The 4 Types of Vaccines that Exist

Escrito y verificado por el biólogo Samuel Antonio Sánchez Amador
Vaccines have dramatically reduced the burden of infectious diseases globally. Studies estimate that 103 million childhood medical conditions have been prevented in the United States alone between 1924 and 2010 thanks to vaccination. Thanks to these products aimed at generating acquired immunity, the world is closer to achieving global health. Find out about the different types of vaccines in this article.
One of the most important contemporary milestones in medicine is the eradication of smallpox by vaccination. This infectious disease (caused by the variola virus) plagued humanity for more than 3,000 years, claiming 300 million lives in the 20th century alone. Thanks to vaccines, the world has been free of smallpox since 1980.
It may sound utopian, but a well-designed and equitably distributed vaccine has been shown to be able to wipe disease off the face of the earth. This is something that’s so relevant in these extraordinary times we’re living in, and so if you’d like to know more about vaccines, especially their typology and biological foundations, then keep reading.
What’s a vaccine?
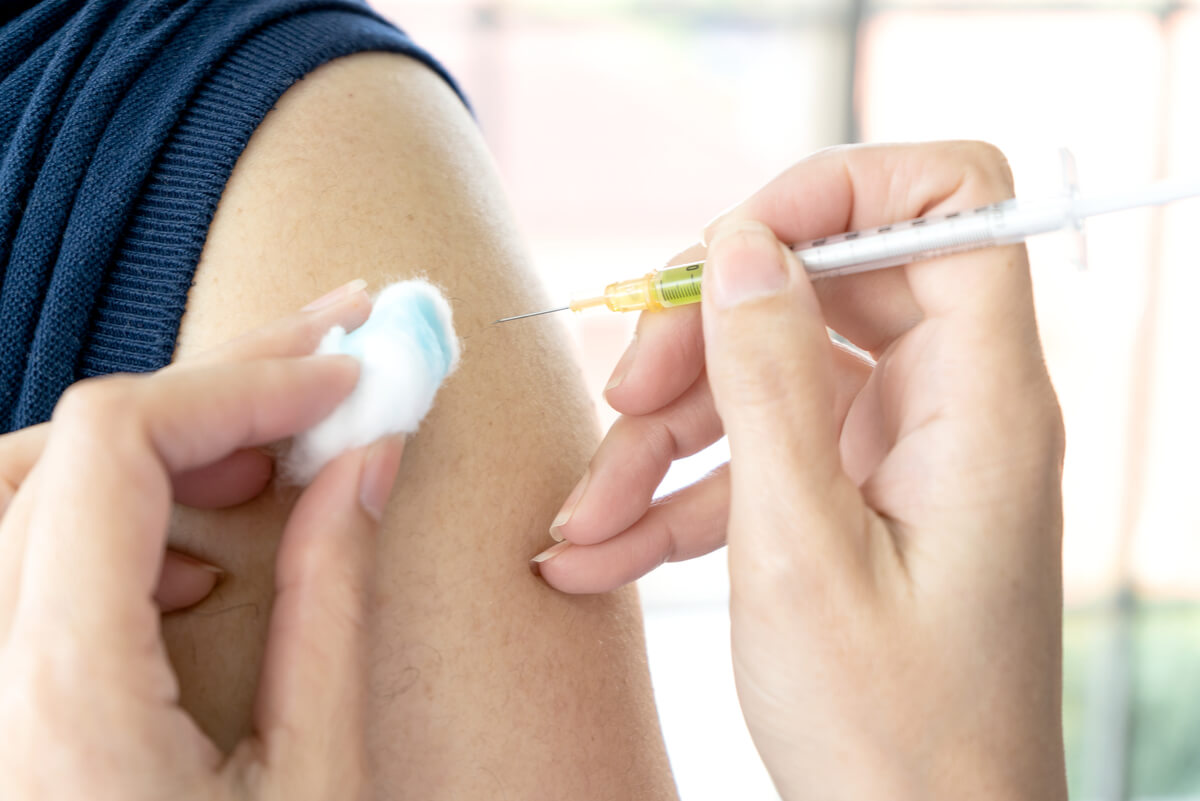
As you might expect, we should start by laying the foundations. The Navarra University Clinic defines a vaccine as follows: ‘a material from a microorganism (or tumor cell) whose inoculation into an organism induces immune resistance against a specific disease’. Said vaccine material can be natural or synthetic products.
