Graves' Disease: Symptoms, Causes and Treatment
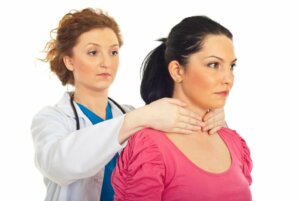
As in other autoimmune disorders, in Graves’ disease, the immune system mistakenly attacks cells in the thyroid gland, causing the thyroid gland to become overactive and producing excessive amounts of hormones. It’s one of the most common causes of hyperthyroidism.
Although there may be exceptions, most patients tend to have high levels of free or total thyroxine (T4) and triiodothyronine (T3), and low levels of TSH.
Symptoms

It’s important to note that Graves’ disease can produce a wide variety of symptoms that are very similar to other forms of hyperthyroidism. The following can be highlighted:
- Dizziness
- Diarrhea
- Insomnia
- Arterial hypertension
- Palpitations
- Irritability
- Heat intolerance
- Agitation and restlessness
- Increased sweating
- Weight loss for no apparent reason
- Persistent tired feeling
- Generalized muscle weakness
- Weakening and hair loss
- Alterations in the menstrual cycle
- Changes in appetite (either an increase or a decrease)
To a lesser extent, it can also cause the following:
- Bulging eyes (Graves’ ophthalmopathy). This usually begins 6 months before or after the diagnosis of Graves’ disease is made.
- Deformities of the fingers and toes (clubbing).
- Reddish and patchy thickening of the skin over the legs (pretibial myxedema).
According to an article published in the Annals of Internal Medicine journal, “Graves’ disease is clinically distinguished from other forms of hyperthyroidism by the presence of diffuse goiter, ophthalmopathy, and, occasionally, pretibial myxedema.”
This means that a dilated thyroid (better known as goiter) is considered one of the most common symptoms, although it isn’t necessarily present in all cases.
Complications
If Graves’ disease isn’t treated, the person may be at higher risk for various complications, such as:
- Osteoporosis
- Thyroid crisis
- Heart disorders (such as heart failure)
- Problems in pregnancy
Causes
As the experts from the American Thyroid Association explain, it appears that this disease has an autoimmune origin: “The antibodies bind to the surface of thyroid cells, stimulating them to produce excess thyroid hormones.” That’s what produces the gland’s overactivity.
They also explain that a high level of stress has often been considered an important risk factor. However, some patients don’t report having been through any particularly recent stressful periods, and neither are they stressed at the time.
In relation to this, according to an article published in the European Journal of Endocrinology, “the role of stress in the pathophysiology of Graves’ disease is suggested by various clinical observations and by recent advances in immunology and a better understanding of the autoimmune diseases”.
However, we still need evidence to confirm the influence of stress on the condition. Other risk factors to consider would be the following:
- Age: Graves’ disease is most common in people under 40 years of age.
- Sex: It has been observed that the disease is usually more common in women.
- Family history: Both Graves’ disease and other autoimmune disorders.
- Pregnancy and family history: These are also risk factors.
- Smoking: Smoking can cause malfunctions in your thyroid.
Diagnosis
To diagnose Graves’ disease, the doctor will question the patient and give them a physical examination. The latter will include an evaluation of the neck area (to detect goiter, nodules, etc.). They’ll also ask for thyroid tests, which may include the following:
- TSH, T3, T4 test, and a thyroid antibody blood test
- Radioactive iodine uptake test
- Computed tomography scan
- Thyroid ultrasound
- MRI scan
- Biopsy
Treatment
Determining the cause is essential in order to treat Graves’ disease successfully. Once doctors have discovered the cause, they can decide on the correct way to combat it, depending on the patient’s condition, age, sex, etc.
We should point out that this isn’t a curative treatment, but, rather, a treatment to regulate the thyroid hormones and reduce the severity of symptoms.
Antithyroid drugs, for example, methimazole (found in pharmacies with the name Tapazol®) or propylthiouracil (found in pharmacies with the name PTU®) are often included. As the MSD Manual explains, “These drugs block thyroid peroxidase, reduce the organization of iodine, and alter the coupling reaction”.
Although doctors often won’t resort to them, in some cases, they may use radioactive iodine or even surgery. The latter is a good option when the patient’s body has rejected any of the previous options and when the goiter has become too large. It’s a procedure that restores normal function and is quite successful.
The person may require other drugs to treat persistent symptoms and to keep the disease under control. This will also require regular medical monitoring.
As in other autoimmune disorders, in Graves’ disease, the immune system mistakenly attacks cells in the thyroid gland, causing the thyroid gland to become overactive and producing excessive amounts of hormones. It’s one of the most common causes of hyperthyroidism.
Although there may be exceptions, most patients tend to have high levels of free or total thyroxine (T4) and triiodothyronine (T3), and low levels of TSH.
Symptoms

