Melasma: Symptoms, Causes, Prevention and Treatment

Melasma is the name given to the presence of dark spots, of variable size and shape, generally on the faces of women. There are also manifestations in men, although these are less common.
These occur in response to exposure to ultraviolet light and hormonal changes typical of pregnancy or the use of contraceptives. If you suffer from this condition or are interested in knowing a little more about it, we have prepared the following article for you.
What are the clinical manifestations?
Melasma is facial hyperpigmentation, although there are also extra facial presentations. The name refers to a more intense coloration than the person’s normal skin color. A dark brown color is the most common in this type of injury.
It usually appears symmetrically, with almost the same shapes on both sides of the body. The appearance of the spots is progressive without including associated symptoms, such as itching, burning or pain.
It’s relapsing in nature, so they can decrease in size and appear several weeks later. Due to its facial location, it could influence the appearance of anxiety disorders, self-esteem, or depression with variable severity.
What are the main types of melasma?
There are several classifications that doctors use for this condition. The most widely used is the one that distinguishes facial from extra facial lesions.
Facial melasma has several locations. They can be centrofacial (when it affects cheeks, nose, and upper lips), malar (a little behind both cheeks), and mandibular (very rare and affects the surface of the corresponding bone).
In the case of extrafacial melasma, it usually occurs in the upper limbs, sternum, and neck. The fact that it isn’t an accepted clinical variety is very striking, since some dermatologists consider that it’s a melanoderma.
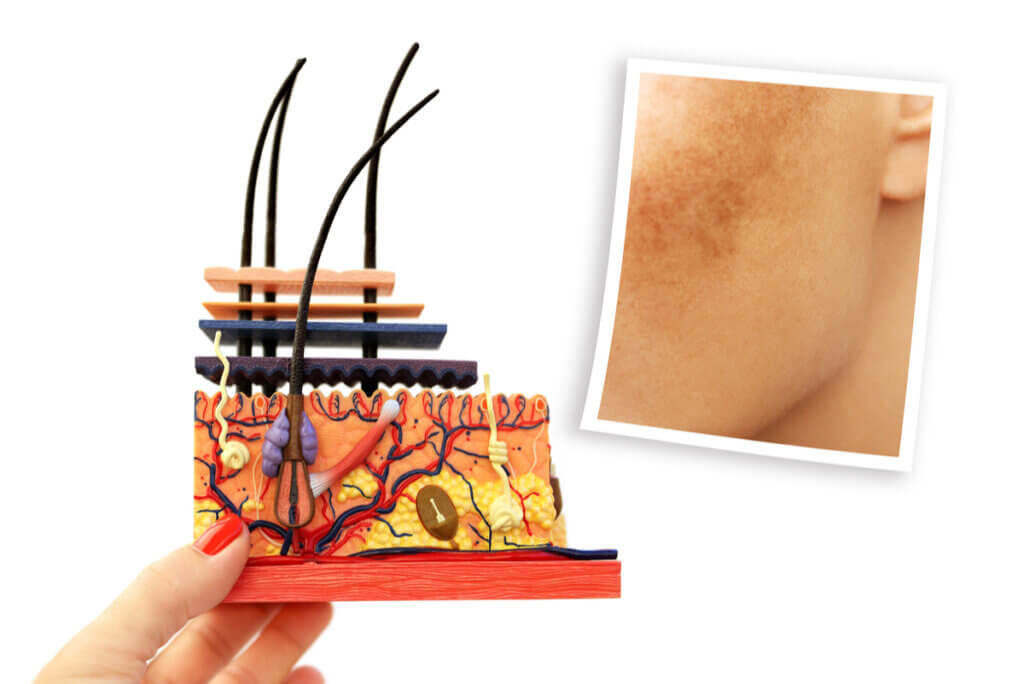
Why do the lesions appear?
Not in all cases is it possible to detect a specific cause. However, it’s known that, at a cellular level, there’s an increase in the number of melanocytes. These are the skin cells responsible for the production of melanin, the main pigment in the skin.
Because these cells appear unevenly in response to various stimuli, the lesions are highly varied and scattered. Thanks to the study of the skin through biopsies, it has been possible to distinguish other less obvious alterations that include the following:
- An increase in the number of mast cells, which are cells belonging to the immune system.
- A greater abundance of blood vessels, related to the increase in the number of cells.
- Constant exposure to ultraviolet light could trigger a phenomenon known as solar elastosis. This involves the deterioration of the tissue that binds and supports the cells of the epidermis, progressively weakening it.