The world’s first vaccine was produced thanks to the experiments of Edward Jenner, a physicist and scientist who created the smallpox vaccine. The story is well known in research: an 8-year-old boy was inoculated with a sample of the cowpox virus and, surprisingly, the infant developed immunity to human smallpox.
Due to the similarity between the two viral agents, it was easy to stimulate the immune system to effectively combat the variola virus in our species through exposure to cowpox. That’s how the word vaccine emerged, whose etymological root is in the word vacca, which means cow. From here on, the rest is history.
That discovery was made in 1796. Edward Jenner’s work is said to have saved more lives than that of any other human being.
The key is in acquired immunity
The StatPearls medical portal defines, quickly and easily, what the immune mechanisms of a vaccine are. These preparations affect the patient’s immune system on two predominant fronts: B and T lymphocytes. Prior to exposure to a pathogen, these cell bodies have the potential to respond to a specific antigen and to specialize.
By means of a vaccine, an antigen of the microorganism to be fought is introduced, that is, a specific substance designed to trigger an immune response, mediated by antibodies. When inoculated into the body, the attenuated antigen of the pathogen is phagocytosed and disintegrated by macrophages, responsible for ingesting dangerous microorganisms.
The peptides created by the protein breakdown of the infectious microorganism are “exposed” in the macrophage membrane. We won’t go into all the technical details of the process, as it’s enough for us to understand that a “cascade” is produced which stimulates the synthesis and specialization of the different types of lymphocytes.
The general key is that, in a vaccine, an attenuated form of the pathogen is usually inoculated into the body. Thus, the patient’s immune system recognizes it and, when the real danger enters the body, this mechanism can already respond quickly on two different fronts:
- Neutralizing the infectious agent before it can enter the cells of the body. Remember that viruses require the host’s cellular machinery to multiply. If viruses are removed before they enter them, the infection is cut directly.
- Recognizing and destroying cells that have been infected. Even if some cells are infected, if they are eliminated quickly, and general illness is avoided.
Some vaccine milestones
Unfortunately, the term “vaccine” has a certain negative social connotation today, as ignorance generates fear and, sometimes, certain people or groups can take advantage of it. To eliminate mistrust, we’re going to bring you some data that underlines the importance of these immunization mechanisms throughout history.
- Thanks to vaccines, the last case of smallpox in the world was registered in 1977. In 1980, the World Health Organization (WHO) declared the Earth free of smallpox.
- On August 25, 2020, the WHO declared Africa free of the wild poliovirus. With more than 9 billion doses, 1.8 million serious cases have been prevented.
- In 2015, thanks to the MMR triple viral vaccine, the Americas were pronounced rubella-free.
- The global mortality of the measles virus has been reduced by 80% thanks to vaccination.
As you can see, immunization is undoubtedly positive for world society. The World Health Organization and other sources say that vaccines prevent about 60 deaths per hour.
The 4 types of vaccines
Now you know what vaccines are capable of, when they were discovered, and how they work. We’re now going to look at the information provided by the Vaccines.gov portal to bring you the 4 types of vaccines that currently exist.
