What Is Chronic Urticaria?
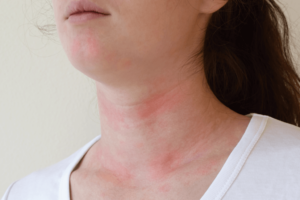
According to the British Skin Foundation, hives are a skin reaction that affects 1 in 5 people at least once in their life. In most cases, it disappears in a matter of hours or days, but others have to deal with flare-ups for weeks or years. These cases are known as chronic urticaria.
According to some researchers, the lifetime prevalence of chronic urticaria ranges from 0.5% to 5% of patients. It often isn’t possible to find the triggers of these reactions, so they’re classified as idiopathic.
Causes of chronic urticaria
Hives occur when a group of cells called mast cells releases histamine and other chemicals near the surface of the skin. Histamine is a substance that the body secretes to fight against allergic reactions, but the truth is that most cases of hives aren’t considered as such.
That is, many (but not all) patients aren’t allergic. So, this chemical reaction remains a mystery to specialists.
Although the exact causes of chronic urticaria aren’t known, there are several hypotheses that have some evidence behind them. The evidence points to the following factors:
- Physical factors: Exogenous mechanical stimuli can produce episodes of chronic urticaria. Many can’t be controlled by patients. For example, changes in temperature (hot or cold), stress, sun exposure, contact with water, friction or exercise.
- Autoimmune reaction: At the end of the 20th century, it was proposed that chronic urticaria could be an autoimmune reaction. This would explain why many patients also develop other disorders, such as systemic lupus erythematosus, rheumatoid arthritis, or cryoglobulinemia.
- Infections: Although the association isn’t entirely clear, studies and research indicate that infections by viruses, parasites and fungi can explain some cases. Some of the possible culprits are Streptococcus, Mycoplasma, Helicobacter pylori, hepatitis B virus, herpes simplex virus and candida.
- Others: The intake of some medications, neurological factors, and direct contact with some triggers can cause this type of urticaria.
Of course, chronic hives can also be a manifestation of an allergic or pseudo-allergic reaction. In this sense, the evidence indicates that these episodes are related to the intake of certain food groups.

Symptoms of chronic urticaria
The symptoms of chronic urticaria are very varied and appear differently in each patient. They’re usually indistinguishable from the acute variant, only this time the manifestations extend for more than 6 weeks.
These are the main characteristics of the disorder. If you develop it for more than 1 month and a half, regardless of whether the signs are intermittent, then your case corresponds to the chronic variant. According to researchers, we can point out the following clinical characteristics:
- Skin rashes of varying shapes and sizes.
- Itching and swelling in the affected areas.
- Angioedema: swelling under the skin, not on the surface.
- Nausea, dizziness, abdominal pain, headache, and shortness of breath (not in all patients).
The manifestations can occur in any part of the body and be general or localized. However, the preferred areas are the arms, legs, and back. Without a doubt, the most characteristic sign is that the rash is accompanied by itching.
This causes the symptoms to get worse and the rashes to grow and join each other. All of this can trigger anxiety.
How is chronic urticaria diagnosed?
Diagnosis of chronic urticaria can be performed on an outpatient basis, although the specialist may order some tests to rule out other explanations. The first thing you’ll do is assess the symptoms, the patient’s history, family history, and day-to-day habits.
To find the possible causes of the episodes, researchers suggest performing different skin stimulation tests (for cold, heat or pressure). This detection process can take several weeks, as exercise and diet must also be ruled out.
The patient will be asked to keep a diary that reflects all the activities that they carried out before an outbreak appeared or worsened. In this way, catalysts can be found more objectively. The doctor will also assess the risk of the person developing an anaphylactic reaction.

Treatment options
Treatment for chronic hives varies according to the trigger. If what is causing the flare-ups is found, the patient can initiate lifestyle changes to minimize the chance of a reaction.
For example, avoid some foods that trigger episodes or reduce sun exposure. The researchers recommend treating symptoms with antihistamines. You can use the first generation or the second generation. Among the latter is loratadine.
The dose is regulated by the doctor and it isn’t uncommon for it to double or triple if there are no improvements during the first weeks. Additionally, the American Academy of Dermatology (AAD) recommends that all patients:
- Avoid stressful situations
- Wear loose clothing whenever possible
- Apply fragrance-free moisturizers several times a day
- Relieve breakouts by applying cold compresses (unless cold is the trigger)
- Avoid applying pressure to the skin (bags and straps can cause breakouts)
- Consult with the specialist if there’s no improvement after the treatment
Knowing the causative agents is essential
Keep in mind that chronic urticaria is a very unpredictable condition. It can last for years with daily flare-ups and then fade for the same amount of time.
The important thing is that you know how to diagnose it, that you’re receiving treatment, and that you put a series of habits in place to avoid exposing yourself to the catalysts. The recognition of the causative agents is the key.
According to the British Skin Foundation, hives are a skin reaction that affects 1 in 5 people at least once in their life. In most cases, it disappears in a matter of hours or days, but others have to deal with flare-ups for weeks or years. These cases are known as chronic urticaria.
According to some researchers, the lifetime prevalence of chronic urticaria ranges from 0.5% to 5% of patients. It often isn’t possible to find the triggers of these reactions, so they’re classified as idiopathic.
Causes of chronic urticaria
Hives occur when a group of cells called mast cells releases histamine and other chemicals near the surface of the skin. Histamine is a substance that the body secretes to fight against allergic reactions, but the truth is that most cases of hives aren’t considered as such.
That is, many (but not all) patients aren’t allergic. So, this chemical reaction remains a mystery to specialists.
Although the exact causes of chronic urticaria aren’t known, there are several hypotheses that have some evidence behind them. The evidence points to the following factors:
- Physical factors: Exogenous mechanical stimuli can produce episodes of chronic urticaria. Many can’t be controlled by patients. For example, changes in temperature (hot or cold), stress, sun exposure, contact with water, friction or exercise.
- Autoimmune reaction: At the end of the 20th century, it was proposed that chronic urticaria could be an autoimmune reaction. This would explain why many patients also develop other disorders, such as systemic lupus erythematosus, rheumatoid arthritis, or cryoglobulinemia.
- Infections: Although the association isn’t entirely clear, studies and research indicate that infections by viruses, parasites and fungi can explain some cases. Some of the possible culprits are Streptococcus, Mycoplasma, Helicobacter pylori, hepatitis B virus, herpes simplex virus and candida.
- Others: The intake of some medications, neurological factors, and direct contact with some triggers can cause this type of urticaria.
Of course, chronic hives can also be a manifestation of an allergic or pseudo-allergic reaction. In this sense, the evidence indicates that these episodes are related to the intake of certain food groups.