It’s important to note that Graves’ disease can produce a wide variety of symptoms that are very similar to other forms of hyperthyroidism. The following can be highlighted:
- Dizziness
- Diarrhea
- Insomnia
- Arterial hypertension
- Palpitations
- Irritability
- Heat intolerance
- Agitation and restlessness
- Increased sweating
- Weight loss for no apparent reason
- Persistent tired feeling
- Generalized muscle weakness
- Weakening and hair loss
- Alterations in the menstrual cycle
- Changes in appetite (either an increase or a decrease)
To a lesser extent, it can also cause the following:
- Bulging eyes (Graves’ ophthalmopathy). This usually begins 6 months before or after the diagnosis of Graves’ disease is made.
- Deformities of the fingers and toes (clubbing).
- Reddish and patchy thickening of the skin over the legs (pretibial myxedema).
According to an article published in the Annals of Internal Medicine journal, “Graves’ disease is clinically distinguished from other forms of hyperthyroidism by the presence of diffuse goiter, ophthalmopathy, and, occasionally, pretibial myxedema.”
This means that a dilated thyroid (better known as goiter) is considered one of the most common symptoms, although it isn’t necessarily present in all cases.
Complications
If Graves’ disease isn’t treated, the person may be at higher risk for various complications, such as:
- Osteoporosis
- Thyroid crisis
- Heart disorders (such as heart failure)
- Problems in pregnancy
Causes
As the experts from the American Thyroid Association explain, it appears that this disease has an autoimmune origin: “The antibodies bind to the surface of thyroid cells, stimulating them to produce excess thyroid hormones.” That’s what produces the gland’s overactivity.
They also explain that a high level of stress has often been considered an important risk factor. However, some patients don’t report having been through any particularly recent stressful periods, and neither are they stressed at the time.
In relation to this, according to an article published in the European Journal of Endocrinology, “the role of stress in the pathophysiology of Graves’ disease is suggested by various clinical observations and by recent advances in immunology and a better understanding of the autoimmune diseases”.
However, we still need evidence to confirm the influence of stress on the condition. Other risk factors to consider would be the following:
- Age: Graves’ disease is most common in people under 40 years of age.
- Sex: It has been observed that the disease is usually more common in women.
- Family history: Both Graves’ disease and other autoimmune disorders.
- Pregnancy and family history: These are also risk factors.
- Smoking: Smoking can cause malfunctions in your thyroid.
Diagnosis

To diagnose Graves’ disease, the doctor will question the patient and give them a physical examination. The latter will include an evaluation of the neck area (to detect goiter, nodules, etc.). They’ll also ask for thyroid tests, which may include the following:
- TSH, T3, T4 test, and a thyroid antibody blood test
- Radioactive iodine uptake test
- Computed tomography scan
- Thyroid ultrasound
- MRI scan
- Biopsy
Treatment
Determining the cause is essential in order to treat Graves’ disease successfully. Once doctors have discovered the cause, they can decide on the correct way to combat it, depending on the patient’s condition, age, sex, etc.
We should point out that this isn’t a curative treatment, but, rather, a treatment to regulate the thyroid hormones and reduce the severity of symptoms.
Antithyroid drugs, for example, methimazole (found in pharmacies with the name Tapazol®) or propylthiouracil (found in pharmacies with the name PTU®) are often included. As the MSD Manual explains, “These drugs block thyroid peroxidase, reduce the organization of iodine, and alter the coupling reaction”.
Although doctors often won’t resort to them, in some cases, they may use radioactive iodine or even surgery. The latter is a good option when the patient’s body has rejected any of the previous options and when the goiter has become too large. It’s a procedure that restores normal function and is quite successful.
The person may require other drugs to treat persistent symptoms and to keep the disease under control. This will also require regular medical monitoring.
-
Diaz Deysy, Cieza, Centeno Clemente Carmen, and Pinto Valdivia Miguel. 2008. “Características Clínicas, Perfil Hormonal y Marcadores de Autoinmunidad de Pacientes Con Enfermedad de Graves.” Rev Med Hered 19 (4): 157. http://www.scielo.org.pe/pdf/rmh/v19n4/v19n4ao3.pdf.
- Falgarone, Géraldine, Hassan M Heshmati, Régis Cohen, and Gérard Reach. ” MECHANISMS IN ENDOCRINOLOGY: Role of emotional stress in the pathophysiology of Graves’ disease”. European Journal of Endocrinology 168.1 (2013): R13-R18. < https://doi.org/10.1530/EJE-12-0539>. Web. 16 Jun. 2021.
-
Hershman, Jerome M. n.d. “Hipertiroidismo – Trastornos Endocrinológicos y Metabólicos.” Manual MSD Versión Para Profesionales. Accessed June 16, 2021. https://www.msdmanuals.com/es/professional/trastornos-endocrinológicos-y-metabólicos/trastornos-tiroideos/hipertiroidismo.
- Young P., Finn B. C., Bruetman J. E.. La enfermedad de Graves, signos y síntomas. An. Med. Interna (Madrid) [Internet]. 2007 Oct [citado 2021 Jun 16] ; 24( 10 ): 505-508. Disponible en: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0212-71992007001000010&lng=es.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