1. Live attenuated vaccines
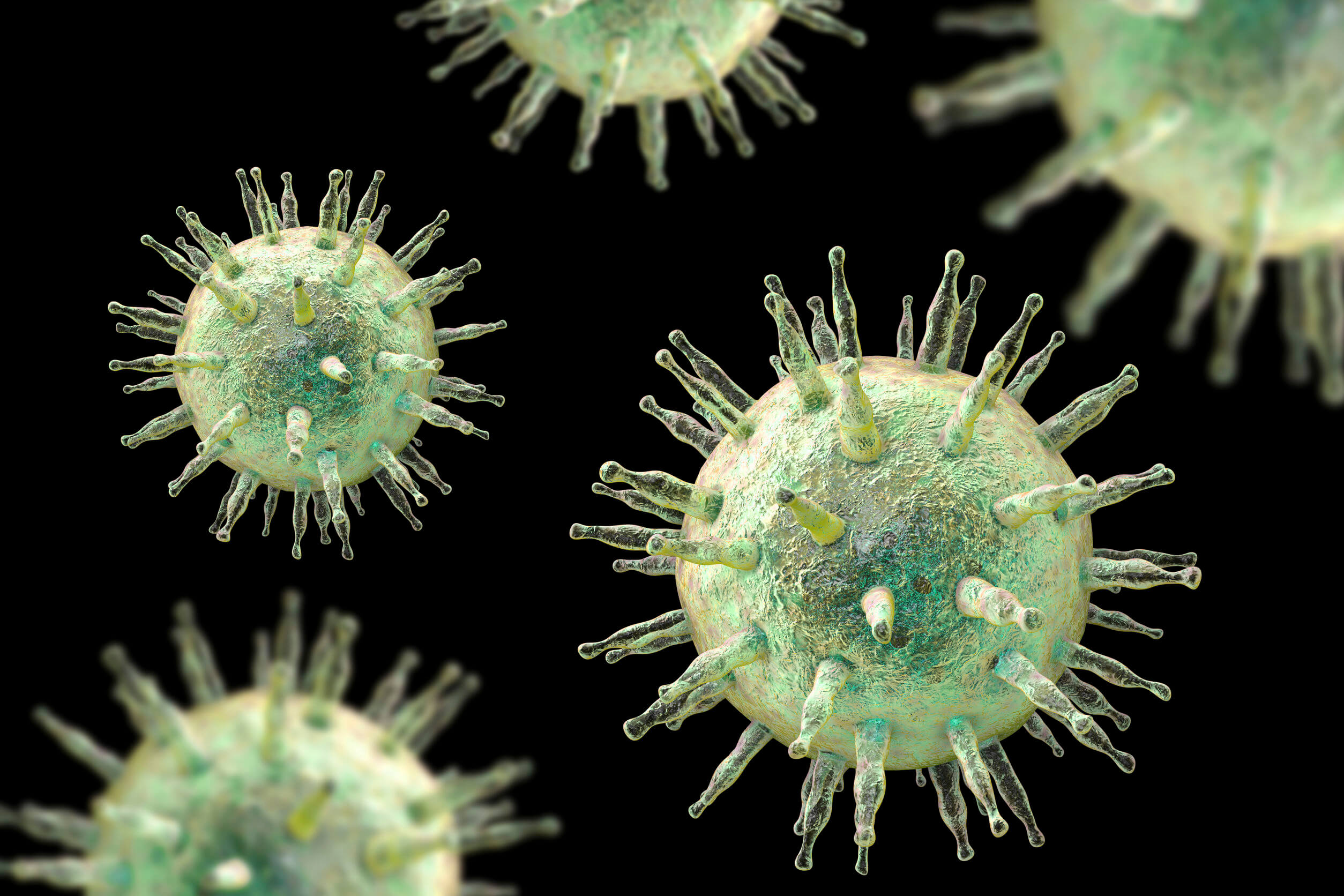
Live attenuated vaccines are the ones that first come to mind when exploring this topic. They’re the ones that contain a complete version of the pathogenic microorganism, but in a weakened form.
Thanks to this, they’re able to stimulate an exact and safe immune response in the patient, since their inoculation doesn’t cause disease in healthy people.
This “weakening” occurs through genetic modification, according to the Vaccine Knowledge Project. This can either be natural or engineered by medical professionals, but one of the most common methods of obtaining it is through consecutive cell cultures.
For example, chicken embryos can be used for several viral generations to replicate in them. With each generation, the virus mutates (unconsciously) towards the specialization in chickens and, therefore, it loses pathogenicity towards us. Over time (up to 200 passes) the pathogen will lose its ability to replicate in human cells.
There are many advantages reported by this method of obtaining immunity by live attenuated vaccines. Among them, we find the following:
- It activates all the phases of the immune response in humans and provides a long-lasting response.
- These vaccines are easy to transport and their production cost is low (due to their general simplicity).
- With one or two doses, most live attenuated vaccines are capable of protecting the patient for life.
Unfortunately, this methodology also carries its risks. In immunosuppressed people, the weakened virus may still be able to infect them, with potentially serious effects. Furthermore, natural mutations throughout cultures may also cause the virus to revert to virulence.
A clear example of a live attenuated vaccine is the MMR vaccine, which provides protection against rubella, mumps and measles together. Thanks to it, the incidence of measles is less than 1% of the world population.
