The Diagnosis of Breast Cancer

Your chances of getting breast cancer increase as you get older. Women should have annual tests after the age of 40, a preventive habit to locate abnormalities in their early stages. The diagnosis of breast cancer uses different imaging and laboratory tests, which we’ll look at in detail in the following article.
It’s important to remember that many times, the symptoms of the disease don’t appear until it has progressed to more serious episodes. Even so, different tests can detect it in advance; a very important advance to tip the balance towards a more positive prognosis.
Breast self-exams and the diagnosis of breast cancer
Although in no case can it replace a diagnosis mediated by a specialist, and its effects are in any case limited, research continues to point out the importance of breast self-examination as a method of early detection of the disease.
The controversy isn’t minor, especially when the evidence indicates that a good part of those who practice it have erroneous knowledge about how to do it or how often.
Self-examination can be considered a prediagnosis that alerts women to a problem. It can then serve as a guide for other tests and exams with a greater spectrum of reliability.
As the American Cancer Society reminds us, the results of self-examination should be taken with measure. They can give false hope that everything’s in order, although becoming familiar with the size and shape of the breasts is important to detect possible changes in them due to the symptoms. If you have questions, be sure to talk to your doctor about how to perform self-breast exams correctly.
The diagnosis of breast cancer by means of physical and clinical examinations
To make a diagnosis of breast cancer, a specialist can resort to a multitude of tests. Routinely, you may opt for a physical examination before proceeding with much more complex examinations. These consist of the following:
- Interview to determine risk factors: Here, a general assessment of the state of health is carried out in search of possible alterations or collateral damage caused by the disease. The doctor will take into account at this point a family history of cancer, health habits, diet, and other risk factors.
- Physical examination for breast cancer: Through them, the specialist will palpate the breast area in search of malformations or nodules that indicate the possible development of the disease. This can also be extended to peripheral areas.
During both examinations, the color, texture, and appearance of the breast and nipple are taken into account, always considering the changes that the patient has noticed during the last months. This is only an initial diagnosis, generally used to make way for more comprehensive tests.
The diagnosis of breast cancer through imaging
According to the evidence, the diagnosis of cancer through imaging tests is one of the safest methods that specialists can use. Although research has motivated the development of new tests, the truth is that those carried out by imaging continue to be a benchmark in medicine. The most used are the following:
Mammography
Mammography is a cancer diagnostic test in which x-ray images of the breasts are obtained. It’s done on a special machine, called a mammogram, by pressing the breast into two plates to get an X-ray. This method can detect the disease up to 2-3 years before the first symptoms appear.
There are two types: Detection and diagnostic. The first obtains images in a general way, the second does so in a specific area (the one in which a nodule has been detected through clinical examination, for example). Because the test doesn’t distinguish cancer from other breast conditions, complementary methods are necessary for an accurate diagnosis.
