Nodular Acne: Everything You Need to Know
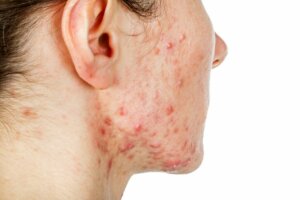
In the area of dermatology, one of the most frequent reasons for consultation is acne. And, although we tend to think of this as something typical of puberty, it’s actually a condition that can have several different types of manifestations and levels of severity. In this sense, one of the most severe forms of acne is nodular acne (also called nodulocystic acne).
In fact, this type of acne is classified as grade 4 acne, according to the scale known as Investigator’s Global Assessment (IGA). This means that it produces lesions that are much deeper and more difficult to treat than other more common forms of acne. Let’s learn more about it below to understand why.
Nodular acne symptoms
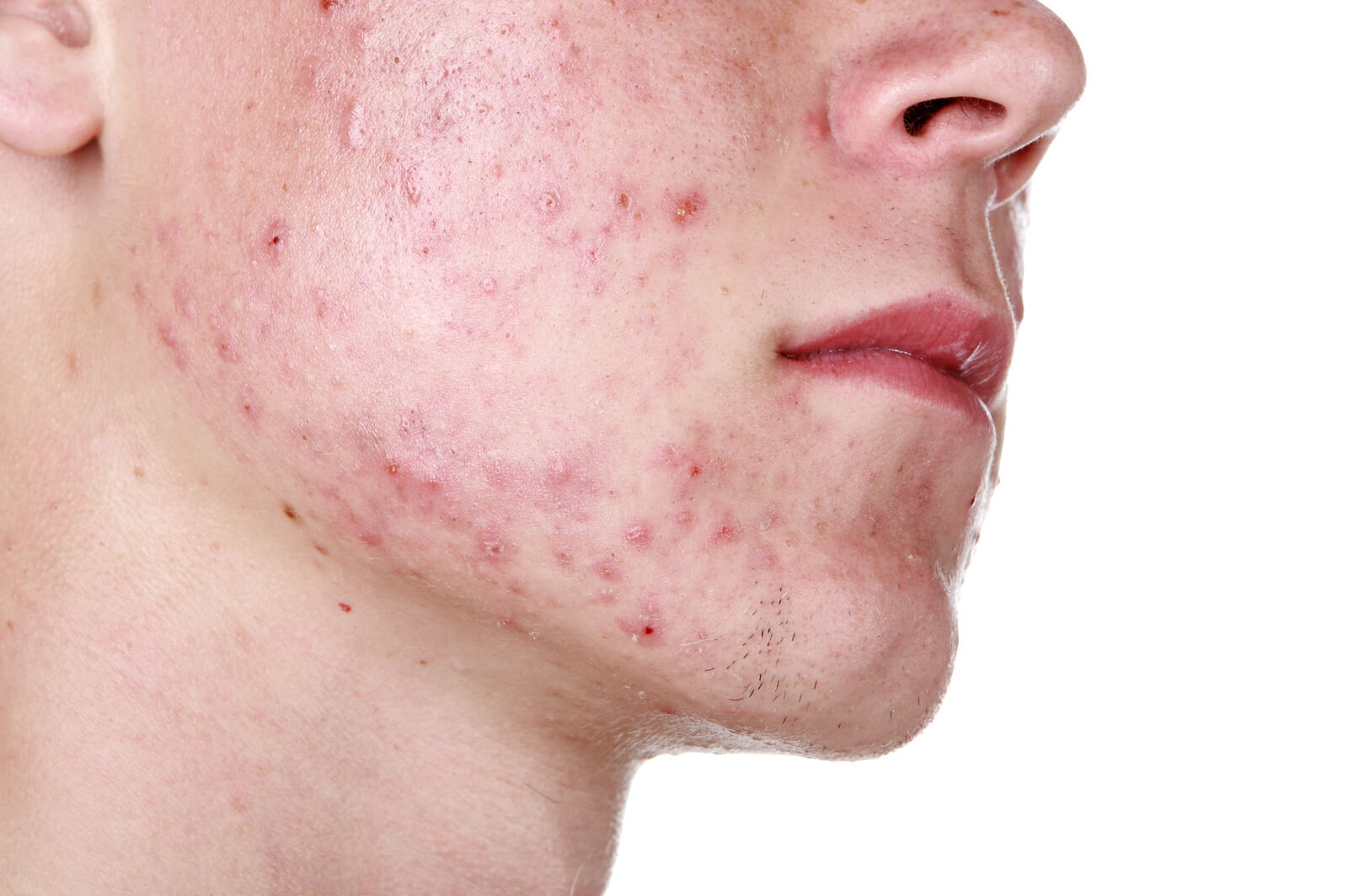
As its name implies, one of nodular acne’s main characteristics is that it causes nodules to appear on the skin. These inflammatory and infiltrating lesions don’t always evolve into abscesses, or spots, as is often the case in acne conglobata. However, the nodules can be very painful and leave noticeable marks.