2. Inactivated vaccines
Talking about “life” in viruses is complex, since they don’t even have a cell, which is the minimum requirement to consider something to be living. Rather, they are protein capsids that contain within them DNA or RNA, capable of replicating themselves when they enter a host cell.
In the case of inactivated vaccines, a “dead” version of the germ is used, which is usually inactivated with the application of heat or exposure to certain chemicals (such as formalin). The microorganism is unable to replicate in the host, but its antigens are preserved and, therefore, macrophages are able to recognize it.
As you can imagine, these vaccines are used to immunize against very dangerous viruses and pathogens, such as those that cause hepatitis A, polio or rabies. If the pathogen is dead, the possibility of causing an infection is completely eliminated, but unfortunately, the immune response is weaker.
For this reason, several doses of vaccination (or booster vaccines) are usually necessary to maintain immunity in the patient in the long term. As indicated by the Historyofvaccines.orgportal, you get a lesser effect in exchange for zero danger.
3. Subunit, recombinant, polysaccharide, and combination vaccines
Here we’re talking about a heterogeneous group, because, in this case, parts of the pathogen are used to generate immunity, but never the entire microorganism. For example, specific proteins can be isolated from the germ, and they can act as antigens on their own, thus obviating the need to inoculate the pathogen in its entirety.
A very curious type of vaccine is one that is synthesized thanks to genetic engineering. Using recombination techniques, the genomic sequences of the virus that encode the antigen can be inserted into other pathogens or cells (yeast, for example), which are the ones that are inoculated. This method is known as genetic recombination.
Because they aren’t usually as effective as live attenuated vaccines, adjuvants to subunit or polysaccharide vaccines are sometimes necessary. These help to strengthen the immune response and promote the memory mechanism for a longer time, and are often the cause of annoying local reactions.
The hepatitis B virus, the pertussis virus, the human papilloma virus (HPV) or the shingles virus are fought with vaccines of this category.
4. Toxoid vaccines
Last (but not least) we find toxoid vaccines. These vaccines contain toxins or chemical compounds produced by the bacteria or virus against which you want to immunize. A very clear example of the usefulness of this vaccine is that of tetanus, as the dangerous thing here is the toxin that Clostridium tetani produces, not the organism itself.
Thus, in this case, the toxin (tetanospasmin) can be inactivated by chemical treatment, which allows its inoculation without the patient suffering from the effects. The immune system recognizes this toxic agent in future exposures and is, therefore, able to respond quickly when the time comes.
Going beyond the myths
As you may have seen, vaccine creation is easy to understand and can be summarized in a few lines. Sometimes weakened pathogens are used, other times dead organisms are used, and, exceptionally, germ toxins or key subunits that elicit the immune system response are also used.
Be that as it may, the premise is always the same: to accustom the body to the pathogen with non-dangerous methods, so that our immune cells know how to respond at the right time. Vaccines are approved by government bodies (such as the European Medicines Agency), so there is nothing to fear when it comes to undergoing vaccination.
Vaccines have dramatically reduced the burden of infectious diseases globally. Studies estimate that 103 million childhood medical conditions have been prevented in the United States alone between 1924 and 2010 thanks to vaccination. Thanks to these products aimed at generating acquired immunity, the world is closer to achieving global health. Find out about the different types of vaccines in this article.
One of the most important contemporary milestones in medicine is the eradication of smallpox by vaccination. This infectious disease (caused by the variola virus) plagued humanity for more than 3,000 years, claiming 300 million lives in the 20th century alone. Thanks to vaccines, the world has been free of smallpox since 1980.
It may sound utopian, but a well-designed and equitably distributed vaccine has been shown to be able to wipe disease off the face of the earth. This is something that’s so relevant in these extraordinary times we’re living in, and so if you’d like to know more about vaccines, especially their typology and biological foundations, then keep reading.
What’s a vaccine?

As you might expect, we should start by laying the foundations. The Navarra University Clinic defines a vaccine as follows: ‘a material from a microorganism (or tumor cell) whose inoculation into an organism induces immune resistance against a specific disease’. Said vaccine material can be natural or synthetic products.