Breast ultrasound
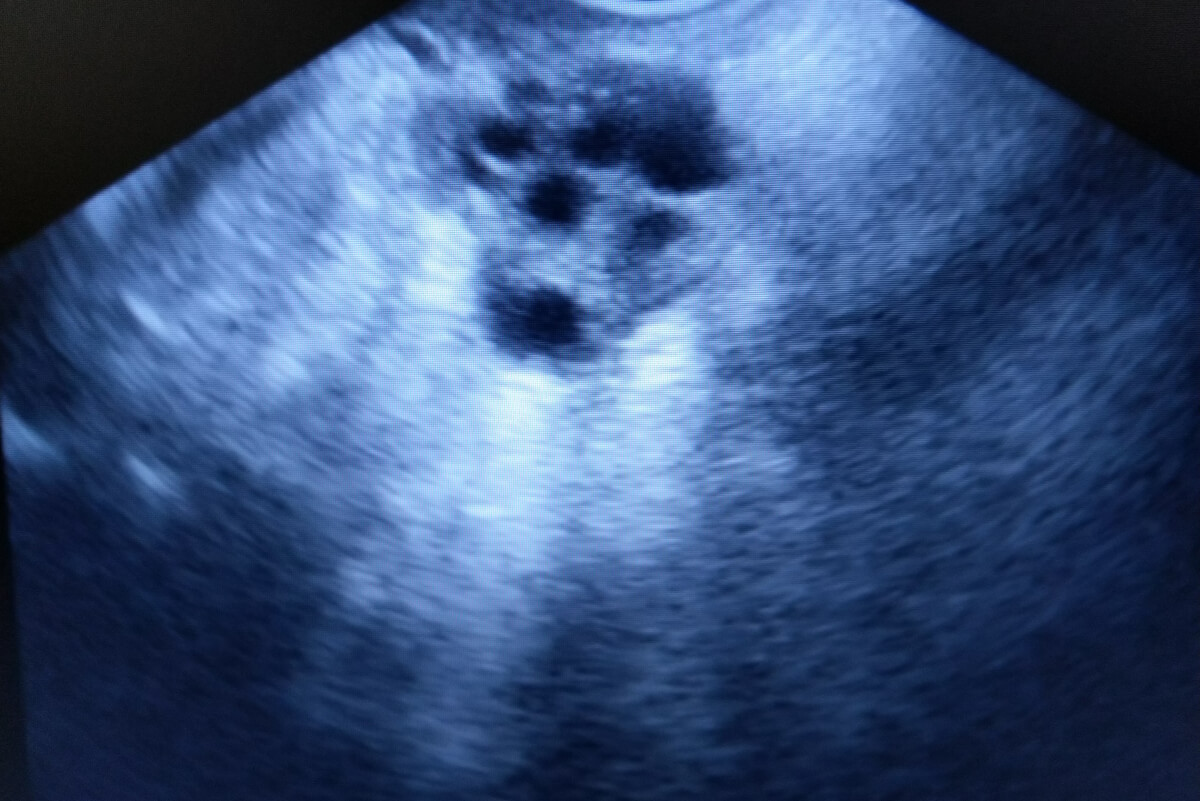
Ultrasound is a procedure in which high-energy sound waves are bounced off the breast tissues. The rebound effect of these waves generates an image of the internal appearance called a breast ultrasound or breast sonogram.
It’s very common for breast ultrasound to be used as an adjunct to a mammogram, especially when abnormal areas have been detected. In this case, the test can be helpful in distinguishing a fluid-filled cyst from a solid malformation. Even so, its scope is limited and requires other tests to confirm the presence of the disease.
Magnetic resonance (MRI)
This study takes place with the help of magnetic fields that result in a series of internal images of the breast. An MRI is an adjunct test to mammography, not a main procedure. This is because it’s less effective than this or ultrasound in detecting certain types of breast cancer. Despite this, it can be very useful in certain contexts.
These are the most widely used imaging methods in the diagnosis of breast cancer. Depending on the specialist’s criteria, a positron emission tomography (PET scan) or computed tomography may also be useful. The three procedures described, however, are the most used today.
Laboratory tests for breast cancer
The above tests are used to identify abnormalities or nodules, but only through laboratory tests can a diagnosis of breast cancer be confirmed. The most important of all is a biopsy, as it allows the tissue to be studied directly under a microscope.
This procedure consists of extracting samples of breast cells and analyzing them thoroughly. There are many types of biopsy, and the most used are those mentioned below:
- Excision: In which a complete extraction of the mass is carried out.
- Incision: Only a part of the mass is removed as a sample for later analysis.
- Fine needle aspiration: Also called FNA, it consists of obtaining a tissue sample with the help of a fine needle connected to a syringe. If it’s a cyst, the procedure can drain the fluid.
- Coarse Needle Puncture: A wider, hollow needle is used, making it easier to remove more tissue.
To get to the tissue, the doctor will use imaging tests to locate it. The material obtained is taken to the laboratory to determine the possible presence of cancer cells.
In the case of obtaining reliable evidence, other laboratory tests will also be carried out to determine how quickly it grows, the probability of recidivism, and the possibility of its spread, among other things. Some of those that are used are the following:
- Estrogen and progesterone receptor test
- Multigene tests ( MammaPrint and OncoType DX )
- Human epidermal growth factor receptor 2 test
Complementary tests are also performed to elucidate the stage of the cancer detected; that is, its possible spread to other parts of the body.
