Glaucoma: Symptoms, Causes and Treatments

Escrito y verificado por el biólogo Samuel Antonio Sánchez Amador
Glaucoma is the leading cause of irreversible blindness worldwide and represents a serious public health problem. The current prevalence is about 60 million patients, of which 8.4 million are blind. This number is increasing each year, and so it’s estimated that by 2040 there’ll be about 11.8 million people with glaucoma.
These numbers are breathtaking, but the bad news doesn’t end here. Despite receiving the correct treatment, 10% of glaucoma patients experience some loss of vision. In addition, there’s no cure for the damage caused by this condition, as once you lose your sight you don’t recover.
Fortunately, the progression of the disease can be stopped through a series of clinical approaches. For this reason, it’s essential to detect the disease early, as indicated by the UN News portal, 90% of blindness due to glaucoma can be prevented with early detection and treatment.
The functioning of the eye
Before entering fully into the clinical world of glaucoma, we find it interesting to establish some physiological bases on one of the most important structures of our body: the eyes. Each of them is defined as a visual organ that detects light and converts it into electrochemical impulses, whose function is to travel through the optic nerve to the brain.
The MSD Manuals portal and other sources specialized in ophthalmology show us the essential parts of the eye apparatus. We summarize them briefly in the following list:
- Orbit: A bony cavity that houses the eyeball. It’s a basin formed by 7 convergent bones. Its function is to protect and anchor, as 6 different muscles (the extraocular ones) rest on these bone structures that allow the movements of the eyes.
- Sclera: A layer of thick, tough tissue (the white of the eye) that covers almost the entire surface of the eyeball.
- Conjunctiva: A thin, transparent membrane that protects the sclera and helps lubricate the eye.
- Cornea: A transparent and curved layer located in front of the iris and the pupil, whose function is to act as a protective barrier and concentrate light on the retina.
- Pupil: The black point located in the center of the eye.
- Iris: A colored circular area that surrounds the pupil. It controls the amount of light that enters the eye.
- Lens: This is behind the iris and changes the way light is focused on the retina.
- Retina: It contains cells that perceive light (photoreceptors) and the blood vessels that nourish them.
We have missed many structures along the way, but with this general map of the ocular structure, it’s more than enough to understand the pathology at hand.
In short, light passes through the cornea, aqueous humor, pupil, lens, and vitreous before reaching the retina. Once it has passed through all these structures, a real and inverted image is formed in the retina, which will be carried by the optic nerve to the cerebral cortex. This is where the stimulus is interpreted.
What is glaucoma?
Aqueous humor is a colorless liquid found between the anterior and posterior chambers of the eye. Its main function is to nourish and oxygenate ocular structures that aren’t directly irrigated by blood capillaries, such as the cornea and lens.
In a healthy person, aqueous humor leaves the eye through the pupil, and is then absorbed into the bloodstream through a drainage system. As indicated by the Glaucoma.org portal, if the drainage is adequate, then the pressure of the eye remains normal: the regulation of this fluid is an active, continuous, and necessary process for eye health.
Glaucoma and intraocular pressure
The intraocular pressure (IOP) is the value that quantifies the pressure exerted by the aqueous humor in the ocular apparatus. In general, a normal value is considered to be between 10 and 20 millimeters of mercury. Based on this premise, it’s essential to know that most types of glaucoma occur when the drainage system becomes clogged and aqueous humor accumulates.
As this fluid is stored between the anterior and posterior chambers of the eye, an increase in intraocular pressure occurs, which can permanently damage the optic nerve. If the damage is continuous and not treated, the dreaded loss of vision occurs.
Although a high intraocular pressure favors the appearance of glaucoma, it doesn’t explain it in all cases. Many people can have a high IOP and never develop glaucoma. On the other hand, not all glaucoma patients have an elevated IOP. This relationship is likely, but it doesn’t occur in all people, far from it.
Why does it happen?
