Vitiligo: Symptoms, Causes and Treatment

Nowadays, many celebrities have put all kinds of ailments in the public eye, with the aim of making people more aware, and promoting research. Some of the most prominent in recent years have been rosacea, lupus, and vitiligo.
Vitiligo is an autoimmune disease that affects people chronically. It’s characterized by causing progressive changes in skin pigmentation. For this reason, it doesn’t have a uniform appearance and, instead, it shows off patches of light color (which become more and more extensive).
According to an article published by the Spanish Association of Pediatrics (AEPED) on skin pigmentation disorders, vitiligo can affect anyone, regardless of complexion, sex, or age. Worldwide, it affects 1% of the population.
Likewise, the authors indicate that “the maximum incidence occurs in the third decade of life, 50% of cases occur before the age of 20”.
Symptoms
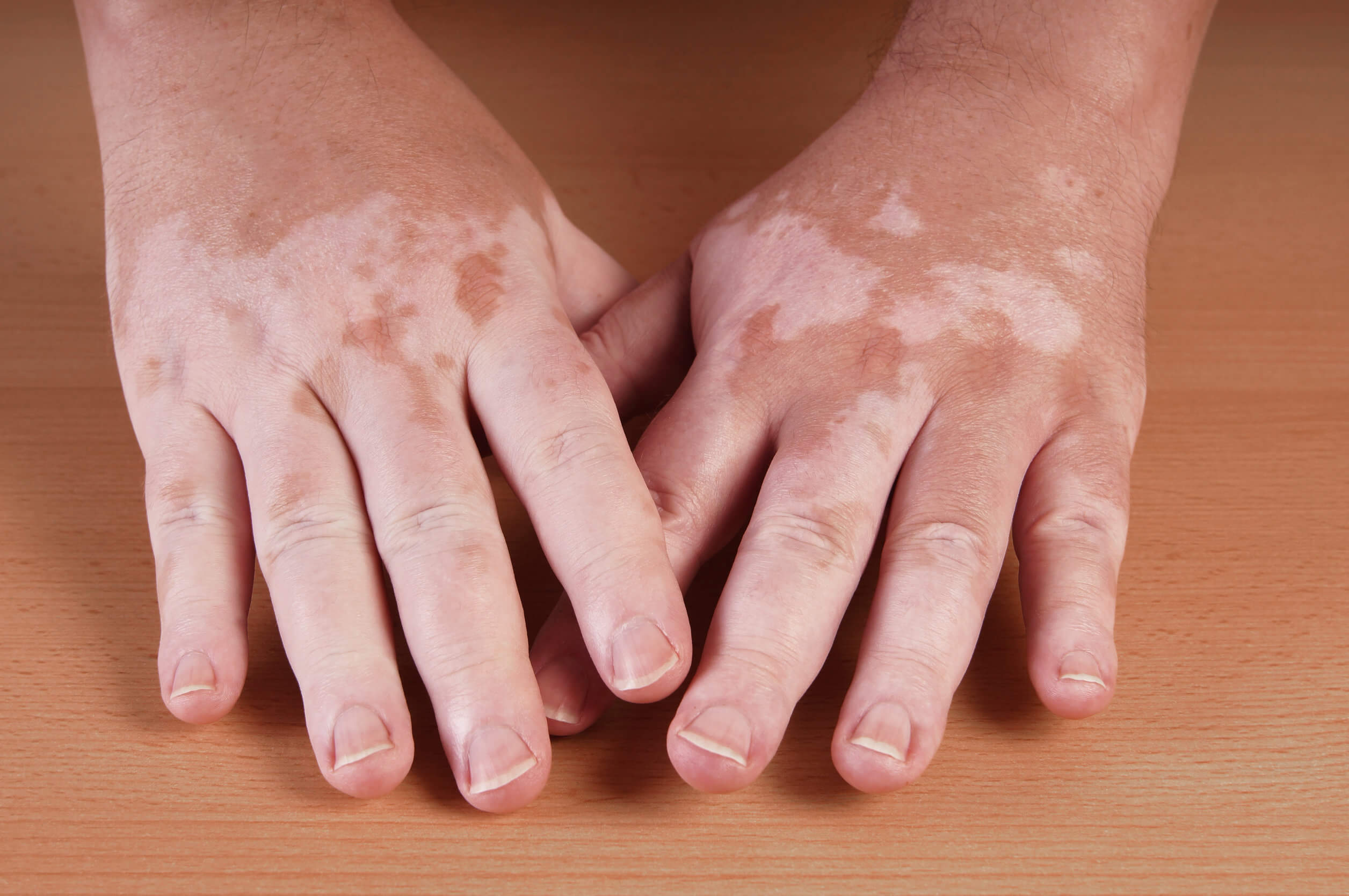
The most characteristic symptom of vitiligo is depigmentation of the skin. As the authors of the aforementioned article indicate, the lesions appear as white patches with well-defined borders. These can vary in size and, as the disease progresses, they can spread to cover other areas of the body.