Differential diagnostics
It’s important for the patient to keep in mind that not all lumps or nodules detected through imaging tests are caused by breast cancer. Only a laboratory test can confirm the presence of the disease, as there are many differential diagnoses. Studies suggest the following:
- Lobular carcinoma
- Small cell carcinoma
- Chronic mastitis
- Lymphoid proliferation
- Melanoma
- Cyst
- Intramammary lymph node
It’s important to remember that changes in the shape or size of the breasts are relatively common as you age. The consideration of risk factors, family history, the patient’s own assessment of possible symptoms, and tests aimed at the diagnosis of breast cancer work together when determining the disease.
We conclude by reiterating the importance of the prevention of breast cancer. Studies indicate a consensus on the importance of breast screening in the absence of symptoms, something that has a positive impact when treating the condition.
Your chances of getting breast cancer increase as you get older. Women should have annual tests after the age of 40, a preventive habit to locate abnormalities in their early stages. The diagnosis of breast cancer uses different imaging and laboratory tests, which we’ll look at in detail in the following article.
It’s important to remember that many times, the symptoms of the disease don’t appear until it has progressed to more serious episodes. Even so, different tests can detect it in advance; a very important advance to tip the balance towards a more positive prognosis.
Breast self-exams and the diagnosis of breast cancer

Although in no case can it replace a diagnosis mediated by a specialist, and its effects are in any case limited, research continues to point out the importance of breast self-examination as a method of early detection of the disease.
The controversy isn’t minor, especially when the evidence indicates that a good part of those who practice it have erroneous knowledge about how to do it or how often.
Self-examination can be considered a prediagnosis that alerts women to a problem. It can then serve as a guide for other tests and exams with a greater spectrum of reliability.
As the American Cancer Society reminds us, the results of self-examination should be taken with measure. They can give false hope that everything’s in order, although becoming familiar with the size and shape of the breasts is important to detect possible changes in them due to the symptoms. If you have questions, be sure to talk to your doctor about how to perform self-breast exams correctly.
The diagnosis of breast cancer by means of physical and clinical examinations
To make a diagnosis of breast cancer, a specialist can resort to a multitude of tests. Routinely, you may opt for a physical examination before proceeding with much more complex examinations. These consist of the following:
- Interview to determine risk factors: Here, a general assessment of the state of health is carried out in search of possible alterations or collateral damage caused by the disease. The doctor will take into account at this point a family history of cancer, health habits, diet, and other risk factors.
- Physical examination for breast cancer: Through them, the specialist will palpate the breast area in search of malformations or nodules that indicate the possible development of the disease. This can also be extended to peripheral areas.
During both examinations, the color, texture, and appearance of the breast and nipple are taken into account, always considering the changes that the patient has noticed during the last months. This is only an initial diagnosis, generally used to make way for more comprehensive tests.
The diagnosis of breast cancer through imaging
According to the evidence, the diagnosis of cancer through imaging tests is one of the safest methods that specialists can use. Although research has motivated the development of new tests, the truth is that those carried out by imaging continue to be a benchmark in medicine. The most used are the following:
Mammography
Mammography is a cancer diagnostic test in which x-ray images of the breasts are obtained. It’s done on a special machine, called a mammogram, by pressing the breast into two plates to get an X-ray. This method can detect the disease up to 2-3 years before the first symptoms appear.
There are two types: Detection and diagnostic. The first obtains images in a general way, the second does so in a specific area (the one in which a nodule has been detected through clinical examination, for example). Because the test doesn’t distinguish cancer from other breast conditions, complementary methods are necessary for an accurate diagnosis.
Breast ultrasound

Ultrasound is a procedure in which high-energy sound waves are bounced off the breast tissues. The rebound effect of these waves generates an image of the internal appearance called a breast ultrasound or breast sonogram.