After having looked in depth at the pathology itself, the next step is always to try to find the causes. Glaucoma is the consequence of damage to the optic nerve and its consequent deterioration. As this structure is affected, blind spots begin to appear in the patient’s vision, as indicated by the Mayo Clinic.
Based on the possible causes of glaucoma, different varieties of the disease can be differentiated. We’re now going to show them to you.
Open-angle glaucoma
This is the most frequent form of the pathology, as it represents more than 90% of all cases. This variant of glaucoma is based on the following main pillars:
- It’s caused by the slow clogging of the drainage channels described above. The accumulation of fluid causes an increase in intraocular pressure (IOP).
- It has a wide-open angle between the iris and the cornea, hence its name. Despite an adequate drainage angle, the trabecular meshwork (network of spongy tissues around the base of the cornea) is partially blocked. Therefore, aqueous humor accumulates.
- It develops slowly and is a lifelong condition. This condition is also known as “the thief of sight”, as its symptoms appear gradually and over time.
- It has symptoms and effects that aren’t noticed at first glance.
Angle-closure glaucoma
This is a much less frequent form, but it also carries serious health problems globally. Without going any further, the Mexican Journal of Ophthalmology estimated that 5.3 million people would be blind due to this pathological variant in 2020.
In this disease, the aqueous humor drainage channels are blocked, so there’s a clear angle between the iris and the cornea. Unlike its stealthy brother, angle-closure glaucoma comes on very quickly, causes very noticeable symptoms, and requires immediate medical attention.
Normal-tension glaucoma
This time the optic nerve is damaged despite normal intraocular pressure. The exact cause isn’t known, but it’s suspected that it could be due to an intrinsic weakness of the optic nerve or a lack of blood supply to it.
Congenital glaucoma
In congenital glaucoma, there’s a birth defect in the development of the angle described above. As a consequence, there’s an increase in intraocular pressure and damage to the optic nerve in the first stages of the patient’s life. It’s a rare condition, affecting only 1 in 30,000 live newborns.
