamous cell carcinoma, respectively) are more common than melanoma. In this case, although its frequency is 4% of all cancerous skin lesions, it also has a high mortality. For this reason, early diagnosis to receive timely treatment is essential.
Other important terms that we need to know
The doctor may mention certain terms in your appointments. Understanding them will make it easier to understand the different stages of melanoma. They’re the following:
- Epidermis: This is the most superficial layer of cells of the skin.
- Nevus: Also known as moles, they’re benign tumors of the skin. Generally, they’re present from birth but some can appear during adulthood.
- Biopsy: This consists of taking a sample of some tissue (in this case, the skin) to allow the specialist to examine its characteristics under the microscope, and to determine if it’s a benign or malignant lesion.
- In situ: This is cancer that hasn’t spread beyond a small area of skin.
- Sentinel lymph node: This fulfills the function of the main tumor drainage.
- Microsatellite metastases: Microscopic cutaneous or subcutaneous metastases, which may be adjacent or far away from the primary melanoma.
- Satellite metastases: These are within the lymphatic system less than 2 centimeters (under an inch) from the melanoma.
How to detect melanoma early
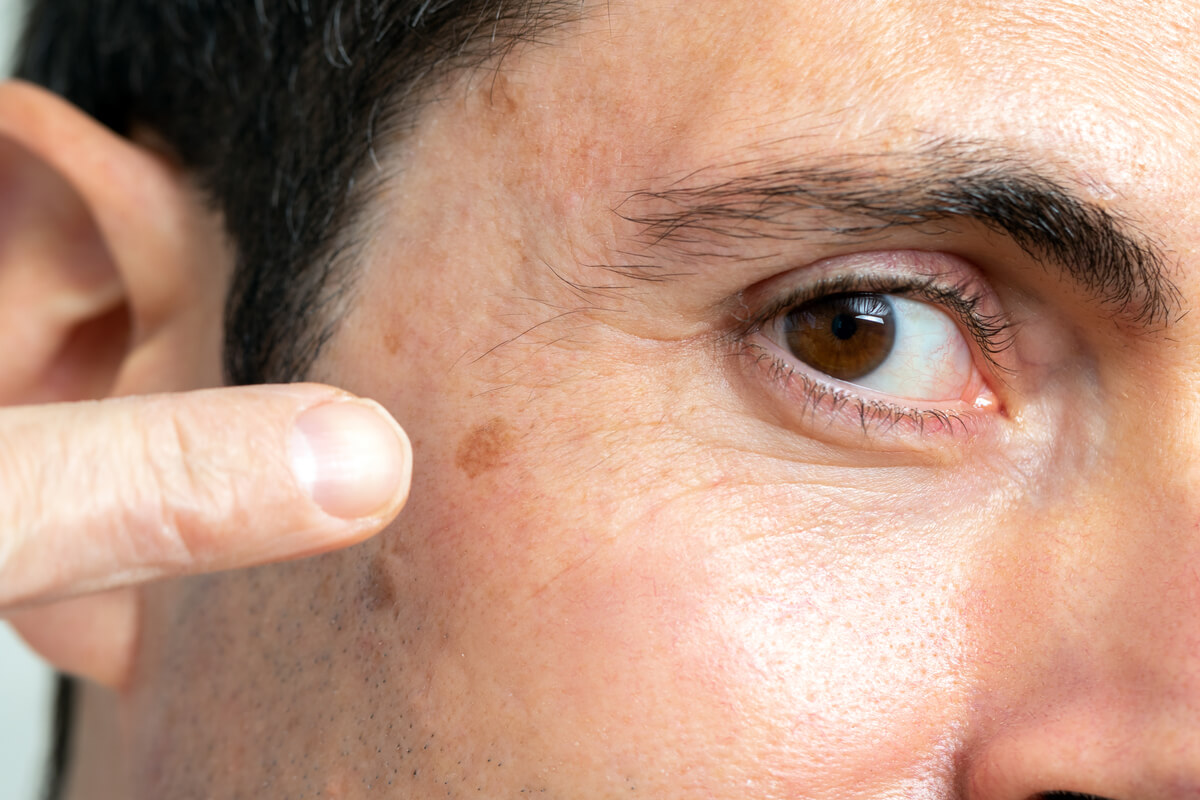
The main thing is to look for any new or unusual changes in the skin, whether it’s been exposed to the sun or not. Melanomas usually appear on the legs (women) and the trunk (men). In darker-colored people, this tumor is usually diagnosed later, has a worse prognosis, and is more frequently located on the palms, soles, and mouth. It’s usually more common in people over 80 years of age.