The world’s first vaccine was produced thanks to the experiments of Edward Jenner, a physicist and scientist who created the smallpox vaccine. The story is well known in research: an 8-year-old boy was inoculated with a sample of the cowpox virus and, surprisingly, the infant developed immunity to human smallpox.
Due to the similarity between the two viral agents, it was easy to stimulate the immune system to effectively combat the variola virus in our species through exposure to cowpox. That’s how the word vaccine emerged, whose etymological root is in the word vacca, which means cow. From here on, the rest is history.
That discovery was made in 1796. Edward Jenner’s work is said to have saved more lives than that of any other human being.
The key is in acquired immunity
The StatPearls medical portal defines, quickly and easily, what the immune mechanisms of a vaccine are. These preparations affect the patient’s immune system on two predominant fronts: B and T lymphocytes. Prior to exposure to a pathogen, these cell bodies have the potential to respond to a specific antigen and to specialize.
By means of a vaccine, an antigen of the microorganism to be fought is introduced, that is, a specific substance designed to trigger an immune response, mediated by antibodies. When inoculated into the body, the attenuated antigen of the pathogen is phagocytosed and disintegrated by macrophages, responsible for ingesting dangerous microorganisms.
The peptides created by the protein breakdown of the infectious microorganism are “exposed” in the macrophage membrane. We won’t go into all the technical details of the process, as it’s enough for us to understand that a “cascade” is produced which stimulates the synthesis and specialization of the different types of lymphocytes.
The general key is that, in a vaccine, an attenuated form of the pathogen is usually inoculated into the body. Thus, the patient’s immune system recognizes it and, when the real danger enters the body, this mechanism can already respond quickly on two different fronts:
- Neutralizing the infectious agent before it can enter the cells of the body. Remember that viruses require the host’s cellular machinery to multiply. If viruses are removed before they enter them, the infection is cut directly.
- Recognizing and destroying cells that have been infected. Even if some cells are infected, if they are eliminated quickly, and general illness is avoided.
Some vaccine milestones
Unfortunately, the term “vaccine” has a certain negative social connotation today, as ignorance generates fear and, sometimes, certain people or groups can take advantage of it. To eliminate mistrust, we’re going to bring you some data that underlines the importance of these immunization mechanisms throughout history.
- Thanks to vaccines, the last case of smallpox in the world was registered in 1977. In 1980, the World Health Organization (WHO) declared the Earth free of smallpox.
- On August 25, 2020, the WHO declared Africa free of the wild poliovirus. With more than 9 billion doses, 1.8 million serious cases have been prevented.
- In 2015, thanks to the MMR triple viral vaccine, the Americas were pronounced rubella-free.
- The global mortality of the measles virus has been reduced by 80% thanks to vaccination.
As you can see, immunization is undoubtedly positive for world society. The World Health Organization and other sources say that vaccines prevent about 60 deaths per hour.
The 4 types of vaccines
Now you know what vaccines are capable of, when they were discovered, and how they work. We’re now going to look at the information provided by the Vaccines.gov portal to bring you the 4 types of vaccines that currently exist.
1. Live attenuated vaccines

Live attenuated vaccines are the ones that first come to mind when exploring this topic. They’re the ones that contain a complete version of the pathogenic microorganism, but in a weakened form.
Thanks to this, they’re able to stimulate an exact and safe immune response in the patient, since their inoculation doesn’t cause disease in healthy people.
This “weakening” occurs through genetic modification, according to the Vaccine Knowledge Project. This can either be natural or engineered by medical professionals, but one of the most common methods of obtaining it is through consecutive cell cultures.
For example, chicken embryos can be used for several viral generations to replicate in them. With each generation, the virus mutates (unconsciously) towards the specialization in chickens and, therefore, it loses pathogenicity towards us. Over time (up to 200 passes) the pathogen will lose its ability to replicate in human cells.
There are many advantages reported by this method of obtaining immunity by live attenuated vaccines. Among them, we find the following:
- It activates all the phases of the immune response in humans and provides a long-lasting response.
- These vaccines are easy to transport and their production cost is low (due to their general simplicity).
- With one or two doses, most live attenuated vaccines are capable of protecting the patient for life.
Unfortunately, this methodology also carries its risks. In immunosuppressed people, the weakened virus may still be able to infect them, with potentially serious effects. Furthermore, natural mutations throughout cultures may also cause the virus to revert to virulence.