Exogenous risk factors
Within this group, the most important aspect is exposure to ultraviolet light. This represents a type of radiation that isn’t very visible to the human eye, adapting a rather faint violet hue.
It’s likely that, for this reason, the lesions are on the face and in areas exposed to light. The use of sunscreen is an excellent way to prevent the appearance of injuries.
The rest of the physical factors include facial trauma, although the lesions don’t always occur in the same way nor do they tend to recur. Exposure to certain chemical elements could also favor the appearance of melasma. These include cosmetics and the effect of certain skin cleansers.
Endogenous risk factors
Contrary to popular belief, melasma is not the result of liver or kidney disease. Among the endogenous risk factors, the most important are sex, the level of certain hormones, and skin type.
Women are the most prone to the disease. This could be due to genetic characteristics inherent to the female sex, such as the hormonal load during pregnancy. In addition, due to the increasing use of oral contraceptives (OCs), the incidence of melasma has increased greatly in recent years.
It can appear on any type of skin, however they’re more frequent in those with dark tones. In slightly more complex terms, it affects phototypes III to V.
After the introduction of finasteride as a therapeutic alternative for the treatment of androgenic alopecia, more cases of melasma began to be seen in men. This drug is associated with hormonal changes, which could cause spots, according to a 2014 case report.
Can the appearance of melasma be prevented?
In theory, the occurrence of these lesions can be prevented by avoiding modifiable risk factors. However, in some cases, it’s difficult to stop using certain types of hormone treatments. It’s best to avoid exposure to sunlight.
The recommendation is to resort to chemical photoprotection, that is, sunscreens. The choice depends a lot on the possibilities of each patient, being necessary to choose the best quality/price ratio and optimize other personal measures to protect yourself.
A sun protection factor (SPF) of type 50+ is recommended. A trusted dermatologist must carry out the pertinent indications, but it usually requires several applications throughout the day and at any time of the year.
Other personal measures are necessary. Wearing hats and glasses are simple habits that can help prevent the appearance of new injuries. Finally, it’s best to avoid the use of irritating cosmetics that are susceptible to chemical modifications when exposed to abundant sunlight.
Is there treatment for melasma?
This condition is recurring, so, in certain circumstances, it can disappear on its own. However, even more so when a patient is exposed to permanent risk factors, there are therapeutic alternatives to reduce symptoms. These not only have an effect on the size of the lesions, but also on the psychological manifestations.
Topical treatment isn’t only the most effective, but is also associated with far fewer adverse effects. This has the particularity that it’s preferred in polytherapy, which means that combinations between several drugs are preferred.
Topical treatment
The most commonly used medications are hydroquinone, retinoids, and steroids. Hydroquinone has the advantage of producing very few adverse effects.
Retinoids are derivatives of vitamin A and are widely used in dermatology, both orally and topically. This last presentation isn’t recommended in pregnant women, since it’s known to have a teratogenic effect.
When speaking of steroids, reference is being made to a group of similar substances that usually have an immunosuppressive effect. This decreases inflammation in the lesions and promotes satisfactory improvements, but they are not recommended as sole therapy.
Systemic treatment
The options are more limited than in the previous section and include tranexamic acid, carotenoids, and melatonin. Most of these therapeutic alternatives are recommended in the long term and require the combination with powerful sunscreens to avoid the appearance of new lesions.