Diagnosing a melanoma isn’t easy. Only 30% develop over a previous mole and 70% can develop on normal skin. Fortunately, these tumors have some very particular characteristics that facilitate their early diagnosis. We’ll tell you about them below.
Nevus or melanoma?
Through dermoscopy, the dermatologist will look for signs that help differentiate a benign lesion from one that’s possibly malignant, and they’ll be able to define the stage of melanoma. These features include the following:
- A – Asymmetry: Unlike moles, melanomas are usually asymmetric, that is, if we pass an imaginary line through the middle, its two halves are different.
- B – Border: They’re irregular, extended, or wavy.
- C – Color: Melanomas usually have different colors or shades of the same color (red, black, brown, white, blue). Rarely, some melanomas known as melanocytic appear lighter than the skin.
- D – Diameter: Size is important. A lesion larger than 6 millimeters is usually suspicious.
- E – Evolution: Skin lesions shouldn’t constantly change. A mole that grows in size or changes shape, color, elevation, or begins to itch or bleed should be evaluated by a doctor.
Although the specialist will evaluate the patient and give the final diagnosis, each person must be attentive to these changes to go to see a doctor as soon as possible.
Staging or stages of melanoma
The stages of melanoma allow the doctor to decide the treatment plan and estimate the prognosis. In this way, the doctor can discuss the course of action with the patient.
TNM system
Before mentioning staging, we need to know what the TNM system is. The American Joint Committee on Cancer (AJCC) classifies different types of cancer (including melanoma) according to a commonly used system, the TNM system, which is based on the following 3 characteristics:
T – Thickness
This is the depth that the skin lesion has reached, and it’s measured through the Breslow index. It’s a measurement in millimeters from the granular layer of the skin to the maximum depth reached by the melanoma at a right angle to the epidermis.
Although there are many factors involved in the survival of patients diagnosed with melanoma, the thickness of the lesion is one of the most important. The thicker it is, the worse the prognosis and vice versa.
Melanoma ulceration also falls into this category. Ulcers appear on the skin, in this case on melanoma. Their presence represents an increased risk of spreading the cancer.
N – Lymph nodes
Lymph nodes are structures that are part of the immune system and the system that carries lymph throughout the body. Being distributed throughout the body, they’re often the first place the tumors spread from.
The presence or absence of affected lymph nodes surrounding the melanoma will determine this name. There’s a subcategory called “in situ”, which involves local lymph nodes but without any spread to systemic lymph nodes.
M – Metastasis
This is the metastasis or spread of cancer to other lymph nodes, adjacent skin, or organs. The most frequent areas of spread are the following:
- Skin and subcutaneous tissue
- Lungs
- The central nervous system
- The liver
- Bone
In the new 2018 melanoma stage classification, the AJCC has introduced the use of lactate dehydrogenase (LDH) levels to this category. LDH is an enzyme that participates in redox (a type of chemical reaction) and is released when there’s damage to cells in the body, such as cancer.
Stages and prognosis of melanoma
For melanoma, different stages have been established: 0, I, II, III, IV, and V. As the number increases, it means that the tumor has spread more in the body and has a worse prognosis. According to this, they’re grouped into three large groups:
- Early-stage: This covers stages 0 and I.
- Stage 0: Also called melanoma in situ, it’s limited to the superficial layer of the skin (epidermis).
- Stage I: The melanoma is localized but invasive, that is, it has spread to the next layer of skin (dermis) and measures <1 millimeter according to Breslow.
- Intermediate to high risk (loco-regional): the tumor has invaded the lymph nodes or skin near the tumor. This corresponds to stage II.
- Stage II: The melanoma reaches a depth> 1 millimeter and may or may not be ulcerated. Its risk of spreading to the regional nodes is high, so the doctor may order a sentinel node biopsy.
- Advanced stage (metastatic): The cancer has spread far away from the area where the melanoma started to develop. It corresponds to stages III and IV.
- Stage III: In this case, the thickness is no longer the determining factor, but, rather, the spread. The tumor has spread more than 2 centimeters (nearly an inch) from the origin or has reached local lymph nodes (microsatellite or satellite metastases). On physical examination, these nodes may or may not be palpable.
- Stage IV: In this final stage, there’s the involvement of multiple lymph nodes or other organs (lung, liver, CNS, bone, or gastrointestinal system).
Final classification of melanoma
In this way, a number is assigned to each characteristic (T, N, M) and a letter (a, b, c, d) if there’s a subcategory. So, the stages of melanoma would bear the following name according to the findings in each patient.