A clear example of a live attenuated vaccine is the MMR vaccine, which provides protection against rubella, mumps and measles together. Thanks to it, the incidence of measles is less than 1% of the world population.
2. Inactivated vaccines
Talking about “life” in viruses is complex, since they don’t even have a cell, which is the minimum requirement to consider something to be living. Rather, they are protein capsids that contain within them DNA or RNA, capable of replicating themselves when they enter a host cell.
In the case of inactivated vaccines, a “dead” version of the germ is used, which is usually inactivated with the application of heat or exposure to certain chemicals (such as formalin). The microorganism is unable to replicate in the host, but its antigens are preserved and, therefore, macrophages are able to recognize it.
As you can imagine, these vaccines are used to immunize against very dangerous viruses and pathogens, such as those that cause hepatitis A, polio or rabies. If the pathogen is dead, the possibility of causing an infection is completely eliminated, but unfortunately, the immune response is weaker.
For this reason, several doses of vaccination (or booster vaccines) are usually necessary to maintain immunity in the patient in the long term. As indicated by the Historyofvaccines.orgportal, you get a lesser effect in exchange for zero danger.
3. Subunit, recombinant, polysaccharide, and combination vaccines
Here we’re talking about a heterogeneous group, because, in this case, parts of the pathogen are used to generate immunity, but never the entire microorganism. For example, specific proteins can be isolated from the germ, and they can act as antigens on their own, thus obviating the need to inoculate the pathogen in its entirety.
A very curious type of vaccine is one that is synthesized thanks to genetic engineering. Using recombination techniques, the genomic sequences of the virus that encode the antigen can be inserted into other pathogens or cells (yeast, for example), which are the ones that are inoculated. This method is known as genetic recombination.
Because they aren’t usually as effective as live attenuated vaccines, adjuvants to subunit or polysaccharide vaccines are sometimes necessary. These help to strengthen the immune response and promote the memory mechanism for a longer time, and are often the cause of annoying local reactions.
The hepatitis B virus, the pertussis virus, the human papilloma virus (HPV) or the shingles virus are fought with vaccines of this category.
4. Toxoid vaccines
Last (but not least) we find toxoid vaccines. These vaccines contain toxins or chemical compounds produced by the bacteria or virus against which you want to immunize. A very clear example of the usefulness of this vaccine is that of tetanus, as the dangerous thing here is the toxin that Clostridium tetani produces, not the organism itself.
Thus, in this case, the toxin (tetanospasmin) can be inactivated by chemical treatment, which allows its inoculation without the patient suffering from the effects. The immune system recognizes this toxic agent in future exposures and is, therefore, able to respond quickly when the time comes.
Going beyond the myths
As you may have seen, vaccine creation is easy to understand and can be summarized in a few lines. Sometimes weakened pathogens are used, other times dead organisms are used, and, exceptionally, germ toxins or key subunits that elicit the immune system response are also used.
Be that as it may, the premise is always the same: to accustom the body to the pathogen with non-dangerous methods, so that our immune cells know how to respond at the right time. Vaccines are approved by government bodies (such as the European Medicines Agency), so there is nothing to fear when it comes to undergoing vaccination.
- Contagious diseases in the United States from 1888 to the present. N. Engl. J. Med. 2013;369:2152–2158
- Vacuna, Clínica Universidad Navarra. Recogido a 11 de abril en https://www.cun.es/diccionario-medico/terminos/vacuna#:~:text=f.,bien%20un%20producto%20de%20s%C3%ADntesis.
- Ginglen, J. G., & Doyle, M. Q. (2017). Immunization.
- 10 datos sobre la inmunización, OMS. Recogido a 11 de abril en https://www.who.int/es/news-room/facts-in-pictures/detail/immunization
- Tipos de vacunas, vaccines.gov. Recogido a 11 de abril en https://www.vaccines.gov/es/b%C3%A1sicos/tipos
- Types of vaccine, vk. Recogido a 11 de abril en https://vk.ovg.ox.ac.uk/vk/types-of-vaccine
- Diferentes tipos de vacunas, Historyofvaccines. Recogido a 11 de abril en https://www.historyofvaccines.org/es/contenido/articulos/diferentes-tipos-de-vacunas
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







