What Is Thrush or Oral Candidiasis?
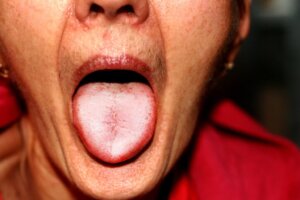
Oral thrush is often an underestimated condition and one that can be difficult for patients to diagnose. Normally, when a person thinks about infections, they do so in relation to bacteria and viruses; and not as much in regard to fungi. Although it’s true that they’re less frequent in comparison, fungal infections are also frequent. With that in mind, we want to tell you everything you need to know about oral candidiasis.
This fungal infection is also known as oropharyngeal candidiasis, thrush, or oral thrush. It’s not usually associated with major complications, but it can cause discomfort in patients. Knowing the symptoms and prevention systems is useful to avoid these episodes. We’ll teach you everything you need to know about oral candidiasis, with an emphasis on its symptoms and prevention.
What is oral thrush?
Oral candidiasis is a fungal infection of the oral cavity first described in 1838 by the pediatrician François Veilleux. Specifically, the infection is caused by the Candida fungus, almost always by the species Candida albicans. However, other species such as C. krusei, C. tropicalis, and C. glabrata can also cause episodes in older adults.
As the Centers for Disease Control and Prevention (CDC) remind us, the fungus, popularly known as yeast, lives under normal conditions on the surface of the skin, mouth, throat, intestine, and vagina. It does so without causing major problems, although under certain circumstances, it can multiply and cause infection.
This condition on its own is harmless and doesn’t cause pain, but it can be very uncomfortable for the patient and deteriorate their well-being. For reasons that we’ll explain shortly, it’s more common in babies from 4 weeks to 6 months and in older adults. It’s characterized by white plaques in the oral cavity, which can sometimes extend into the esophagus.
The symptoms of oral thrush
Oral candidiasis infection can have many symptoms, although almost all of them are focused on the oral cavity. Here are the most significant:
- Raised white areas on the surface of the tongue, cheeks, gums, tonsils, and palate
- A cottony feeling in the mouth
- Cracks in the tongue and redness in the corners of the mouth
- Loss of taste
- Fever and painful swallowing, especially when the infection spreads beyond the esophagus
The causes of oral thrush

The fungus inhabits all human beings, although the immune system generally keeps its population under control. It’s for this reason that infections are so common in babies, as their immune systems are still getting stronger. The same applies to elderly patients, two groups in which oral candidiasis is more common.
At the same time, and as experts point out, candidiasis in the mouth is also common in patients with immunosuppression. For example, those who’ve undergone cancer therapy or have HIV infection. We also know that the use of antibiotics and oral corticosteroids can lead to an infection of this type.
In the case of babies, they can contract the fungus through the mother’s birth canal, or through breastfeeding with the interaction of the nipple.
The most common risk factors in any age group are:
- Wearing dentures
- Suffering from diabetes
- Following a treatment that causes dry mouth
- Smoking
- Poor oral hygiene
- High concentrations of sugar and yeast in the diet
- Poor hygiene regarding inhalers, in the case of patients with asthma and COPD
- Patients who’ve undergone recent surgery
- Suffering from kidney failure
In episodes where oral yeast infection progresses into the esophagus and beyond, they usually focus only on people with severely compromised immune systems. In general, having a weak immune system is considered the main trigger for oral thrush.
Diagnosis and treatment options

