Prions: What Are They and What Diseases Do They Cause?
Thousands of infectious agents are capable of causing disease. Many of these organisms have been studied over the years and are well known. However, there are little-studied particles, such as prions, that are capable of causing incurable and fatal diseases too.
These pathogens cause a group of diseases known as spongiform encephalopathies that affect some mammals, including humans. They get this name because of the many microscopic holes they make in brain cells, which mimic the appearance of a sponge.
Prions have many mechanisms that are currently unknown. This is because the diseases they produce have a low incidence in the world population, so they haven’t been studied in depth.
What are prions?
Also known as scrapie proteins or PrP Sc, they are very peculiar pathogens, since they aren’t living organisms like bacteria or parasites, nor do they have genetic material like viruses. They come from a normal protein called cellular prion protein (PrP C ), which has an unknown function in the brain.
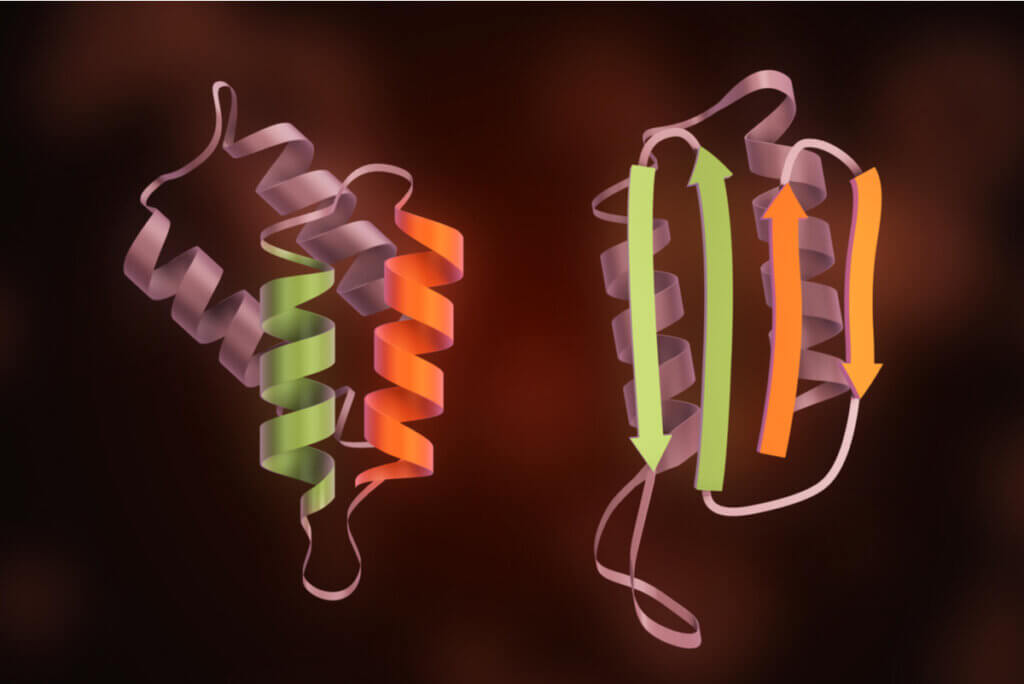
All proteins undergo a folding process through which they acquire their three-dimensional structure. However, the cellular prion protein can fold incorrectly, giving rise to prions.
These new pathogenic proteins aren’t water soluble, so they aren’t capable of disintegrating in water. In addition, they’re also resistant to the enzymes responsible for destroying them, known as proteases. In this way, the compound remains intact in the brain and will gradually accumulate.
Mutated proteins are self-replicating, that is, they have the ability to transform nearby PrP C into their pathogenic form. So the protein concentration of scrapie will increase over time. When a certain concentration is reached, the symptoms will appear.
The high concentration of pathogens will give rise to multiple histological changes in the brain, among which the formation of small bubbles in the cells and microscopic holes stand out. All of these changes will ultimately result in neuronal death.
Prion-borne diseases
As previously stated, prions cause a group of neurodegenerative diseases called spongiform encephalopathies. These can affect humans and animals alike, causing serious neurological problems and behavioral changes.