Pigmentary glaucoma
On this occasion, the granules that pigment the iris accumulate in the drainage channel, preventing the aqueous humor from leaking correctly. It’s the most common type in young adults, and up to 50% of people who suffer from pigment dispersion syndrome will develop it, as indicated by the Baviera Clinic.
Symptoms
In most cases, glaucoma progresses silently to advanced stages, as almost all patients experience the open-angle variant. Little by little, the individual loses lateral vision and blind spots appear, which frequently occur in both eyes.
In the more advanced stages, an event known as “tunnel vision” occurs. This clinical manifestation receives this name because the patient loses lateral sight and extension of his visual field, so he perceives the images as if he were inside a tunnel.
In the less frequent variants of glaucoma (closed-angle), other symptoms can appear, some of them very serious. Of all the possible ones, we can highlight the following:
- Blurry vision
- Eye pain and headache
- Nausea and vomiting
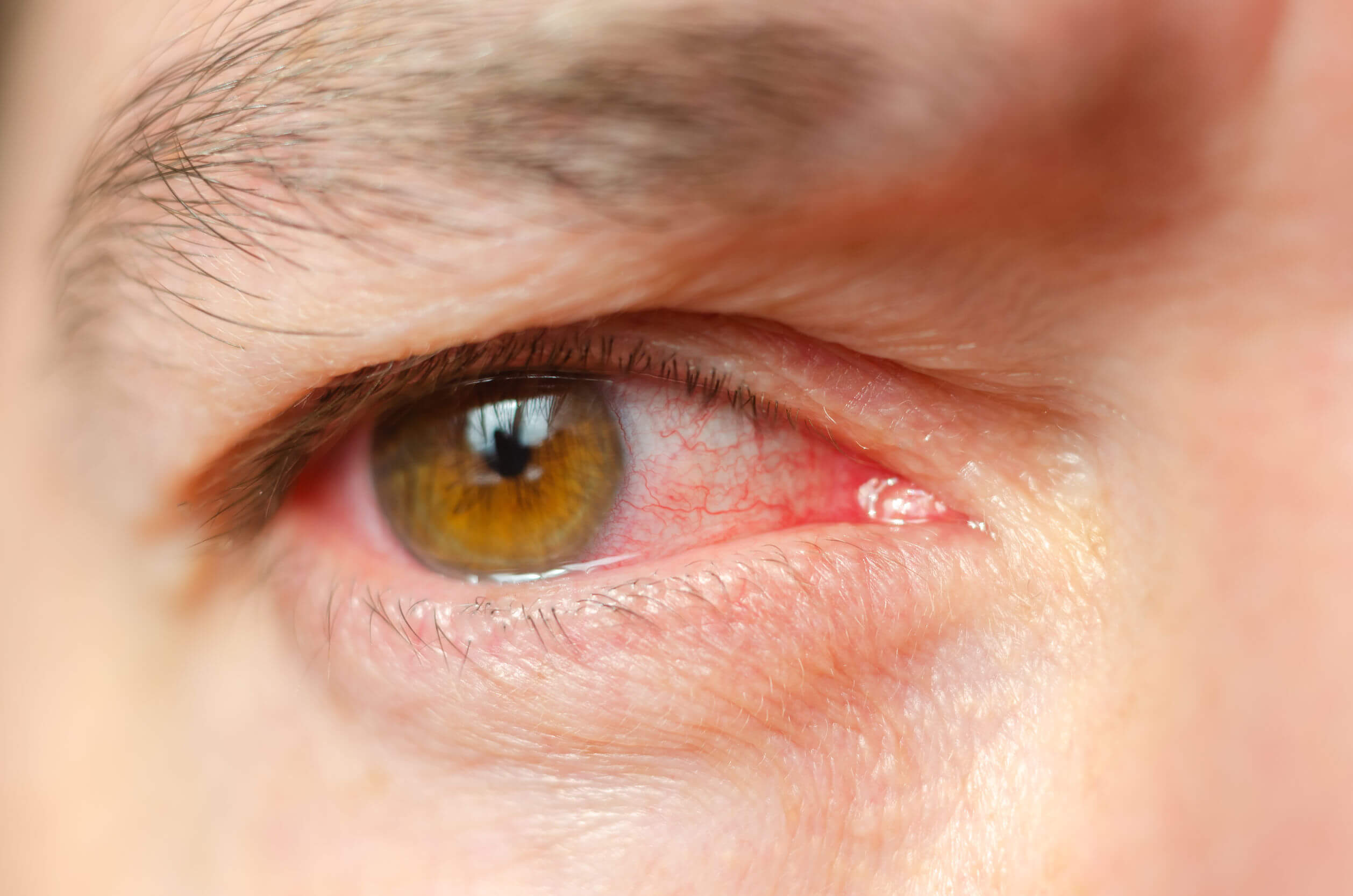
- Redness of the eyes
- The appearance of halos around lights
As you can see, the symptoms vary depending on the variant suffered by the patient. Closed-angle glaucoma presents in an obvious and aggressive way, while open-angle glaucoma progresses slowly and isn’t noticed, in many cases, until it’s too late. However, both variants cause vision loss.
Treatment
The American Academy of Ophthalmology (AAO) indicates that open-angle glaucoma can only be detected, in the early stages, with a comprehensive eye examination. It isn’t even valid with a test that only measures intraocular pressure, because, as we’ve seen, there are patients who develop glaucoma with these normal values.
As we’ve said already, the damage caused by glaucoma can’t be reversed, but it is possible to prevent its progression in the short and long term. Methods already mentioned show us some of the alternatives that can be followed to combat this worrying pathology:
- Medications: Glaucoma can be controlled with the use of certain eye drops. These should be used daily for the rest of the patient’s life, as they’re necessary in order to reduce intraocular pressure.
