What Is Pulmonary Embolism?

When a blood clot appears in one of the main arteries of the lung it’s called a pulmonary embolism. This disease affects around 1 in 1,000 people, according to a report by the US Centers for Disease Control and Prevention.
This pathology is considered a cardiovascular disease. It can lower oxygen levels in the blood and, if not treated in time, causes permanent lung damage and even death.
Symptoms of pulmonary embolism

Pulmonary embolisms prevent the lung from receiving the blood that it must replenish with oxygen and then pump it to the heart. The heart, in turn, is responsible for distributing oxygen to the rest of the body. Therefore, it isn’t only the lungs that are involved in a pulmonary embolism, as the heart and other vital organs can be affected too.
Some of the signs of pulmonary embolism are as follows:
- Shortness of breath, which can be sudden
- Chest pain, which may be worse when inhaled
- A high heart rate
- Accelerated breathing
- Dizziness
- Cough, which is usually dry and can cause bleeding
- Wheezing
- Bluish lips and fingers (cyanosis)
When the disease becomes severe, it can lead to shock, cardiac arrest, loss of consciousness, or death. The severity of the disease is measured by the volume of the pulmonary embolism.
However, even if the pulmonary embolism is small, it’s still considered an emergency, as it can cause a pulmonary infarction.
Causes of pulmonary embolism
Although blood clots can be caused by several different reasons, they’re most often caused by deep vein thrombosis, a formation of clots in deep veins in the body. It usually starts in the legs or pelvis and travels to the blood vessels in the lungs.
Blood clots can be generated by various causes, and some of these could be the following:
- Injury or damage. When a muscle is injured or torn, or a bone is fractured, there’s a risk of damaging blood vessels and causing clots.
- Medical conditions. Some medical conditions or treatments may cause blood clots. For example, chemotherapy makes a person prone to them.
- Inactivity: When a person has long periods of inactivity, they can develop blood clots, whether they’re in bed recovering from an illness or spending many hours sitting down.
On the other hand, a study published in the Journal of Anaesthesiology Clinical Pharmacology revealed that, on rare occasions, a particle that enters the bloodstream can cause a pulmonary embolism.
Risk factors
Risk factors could include the following:
- Being a cancer patient
- Being overweight or obese
- A sedentary lifestyle
- Being over 60 years of age
- Having suffered a leg or hip fracture
- Having had a heart attack or stroke
- Taking testosterone or estrogen
- Suffering from a genetic blood clotting disorder
- Having inflammatory bowel disease
- Aa family member having suffered a pulmonary embolism.
Diagnosis
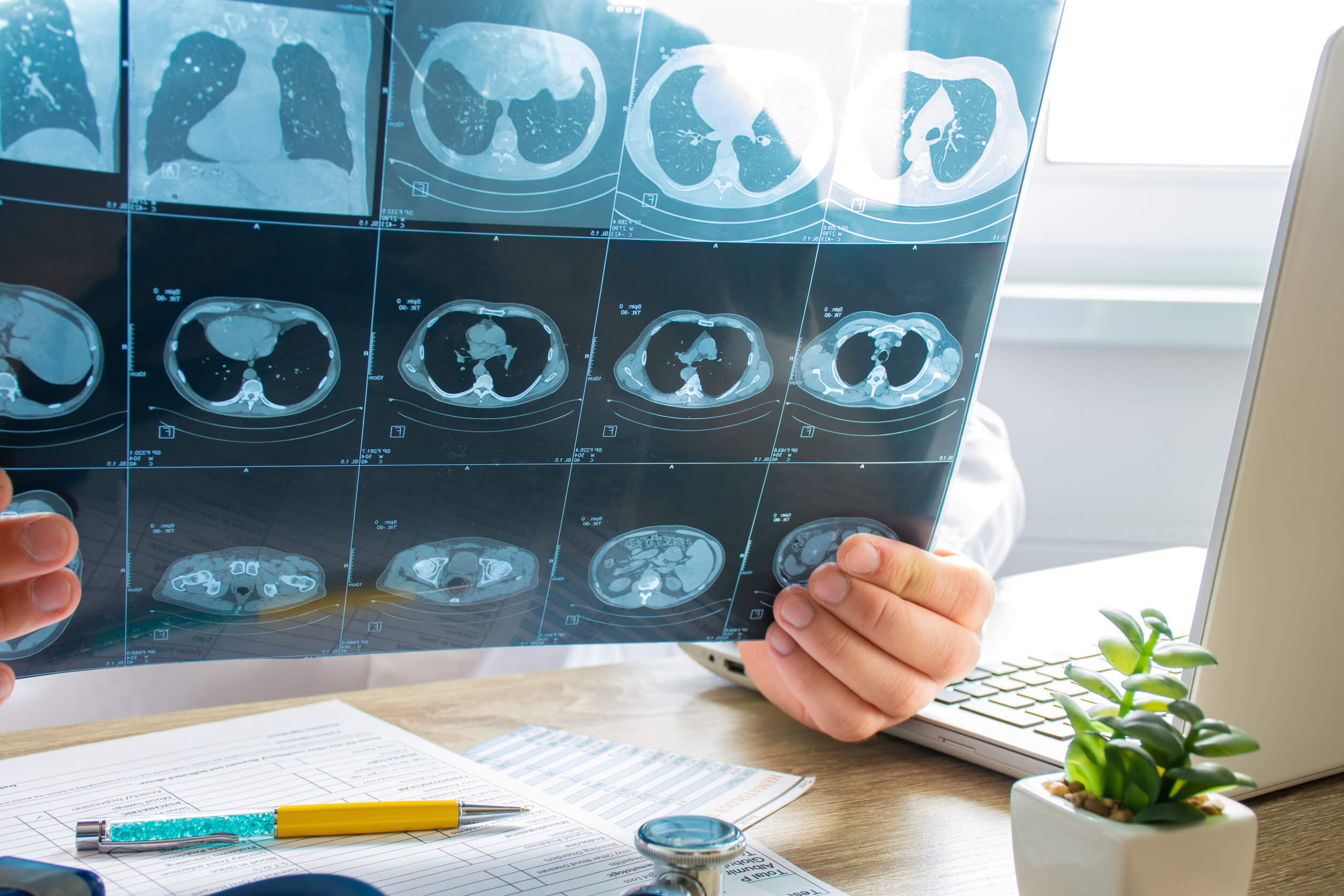
If you have heart disease, high blood pressure, or emphysema, it can be difficult to diagnose a pulmonary embolism. In general, the doctor will ask you some routine questions such as what you have felt or if you have a family member who has suffered from pulmonary embolism, among others. After that, they’ll perform some medical tests such as:
- Chest X-ray – the doctor will be able to take a closer look at the lungs and heart to see if there are any abnormalities
- Magnetic resonance
- Electrocardiograph
- Pulmonary angiography – this consists of an injection with a special dye and an x-ray to see if there’s a blood clot.
- Computed tomography