These pathologies are characterized by long incubation periods, which can take years after the initial exposure. The symptoms may vary, depending on the encephalopathy presented, however, rapidly progressing dementia is a factor that all of them have in common.
In the case of animals, the best-documented disease is bovine spongiform encephalopathy, also known as mad cow disease. For their part, in humans, they can be divided into three different groups.

1. Sporadic prion diseases
Sporadic prion diseases are the most common form of presentation. However, how the first prion is formed in the body is still unknown. The most accepted theory is that it’s an error in cell metabolism, but more studies are necessary.
Creutzfeldt-Jakob disease (CJD)
This is the most frequent pathology of all and studies establish that it’s diagnosed in 1 person per year for every million inhabitants. The average age of onset of symptoms is over 40 years of age. Among the symptoms presented by the patients, the following stand out:
- Amnesia and confusion
- Gait disturbances and lack of coordination
- involuntary muscle movements
- Psychiatric disorders such as anxiety or depression
- Dementia
Once it’s detected, the disease has a rapid evolution, producing the death of the patient in a period that can vary between 4 months and 2 years.
Fatal insomnia
Fatal insomnia differs from the rest of the pathologies produced by prions by affecting to a greater extent a part of the brain called the thalamus, which is in charge of controlling the sleep-wake cycle.
This usually appears after the age of 30 and includes cognitive deterioration and the inability to perform voluntary movements, or ataxia. This form of presentation isn’t characterized by the presence of problems associated with sleep, however, during an electroencephalogram it’s possible to notice various changes.
This specific pathology is less aggressive than Creutzfeldt-Jakob disease, with a life expectancy of more than 6 years after diagnosis.
Variable protease-sensitive prionopathy
This is a variation identified in 2008, which is characterized by the ability of proteases to destroy prions. Protease-responsive variable prionopathy usually occurs in patients older than 70, and there’s a life expectancy of only 24 months after the onset of symptoms.
Studies establish that it represents between 3% and 5% of all prionopathies. In addition, among the symptoms of the disease include the following:
- Loss of inhibition
- Euphoria of inexplicable origin
- Loss of interest in usual activities
- Speech problems and lack of coordination
- Impaired mental function
2. Familial prion diseases
Unlike the previous group, in familial prion diseases, it has been possible to associate the appearance of the first prions with a mutation in the PrP C gene that can be hereditary. Here we can also find CJD and fatal insomnia.
Familial Creutzfeldt-Jakob disease (CJD)
This form of presentation accounts for 10% of all CJD cases and various studies have associated its appearance with possible codon 129 genotypes. Symptoms and life expectancy don’t vary greatly with respect to the sporadic form.
Familial fatal insomnia
The familial form of fatal insomnia is much more aggressive than the sporadic form and reduces the patient’s life expectancy to a maximum of 6 years after diagnosis. Studies have confirmed that its appearance is the product of mutations in the PNRP gene.
Its main difference with respect to the sporadic form lies in the fact that the patient will experience sleep-related problems. At first, it will be difficult to fall asleep, however, it will worsen until the ability to sleep is lost.
Gerstmann-Sträussler-Scheinker disease
This disease is very similar to CJD, however it appears in younger patients and has a slower progression. In this sense, it’s diagnosed in patients between 30 and 40 years of age and gives a life expectancy of at least 5 years after diagnosis.
Like fatal familial insomnia, its onset is related to an alteration in the PNRP gene, according to the Genetic and Rare Diseases Information Center. The clinic is the same as that of CJD, however, patients also usually report the following signs:
- Nystagmus (involuntary eye movements)
- Deafness
- Stiffness and muscle incoordination
- Respiratory muscle disease
3. Contracted prion diseases
There’s very little scientific documentation to support the appearance of contracted prion diseases, since they’re the rarest form of presentation of all. However, they’re produced by one of the following situations:
- Ingestion of contaminated meat: animal or human.
- Organ transplant or blood donation with prions.
- Brain surgery with materials contaminated with prions.
- Injection of contaminated substances.