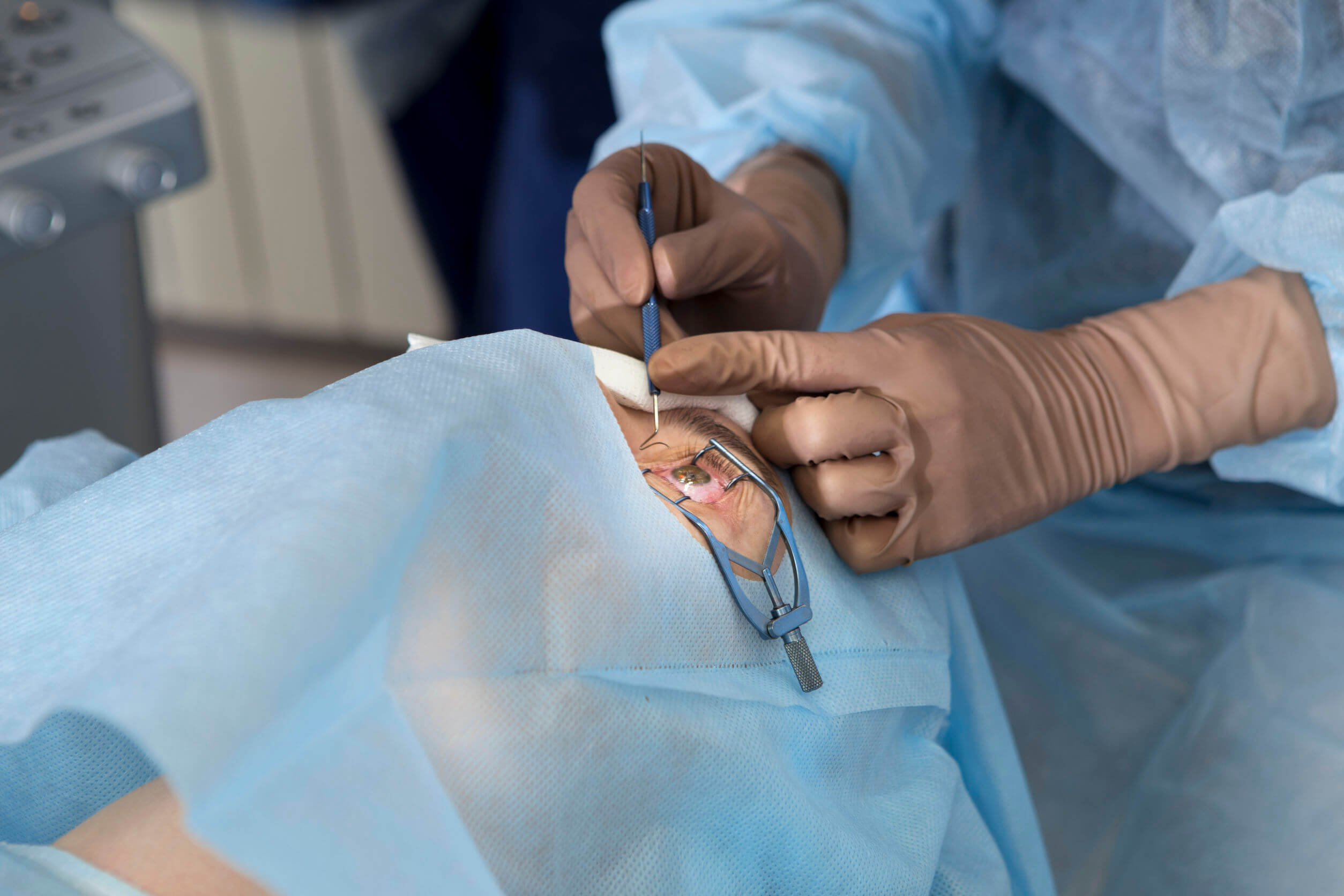
- Surgery with laser: Trabeculoplasty and iridotomy are the procedures included in this section. In both cases, lasers are used to modify the structures involved so that the aqueous humor can flow again correctly.
