How to Cope with Psoriasis

Psoriasis is a chronic disease for which there is still no cure. However, many treatments are effective in counteracting flare-ups, reducing symptoms, and improving the quality of life for patients. Knowing how to deal with psoriasis is very important from the beginning, especially if you have one of the more serious variants.
You only learn to accept the disease with time, family support, psychology specialists, and programs that try to address it from different fronts. Today we’ll take a closer look at some things you can do to cope with psoriasis and banish prejudices, insecurities and fears that only negatively affect your health.
Physical care and psoriasis
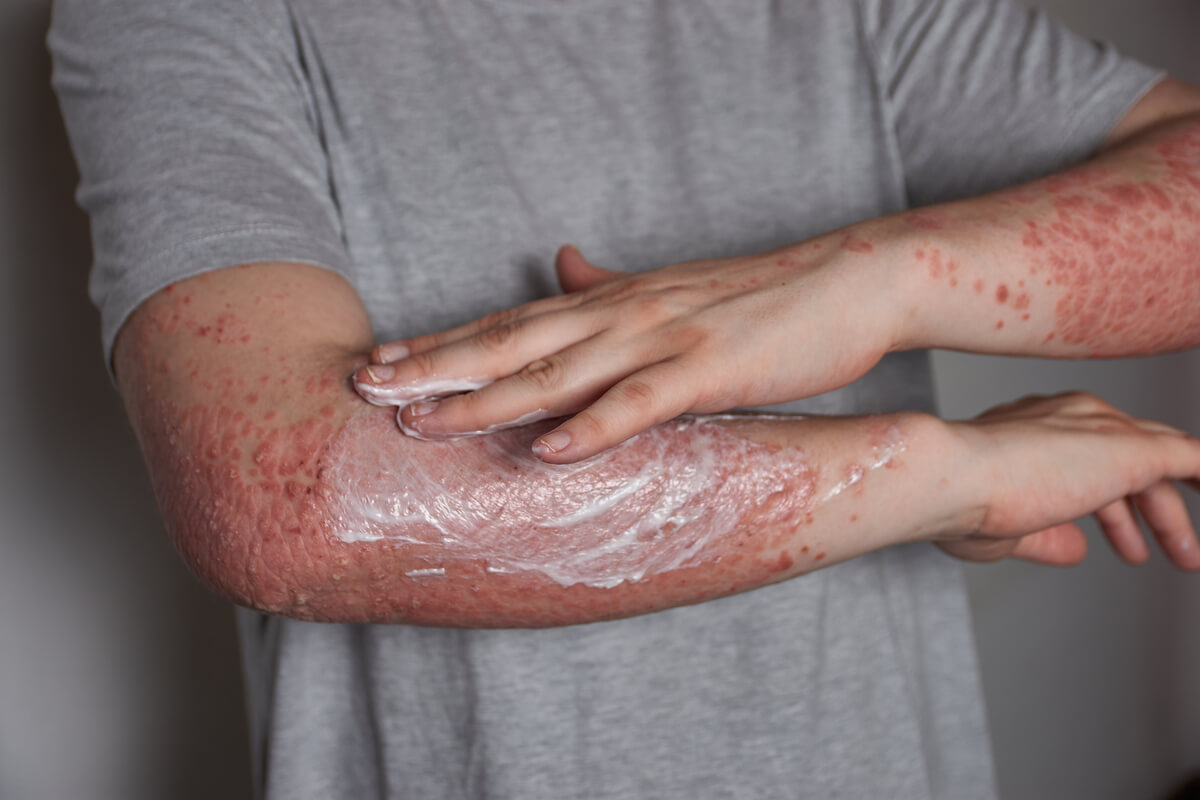
Not all patients live with the disease in the same way. The evidence indicates that the more severe variants, such as pustular, palmoplantar and arthropathic psoriasis, tend to create greater complications in the quality of life. There are many things you can do to cope, including physical care.
It’s very common for people to devote all their effort to topical or systemic treatment, leaving out some basic recommendations to tolerate the disease more effectively. In this way, every patient with psoriasis should take the following into account.