T – Thickness
- TX: non-evaluable thickness (for example, curettage sample).
- T0: No evidence of primary tumor (indeterminate or complete regression of primary)
- Tis: melanoma in situ.
- T1a: <0.8 millimeters thick without ulceration.
- T1b: <0.8 millimeters thick with ulceration or 0.8 – 1.0 mm thick with or without ulceration.
- T2a: > 1.0 – 2.0 millimeters thick without ulceration.
- T2b: > 1.0 – 2.0 millimeters thick with ulceration.
- T3a: > 2.0 – 4.0 millimeters thick without ulceration.
- T3b: > 2.0 – 4.0 millimeters thick with ulceration.
- T4a: > 4.0 millimeters thick without ulceration.
- T4b: > 4.0 millimeters thick with ulceration.
N – Lymph nodes
- NX: Not evaluable (staging procedure not performed or nodule previously removed).
- N0: No regional metastasis.
- N1a: One nodal metastasis, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N1b: One nodal metastasis, clinically detected (no in-transit / satellite / microsatellite metastases).
- N1c: Negative for nodal metastasis, clinically hidden (positive for in-transit / satellite / microsatellite metastases).
- N2a: Two to three nodal metastases, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N2b: Two to three nodal metastases, clinically detected (no in-transit / satellite / microsatellite metastases).
- N2c: One nodal metastasis, clinically hidden or detected (positive for in-transit / satellite / microsatellite metastases).
- N3a: Four or more nodal metastases, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N3b: Four or more nodal metastases, clinically detected (no in-transit / satellite / microsatellite metastases).
- N3c: Four or more nodal metastases (positive for in-transit / satellite / microsatellite metastases).
M – Metastasis
- M0: No evidence of distant metastasis
- M1a (0): Distant metastases in the skin, soft tissues (including muscle) or non-regional lymph node + non-elevated LDH.
- M1a (1): Distant metastases in the skin, soft tissues (including muscle) or non-regional lymph node + elevated LDH.
- M1b (0): Lung metastasis + non-elevated LDH.
- M1b (1): Lung metastasis + elevated LDH.
- M1c (0): Metastasis to an organ other than the CNS + non-elevated LDH.
- M1c (1): Metastasis to an organ other than the CNS + elevated LDH.
- M1d (0): Metastasis to the CNS + non-elevated LDH.
- M1d (1): Metastasis to the CNS + elevated LDH.
Care and prevention is the key
Having sunburn 5 or more times between the ages of 15-20 increases the risk of melanoma by 80% and non-melanoma skin cancer by 70%. Decreasing your exposure to the sun on the beach and using sunscreen consistently can help lower your risk of developing skin cancer.
If you have any new nevus or spot, new change (pain, growth, itching, inflammation) or anything unusual in a lesion, you should go and see your dermatologist as soon as possible. If you have had melanoma, have a checkup regularly with your dermatologist, for an early diagnosis of melanoma recurrence.
Before talking about the stages of melanoma, we’d like to point out that we normally find several types of cells in the skin. These include basal cells, squamous cells, and melanocytes.
Melanocytes are cells that produce melanin, a pigment that protects against ultraviolet (UV) rays and colors the skin, hair, and eyes. The higher the number of melanocytes, the darker the skin, and it’s for this reason that white-skinned people are more likely to develop this type of tumor.
When benign tumors develop from melanocytes, they’re called nevi or moles. In contrast, the malignant tumor that arises from melanocytes is called melanoma.
Skin carcinomas originating from basal and squamous cells (basal cell and squamous cell carcinoma, respectively) are more common than melanoma. In this case, although its frequency is 4% of all cancerous skin lesions, it also has a high mortality. For this reason, early diagnosis to receive timely treatment is essential.
Other important terms that we need to know
The doctor may mention certain terms in your appointments. Understanding them will make it easier to understand the different stages of melanoma. They’re the following:
- Epidermis: This is the most superficial layer of cells of the skin.
- Nevus: Also known as moles, they’re benign tumors of the skin. Generally, they’re present from birth but some can appear during adulthood.
- Biopsy: This consists of taking a sample of some tissue (in this case, the skin) to allow the specialist to examine its characteristics under the microscope, and to determine if it’s a benign or malignant lesion.
- In situ: This is cancer that hasn’t spread beyond a small area of skin.
- Sentinel lymph node: This fulfills the function of the main tumor drainage.
- Microsatellite metastases: Microscopic cutaneous or subcutaneous metastases, which may be adjacent or far away from the primary melanoma.