- Surgical surgery: Drainage devices may be implanted in the eye or a crease created in the sclera so that fluid can drain. In some cases, removal of the ocular lens can help decrease pressure.
Unfortunately, up to 50% of those affected by this pathology don’t know that they have it, and the treatment arrives too late. All of these approaches can delay the condition and reduce intraocular pressure, but not reverse the damage already present. Furthermore, as we’ve said, up to 15% of patients get worse even when they receive the relevant treatment.
A complex and common pathology
We’re facing a very difficult medical condition here, as it’s the leading cause of blindness in the world and up to half of the people who suffer from it aren’t aware of it. The worst thing about open-angle glaucoma isn’t the short-term damage it generates on the optic nerve, but rather that it’s gradual and, in many cases, imperceptible.
As this disease is silent and elusive, we recommend that all adult readers visit the ophthalmologist routinely for appropriate check-ups and tests. A visit to the doctor every 2 years is not much to ask when compared with the benefit of diagnosing glaucoma early on.
Glaucoma is the leading cause of irreversible blindness worldwide and represents a serious public health problem. The current prevalence is about 60 million patients, of which 8.4 million are blind. This number is increasing each year, and so it’s estimated that by 2040 there’ll be about 11.8 million people with glaucoma.
These numbers are breathtaking, but the bad news doesn’t end here. Despite receiving the correct treatment, 10% of glaucoma patients experience some loss of vision. In addition, there’s no cure for the damage caused by this condition, as once you lose your sight you don’t recover.
Fortunately, the progression of the disease can be stopped through a series of clinical approaches. For this reason, it’s essential to detect the disease early, as indicated by the UN News portal, 90% of blindness due to glaucoma can be prevented with early detection and treatment.
The functioning of the eye
Before entering fully into the clinical world of glaucoma, we find it interesting to establish some physiological bases on one of the most important structures of our body: the eyes. Each of them is defined as a visual organ that detects light and converts it into electrochemical impulses, whose function is to travel through the optic nerve to the brain.
The MSD Manuals portal and other sources specialized in ophthalmology show us the essential parts of the eye apparatus. We summarize them briefly in the following list:
- Orbit: A bony cavity that houses the eyeball. It’s a basin formed by 7 convergent bones. Its function is to protect and anchor, as 6 different muscles (the extraocular ones) rest on these bone structures that allow the movements of the eyes.
- Sclera: A layer of thick, tough tissue (the white of the eye) that covers almost the entire surface of the eyeball.
- Conjunctiva: A thin, transparent membrane that protects the sclera and helps lubricate the eye.
- Cornea: A transparent and curved layer located in front of the iris and the pupil, whose function is to act as a protective barrier and concentrate light on the retina.
- Pupil: The black point located in the center of the eye.
- Iris: A colored circular area that surrounds the pupil. It controls the amount of light that enters the eye.
- Lens: This is behind the iris and changes the way light is focused on the retina.
- Retina: It contains cells that perceive light (photoreceptors) and the blood vessels that nourish them.
We have missed many structures along the way, but with this general map of the ocular structure, it’s more than enough to understand the pathology at hand.
In short, light passes through the cornea, aqueous humor, pupil, lens, and vitreous before reaching the retina. Once it has passed through all these structures, a real and inverted image is formed in the retina, which will be carried by the optic nerve to the cerebral cortex. This is where the stimulus is interpreted.
What is glaucoma?

Aqueous humor is a colorless liquid found between the anterior and posterior chambers of the eye. Its main function is to nourish and oxygenate ocular structures that aren’t directly irrigated by blood capillaries, such as the cornea and lens.