- Duplex venous ultrasound – this uses radio waves to rule out blood clots in the legs, probably related to pulmonary embolism
- Venography or venogram – this is an X-ray of the veins in the legs
- D-dimer test
Treatment of pulmonary embolism
Treatment will depend on the size and location of the pulmonary embolism. If it’s detected early, then the doctor may prescribe these medications:
- Anticoagulants: Such as heparin, warfarin, or arixtra. These are blood thinners that prevent clots from forming.
- Thrombolytics: Their function is to quickly dissolve a blood clot. Keep in mind that these medications are used only for emergencies, as their side effects could be dangerous.
Another way to remove blood clots is through surgery. Among the surgical procedures we have the following:
- Vena cava filter placement: This surgery is performed to prevent the blood clot from traveling from the leg to the lung, and a small incision will be made to insert a filter into the inferior vena cava.
- Open surgery: This type of surgery is only used if the person is in shock or the resources to dissolve the clot have been exhausted.
- Clot extraction: This involves inserting a catheter to suck out a blood clot that is lodged in an artery. It’s a difficult procedure, and so some doctors prefer other types of treatment.
After-care and follow-up
After your doctor treats your pulmonary embolism, they may prescribe some blood-thinning medications to prevent them from forming again. In addition, they’ll also recommend using compression measures to prevent blood from clotting in the legs.
If you have frequent pulmonary embolisms, you can easily develop a more serious condition such as pulmonary hypertension.
When a blood clot appears in one of the main arteries of the lung it’s called a pulmonary embolism. This disease affects around 1 in 1,000 people, according to a report by the US Centers for Disease Control and Prevention.
This pathology is considered a cardiovascular disease. It can lower oxygen levels in the blood and, if not treated in time, causes permanent lung damage and even death.
Symptoms of pulmonary embolism

Pulmonary embolisms prevent the lung from receiving the blood that it must replenish with oxygen and then pump it to the heart. The heart, in turn, is responsible for distributing oxygen to the rest of the body. Therefore, it isn’t only the lungs that are involved in a pulmonary embolism, as the heart and other vital organs can be affected too.
Some of the signs of pulmonary embolism are as follows:
- Shortness of breath, which can be sudden
- Chest pain, which may be worse when inhaled
- A high heart rate
- Accelerated breathing
- Dizziness
- Cough, which is usually dry and can cause bleeding
- Wheezing
- Bluish lips and fingers (cyanosis)
When the disease becomes severe, it can lead to shock, cardiac arrest, loss of consciousness, or death. The severity of the disease is measured by the volume of the pulmonary embolism.
However, even if the pulmonary embolism is small, it’s still considered an emergency, as it can cause a pulmonary infarction.
Causes of pulmonary embolism
Although blood clots can be caused by several different reasons, they’re most often caused by deep vein thrombosis, a formation of clots in deep veins in the body. It usually starts in the legs or pelvis and travels to the blood vessels in the lungs.
Blood clots can be generated by various causes, and some of these could be the following:
- Injury or damage. When a muscle is injured or torn, or a bone is fractured, there’s a risk of damaging blood vessels and causing clots.