The nodules have the appearance of large grains (which may be greater than 1 centimeter (0.4 inches) in diameter), very swollen, of rounded size and reddish in color. They don’t have a spontaneous expulsion like blackheads and pimples. That’s why they’re so painful and easily leave noticeable scars.
Regarding nodules, experts clarify the following:
“Cystic nodular acne is characterized by inflammations mainly composed of lymphocytes and giant cells, while pustular lesions are composed of a neutrophilic infiltrate.”
We should note that nodules aren’t the only type of injury that nodular acne can cause. These happen to be the most prominent, when compared to other lesions. In this way, a person with nodular acne may also have persistent blackheads, pustules, and papules.
On the other hand, it’s important to note that nodules don’t only affect the face, neck, and upper part of the trunk. It can spread throughout the chest and back and reach other parts of the body.
In addition to the lesions, it’s common for patients to suffer from seborrhea, an alteration of the sebaceous glands that, as a consequence, causes the skin to present an exaggerated amount of sebum.
Contrary to what people often think, nodular acne and acne conglobata aren’t the same. The second is a variant of the first, along with fulminant acne and facial pyoderma.
Causes
Acne is a skin condition that doesn’t have a single cause, whatever its type. This is confirmed by numerous studies, such as that published in the Venezuelan Archives of Pharmacology and Therapeutics magazine. This report also explains the various factors that influence the appearance of acne:
“Environmental, hormonal [androgen], nutritional, immunological, infectious and genetic components. The latter seems to be especially important, and is present in sporadic cases as well as in familial patterns.”
On the other hand, experts consider that the incidence of nodular acne is higher in men (adolescents and young adults). Having said that, it can also affect adult women, especially those who suffer from polycystic ovary syndrome, according to the hypotheses of recent decades.
Treatment

Unfortunately, over-the-counter treatments and skin cleansers (soaps, gels, scrubs, creams, etc.) aren’t effective against this type of acne.
- The treatment of nodular acne must be intensive. It may include an oral antibiotic, retinoids, benzoyl peroxide, and emollients.
- For women, hormonal treatment may be considered.
- As indicated in scientific literature, isotretinoin is commonly included in the treatment of severe nodulocystic acne, as well as comedonal or papulopustular acne that’s resistant to topical treatments and the newer systemic antibiotics.
Living with nodular acne
Experts don’t recommend that people with nodular acne attempt to touch their lesions at home in any way. Not only can this cause more pain and inflammation, but it can also make the wounds (and later scars) even deeper and harder to treat.
To reduce inflammation or mitigate pain, you can use ice packs (always wrapped in gauze or a clean, fine cloth, to prevent skin burns). And, in more severe cases, the doctor may prescribe cortisone injections, although these tend to be left as a last resort.
As a final recommendation, we can highlight the importance of going to the dermatologist in the event of any aggravation or concern that may arise during the treatment. In this way, not only can the problem be addressed in the most appropriate way, but further damage to the skin can also be prevented.
In the area of dermatology, one of the most frequent reasons for consultation is acne. And, although we tend to think of this as something typical of puberty, it’s actually a condition that can have several different types of manifestations and levels of severity. In this sense, one of the most severe forms of acne is nodular acne (also called nodulocystic acne).
In fact, this type of acne is classified as grade 4 acne, according to the scale known as Investigator’s Global Assessment (IGA). This means that it produces lesions that are much deeper and more difficult to treat than other more common forms of acne. Let’s learn more about it below to understand why.
Nodular acne symptoms

As its name implies, one of nodular acne’s main characteristics is that it causes nodules to appear on the skin. These inflammatory and infiltrating lesions don’t always evolve into abscesses, or spots, as is often the case in acne conglobata. However, the nodules can be very painful and leave noticeable marks.
The nodules have the appearance of large grains (which may be greater than 1 centimeter (0.4 inches) in diameter), very swollen, of rounded size and reddish in color. They don’t have a spontaneous expulsion like blackheads and pimples. That’s why they’re so painful and easily leave noticeable scars.
Regarding nodules, experts clarify the following:
“Cystic nodular acne is characterized by inflammations mainly composed of lymphocytes and giant cells, while pustular lesions are composed of a neutrophilic infiltrate.”
We should note that nodules aren’t the only type of injury that nodular acne can cause. These happen to be the most prominent, when compared to other lesions. In this way, a person with nodular acne may also have persistent blackheads, pustules, and papules.