- Satellite metastases: These are within the lymphatic system less than 2 centimeters (under an inch) from the melanoma.
How to detect melanoma early

The main thing is to look for any new or unusual changes in the skin, whether it’s been exposed to the sun or not. Melanomas usually appear on the legs (women) and the trunk (men). In darker-colored people, this tumor is usually diagnosed later, has a worse prognosis, and is more frequently located on the palms, soles, and mouth. It’s usually more common in people over 80 years of age.
Diagnosing a melanoma isn’t easy. Only 30% develop over a previous mole and 70% can develop on normal skin. Fortunately, these tumors have some very particular characteristics that facilitate their early diagnosis. We’ll tell you about them below.
Nevus or melanoma?
Through dermoscopy, the dermatologist will look for signs that help differentiate a benign lesion from one that’s possibly malignant, and they’ll be able to define the stage of melanoma. These features include the following:
- A – Asymmetry: Unlike moles, melanomas are usually asymmetric, that is, if we pass an imaginary line through the middle, its two halves are different.
- B – Border: They’re irregular, extended, or wavy.
- C – Color: Melanomas usually have different colors or shades of the same color (red, black, brown, white, blue). Rarely, some melanomas known as melanocytic appear lighter than the skin.
- D – Diameter: Size is important. A lesion larger than 6 millimeters is usually suspicious.
- E – Evolution: Skin lesions shouldn’t constantly change. A mole that grows in size or changes shape, color, elevation, or begins to itch or bleed should be evaluated by a doctor.
Although the specialist will evaluate the patient and give the final diagnosis, each person must be attentive to these changes to go to see a doctor as soon as possible.
Staging or stages of melanoma
The stages of melanoma allow the doctor to decide the treatment plan and estimate the prognosis. In this way, the doctor can discuss the course of action with the patient.
TNM system
Before mentioning staging, we need to know what the TNM system is. The American Joint Committee on Cancer (AJCC) classifies different types of cancer (including melanoma) according to a commonly used system, the TNM system, which is based on the following 3 characteristics:
T – Thickness
This is the depth that the skin lesion has reached, and it’s measured through the Breslow index. It’s a measurement in millimeters from the granular layer of the skin to the maximum depth reached by the melanoma at a right angle to the epidermis.
Although there are many factors involved in the survival of patients diagnosed with melanoma, the thickness of the lesion is one of the most important. The thicker it is, the worse the prognosis and vice versa.
Melanoma ulceration also falls into this category. Ulcers appear on the skin, in this case on melanoma. Their presence represents an increased risk of spreading the cancer.
N – Lymph nodes
Lymph nodes are structures that are part of the immune system and the system that carries lymph throughout the body. Being distributed throughout the body, they’re often the first place the tumors spread from.
The presence or absence of affected lymph nodes surrounding the melanoma will determine this name. There’s a subcategory called “in situ”, which involves local lymph nodes but without any spread to systemic lymph nodes.
M – Metastasis
This is the metastasis or spread of cancer to other lymph nodes, adjacent skin, or organs. The most frequent areas of spread are the following:
- Skin and subcutaneous tissue
- Lungs
- The central nervous system
- The liver
- Bone
In the new 2018 melanoma stage classification, the AJCC has introduced the use of lactate dehydrogenase (LDH) levels to this category. LDH is an enzyme that participates in redox (a type of chemical reaction) and is released when there’s damage to cells in the body, such as cancer.
Stages and prognosis of melanoma
For melanoma, different stages have been established: 0, I, II, III, IV, and V. As the number increases, it means that the tumor has spread more in the body and has a worse prognosis. According to this, they’re grouped into three large groups:
- Early-stage: This covers stages 0 and I.
- Stage 0: Also called melanoma in situ, it’s limited to the superficial layer of the skin (epidermis).
- Stage I: The melanoma is localized but invasive, that is, it has spread to the next layer of skin (dermis) and measures <1 millimeter according to Breslow.
- Intermediate to high risk (loco-regional): the tumor has invaded the lymph nodes or skin near the tumor. This corresponds to stage II.
- Stage II: The melanoma reaches a depth> 1 millimeter and may or may not be ulcerated. Its risk of spreading to the regional nodes is high, so the doctor may order a sentinel node biopsy.
- Advanced stage (metastatic): The cancer has spread far away from the area where the melanoma started to develop. It corresponds to stages III and IV.