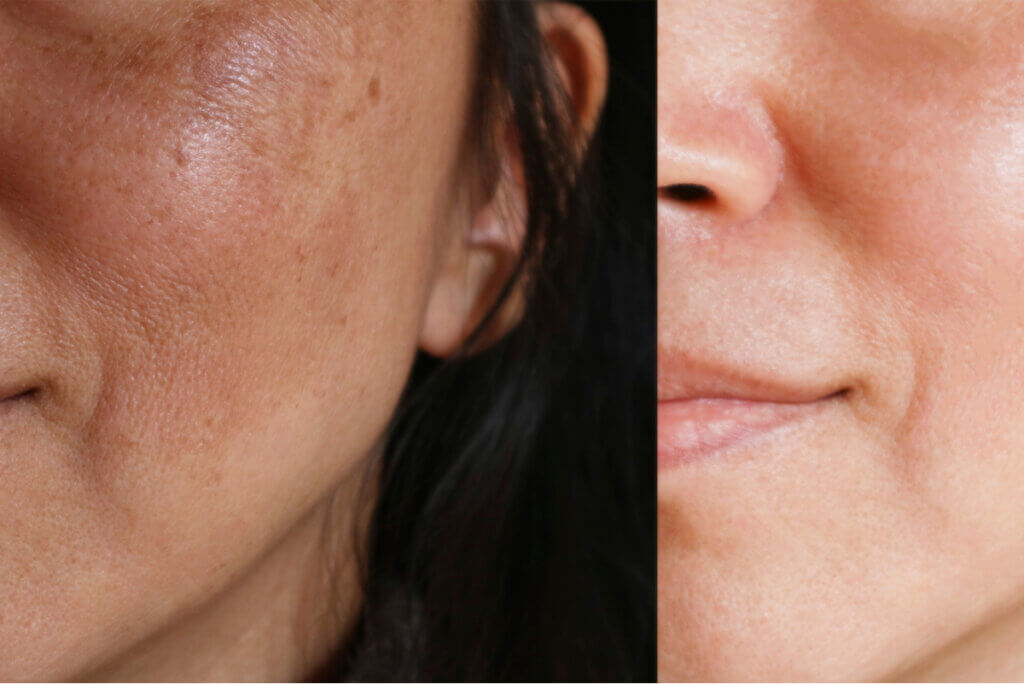
An important aesthetic issue
Melasma has an important aesthetic aspect, so alternatives are valued to improve the appearance of the spots in people who want to remove or reduce them. Did you know that there are tools for it?
Superficial chemoexfoliation is one of them. It isn’t used as first-line therapy, but is reserved for cases in which topical or oral treatment has failed.
Carrying out this procedure involves applying chemical substances to the skin in order to eliminate dead cells. Added medications include glycolic acid and tretinoin. Always remember to consult an expert if you decide to use one of these approaches.
Melasma is the name given to the presence of dark spots, of variable size and shape, generally on the faces of women. There are also manifestations in men, although these are less common.
These occur in response to exposure to ultraviolet light and hormonal changes typical of pregnancy or the use of contraceptives. If you suffer from this condition or are interested in knowing a little more about it, we have prepared the following article for you.
What are the clinical manifestations?
Melasma is facial hyperpigmentation, although there are also extra facial presentations. The name refers to a more intense coloration than the person’s normal skin color. A dark brown color is the most common in this type of injury.
It usually appears symmetrically, with almost the same shapes on both sides of the body. The appearance of the spots is progressive without including associated symptoms, such as itching, burning or pain.
It’s relapsing in nature, so they can decrease in size and appear several weeks later. Due to its facial location, it could influence the appearance of anxiety disorders, self-esteem, or depression with variable severity.
What are the main types of melasma?
There are several classifications that doctors use for this condition. The most widely used is the one that distinguishes facial from extra facial lesions.
Facial melasma has several locations. They can be centrofacial (when it affects cheeks, nose, and upper lips), malar (a little behind both cheeks), and mandibular (very rare and affects the surface of the corresponding bone).
In the case of extrafacial melasma, it usually occurs in the upper limbs, sternum, and neck. The fact that it isn’t an accepted clinical variety is very striking, since some dermatologists consider that it’s a melanoderma.

Why do the lesions appear?
Not in all cases is it possible to detect a specific cause. However, it’s known that, at a cellular level, there’s an increase in the number of melanocytes. These are the skin cells responsible for the production of melanin, the main pigment in the skin.
Because these cells appear unevenly in response to various stimuli, the lesions are highly varied and scattered. Thanks to the study of the skin through biopsies, it has been possible to distinguish other less obvious alterations that include the following:
- An increase in the number of mast cells, which are cells belonging to the immune system.
- A greater abundance of blood vessels, related to the increase in the number of cells.
- Constant exposure to ultraviolet light could trigger a phenomenon known as solar elastosis. This involves the deterioration of the tissue that binds and supports the cells of the epidermis, progressively weakening it.
Exogenous risk factors
Within this group, the most important aspect is exposure to ultraviolet light. This represents a type of radiation that isn’t very visible to the human eye, adapting a rather faint violet hue.
It’s likely that, for this reason, the lesions are on the face and in areas exposed to light. The use of sunscreen is an excellent way to prevent the appearance of injuries.
The rest of the physical factors include facial trauma, although the lesions don’t always occur in the same way nor do they tend to recur. Exposure to certain chemical elements could also favor the appearance of melasma. These include cosmetics and the effect of certain skin cleansers.
Endogenous risk factors
Contrary to popular belief, melasma is not the result of liver or kidney disease. Among the endogenous risk factors, the most important are sex, the level of certain hormones, and skin type.
