Why Do Joints Crack?

Joint cracking is a common phenomenon, and we often hear about certain health problems it may be associated with. So, why do joints crack? Find out all about it here!
However, in the vast majority of cases, it doesn’t have clinical significance, despite the fact that there are some pathologies that can occur when pain appears during the cracking.
Are you interested in getting to know a little more about the subject? We’ve prepared a short article for you to answer the most frequent questions about this subject. Keep reading!
The origin of joint cracking
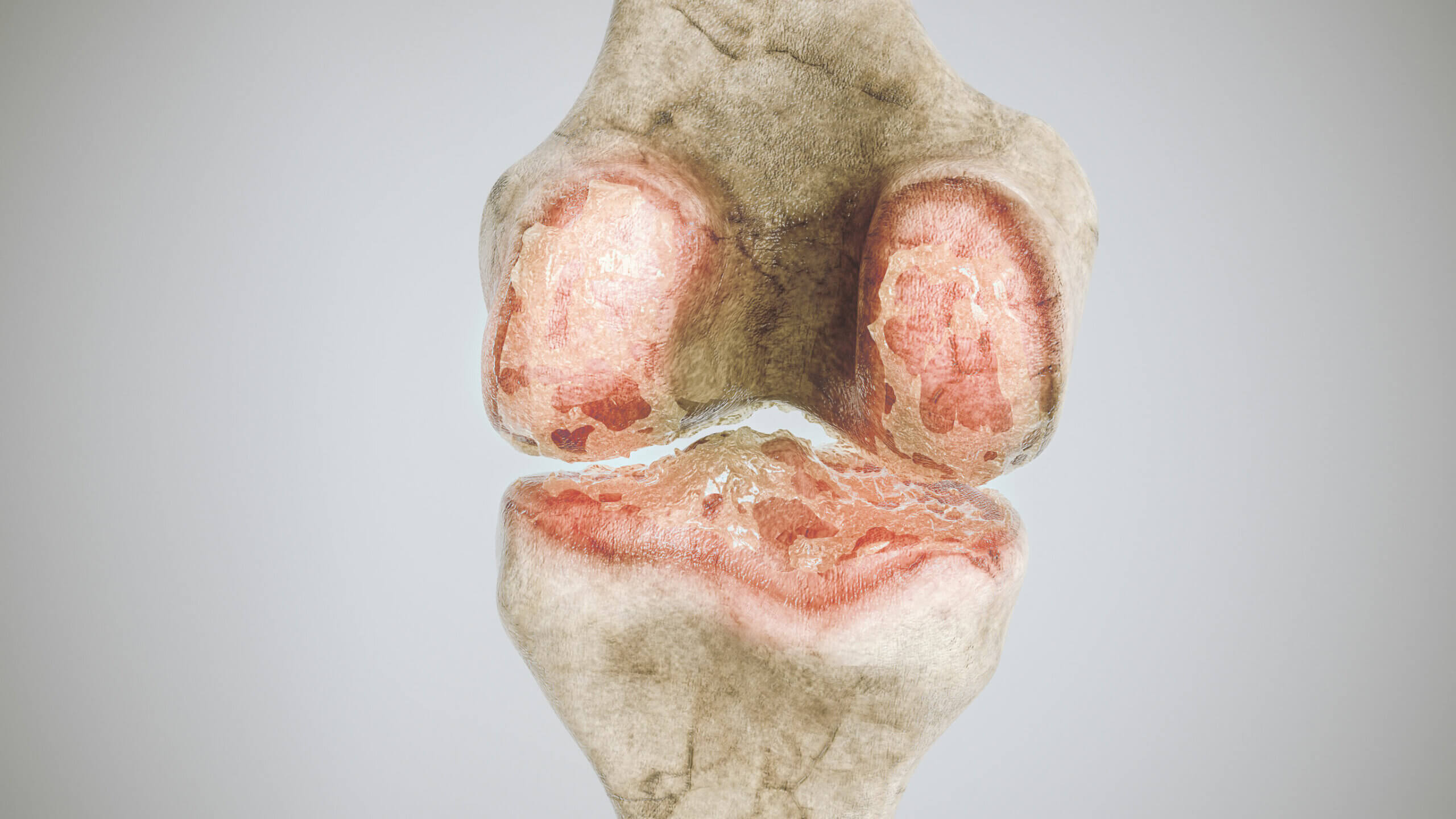
Joints, as you’ll see a little later, contain fluid inside them. These, by their nature, are exposed to constant pressure changes as a result of their mobilization, especially those that are more flexible.
When stretching or pressing on these structures it’s possible that you’ll hear a characteristic crack, which is usually painless. This is simply the physical phenomenon of cavitation, which can also be reproduced on a large scale.