- Stage III: In this case, the thickness is no longer the determining factor, but, rather, the spread. The tumor has spread more than 2 centimeters (nearly an inch) from the origin or has reached local lymph nodes (microsatellite or satellite metastases). On physical examination, these nodes may or may not be palpable.
- Stage IV: In this final stage, there’s the involvement of multiple lymph nodes or other organs (lung, liver, CNS, bone, or gastrointestinal system).
Final classification of melanoma

In this way, a number is assigned to each characteristic (T, N, M) and a letter (a, b, c, d) if there’s a subcategory. So, the stages of melanoma would bear the following name according to the findings in each patient.
T – Thickness
- TX: non-evaluable thickness (for example, curettage sample).
- T0: No evidence of primary tumor (indeterminate or complete regression of primary)
- Tis: melanoma in situ.
- T1a: <0.8 millimeters thick without ulceration.
- T1b: <0.8 millimeters thick with ulceration or 0.8 – 1.0 mm thick with or without ulceration.
- T2a: > 1.0 – 2.0 millimeters thick without ulceration.
- T2b: > 1.0 – 2.0 millimeters thick with ulceration.
- T3a: > 2.0 – 4.0 millimeters thick without ulceration.
- T3b: > 2.0 – 4.0 millimeters thick with ulceration.
- T4a: > 4.0 millimeters thick without ulceration.
- T4b: > 4.0 millimeters thick with ulceration.
N – Lymph nodes
- NX: Not evaluable (staging procedure not performed or nodule previously removed).
- N0: No regional metastasis.
- N1a: One nodal metastasis, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N1b: One nodal metastasis, clinically detected (no in-transit / satellite / microsatellite metastases).
- N1c: Negative for nodal metastasis, clinically hidden (positive for in-transit / satellite / microsatellite metastases).
- N2a: Two to three nodal metastases, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N2b: Two to three nodal metastases, clinically detected (no in-transit / satellite / microsatellite metastases).
- N2c: One nodal metastasis, clinically hidden or detected (positive for in-transit / satellite / microsatellite metastases).
- N3a: Four or more nodal metastases, clinically hidden (no in-transit / satellite / microsatellite metastases).
- N3b: Four or more nodal metastases, clinically detected (no in-transit / satellite / microsatellite metastases).
- N3c: Four or more nodal metastases (positive for in-transit / satellite / microsatellite metastases).
M – Metastasis
- M0: No evidence of distant metastasis
- M1a (0): Distant metastases in the skin, soft tissues (including muscle) or non-regional lymph node + non-elevated LDH.
- M1a (1): Distant metastases in the skin, soft tissues (including muscle) or non-regional lymph node + elevated LDH.
- M1b (0): Lung metastasis + non-elevated LDH.
- M1b (1): Lung metastasis + elevated LDH.
- M1c (0): Metastasis to an organ other than the CNS + non-elevated LDH.
- M1c (1): Metastasis to an organ other than the CNS + elevated LDH.
- M1d (0): Metastasis to the CNS + non-elevated LDH.
- M1d (1): Metastasis to the CNS + elevated LDH.
Care and prevention is the key
Having sunburn 5 or more times between the ages of 15-20 increases the risk of melanoma by 80% and non-melanoma skin cancer by 70%. Decreasing your exposure to the sun on the beach and using sunscreen consistently can help lower your risk of developing skin cancer.
If you have any new nevus or spot, new change (pain, growth, itching, inflammation) or anything unusual in a lesion, you should go and see your dermatologist as soon as possible. If you have had melanoma, have a checkup regularly with your dermatologist, for an early diagnosis of melanoma recurrence.
- Blundo A, et al. Comparative Analysis of Diagnostic Techniques for Melanoma Detection: A Systematic Review of Diagnostic Test Accuracy Studies and Meta-Analysis. Front. Med.2021; 8:637069. doi: 10.3389/fmed.2021.637069
- Naik P. Cutaneous Malignant Melanoma: A Review of Early Diagnosis and Management. World J Oncol. 2021;12(1):7-19. doi: https://doi.org/10.14740/wjon1349
- Keunga E, Gershenwald J. The eighth edition American Joint Committee on Cancer (AJCC) melanoma staging system: implications for melanoma treatment and care. Expert Rev Anticancer Ther. August 2018; 18(8):775–784. doi:10.1080/14737140.2018.1489246.
- PathologyOutlines.com [Internet]. LeBlanc R. Skin melanocytic tumor: Staging [actualizado 2019; cited junio 2021]. Disponible en: https://www.pathologyoutlines.com/topic/skintumormelanocyticmelanomastaging.html
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