The patches cover the body asymmetrically. The most affected areas are usually the hands and face, as well as the elbows, knees, armpits, groin folds, forearms, and genitals.
In addition to affecting the skin, mucous membranes, and even the retina, vitiligo can affect hair. Therefore, people with this disease may have different colored hair, facial hair (eyelashes, eyebrows, mustache, beard) and body hair (areas with white hair and areas with dark hair).
Other symptoms that may occur are the following:
- Itching and discomfort in the affected areas
- Premature graying of facial and other hair
Regarding the progression of the disease, it’s worth highlighting what was stated in an article published in the journal Dermatology, “the natural course of vitiligo is unpredictable. Sometimes there’s an abrupt onset, followed by a progression for an indeterminate time, and then a stability that can be from a short time to decades”.
Causes
Although vitiligo has been known for a long time, its cause hasn’t yet been established.
However, several hypotheses have been put forward that mainly involve autoimmune and genetic mechanisms, in combination with various triggers, such as a high level of emotional stress.
What must be taken into account is that it’s a disease that causes the cells that are responsible for producing melanin (that is, melanocytes), to suspend their function or die. This leads to progressive depigmentation.
“For experts in pigment cells, vitiligo represents an opportunity to study the basic biological mechanisms of the functions of melanocytes“, state authors such as Carmen Lucía Pimentel, Lluis Pug and Agustín Alomar.
Triggers
Although it hasn’t yet been possible to specify a cause, it has been possible to determine some triggers of vitiligo. Among them are the following:
- Viral infections
- High level of stress/chronic stress
- Severe sunburn
- Severe skin trauma
- Exposure to aggressive chemicals
Diagnosis

The diagnosis of vitiligo is primarily clinical. At the consultation and physical examination, the doctor can easily detect the patches (achromic macules) in the most typical locations. However, sometimes a more exhaustive review may be necessary and, in others, a skin biopsy may even be requested, although this isn’t very common.
When vitiligo occurs in young children, parents may confuse it with pityriasis alba. This is one of the scenarios in which differential diagnosis comes into play.
Other diseases that are considered when carrying out a differential diagnosis are achromic nevus, anemic nevus, and tuberous sclerosis.
Treatment
There’s no treatment that can reverse the disease or cure it. However, there are several options that help control symptoms and mitigate their impact on quality of life.
All vitiligo patients are advised to protect themselves from solar radiation on a daily basis to avoid burns and the aggravation of existing lesions. In order to do this, they shouldn’t only use adequate sunscreen, but they should also wear clothing that covers their skin and keeps it protected from other factors, such as wind, cold, and heat.
“The aim of any therapeutic modality is to regenerate the epidermal melanocytes in order to obtain a complete and permanent repigmentation of the affected areas”, indicates an article published in Elsevier.
To do this, you can resort to some topical corticosteroids (in pills or injections) and topical medications to control inflammation, among others. Again, these aren’t going to stop the progression of the disease, but they may help control symptoms.
Another popular treatment option is ultraviolet B phototherapy, as well as combining it with a plant-based substance called psoralen.
Regular check-ups and good communication with your doctor will be essential in order to make the necessary modifications in treatment and maintain quality of life.
Nowadays, many celebrities have put all kinds of ailments in the public eye, with the aim of making people more aware, and promoting research. Some of the most prominent in recent years have been rosacea, lupus, and vitiligo.
Vitiligo is an autoimmune disease that affects people chronically. It’s characterized by causing progressive changes in skin pigmentation. For this reason, it doesn’t have a uniform appearance and, instead, it shows off patches of light color (which become more and more extensive).
According to an article published by the Spanish Association of Pediatrics (AEPED) on skin pigmentation disorders, vitiligo can affect anyone, regardless of complexion, sex, or age. Worldwide, it affects 1% of the population.
Likewise, the authors indicate that “the maximum incidence occurs in the third decade of life, 50% of cases occur before the age of 20”.
Symptoms

The most characteristic symptom of vitiligo is depigmentation of the skin. As the authors of the aforementioned article indicate, the lesions appear as white patches with well-defined borders. These can vary in size and, as the disease progresses, they can spread to cover other areas of the body.
The patches cover the body asymmetrically. The most affected areas are usually the hands and face, as well as the elbows, knees, armpits, groin folds, forearms, and genitals.