This occurs because the molecules that are suspended in the synovial fluid reach a certain vapor pressure, which is why they temporarily change to a gaseous state, producing small bubbles. When these collide with any of the walls of the joint, they burst and produce the characteristic sound.
After that, the molecules involved return to their original liquid state and aren’t capable of undergoing the cavitation process for a certain period of time, which is determined by their physicochemical characteristics. That’s why this cracking of the joints, in most cases, doesn’t repeat until around 20 minutes have passed.
Joint anatomy
Joints are anatomical areas where two bones communicate with each other. They’re vital in order to guarantee the proper functioning of the locomotor system, and, according to their structural characteristics, they’re divided into three types: cartilaginous, fibrous, and synovial. It’s the latter one that we’re going to refer to now.
Synovial fluid and membrane
The innermost part of the joints is occupied by synovial fluid. This is yellowish in color, and has a chemical composition similar to that of blood plasma, although there are important differences. For example, the number of some proteins and cells is fewer in synovial fluid.
This fluid is produced by a structure called the synovial membrane, which covers the joint capsule. This liquid is responsible for allowing the free movement of the joint, as well as for cushioning any type of damage that these structures may suffer from external factors.
It’s within this synovial fluid that gas bubbles are formed during the cavitation process. There isn’t enough evidence to support the idea that the constant creaking of the joints can damage any of these anatomical areas.
Other structures
Some joints have a small piece of cartilaginous tissue that lines the surface of the bones. This is called articular cartilage and is vital in order to ensure proper displacement of the synovial joints.
In their external part, the joints are characterized by the presence of strong ligaments, tendons, and muscles that allow the bone surfaces to adhere to each other, guaranteeing stability.
Can the creaking of the joints be pathological?
In the vast majority of cases, as it is a natural physical phenomenon, there’s no relationship with pathologies.
However, it’s possible that, if pain occurs, the affected person will experience degenerative or inflammatory disorders in the joints, or even defects in the connective tissue.
Some of these conditions are osteoarthritis, synovitis, and Ehler-Danlos syndrome. Here’s a summary of them.
Osteoarthritis
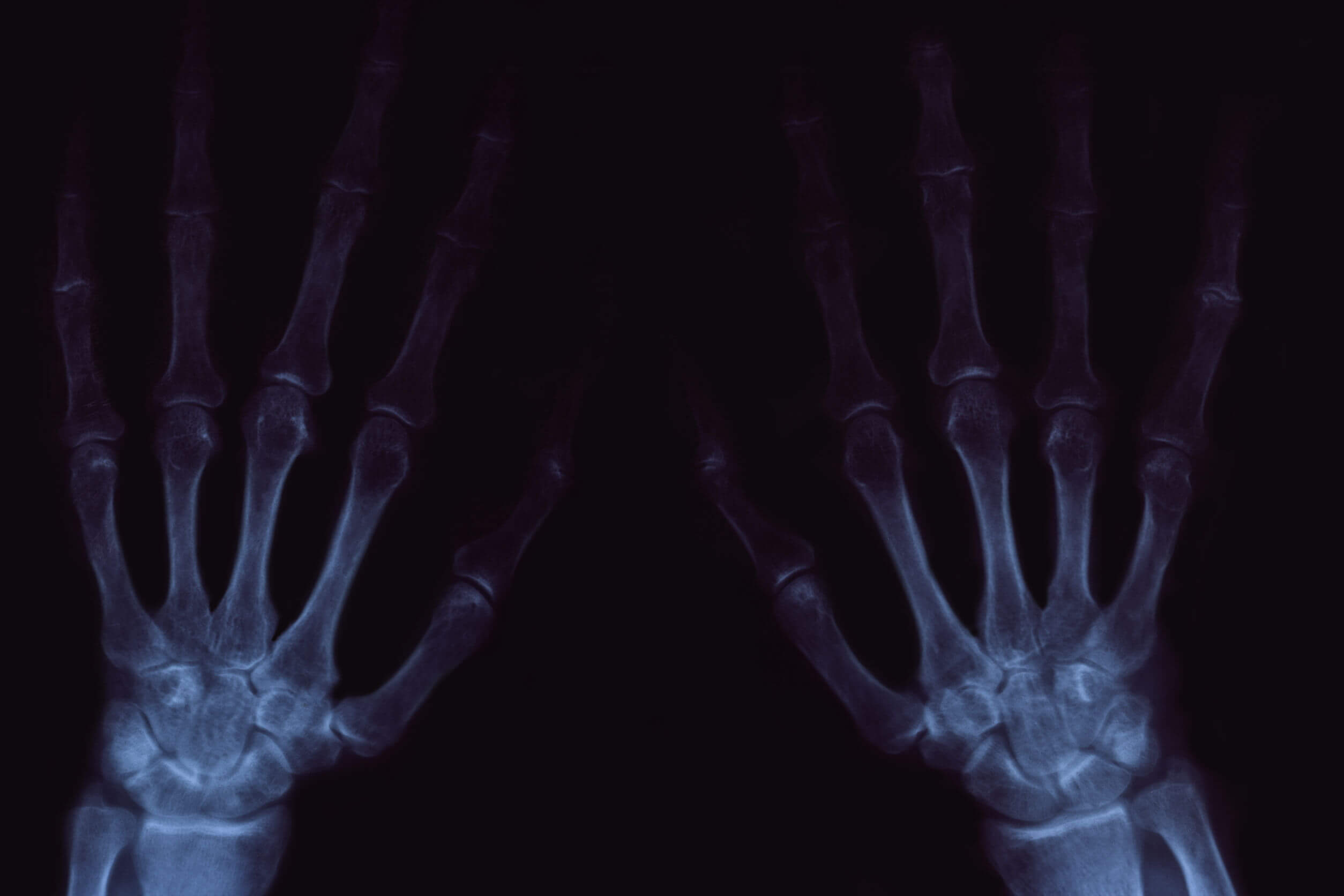
This is a degenerative condition of the joints, the incidence of which increases considerably with age. It can affect a large number of joints, regardless of size.