In a healthy person, aqueous humor leaves the eye through the pupil, and is then absorbed into the bloodstream through a drainage system. As indicated by the Glaucoma.org portal, if the drainage is adequate, then the pressure of the eye remains normal: the regulation of this fluid is an active, continuous, and necessary process for eye health.
Glaucoma and intraocular pressure
The intraocular pressure (IOP) is the value that quantifies the pressure exerted by the aqueous humor in the ocular apparatus. In general, a normal value is considered to be between 10 and 20 millimeters of mercury. Based on this premise, it’s essential to know that most types of glaucoma occur when the drainage system becomes clogged and aqueous humor accumulates.
As this fluid is stored between the anterior and posterior chambers of the eye, an increase in intraocular pressure occurs, which can permanently damage the optic nerve. If the damage is continuous and not treated, the dreaded loss of vision occurs.
Although a high intraocular pressure favors the appearance of glaucoma, it doesn’t explain it in all cases. Many people can have a high IOP and never develop glaucoma. On the other hand, not all glaucoma patients have an elevated IOP. This relationship is likely, but it doesn’t occur in all people, far from it.
Why does it happen?
After having looked in depth at the pathology itself, the next step is always to try to find the causes. Glaucoma is the consequence of damage to the optic nerve and its consequent deterioration. As this structure is affected, blind spots begin to appear in the patient’s vision, as indicated by the Mayo Clinic.
Based on the possible causes of glaucoma, different varieties of the disease can be differentiated. We’re now going to show them to you.
Open-angle glaucoma
This is the most frequent form of the pathology, as it represents more than 90% of all cases. This variant of glaucoma is based on the following main pillars:
- It’s caused by the slow clogging of the drainage channels described above. The accumulation of fluid causes an increase in intraocular pressure (IOP).
- It has a wide-open angle between the iris and the cornea, hence its name. Despite an adequate drainage angle, the trabecular meshwork (network of spongy tissues around the base of the cornea) is partially blocked. Therefore, aqueous humor accumulates.
- It develops slowly and is a lifelong condition. This condition is also known as “the thief of sight”, as its symptoms appear gradually and over time.
- It has symptoms and effects that aren’t noticed at first glance.
Angle-closure glaucoma
This is a much less frequent form, but it also carries serious health problems globally. Without going any further, the Mexican Journal of Ophthalmology estimated that 5.3 million people would be blind due to this pathological variant in 2020.
In this disease, the aqueous humor drainage channels are blocked, so there’s a clear angle between the iris and the cornea. Unlike its stealthy brother, angle-closure glaucoma comes on very quickly, causes very noticeable symptoms, and requires immediate medical attention.
Normal-tension glaucoma
This time the optic nerve is damaged despite normal intraocular pressure. The exact cause isn’t known, but it’s suspected that it could be due to an intrinsic weakness of the optic nerve or a lack of blood supply to it.
Congenital glaucoma
In congenital glaucoma, there’s a birth defect in the development of the angle described above. As a consequence, there’s an increase in intraocular pressure and damage to the optic nerve in the first stages of the patient’s life. It’s a rare condition, affecting only 1 in 30,000 live newborns.
Pigmentary glaucoma
On this occasion, the granules that pigment the iris accumulate in the drainage channel, preventing the aqueous humor from leaking correctly. It’s the most common type in young adults, and up to 50% of people who suffer from pigment dispersion syndrome will develop it, as indicated by the Baviera Clinic.
Symptoms
In most cases, glaucoma progresses silently to advanced stages, as almost all patients experience the open-angle variant. Little by little, the individual loses lateral vision and blind spots appear, which frequently occur in both eyes.
In the more advanced stages, an event known as “tunnel vision” occurs. This clinical manifestation receives this name because the patient loses lateral sight and extension of his visual field, so he perceives the images as if he were inside a tunnel.