On the other hand, it’s important to note that nodules don’t only affect the face, neck, and upper part of the trunk. It can spread throughout the chest and back and reach other parts of the body.
In addition to the lesions, it’s common for patients to suffer from seborrhea, an alteration of the sebaceous glands that, as a consequence, causes the skin to present an exaggerated amount of sebum.
Contrary to what people often think, nodular acne and acne conglobata aren’t the same. The second is a variant of the first, along with fulminant acne and facial pyoderma.
Causes
Acne is a skin condition that doesn’t have a single cause, whatever its type. This is confirmed by numerous studies, such as that published in the Venezuelan Archives of Pharmacology and Therapeutics magazine. This report also explains the various factors that influence the appearance of acne:
“Environmental, hormonal [androgen], nutritional, immunological, infectious and genetic components. The latter seems to be especially important, and is present in sporadic cases as well as in familial patterns.”
On the other hand, experts consider that the incidence of nodular acne is higher in men (adolescents and young adults). Having said that, it can also affect adult women, especially those who suffer from polycystic ovary syndrome, according to the hypotheses of recent decades.
Treatment

Unfortunately, over-the-counter treatments and skin cleansers (soaps, gels, scrubs, creams, etc.) aren’t effective against this type of acne.
- The treatment of nodular acne must be intensive. It may include an oral antibiotic, retinoids, benzoyl peroxide, and emollients.
- For women, hormonal treatment may be considered.
- As indicated in scientific literature, isotretinoin is commonly included in the treatment of severe nodulocystic acne, as well as comedonal or papulopustular acne that’s resistant to topical treatments and the newer systemic antibiotics.
Living with nodular acne
Experts don’t recommend that people with nodular acne attempt to touch their lesions at home in any way. Not only can this cause more pain and inflammation, but it can also make the wounds (and later scars) even deeper and harder to treat.
To reduce inflammation or mitigate pain, you can use ice packs (always wrapped in gauze or a clean, fine cloth, to prevent skin burns). And, in more severe cases, the doctor may prescribe cortisone injections, although these tend to be left as a last resort.
As a final recommendation, we can highlight the importance of going to the dermatologist in the event of any aggravation or concern that may arise during the treatment. In this way, not only can the problem be addressed in the most appropriate way, but further damage to the skin can also be prevented.
- Cuellar-Barboza AB, Cárdenas-de la Garza JA, Martínez-Moreno A, Reyna-Rodríguez IL y col. Terapia esteroidea en pacientes con acné. Dermatol Rev Mex. 2018 noviembrediciembre;62(6):506-515.
-
Gómez-Flores, Minerva, and S Chávez-Álvarez. 2019. “Asociaciones Hormonales Del Acné y Tratamiento.” Dermatología, Revista Mexicana 63 (1): 25–32. https://www.medigraphic.com/pdfs/derrevmex/rmd-2019/rmds191d.pdf.
- Gutiérrez Cecilia, Ávila Raquel, Rojas Milagros, Olivar Luis Carlos, Mejías José Carlos, Chávez-Castillo Mervin et al . Acné conglobata: A propósito de un caso. AVFT [Internet]. 2014 Jun [citado 2021 Jun 05] ; 33( 2 ): 51-59. Disponible en: http://ve.scielo.org/scielo.php?script=sci_arttext&pid=S0798-02642014000200001&lng=es.
-
“Investigator’s Global Assessment (IGA) of Acne Severity.” n.d. NPS MedicineWise. Accessed June 5, 2021. https://www.nps.org.au/radar/articles/investigators-global-assessment-iga-of-acne-severity-additional-content-adapalene-with-benzoyl-peroxide-epiduo-for-severe-acne-vulgaris.
-
López-Estebaranz, J.L., P. Herranz-Pinto, and B. Dréno. 2017. “Consenso Español Para Establecer Una Clasificación y Un Algoritmo de Tratamiento Del Acné.” Actas Dermo-Sifiliográficas 108 (2): 120–31. https://doi.org/10.1016/j.ad.2016.10.001.
-
Newman MD, Bowe WP, Heughebaert C, and AR Shalita. 2011. “Consideraciones Terapeuticas Para Acne Nodular Severo – Artículos – IntraMed.” American Journal of Clinical Dermatology 12 (1): 7–14. https://www.intramed.net/contenidover.asp?contenidoid=75066.
-
Vega, J., L. Sánchez-Velicia, and T. Pozo. 2010. “Eficacia de Etanercept En El Tratamiento Del Acné Conglobata.” Actas Dermo-Sifiliograficas 101 (6): 553–54. https://doi.org/10.1016/j.ad.2009.12.026.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