From a clinical point of view, the most prominent aspect is joint pain. This may be accompanied by stiffness and occasional bulking.
At the radiological level, it’s possible to show some structures called osteophytes, bony protrusions that usually develop at the ends of the bones.
Despite its degenerative component, there’s also a clear inflammatory process that explains the symptoms. Therefore, many patients may benefit from treatment with non-steroidal anti-inflammatory drugs, such as ibuprofen.
Synovitis and cracking joints
This is the inflammation of the synovium. It can occur in isolation or as a result of other inflammatory conditions in the same area, such as rheumatoid arthritis. It’s characterized by the appearance of abrupt pain and an increase in volume in the affected joint.
Other diseases that can be accompanied by synovitis are tendinitis, gout, lupus, and the same osteoarthritis that we discussed in the previous section.
Ehler-Danlos syndrome
Unlike the previous ones, this disease is characterized by the fact that it affects the correct functioning of the connective tissue. This tissue is found in a large number of organs, and allows support and communication between various structures. Joints, for example, contain abundant connective tissue.
According to a publication from Mayo Clinic, affected patients tend to have hypermobility in the joints, in addition to great flexibility in any part of the skin surface. The fragility of the skin is also very characteristic, and, in many cases, they tend to suffer from involuntary injuries such as bruises.
Its origin is genetic, and several mutations responsible for the disease have been discovered. In some cases, as blood vessels also contain abundant connective tissue in their walls, patients are at risk of rupturing some of the most important arteries for the body.
When to go to a doctor?
As we mentioned before, the cracking of the joints isn’t connected to a disease, as long as there’s no associated pain. Until now, no relationship has been identified between this habit and the incidence of joint diseases, despite the fact that, in general, professionals don’t recommend that you consciously crack your joints.
If there’s pain, then there may be an underlying disease. This is more likely if there are symptoms such as joint stiffness, swelling, or a rise in temperature. In these cases, it’s advisable to go to a specialist in medical diseases of the musculoskeletal system: the rheumatologist.
If you require a medical evaluation, unless you experience any alarming symptoms, it’s advisable to ask for an appointment in advance. If you’re not able to see a rheumatologist, there are several specialists who can address your problem in its initial stages, such as family doctors and internists.
Joint cracking is a common phenomenon, and we often hear about certain health problems it may be associated with. So, why do joints crack? Find out all about it here!
However, in the vast majority of cases, it doesn’t have clinical significance, despite the fact that there are some pathologies that can occur when pain appears during the cracking.
Are you interested in getting to know a little more about the subject? We’ve prepared a short article for you to answer the most frequent questions about this subject. Keep reading!
The origin of joint cracking

Joints, as you’ll see a little later, contain fluid inside them. These, by their nature, are exposed to constant pressure changes as a result of their mobilization, especially those that are more flexible.
When stretching or pressing on these structures it’s possible that you’ll hear a characteristic crack, which is usually painless. This is simply the physical phenomenon of cavitation, which can also be reproduced on a large scale.
This occurs because the molecules that are suspended in the synovial fluid reach a certain vapor pressure, which is why they temporarily change to a gaseous state, producing small bubbles. When these collide with any of the walls of the joint, they burst and produce the characteristic sound.
After that, the molecules involved return to their original liquid state and aren’t capable of undergoing the cavitation process for a certain period of time, which is determined by their physicochemical characteristics. That’s why this cracking of the joints, in most cases, doesn’t repeat until around 20 minutes have passed.