- Avoid exposing the broken areas to the sun or cold. Appropriate clothing should be worn for the occasion.
- Keep skin hydrated to prevent dryness from making breakouts worse.
- Implement a healthy diet. Some cases can get worse with the interaction of food groups.
- Exercise regularly.
- Use insect repellants to avoid bites in the affected areas.
- Avoid scratching the affected areas. This only causes more burning, inflammation, and redness.
- Wear loose clothing that minimizes friction.
Along with this, you should also avoid harmful habits such as drinking alcohol in excess or smoking. Maintaining a healthy weight, using sunscreen, and avoiding shaving the affected areas also go a long way to reducing the onset of symptoms.
Psychological therapy to cope with psoriasis
Today we’ll get to know the importance of a comprehensive methodology in the treatment of psoriasis. We’re talking here about the psychosocial aspect, as there’s evidence that the symptoms, the absence of a cure, and the deterioration of the quality of life in general can all negatively affect a patient’s perception.
Thus arises the need for a multidisciplinary approach that takes into account the psychological health of those affected.
Collateral disorders caused by the disease have been studied. There’s a predisposition to developing low self-esteem, depression, and anxiety. Patients are often afraid of being stigmatized or prejudiced around the disease, which leads them to isolate themselves from their circle to avoid rejection.
Because of all this, it’s very important that, after the diagnosis, psychological therapy is included in the program, especially if the patient is prone to severe outbreaks. Keep in mind that psoriasis is a disease that you must deal with all your life and, although it experiences stages of remission, it will always be latent in the body.
The importance of social support in coping with psoriasis

Family support is known to be of great help in coping with psoriasis. It’s much easier for patients to improve their self-perception with the support of the family group than if they do it alone, and so the closest circle is a good place to start.
It’s also important to take into account how this condition affects the lives of those who accompany the affected person. For example, a study published in the Journal of the American Academy of Dermatology in 2014 suggests that up to 87.8% of cohabitants experience changes in their quality of life after diagnosis.
Experts recommend that patients attend supportive therapy groups of people with the disease. This type of experience can contribute to developing understanding and acceptance; especially when attending with a loved one.
Although you can always benefit from face-to-face sessions, you can also opt for online therapy or through social networks.
Final tips for coping with psoriasis
Although it’s true that treatment options are limited for psoriasis patients, there are still dozens of alternatives that can be tried when an improvement in symptoms can’t be seen. This is something that everyone should know: if one treatment is not effective, it is always possible to opt for another to alleviate the sequelae.
It’s helpful for patients to try to raise awareness among those around them. For example, there’s an erroneous idea that it can be spread by contact. If family, friends and colleagues understand that this is not the case, then a closer social interaction can be strengthened that will then contribute to the strengthening of the psychosocial aspect.
The important thing, in any case, is that people learn to cope with psoriasis over time, in the company of experts and with the support of family and friends. It’s a long and drawn-out process, which will always produce positive repercussions in the management of the disease. The sooner you understand this, the faster you can learn to live with it.
Psoriasis is a chronic disease for which there is still no cure. However, many treatments are effective in counteracting flare-ups, reducing symptoms, and improving the quality of life for patients. Knowing how to deal with psoriasis is very important from the beginning, especially if you have one of the more serious variants.
You only learn to accept the disease with time, family support, psychology specialists, and programs that try to address it from different fronts. Today we’ll take a closer look at some things you can do to cope with psoriasis and banish prejudices, insecurities and fears that only negatively affect your health.
Physical care and psoriasis

Not all patients live with the disease in the same way. The evidence indicates that the more severe variants, such as pustular, palmoplantar and arthropathic psoriasis, tend to create greater complications in the quality of life. There are many things you can do to cope, including physical care.
It’s very common for people to devote all their effort to topical or systemic treatment, leaving out some basic recommendations to tolerate the disease more effectively. In this way, every patient with psoriasis should take the following into account.
- Avoid exposing the broken areas to the sun or cold. Appropriate clothing should be worn for the occasion.
- Keep skin hydrated to prevent dryness from making breakouts worse.
- Implement a healthy diet. Some cases can get worse with the interaction of food groups.