In addition to affecting the skin, mucous membranes, and even the retina, vitiligo can affect hair. Therefore, people with this disease may have different colored hair, facial hair (eyelashes, eyebrows, mustache, beard) and body hair (areas with white hair and areas with dark hair).
Other symptoms that may occur are the following:
- Itching and discomfort in the affected areas
- Premature graying of facial and other hair
Regarding the progression of the disease, it’s worth highlighting what was stated in an article published in the journal Dermatology, “the natural course of vitiligo is unpredictable. Sometimes there’s an abrupt onset, followed by a progression for an indeterminate time, and then a stability that can be from a short time to decades”.
Causes
Although vitiligo has been known for a long time, its cause hasn’t yet been established.
However, several hypotheses have been put forward that mainly involve autoimmune and genetic mechanisms, in combination with various triggers, such as a high level of emotional stress.
What must be taken into account is that it’s a disease that causes the cells that are responsible for producing melanin (that is, melanocytes), to suspend their function or die. This leads to progressive depigmentation.
“For experts in pigment cells, vitiligo represents an opportunity to study the basic biological mechanisms of the functions of melanocytes“, state authors such as Carmen Lucía Pimentel, Lluis Pug and Agustín Alomar.
Triggers
Although it hasn’t yet been possible to specify a cause, it has been possible to determine some triggers of vitiligo. Among them are the following:
- Viral infections
- High level of stress/chronic stress
- Severe sunburn
- Severe skin trauma
- Exposure to aggressive chemicals
Diagnosis

The diagnosis of vitiligo is primarily clinical. At the consultation and physical examination, the doctor can easily detect the patches (achromic macules) in the most typical locations. However, sometimes a more exhaustive review may be necessary and, in others, a skin biopsy may even be requested, although this isn’t very common.
When vitiligo occurs in young children, parents may confuse it with pityriasis alba. This is one of the scenarios in which differential diagnosis comes into play.
Other diseases that are considered when carrying out a differential diagnosis are achromic nevus, anemic nevus, and tuberous sclerosis.
Treatment
There’s no treatment that can reverse the disease or cure it. However, there are several options that help control symptoms and mitigate their impact on quality of life.
All vitiligo patients are advised to protect themselves from solar radiation on a daily basis to avoid burns and the aggravation of existing lesions. In order to do this, they shouldn’t only use adequate sunscreen, but they should also wear clothing that covers their skin and keeps it protected from other factors, such as wind, cold, and heat.
“The aim of any therapeutic modality is to regenerate the epidermal melanocytes in order to obtain a complete and permanent repigmentation of the affected areas”, indicates an article published in Elsevier.
To do this, you can resort to some topical corticosteroids (in pills or injections) and topical medications to control inflammation, among others. Again, these aren’t going to stop the progression of the disease, but they may help control symptoms.
Another popular treatment option is ultraviolet B phototherapy, as well as combining it with a plant-based substance called psoralen.
Regular check-ups and good communication with your doctor will be essential in order to make the necessary modifications in treatment and maintain quality of life.
- Cristina M, Correa T, Marina L, Vargas G. Vitiligo. Rev Asoc Col Dermatol [Internet]. 2008 [cited 2021 Jul 11];17:86. Available from: https://revistasocolderma.org/sites/default/files/vitiligo.pdf
- Fernández Paniagua D, Valdés Esquivel J, Valverde Madriz P. Generalidades del vitíligo. Rev Medica Sinerg [Internet]. 2020 Aug 1 [cited 2021 Jul 11];5(8):e556. Available from: https://revistamedicasinergia.com/index.php/rms/article/download/556/941?i
- Pimentel CL, Puig L, Alomar A. Vitíligo. Despigmentación cutánea [Internet]. Farmacia Profesional. 2002 [cited 2021 Jul 11]. p. 61–8. Available from: https://www.elsevier.es/es-revista-farmacia-profesional-3-articulo-vitiligo-despigmentacion-cutanea-13028922
- Rey JP. Alteraciones de la pigmentación cutánea. AEPED [Internet]. [cited 2021 Jul 10]; Available from: https://www.aeped.es/sites/default/files/documentos/pigmentacion.pdf
- Vázquez-Martínez O., Méndez-Olvera N, Velásquez-Arenas L, Ocampo-Candiani J. Vitíligo. Panorama general. Dermatología Cosmética, Médica y Quirúrgica [Internet]. 2006 [cited 2021 Jul 11];4(3):187–92. Available from: https://www.medigraphic.com/pdfs/cosmetica/dcm-2006/dcm063g.pdf
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