The best-documented contracted prion disease is Kuru, recorded in the Fore community in New Guinea. The inhabitants of said town used to practice cannibalism as a kind of ritual, which resulted in the consumption of contaminated human brain mass.
Prions are a strange pathogen
For many years, prions represented a real challenge for doctors. They even considered them to be a virus. However, today it’s known that these are proteins present in all humans, which can become pathogens for various reasons.
No effective treatment for prion-produced diseases has been discovered, so the death of the sufferer is inevitable. Despite this, it’s possible to take certain measures to improve the symptoms and offer greater comfort to the affected person.
Thousands of infectious agents are capable of causing disease. Many of these organisms have been studied over the years and are well known. However, there are little-studied particles, such as prions, that are capable of causing incurable and fatal diseases too.
These pathogens cause a group of diseases known as spongiform encephalopathies that affect some mammals, including humans. They get this name because of the many microscopic holes they make in brain cells, which mimic the appearance of a sponge.
Prions have many mechanisms that are currently unknown. This is because the diseases they produce have a low incidence in the world population, so they haven’t been studied in depth.
What are prions?
Also known as scrapie proteins or PrP Sc, they are very peculiar pathogens, since they aren’t living organisms like bacteria or parasites, nor do they have genetic material like viruses. They come from a normal protein called cellular prion protein (PrP C ), which has an unknown function in the brain.
All proteins undergo a folding process through which they acquire their three-dimensional structure. However, the cellular prion protein can fold incorrectly, giving rise to prions.
These new pathogenic proteins aren’t water soluble, so they aren’t capable of disintegrating in water. In addition, they’re also resistant to the enzymes responsible for destroying them, known as proteases. In this way, the compound remains intact in the brain and will gradually accumulate.
Mutated proteins are self-replicating, that is, they have the ability to transform nearby PrP C into their pathogenic form. So the protein concentration of scrapie will increase over time. When a certain concentration is reached, the symptoms will appear.
The high concentration of pathogens will give rise to multiple histological changes in the brain, among which the formation of small bubbles in the cells and microscopic holes stand out. All of these changes will ultimately result in neuronal death.
Prion-borne diseases
As previously stated, prions cause a group of neurodegenerative diseases called spongiform encephalopathies. These can affect humans and animals alike, causing serious neurological problems and behavioral changes.
These pathologies are characterized by long incubation periods, which can take years after the initial exposure. The symptoms may vary, depending on the encephalopathy presented, however, rapidly progressing dementia is a factor that all of them have in common.
In the case of animals, the best-documented disease is bovine spongiform encephalopathy, also known as mad cow disease. For their part, in humans, they can be divided into three different groups.

1. Sporadic prion diseases
Sporadic prion diseases are the most common form of presentation. However, how the first prion is formed in the body is still unknown. The most accepted theory is that it’s an error in cell metabolism, but more studies are necessary.
Creutzfeldt-Jakob disease (CJD)
This is the most frequent pathology of all and studies establish that it’s diagnosed in 1 person per year for every million inhabitants. The average age of onset of symptoms is over 40 years of age. Among the symptoms presented by the patients, the following stand out:
- Amnesia and confusion
- Gait disturbances and lack of coordination
- involuntary muscle movements
- Psychiatric disorders such as anxiety or depression
- Dementia
Once it’s detected, the disease has a rapid evolution, producing the death of the patient in a period that can vary between 4 months and 2 years.
Fatal insomnia
Fatal insomnia differs from the rest of the pathologies produced by prions by affecting to a greater extent a part of the brain called the thalamus, which is in charge of controlling the sleep-wake cycle.
This usually appears after the age of 30 and includes cognitive deterioration and the inability to perform voluntary movements, or ataxia. This form of presentation isn’t characterized by the presence of problems associated with sleep, however, during an electroencephalogram it’s possible to notice various changes.
This specific pathology is less aggressive than Creutzfeldt-Jakob disease, with a life expectancy of more than 6 years after diagnosis.
Variable protease-sensitive prionopathy
This is a variation identified in 2008, which is characterized by the ability of proteases to destroy prions. Protease-responsive variable prionopathy usually occurs in patients older than 70, and there’s a life expectancy of only 24 months after the onset of symptoms.