- Exercise regularly.
- Use insect repellants to avoid bites in the affected areas.
- Avoid scratching the affected areas. This only causes more burning, inflammation, and redness.
- Wear loose clothing that minimizes friction.
Along with this, you should also avoid harmful habits such as drinking alcohol in excess or smoking. Maintaining a healthy weight, using sunscreen, and avoiding shaving the affected areas also go a long way to reducing the onset of symptoms.
Psychological therapy to cope with psoriasis
Today we’ll get to know the importance of a comprehensive methodology in the treatment of psoriasis. We’re talking here about the psychosocial aspect, as there’s evidence that the symptoms, the absence of a cure, and the deterioration of the quality of life in general can all negatively affect a patient’s perception.
Thus arises the need for a multidisciplinary approach that takes into account the psychological health of those affected.
Collateral disorders caused by the disease have been studied. There’s a predisposition to developing low self-esteem, depression, and anxiety. Patients are often afraid of being stigmatized or prejudiced around the disease, which leads them to isolate themselves from their circle to avoid rejection.
Because of all this, it’s very important that, after the diagnosis, psychological therapy is included in the program, especially if the patient is prone to severe outbreaks. Keep in mind that psoriasis is a disease that you must deal with all your life and, although it experiences stages of remission, it will always be latent in the body.
The importance of social support in coping with psoriasis

Family support is known to be of great help in coping with psoriasis. It’s much easier for patients to improve their self-perception with the support of the family group than if they do it alone, and so the closest circle is a good place to start.
It’s also important to take into account how this condition affects the lives of those who accompany the affected person. For example, a study published in the Journal of the American Academy of Dermatology in 2014 suggests that up to 87.8% of cohabitants experience changes in their quality of life after diagnosis.
Experts recommend that patients attend supportive therapy groups of people with the disease. This type of experience can contribute to developing understanding and acceptance; especially when attending with a loved one.
Although you can always benefit from face-to-face sessions, you can also opt for online therapy or through social networks.
Final tips for coping with psoriasis
Although it’s true that treatment options are limited for psoriasis patients, there are still dozens of alternatives that can be tried when an improvement in symptoms can’t be seen. This is something that everyone should know: if one treatment is not effective, it is always possible to opt for another to alleviate the sequelae.
It’s helpful for patients to try to raise awareness among those around them. For example, there’s an erroneous idea that it can be spread by contact. If family, friends and colleagues understand that this is not the case, then a closer social interaction can be strengthened that will then contribute to the strengthening of the psychosocial aspect.
The important thing, in any case, is that people learn to cope with psoriasis over time, in the company of experts and with the support of family and friends. It’s a long and drawn-out process, which will always produce positive repercussions in the management of the disease. The sooner you understand this, the faster you can learn to live with it.
- Barrio Lozano, A. D. Trastornos en la calidad de vida y plan de cuidados estandarizado en un paciente con psoriasis. 2019.
- Martínez-García, E., Arias-Santiago, S., Valenzuela-Salas, I., Garrido-Colmenero, C., García-Mellado, V., & Buendía-Eisman, A. Quality of life in persons living with psoriasis patients. Journal of the American Academy of Dermatology. 2014; 71(2): 302-307.
- Meneguin, S., de Godoy, N. A., Pollo, C. F., Miot, H. A., & de Oliveira, C. Quality of life of patients living with psoriasis: a qualitative study. BMC dermatology. 2000; 20(1): 1-6.
- Perrott, S. B., Murray, A. H., Lowe, J., & Mathieson, C. M. The psychosocial impact of psoriasis: physical severity, quality of life, and stigmatization. Physiology & behavior. 2000; 70(5): 567-571.
- Pibernat, M. R. Convivir con la psoriasis. Ed. Médica Panamericana. 2014.
- Rodriguez, L. N. L. Living with psoriasis: Implications for counseling practice (Doctoral dissertation, University of Puerto Rico, Rio Piedras (Puerto Rico). 2008.
- Wolkenstein, P. Living with psoriasis. Journal of the European Academy of Dermatology and Venereology. 2006; 20:28-32.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