Symptoms of chronic urticaria
The symptoms of chronic urticaria are very varied and appear differently in each patient. They’re usually indistinguishable from the acute variant, only this time the manifestations extend for more than 6 weeks.
These are the main characteristics of the disorder. If you develop it for more than 1 month and a half, regardless of whether the signs are intermittent, then your case corresponds to the chronic variant. According to researchers, we can point out the following clinical characteristics:
- Skin rashes of varying shapes and sizes.
- Itching and swelling in the affected areas.
- Angioedema: swelling under the skin, not on the surface.
- Nausea, dizziness, abdominal pain, headache, and shortness of breath (not in all patients).
The manifestations can occur in any part of the body and be general or localized. However, the preferred areas are the arms, legs, and back. Without a doubt, the most characteristic sign is that the rash is accompanied by itching.
This causes the symptoms to get worse and the rashes to grow and join each other. All of this can trigger anxiety.
How is chronic urticaria diagnosed?
Diagnosis of chronic urticaria can be performed on an outpatient basis, although the specialist may order some tests to rule out other explanations. The first thing you’ll do is assess the symptoms, the patient’s history, family history, and day-to-day habits.
To find the possible causes of the episodes, researchers suggest performing different skin stimulation tests (for cold, heat or pressure). This detection process can take several weeks, as exercise and diet must also be ruled out.
The patient will be asked to keep a diary that reflects all the activities that they carried out before an outbreak appeared or worsened. In this way, catalysts can be found more objectively. The doctor will also assess the risk of the person developing an anaphylactic reaction.

Treatment options
Treatment for chronic hives varies according to the trigger. If what is causing the flare-ups is found, the patient can initiate lifestyle changes to minimize the chance of a reaction.
For example, avoid some foods that trigger episodes or reduce sun exposure. The researchers recommend treating symptoms with antihistamines. You can use the first generation or the second generation. Among the latter is loratadine.
The dose is regulated by the doctor and it isn’t uncommon for it to double or triple if there are no improvements during the first weeks. Additionally, the American Academy of Dermatology (AAD) recommends that all patients:
- Avoid stressful situations
- Wear loose clothing whenever possible
- Apply fragrance-free moisturizers several times a day
- Relieve breakouts by applying cold compresses (unless cold is the trigger)
- Avoid applying pressure to the skin (bags and straps can cause breakouts)
- Consult with the specialist if there’s no improvement after the treatment
Knowing the causative agents is essential
Keep in mind that chronic urticaria is a very unpredictable condition. It can last for years with daily flare-ups and then fade for the same amount of time.
The important thing is that you know how to diagnose it, that you’re receiving treatment, and that you put a series of habits in place to avoid exposing yourself to the catalysts. The recognition of the causative agents is the key.
- Godse, K. V. (2009). Chronic urticaria and treatment options. Indian journal of dermatology. 2009; 54(4), 310.
- Magen E, Mishal J, Schlesinger M, Scharf S. Eradication of Helicobacter pylori infection equally improves chronic urticaria with positive and negative autologous serum skin test. 2007 Oct;12(5):567-71.
- Moneret-Vautrin DA. Urticaires chroniques d’origine alimentaire [Allergic and pseudo-allergic reactions to foods in chronic urticaria]. Ann Dermatol Venereol. 2003 May;130 Spec No 1:1S35-42.
- Sachdeva S, Gupta V, Amin SS, Tahseen M. Chronic urticaria. Indian J Dermatol. 2011 Nov;56(6):622-8.
- Schaefer P. Acute and Chronic Urticaria: Evaluation and Treatment. Am Fam Physician. 2017 Jun 1;95(11):717-724.
- Schoepke N, Doumoulakis G, Maurer M. Diagnosis of urticaria. Indian J Dermatol. 2013 May;58(3):211-8.
- Wai YC, Sussman GL. Evaluating chronic urticaria patients for allergies, infections, or autoimmune disorders. Clin Rev Allergy Immunol. 2002 Oct;23(2):185-93.
- Wedi B, Raap U, Kapp A. Chronic urticaria and infections. Curr Opin Allergy Clin Immunol. 2004 Oct;4(5):387-96.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