Joint anatomy
Joints are anatomical areas where two bones communicate with each other. They’re vital in order to guarantee the proper functioning of the locomotor system, and, according to their structural characteristics, they’re divided into three types: cartilaginous, fibrous, and synovial. It’s the latter one that we’re going to refer to now.
Synovial fluid and membrane
The innermost part of the joints is occupied by synovial fluid. This is yellowish in color, and has a chemical composition similar to that of blood plasma, although there are important differences. For example, the number of some proteins and cells is fewer in synovial fluid.
This fluid is produced by a structure called the synovial membrane, which covers the joint capsule. This liquid is responsible for allowing the free movement of the joint, as well as for cushioning any type of damage that these structures may suffer from external factors.
It’s within this synovial fluid that gas bubbles are formed during the cavitation process. There isn’t enough evidence to support the idea that the constant creaking of the joints can damage any of these anatomical areas.
Other structures
Some joints have a small piece of cartilaginous tissue that lines the surface of the bones. This is called articular cartilage and is vital in order to ensure proper displacement of the synovial joints.
In their external part, the joints are characterized by the presence of strong ligaments, tendons, and muscles that allow the bone surfaces to adhere to each other, guaranteeing stability.
Can the creaking of the joints be pathological?
In the vast majority of cases, as it is a natural physical phenomenon, there’s no relationship with pathologies.
However, it’s possible that, if pain occurs, the affected person will experience degenerative or inflammatory disorders in the joints, or even defects in the connective tissue.
Some of these conditions are osteoarthritis, synovitis, and Ehler-Danlos syndrome. Here’s a summary of them.
Osteoarthritis

This is a degenerative condition of the joints, the incidence of which increases considerably with age. It can affect a large number of joints, regardless of size.
From a clinical point of view, the most prominent aspect is joint pain. This may be accompanied by stiffness and occasional bulking.
At the radiological level, it’s possible to show some structures called osteophytes, bony protrusions that usually develop at the ends of the bones.
Despite its degenerative component, there’s also a clear inflammatory process that explains the symptoms. Therefore, many patients may benefit from treatment with non-steroidal anti-inflammatory drugs, such as ibuprofen.
Synovitis and cracking joints
This is the inflammation of the synovium. It can occur in isolation or as a result of other inflammatory conditions in the same area, such as rheumatoid arthritis. It’s characterized by the appearance of abrupt pain and an increase in volume in the affected joint.
Other diseases that can be accompanied by synovitis are tendinitis, gout, lupus, and the same osteoarthritis that we discussed in the previous section.
Ehler-Danlos syndrome
Unlike the previous ones, this disease is characterized by the fact that it affects the correct functioning of the connective tissue. This tissue is found in a large number of organs, and allows support and communication between various structures. Joints, for example, contain abundant connective tissue.
According to a publication from Mayo Clinic, affected patients tend to have hypermobility in the joints, in addition to great flexibility in any part of the skin surface. The fragility of the skin is also very characteristic, and, in many cases, they tend to suffer from involuntary injuries such as bruises.
Its origin is genetic, and several mutations responsible for the disease have been discovered. In some cases, as blood vessels also contain abundant connective tissue in their walls, patients are at risk of rupturing some of the most important arteries for the body.
When to go to a doctor?
As we mentioned before, the cracking of the joints isn’t connected to a disease, as long as there’s no associated pain. Until now, no relationship has been identified between this habit and the incidence of joint diseases, despite the fact that, in general, professionals don’t recommend that you consciously crack your joints.
If there’s pain, then there may be an underlying disease. This is more likely if there are symptoms such as joint stiffness, swelling, or a rise in temperature. In these cases, it’s advisable to go to a specialist in medical diseases of the musculoskeletal system: the rheumatologist.
If you require a medical evaluation, unless you experience any alarming symptoms, it’s advisable to ask for an appointment in advance. If you’re not able to see a rheumatologist, there are several specialists who can address your problem in its initial stages, such as family doctors and internists.
- Blanco FJ, Fernández Sueiro JL. Artrosis: concepto, clasificación y epidemiología, patogenia. En Pascual E. et al, eds. Reumatología. Editorial ARAN 1998: pp:1609-42.
- Hembrow CH. Symposium. Manipulative treatment. Med J Aust. 1967;
1(25):1274-1280. Cited by: Heilig D. The thrust technique. J Am Osteopath
Assoc. 1981;81:247. - Meal GM, Scott RA. Analysis of the joint crack by simultaneous recording
of sound and tension. J Manipulative Physiol Ther. 1986;9(3):189-195. - Pérez M. Artritis y artrosis, clínica y tratamiento. Farmacia Profesional 2003;17(11):50-54.
- Protapapas M, et al. Joint cracking and popping: Understanding noises
that accompany articular release. JAOA 2002;102(5):283-287. - Suárez S. Enfermedad articular. Farmacia Profesional 2000;14(3)72-9.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