It’s very common for breast ultrasound to be used as an adjunct to a mammogram, especially when abnormal areas have been detected. In this case, the test can be helpful in distinguishing a fluid-filled cyst from a solid malformation. Even so, its scope is limited and requires other tests to confirm the presence of the disease.
Magnetic resonance (MRI)
This study takes place with the help of magnetic fields that result in a series of internal images of the breast. An MRI is an adjunct test to mammography, not a main procedure. This is because it’s less effective than this or ultrasound in detecting certain types of breast cancer. Despite this, it can be very useful in certain contexts.
These are the most widely used imaging methods in the diagnosis of breast cancer. Depending on the specialist’s criteria, a positron emission tomography (PET scan) or computed tomography may also be useful. The three procedures described, however, are the most used today.
Laboratory tests for breast cancer
The above tests are used to identify abnormalities or nodules, but only through laboratory tests can a diagnosis of breast cancer be confirmed. The most important of all is a biopsy, as it allows the tissue to be studied directly under a microscope.
This procedure consists of extracting samples of breast cells and analyzing them thoroughly. There are many types of biopsy, and the most used are those mentioned below:
- Excision: In which a complete extraction of the mass is carried out.
- Incision: Only a part of the mass is removed as a sample for later analysis.
- Fine needle aspiration: Also called FNA, it consists of obtaining a tissue sample with the help of a fine needle connected to a syringe. If it’s a cyst, the procedure can drain the fluid.
- Coarse Needle Puncture: A wider, hollow needle is used, making it easier to remove more tissue.
To get to the tissue, the doctor will use imaging tests to locate it. The material obtained is taken to the laboratory to determine the possible presence of cancer cells.
In the case of obtaining reliable evidence, other laboratory tests will also be carried out to determine how quickly it grows, the probability of recidivism, and the possibility of its spread, among other things. Some of those that are used are the following:
- Estrogen and progesterone receptor test
- Multigene tests ( MammaPrint and OncoType DX )
- Human epidermal growth factor receptor 2 test
Complementary tests are also performed to elucidate the stage of the cancer detected; that is, its possible spread to other parts of the body.
Differential diagnostics
It’s important for the patient to keep in mind that not all lumps or nodules detected through imaging tests are caused by breast cancer. Only a laboratory test can confirm the presence of the disease, as there are many differential diagnoses. Studies suggest the following:
- Lobular carcinoma
- Small cell carcinoma
- Chronic mastitis
- Lymphoid proliferation
- Melanoma
- Cyst
- Intramammary lymph node
It’s important to remember that changes in the shape or size of the breasts are relatively common as you age. The consideration of risk factors, family history, the patient’s own assessment of possible symptoms, and tests aimed at the diagnosis of breast cancer work together when determining the disease.
We conclude by reiterating the importance of the prevention of breast cancer. Studies indicate a consensus on the importance of breast screening in the absence of symptoms, something that has a positive impact when treating the condition.
- Akyolcu, N., & Altun Uğraş, G. Breast self-examination: how important is it in early diagnosis. J Breast Health. 2011; 7(1): 10-14.
- Austoker, J. Breast self examination. 2003; 326(7379): 1–2.
- Bevers, T. B., Anderson, B. O., Bonaccio, E., Buys, S., Daly, M. B., Dempsey, P. J., … & Yankeelov, T. Breast cancer screening and diagnosis. Journal of the National Comprehensive Cancer Network. 2009; 7(10): 1060-1096.
- Hislop, T. G., Coldman, A. J., & Skippen, D. H. Breast self-examination: importance of technique in early diagnosis. Canadian Medical Association Journal. 1984; 131(11): 1349.
- Jafari, S. H., Saadatpour, Z., Salmaninejad, A., Momeni, F., Mokhtari, M., Nahand, J. S., … & Kianmehr, M. Breast cancer diagnosis: Imaging techniques and biochemical markers. Journal of cellular physiology. 2018; 233(7): 5200-5213.
- Wang, L. Early diagnosis of breast cancer. Sensors. 2017; 17(7): 1572.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