The diagnosis of thrush is made on the basis of a sample with a sterile cotton swab. This will be analyzed in a laboratory to determine if it corresponds to an infection of this type.
If the doctor confirms or suspects that it has reached the esophagus, an endoscopy can be performed to rule out the condition. As it’s a very characteristic infection, most experts can diagnose it by looking inside the mouth.
Fortunately, yeast infection is an easy infection to treat in healthy babies and adults. In general, doctors decide to prescribe antifungals for a period of 10-15 days. These can be distributed in pills, tablets, liquid, ointments, or any other presentation.
The symptoms and the infection disappear in this period, during which the patient can opt for home treatments to alleviate the oral symptoms.
Infection in patients with compromised immune systems may be more difficult to treat. Antifungals are also chosen, although treatment can be prolonged for more days and be more aggressive. In conjunction with this, the following should be taken into account:
- Modify the diet in case you feel discomfort when swallowing (avoid spicy and hot foods).
- Implement regular oral hygiene.
- Increase the intake of probiotics in the diet.
- Disinfect objects that regularly come into contact with the mouth. This includes dentures and inhalers.
- Exercise and avoid stressful situations.
If this is the case, the condition that caused the infection will be treated, or in any case, controlled. Many conditions can share symptoms with those of oral thrush. The possibility that these respond to cold sores, esophagitis, pharyngitis, oral hairy leukoplakia, aphthous stomatitis, and perioral dermatitis, among others, should be assessed.
Oral thrush is often an underestimated condition and one that can be difficult for patients to diagnose. Normally, when a person thinks about infections, they do so in relation to bacteria and viruses; and not as much in regard to fungi. Although it’s true that they’re less frequent in comparison, fungal infections are also frequent. With that in mind, we want to tell you everything you need to know about oral candidiasis.
This fungal infection is also known as oropharyngeal candidiasis, thrush, or oral thrush. It’s not usually associated with major complications, but it can cause discomfort in patients. Knowing the symptoms and prevention systems is useful to avoid these episodes. We’ll teach you everything you need to know about oral candidiasis, with an emphasis on its symptoms and prevention.
What is oral thrush?
Oral candidiasis is a fungal infection of the oral cavity first described in 1838 by the pediatrician François Veilleux. Specifically, the infection is caused by the Candida fungus, almost always by the species Candida albicans. However, other species such as C. krusei, C. tropicalis, and C. glabrata can also cause episodes in older adults.
As the Centers for Disease Control and Prevention (CDC) remind us, the fungus, popularly known as yeast, lives under normal conditions on the surface of the skin, mouth, throat, intestine, and vagina. It does so without causing major problems, although under certain circumstances, it can multiply and cause infection.
This condition on its own is harmless and doesn’t cause pain, but it can be very uncomfortable for the patient and deteriorate their well-being. For reasons that we’ll explain shortly, it’s more common in babies from 4 weeks to 6 months and in older adults. It’s characterized by white plaques in the oral cavity, which can sometimes extend into the esophagus.
The symptoms of oral thrush
Oral candidiasis infection can have many symptoms, although almost all of them are focused on the oral cavity. Here are the most significant:
- Raised white areas on the surface of the tongue, cheeks, gums, tonsils, and palate
- A cottony feeling in the mouth
- Cracks in the tongue and redness in the corners of the mouth
- Loss of taste
- Fever and painful swallowing, especially when the infection spreads beyond the esophagus
The causes of oral thrush

The fungus inhabits all human beings, although the immune system generally keeps its population under control. It’s for this reason that infections are so common in babies, as their immune systems are still getting stronger. The same applies to elderly patients, two groups in which oral candidiasis is more common.
At the same time, and as experts point out, candidiasis in the mouth is also common in patients with immunosuppression. For example, those who’ve undergone cancer therapy or have HIV infection. We also know that the use of antibiotics and oral corticosteroids can lead to an infection of this type.
In the case of babies, they can contract the fungus through the mother’s birth canal, or through breastfeeding with the interaction of the nipple.
The most common risk factors in any age group are:
- Wearing dentures
- Suffering from diabetes
- Following a treatment that causes dry mouth
- Smoking
- Poor oral hygiene
- High concentrations of sugar and yeast in the diet
- Poor hygiene regarding inhalers, in the case of patients with asthma and COPD
- Patients who’ve undergone recent surgery
- Suffering from kidney failure
In episodes where oral yeast infection progresses into the esophagus and beyond, they usually focus only on people with severely compromised immune systems. In general, having a weak immune system is considered the main trigger for oral thrush.
Diagnosis and treatment options

The diagnosis of thrush is made on the basis of a sample with a sterile cotton swab. This will be analyzed in a laboratory to determine if it corresponds to an infection of this type.
If the doctor confirms or suspects that it has reached the esophagus, an endoscopy can be performed to rule out the condition. As it’s a very characteristic infection, most experts can diagnose it by looking inside the mouth.
Fortunately, yeast infection is an easy infection to treat in healthy babies and adults. In general, doctors decide to prescribe antifungals for a period of 10-15 days. These can be distributed in pills, tablets, liquid, ointments, or any other presentation.
The symptoms and the infection disappear in this period, during which the patient can opt for home treatments to alleviate the oral symptoms.
Infection in patients with compromised immune systems may be more difficult to treat. Antifungals are also chosen, although treatment can be prolonged for more days and be more aggressive. In conjunction with this, the following should be taken into account:
- Modify the diet in case you feel discomfort when swallowing (avoid spicy and hot foods).
- Implement regular oral hygiene.
- Increase the intake of probiotics in the diet.
- Disinfect objects that regularly come into contact with the mouth. This includes dentures and inhalers.
- Exercise and avoid stressful situations.
If this is the case, the condition that caused the infection will be treated, or in any case, controlled. Many conditions can share symptoms with those of oral thrush. The possibility that these respond to cold sores, esophagitis, pharyngitis, oral hairy leukoplakia, aphthous stomatitis, and perioral dermatitis, among others, should be assessed.
- Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. Oral thrush: Overview. 2012 Apr 26 [Updated 2019 Aug 15].
- Wilson, M., & Wilson, P. J. Oral Thrush. In Close Encounters of the Microbial Kind. 2021; 321-331.
- Taylor M, Raja A. Candidiasis oral. StatPearls [Internet]. Treasure Island (FL). 2021.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