Women are the most prone to the disease. This could be due to genetic characteristics inherent to the female sex, such as the hormonal load during pregnancy. In addition, due to the increasing use of oral contraceptives (OCs), the incidence of melasma has increased greatly in recent years.
It can appear on any type of skin, however they’re more frequent in those with dark tones. In slightly more complex terms, it affects phototypes III to V.
After the introduction of finasteride as a therapeutic alternative for the treatment of androgenic alopecia, more cases of melasma began to be seen in men. This drug is associated with hormonal changes, which could cause spots, according to a 2014 case report.
Can the appearance of melasma be prevented?
In theory, the occurrence of these lesions can be prevented by avoiding modifiable risk factors. However, in some cases, it’s difficult to stop using certain types of hormone treatments. It’s best to avoid exposure to sunlight.
The recommendation is to resort to chemical photoprotection, that is, sunscreens. The choice depends a lot on the possibilities of each patient, being necessary to choose the best quality/price ratio and optimize other personal measures to protect yourself.
A sun protection factor (SPF) of type 50+ is recommended. A trusted dermatologist must carry out the pertinent indications, but it usually requires several applications throughout the day and at any time of the year.
Other personal measures are necessary. Wearing hats and glasses are simple habits that can help prevent the appearance of new injuries. Finally, it’s best to avoid the use of irritating cosmetics that are susceptible to chemical modifications when exposed to abundant sunlight.
Is there treatment for melasma?
This condition is recurring, so, in certain circumstances, it can disappear on its own. However, even more so when a patient is exposed to permanent risk factors, there are therapeutic alternatives to reduce symptoms. These not only have an effect on the size of the lesions, but also on the psychological manifestations.
Topical treatment isn’t only the most effective, but is also associated with far fewer adverse effects. This has the particularity that it’s preferred in polytherapy, which means that combinations between several drugs are preferred.
Topical treatment
The most commonly used medications are hydroquinone, retinoids, and steroids. Hydroquinone has the advantage of producing very few adverse effects.
Retinoids are derivatives of vitamin A and are widely used in dermatology, both orally and topically. This last presentation isn’t recommended in pregnant women, since it’s known to have a teratogenic effect.
When speaking of steroids, reference is being made to a group of similar substances that usually have an immunosuppressive effect. This decreases inflammation in the lesions and promotes satisfactory improvements, but they are not recommended as sole therapy.

Systemic treatment
The options are more limited than in the previous section and include tranexamic acid, carotenoids, and melatonin. Most of these therapeutic alternatives are recommended in the long term and require the combination with powerful sunscreens to avoid the appearance of new lesions.
An important aesthetic issue
Melasma has an important aesthetic aspect, so alternatives are valued to improve the appearance of the spots in people who want to remove or reduce them. Did you know that there are tools for it?
Superficial chemoexfoliation is one of them. It isn’t used as first-line therapy, but is reserved for cases in which topical or oral treatment has failed.
Carrying out this procedure involves applying chemical substances to the skin in order to eliminate dead cells. Added medications include glycolic acid and tretinoin. Always remember to consult an expert if you decide to use one of these approaches.
- Alcalá D, Espinosa N, Jurado F. Melasma en hombres. Rev Cent Dermatol Pascua 2015;24(1):14-20.
- Arellano I, et al. Melasma: Consenso del Grupo Mexicano para el Estudio de los Trastornos Pigmentarios. Dermatología CMQ 2007;5(2):112-122.
- Arellano I, et al. Guías de diagnóstico y manejo de melasma. Dermatología CMQ 2017;16(1):12-23.
- Famenini S, Gharavi NM, Beynet DP. Finasteride associated melasma in a Caucasian male. J Drugs Dermatol. 2014 Apr;13(4):484-6. PMID: 24719069.
- Juárez M, De La Cruz J, Baena A. Melasma en Atención Primaria. Med Fam Andal 2017;18(2):168-175.
- Miniño M, Hernández-Lara P. Exfoliación química (peelings): su utilidad en la dermatología actual. Dermatología CMQ 2003;1(4):236-246.
- Ogbechie-Godec, Oluwatobi A., and Nada Elbuluk. “Melasma: an up-to-date comprehensive review.” Dermatology and therapy 7.3 (2017): 305-318.
- Kwon, Soon-Hyo, et al. “Heterogeneous pathology of melasma and its clinical implications.” International Journal of Molecular Sciences 17.6 (2016): 824.
- McKesey, Jacqueline, Andrea Tovar-Garza, and Amit G. Pandya. “Melasma treatment: an evidence-based review.” American journal of clinical dermatology 21.2 (2020): 173-225.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







