Still's Disease: Symptoms, Causes and Treatment

Still’s disease, also known as systemic juvenile idiopathic arthritis, is an inflammatory disorder of the joints and other parts of the body. It’s considered a rare condition that often goes unnoticed in diagnoses. According to the National Organization for Rare Disorders (NORD), between 1 and 34 cases are reported per million inhabitants.
This type of arthritis is thought to be more common in women than in men, and it mainly develops between the ages of 16 and 35. There are still many unknowns surrounding it, but, in the following lines, we’ll try to tell you what we know about its clinical manifestations and the options available to treat it.
Causes of Still’s disease
Experts still haven’t found the exact causes of this systemic disorder. Researchers believe that genetic predisposition may play a role. Also, an uncontrolled immune response to viruses and bacteria, for example, against Yersinia enterocolitica (as evidence has suggested).
Still’s disease is usually classified as an autoinflammatory syndrome and not as an autoimmune disorder. As the Spanish Association of Familial Mediterranean Fever and Autoinflammatory Syndromes (FMF) points out, this category covers conditions that prevail in patients with innate abnormalities of their immune system.
According to the hypothesis supporting this theory, Still’s disease shares a place with other conditions, such as Muckle-Wells syndrome and neonatal-onset multisystem inflammatory disorder. In most cases, it’s described as an idiopathic disease – one without a specific cause.

Symptoms of Still’s disease
The signs that alert us to the presence of the disease are very varied and differ between each patient. The hallmark of this type of arthritis is that it causes systemic manifestations. That is, the symptoms aren’t concentrated only in the joints, but spread to other parts of the body.
The Arthritis Foundation distinguishes between two stages of this disease: an acute one with general signs and a chronic one with diseases focused on the joints. Let’s see what symptoms can appear at the beginning:
- High fever
- Pink skin lesions that affect the torso, arms, and legs
- Throat pain
- Swelling of the lymph nodes
These four signs develop over a couple of weeks, with variations in intensity. After this, the condition progresses to pain in the knee and wrist joints, as well as muscle pain that interrupts daily activities.
In children and young people, the signs can be more varied. As a complement to those mentioned, and following the Spanish Society of Pediatric Rheumatology (SERPE), in these cases the symptoms below may appear:
- Splenomegaly (inflammation of the spleen)
- Hepatomegaly (inflammation of the liver)
- Pericarditis (inflammation of the pericardium that lines the heart)
- Peritonitis (inflammation of the peritoneum in the abdomen)
- Pleurisy (inflammation of the pleura that lines the lungs)
- Heart conditions (valvular heart disease or myocarditis)
Symptoms develop in episodes or flare-ups. Later, these people can go through remission, or at least a clear decrease in their intensity.
Still’s disease diagnosis
There’s no standard test to diagnose Still’s disease. Doctors generally try to rule out all possible explanations for the symptoms, including other manifestations of arthritis. The process can be very complex.
During this time, the specialist will order a series of laboratory and imaging tests to guide the diagnosis. Before doing so, they will review the patient’s medical history, underlying conditions, patterns of symptoms, family history, and general health.
The researchers suggest including the following in the protocol:
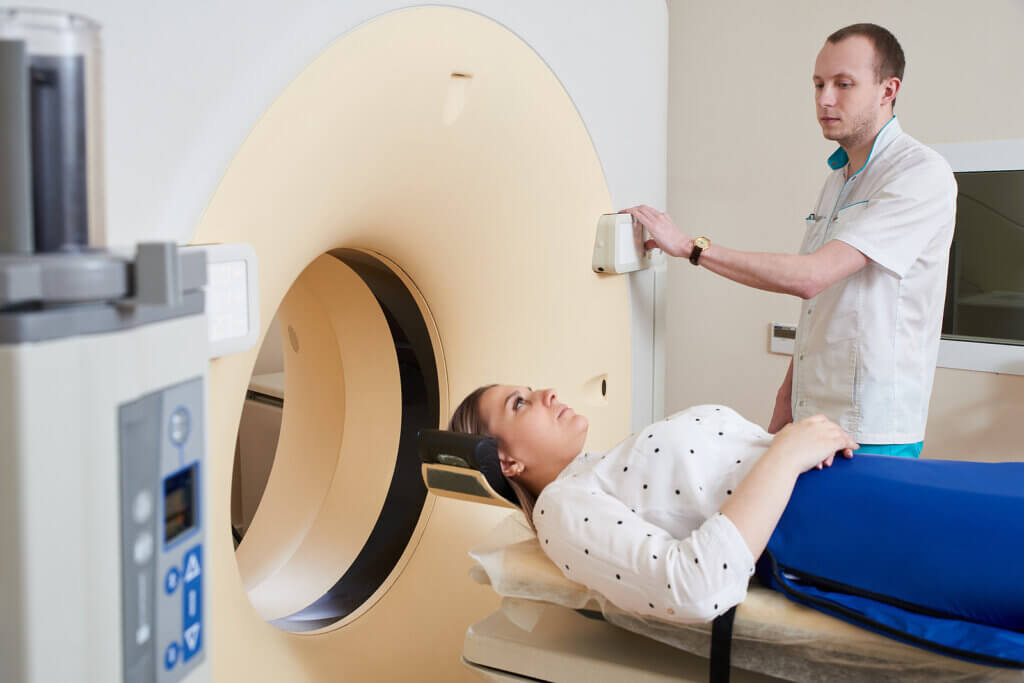
- Computed tomography
- A bone scan
- Magnetic resonance
- Ultrasound
- Complete urine and blood tests
All this helps to rule out other conditions. Once other inflammatory explanations have been ruled out, the doctor will proceed to confirm the diagnosis.
Treatment options
There’s no cure for Still’s disease. Treatment consists of slowing down the symptoms and slowing down the progression. Therefore, therapy is done based on the severity of the signs, age, and possible underlying conditions.
It’s very common for treatment to begin with the prescription of nonsteroidal anti-inflammatory drugs and aspirin, as pointed out by the National Center for Advancing Translational Sciences. Disease-modifying antirheumatic drugs, such as methotrexate, are also prescribed. Specific medications are used to treat derived symptoms, as appropriate.
The sooner you start therapy, the better. Some cases of this disease tend to worsen to chronic stages in the absence of treatment.
It’s very important that the evolution is monitored during the first weeks, thus certifying that the drugs are having an effect. If not, they should be tried with other available alternatives.
Still’s disease, also known as systemic juvenile idiopathic arthritis, is an inflammatory disorder of the joints and other parts of the body. It’s considered a rare condition that often goes unnoticed in diagnoses. According to the National Organization for Rare Disorders (NORD), between 1 and 34 cases are reported per million inhabitants.
This type of arthritis is thought to be more common in women than in men, and it mainly develops between the ages of 16 and 35. There are still many unknowns surrounding it, but, in the following lines, we’ll try to tell you what we know about its clinical manifestations and the options available to treat it.
Causes of Still’s disease
Experts still haven’t found the exact causes of this systemic disorder. Researchers believe that genetic predisposition may play a role. Also, an uncontrolled immune response to viruses and bacteria, for example, against Yersinia enterocolitica (as evidence has suggested).
Still’s disease is usually classified as an autoinflammatory syndrome and not as an autoimmune disorder. As the Spanish Association of Familial Mediterranean Fever and Autoinflammatory Syndromes (FMF) points out, this category covers conditions that prevail in patients with innate abnormalities of their immune system.
According to the hypothesis supporting this theory, Still’s disease shares a place with other conditions, such as Muckle-Wells syndrome and neonatal-onset multisystem inflammatory disorder. In most cases, it’s described as an idiopathic disease – one without a specific cause.