In the less frequent variants of glaucoma (closed-angle), other symptoms can appear, some of them very serious. Of all the possible ones, we can highlight the following:
- Blurry vision
- Eye pain and headache
- Nausea and vomiting
- Redness of the eyes
- The appearance of halos around lights
As you can see, the symptoms vary depending on the variant suffered by the patient. Closed-angle glaucoma presents in an obvious and aggressive way, while open-angle glaucoma progresses slowly and isn’t noticed, in many cases, until it’s too late. However, both variants cause vision loss.
Treatment

The American Academy of Ophthalmology (AAO) indicates that open-angle glaucoma can only be detected, in the early stages, with a comprehensive eye examination. It isn’t even valid with a test that only measures intraocular pressure, because, as we’ve seen, there are patients who develop glaucoma with these normal values.
As we’ve said already, the damage caused by glaucoma can’t be reversed, but it is possible to prevent its progression in the short and long term. Methods already mentioned show us some of the alternatives that can be followed to combat this worrying pathology:
- Medications: Glaucoma can be controlled with the use of certain eye drops. These should be used daily for the rest of the patient’s life, as they’re necessary in order to reduce intraocular pressure.
- Surgery with laser: Trabeculoplasty and iridotomy are the procedures included in this section. In both cases, lasers are used to modify the structures involved so that the aqueous humor can flow again correctly.
- Surgical surgery: Drainage devices may be implanted in the eye or a crease created in the sclera so that fluid can drain. In some cases, removal of the ocular lens can help decrease pressure.
Unfortunately, up to 50% of those affected by this pathology don’t know that they have it, and the treatment arrives too late. All of these approaches can delay the condition and reduce intraocular pressure, but not reverse the damage already present. Furthermore, as we’ve said, up to 15% of patients get worse even when they receive the relevant treatment.
A complex and common pathology
We’re facing a very difficult medical condition here, as it’s the leading cause of blindness in the world and up to half of the people who suffer from it aren’t aware of it. The worst thing about open-angle glaucoma isn’t the short-term damage it generates on the optic nerve, but rather that it’s gradual and, in many cases, imperceptible.
As this disease is silent and elusive, we recommend that all adult readers visit the ophthalmologist routinely for appropriate check-ups and tests. A visit to the doctor every 2 years is not much to ask when compared with the benefit of diagnosing glaucoma early on.
- Día Mundial del Glaucoma: OMS reporta 4,5 millones de afectados por la enfermedad, Noticias ONU. Recogido a 6 de marzo en https://news.un.org/es/story/2009/03/1158791#:~:text=Regiones-,D%C3%ADa%20Mundial%20del%20Glaucoma%3A%20OMS%20reporta%204%2C5%20millones,de%20afectados%20por%20la%20enfermedad&text=El%20glaucoma%20es%20la%20segunda,de%20la%20Salud%20(OMS).
- Estructura y función de los ojos, MSDmanuals. Recogido a 6 de marzo en https://www.msdmanuals.com/es-es/hogar/trastornos-oft%C3%A1lmicos/biolog%C3%ADa-de-los-ojos/estructura-y-funci%C3%B3n-de-los-ojos
- ¿Qué es el glaucoma? Glaucoma Research Foundation. Recogido a 6 de marzo en https://www.glaucoma.org/es/que-es-el-glaucoma.php
- Glaucoma, MayoClinic. Recogido a 6 de marzo en https://www.mayoclinic.org/es-es/diseases-conditions/glaucoma/symptoms-causes/syc-20372839
- Castañeda-Díez, R., Mayorquín-Ruiz, M., & Jiménez-Román, J. (2007). Glaucoma de ángulo cerrado. Perspectiva actual. Revista Mexicana de Oftalmología, 81(5), 272-282.
- ¿Qué es el glaucoma pigmentario? Clínica Baviera. Recogido a 6 de marzo en https://www.clinicabaviera.com/blog/salud-visual/glaucoma-pigmentario/#:~:text=Este%20tipo%20de%20glaucoma%20es,pueden%20evolucionar%20hacia%20un%20glaucoma.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