- Medical conditions. Some medical conditions or treatments may cause blood clots. For example, chemotherapy makes a person prone to them.
- Inactivity: When a person has long periods of inactivity, they can develop blood clots, whether they’re in bed recovering from an illness or spending many hours sitting down.
On the other hand, a study published in the Journal of Anaesthesiology Clinical Pharmacology revealed that, on rare occasions, a particle that enters the bloodstream can cause a pulmonary embolism.
Risk factors
Risk factors could include the following:
- Being a cancer patient
- Being overweight or obese
- A sedentary lifestyle
- Being over 60 years of age
- Having suffered a leg or hip fracture
- Having had a heart attack or stroke
- Taking testosterone or estrogen
- Suffering from a genetic blood clotting disorder
- Having inflammatory bowel disease
- Aa family member having suffered a pulmonary embolism.
Diagnosis

If you have heart disease, high blood pressure, or emphysema, it can be difficult to diagnose a pulmonary embolism. In general, the doctor will ask you some routine questions such as what you have felt or if you have a family member who has suffered from pulmonary embolism, among others. After that, they’ll perform some medical tests such as:
- Chest X-ray – the doctor will be able to take a closer look at the lungs and heart to see if there are any abnormalities
- Magnetic resonance
- Electrocardiograph
- Pulmonary angiography – this consists of an injection with a special dye and an x-ray to see if there’s a blood clot.
- Computed tomography
- Duplex venous ultrasound – this uses radio waves to rule out blood clots in the legs, probably related to pulmonary embolism
- Venography or venogram – this is an X-ray of the veins in the legs
- D-dimer test
Treatment of pulmonary embolism
Treatment will depend on the size and location of the pulmonary embolism. If it’s detected early, then the doctor may prescribe these medications:
- Anticoagulants: Such as heparin, warfarin, or arixtra. These are blood thinners that prevent clots from forming.
- Thrombolytics: Their function is to quickly dissolve a blood clot. Keep in mind that these medications are used only for emergencies, as their side effects could be dangerous.
Another way to remove blood clots is through surgery. Among the surgical procedures we have the following:
- Vena cava filter placement: This surgery is performed to prevent the blood clot from traveling from the leg to the lung, and a small incision will be made to insert a filter into the inferior vena cava.
- Open surgery: This type of surgery is only used if the person is in shock or the resources to dissolve the clot have been exhausted.
- Clot extraction: This involves inserting a catheter to suck out a blood clot that is lodged in an artery. It’s a difficult procedure, and so some doctors prefer other types of treatment.
After-care and follow-up
After your doctor treats your pulmonary embolism, they may prescribe some blood-thinning medications to prevent them from forming again. In addition, they’ll also recommend using compression measures to prevent blood from clotting in the legs.
If you have frequent pulmonary embolisms, you can easily develop a more serious condition such as pulmonary hypertension.
- Centers for Disease Control and Prevention [Updated 2020 Feb 07]. Venous Thromboembolism (Blood Clots) – Data & Statistics. Available from: https://www.cdc.gov/ncbddd/dvt/data.html
- Centers for Disease Control and Prevention [Updated 2020 Feb 07]. Venous Thromboembolism (Blood Clots) – What is VTE?. Available from: https://www.cdc.gov/ncbddd/dvt/facts.html
- National Heart, Lung, and Blood Institute. Venous Thromboembolism. Available from: https://www.nhlbi.nih.gov/health-topics/venous-thromboembolism
- Kaur, K., Bhardwaj, M., Kumar, P., Singhal, S., Singh, T., & Hooda, S. (2016). Amniotic fluid embolism. Journal of anaesthesiology, clinical pharmacology, 32(2), 153–159. https://doi.org/10.4103/0970-9185.173356
- Scoville, E. A., Konijeti, G. G., Nguyen, D. D., Sauk, J., Yajnik, V., & Ananthakrishnan, A. N. (2014). Venous thromboembolism in patients with inflammatory bowel diseases: a case-control study of risk factors. Inflammatory bowel diseases, 20(4), 631–636. https://doi.org/10.1097/MIB.0000000000000007
- Sekhri, V., Mehta, N., Rawat, N., Lehrman, S. G., & Aronow, W. S. (2012). Management of massive and nonmassive pulmonary embolism. Archives of medical science : AMS, 8(6), 957–969. https://doi.org/10.5114/aoms.2012.32402
- Ucar E. Y. (2019). Update on Thrombolytic Therapy in Acute Pulmonary Thromboembolism. The Eurasian journal of medicine, 51(2), 186–190. https://doi.org/10.5152/eurasianjmed.2019.19291
- Chung, J., & Owen, R. J. (2008). Using inferior vena cava filters to prevent pulmonary embolism. Canadian family physician Medecin de famille canadien, 54(1), 49–55.
- Bĕlohlávek, J., Dytrych, V., & Linhart, A. (2013). Pulmonary embolism, part I: Epidemiology, risk factors and risk stratification, pathophysiology, clinical presentation, diagnosis and nonthrombotic pulmonary embolism. Experimental and clinical cardiology, 18(2), 129–138.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