Symptoms of Still’s disease
The signs that alert us to the presence of the disease are very varied and differ between each patient. The hallmark of this type of arthritis is that it causes systemic manifestations. That is, the symptoms aren’t concentrated only in the joints, but spread to other parts of the body.
The Arthritis Foundation distinguishes between two stages of this disease: an acute one with general signs and a chronic one with diseases focused on the joints. Let’s see what symptoms can appear at the beginning:
- High fever
- Pink skin lesions that affect the torso, arms, and legs
- Throat pain
- Swelling of the lymph nodes
These four signs develop over a couple of weeks, with variations in intensity. After this, the condition progresses to pain in the knee and wrist joints, as well as muscle pain that interrupts daily activities.
In children and young people, the signs can be more varied. As a complement to those mentioned, and following the Spanish Society of Pediatric Rheumatology (SERPE), in these cases the symptoms below may appear:
- Splenomegaly (inflammation of the spleen)
- Hepatomegaly (inflammation of the liver)
- Pericarditis (inflammation of the pericardium that lines the heart)
- Peritonitis (inflammation of the peritoneum in the abdomen)
- Pleurisy (inflammation of the pleura that lines the lungs)
- Heart conditions (valvular heart disease or myocarditis)
Symptoms develop in episodes or flare-ups. Later, these people can go through remission, or at least a clear decrease in their intensity.
Still’s disease diagnosis
There’s no standard test to diagnose Still’s disease. Doctors generally try to rule out all possible explanations for the symptoms, including other manifestations of arthritis. The process can be very complex.
During this time, the specialist will order a series of laboratory and imaging tests to guide the diagnosis. Before doing so, they will review the patient’s medical history, underlying conditions, patterns of symptoms, family history, and general health.
The researchers suggest including the following in the protocol:
- Computed tomography
- A bone scan
- Magnetic resonance
- Ultrasound
- Complete urine and blood tests
All this helps to rule out other conditions. Once other inflammatory explanations have been ruled out, the doctor will proceed to confirm the diagnosis.

Treatment options
There’s no cure for Still’s disease. Treatment consists of slowing down the symptoms and slowing down the progression. Therefore, therapy is done based on the severity of the signs, age, and possible underlying conditions.
It’s very common for treatment to begin with the prescription of nonsteroidal anti-inflammatory drugs and aspirin, as pointed out by the National Center for Advancing Translational Sciences. Disease-modifying antirheumatic drugs, such as methotrexate, are also prescribed. Specific medications are used to treat derived symptoms, as appropriate.
The sooner you start therapy, the better. Some cases of this disease tend to worsen to chronic stages in the absence of treatment.
It’s very important that the evolution is monitored during the first weeks, thus certifying that the drugs are having an effect. If not, they should be tried with other available alternatives.
- Angarita, J. M. M. Artritis idiopática juvenil sistémica. 2020.
- Bhargava, J., & Panginikkod, S. Still Disease. StatPearls. 2019.
- Colebunders R, Stevens WJ, Vanagt E, Snoeck J. Adult Still’s disease caused by Yersinia enterocolitica infection. Arch Intern Med. 1984 Sep;144(9):1880-2.
- Gerfaud-Valentin M, Maucort-Boulch D, Hot A, Iwaz J, Ninet J, Durieu I, Broussolle C, Sève P. Adult-onset still disease: manifestations, treatment, outcome, and prognostic factors in 57 patients. Medicine (Baltimore). 2014 Mar;93(2):91-99.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