Studies establish that it represents between 3% and 5% of all prionopathies. In addition, among the symptoms of the disease include the following:
- Loss of inhibition
- Euphoria of inexplicable origin
- Loss of interest in usual activities
- Speech problems and lack of coordination
- Impaired mental function
2. Familial prion diseases
Unlike the previous group, in familial prion diseases, it has been possible to associate the appearance of the first prions with a mutation in the PrP C gene that can be hereditary. Here we can also find CJD and fatal insomnia.
Familial Creutzfeldt-Jakob disease (CJD)
This form of presentation accounts for 10% of all CJD cases and various studies have associated its appearance with possible codon 129 genotypes. Symptoms and life expectancy don’t vary greatly with respect to the sporadic form.
Familial fatal insomnia
The familial form of fatal insomnia is much more aggressive than the sporadic form and reduces the patient’s life expectancy to a maximum of 6 years after diagnosis. Studies have confirmed that its appearance is the product of mutations in the PNRP gene.
Its main difference with respect to the sporadic form lies in the fact that the patient will experience sleep-related problems. At first, it will be difficult to fall asleep, however, it will worsen until the ability to sleep is lost.
Gerstmann-Sträussler-Scheinker disease
This disease is very similar to CJD, however it appears in younger patients and has a slower progression. In this sense, it’s diagnosed in patients between 30 and 40 years of age and gives a life expectancy of at least 5 years after diagnosis.
Like fatal familial insomnia, its onset is related to an alteration in the PNRP gene, according to the Genetic and Rare Diseases Information Center. The clinic is the same as that of CJD, however, patients also usually report the following signs:
- Nystagmus (involuntary eye movements)
- Deafness
- Stiffness and muscle incoordination
- Respiratory muscle disease

3. Contracted prion diseases
There’s very little scientific documentation to support the appearance of contracted prion diseases, since they’re the rarest form of presentation of all. However, they’re produced by one of the following situations:
- Ingestion of contaminated meat: animal or human.
- Organ transplant or blood donation with prions.
- Brain surgery with materials contaminated with prions.
- Injection of contaminated substances.
The best-documented contracted prion disease is Kuru, recorded in the Fore community in New Guinea. The inhabitants of said town used to practice cannibalism as a kind of ritual, which resulted in the consumption of contaminated human brain mass.
Prions are a strange pathogen
For many years, prions represented a real challenge for doctors. They even considered them to be a virus. However, today it’s known that these are proteins present in all humans, which can become pathogens for various reasons.
No effective treatment for prion-produced diseases has been discovered, so the death of the sufferer is inevitable. Despite this, it’s possible to take certain measures to improve the symptoms and offer greater comfort to the affected person.
- Mandujano A, Montes S, Guzmán A, Espinosa B, Rembao D, Martínez-Cairo S, Zenteno E, Guevara J. Fisiopatología de las enfermedades por priones. Gac Med Mex. 2006; 142 (5): 399-406.
- Perrone M, Dinatale E, Pardi G, Guilarte C, De Stefano A, Pacheco A et al . Prión: un agente infeccioso que causa conmoción en la comunidad científica. Acta odontol. venez [Internet]. 2003; 41(1): 87-87.
- Barashi Gozal N, Vargas Acevedo C, Zarco L. Enfermedades priónicas humanas. Universitas Médica. 2013; 54(4): 495-516.
- Sergio A, Rodríguez Q. Prionopatía proteasa-sensible variable: una nueva forma esporádica de enfermedad priónica. Neurología Argentina. 2010; 2(3): 215.
- Arranz-Martínez E, Trillo-Sánchez-Redondo G, Ruiz-García A, Ares-Blanco S. Prionpatías: las encefalopatías por priones. SEMERGEN – Medicina de Familia. 2010; 36(8): 443-448.
- Gambetti P. Introducción a las enfermedades producidas por priones – Enfermedades cerebrales, medulares y nerviosas [Internet]. Manual MSD versión para público general. 2018 [cited 10 December 2020].
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







