Gingivitis: Symptoms, Causes and Treatment
The oral cavity is made up of the teeth and all the tissues that support them, also known as the periodontium. One of the main supporting tissues are the gums, which is why they can be affected by many different pathologies. Among the diseases that affect these tissues, inflammation of the gums or gingivitis stands out.
This is one of the most frequent gingival diseases worldwide, with a prevalence of between 20 and 50% depending on the population studied. This pathology can be accompanied by an infection of the tissue and can affect other deeper structures, thus being the first stage of periodontal disease.
There are many different degrees of this disease, although, in general terms, it begins with a slight bleeding from the gums when brushing. In the most severe cases, inflammation can affect the periodontal ligaments and bone tissue, causing their destruction, so timely treatment is essential.
Causes of gingivitis

One of the main causes of this disease is the chronic effect of dental plaque resulting from poor or inadequate oral hygiene. The mouth contains a large number of bacteria, which combine with mucus and food debris to form a substance called plaque, which will coat the tooth.
Dental plaque must be removed every day with proper brushing, otherwise conditions such as cavities or halitosis will appear. When plaque isn’t removed, it tends to accumulate at the base of the tooth, harden, and form a hard deposit called tartar.
This plaque and tartar cause inflammation of the gums and, consequently, gingivitis. Both factors, together with inadequate hygiene, favor the accumulation of germs in the tissue. All of these microorganisms produce toxins, which greatly worsens the disease.
Risk factor’s
Despite the high frequency of the disease, multiple investigations have managed to determine some risk factors that favor its application.
These factors are related to the weakness of the immune system and anatomical alterations of the mouth, among which the following stand out:
- Pregnancy
- Old age
- Misaligned teeth that irritate the gums
- Stress
- Some medications such as phenytoin or heavy metals
- Poorly fitting dentures
- Uncontrolled diabetes mellitus
Gingivitis symptoms
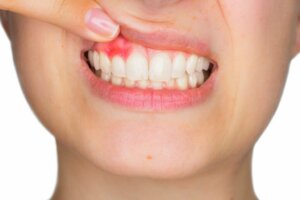
The symptoms of gingivitis are very subtle and can be difficult to notice with the naked eye as they’re not particularly bothersome. In this sense, it’s important to be familiar with the normal appearance of the gums in order to be able to identify the pathology. Normal gums are a pale pink tissue, moist, not painful on palpation, and firmly attached to the teeth.
One of the main symptoms of this disease is gingivorrhagia or bleeding gums, especially after brushing. The expelled blood is usually scarce and bright red. It’s often seen in the foam produced by toothpaste in small droplets or with a pink tint.
On the other hand, the gums may show changes in their appearance as a result of inflammation and the action of bacteria. In this sense, it’s possible to notice any of the following symptoms:
- Enlarged gums
- Reddish color in the oral mucosa, similar to irritated tissue
- Bad breath
- Receding gums
- Pain or discomfort when touching the gums
- Bright appearance of the gums
- Mouth ulcers in the most severe cases
Diagnosis
The diagnosis of this gingival pathology is very simple and is based on a quick examination by the dentist. He will inspect the patient’s mouth to verify the condition of the gums and verify the existence of the disease.
The dentist may touch the gums with his fingers and stimulate them to check for tenderness and bleeding. They may also ask you pertinent questions in order to identify the existence of any of the risk factors described above.
For their part, dentists usually measure the depth of the space between the gum and the tooth to check the risk of suffering from gingivitis, this space must be less than 3 millimeters.
A dental X-ray is necessary, especially in the most severe cases. This is done in order to determine if there’s a decrease in bone mass, which would indicate the presence of periodontitis, one of the most frequent complications of the disease.
Gingivitis treatment
The treatment of gingivitis is aimed at reducing inflammation and eliminating the infection from the tissue. On the other hand, it’s necessary to eliminate the direct cause of the disease, so the dental implant must be removed and adjusted when the irritation is the result of a defect in it.
Gingivitis is reversible as long as both plaque and tartar are removed from the teeth. In this sense, the dentist must use various instruments to remove solid deposits and perform a proper clean.
Some specialists recommend the use of antiseptic rinses the days before cleaning to reduce inflammation.
Once the tartar and plaque are removed, the gum inflammation usually goes away on its own within a few days. Gingivitis is a disease that tends to recur, so good oral hygiene and continuous dental check-ups are essential.
How to prevent its appearance?
The best method to prevent the appearance of any dental or gum disease is proper oral hygiene and proper tooth care. Plaque removal is very important, which is why many dentists recommend brushing at least two times a day with a suitable brush.
Some research claims that electric brushes are better at removing plaque and calculus, however, a good brushing technique is also essential. In this sense, it’s necessary to try to cover all the teeth with the bristles of the brush, without forgetting the attached structures such as the tongue.
Proper tooth brushing should be accompanied by flossing at least once a day, as it’s the most effective way to remove plaque lodged between the teeth. The use of mouthwash is also highly recommended, since it helps to eliminate germs found in the mouth and, in turn, to improve breath.
Timely treatment is essential
Gingivitis is a periodontal disease characterized by bleeding and inflammation of the gums. It’s caused by multiple factors, although it’s closely related to inadequate oral hygiene. In this sense, the best way to prevent and treat it is through the removal of tartar and proper tooth brushing.
Although it may not seem so serious, gingivitis can progress and turn into periodontitis, which is a disease that can lead to the destruction of bone tissue in the mouth. Early diagnosis and care are of great importance, which is why a specialist should be consulted in the event of any suspicious symptoms.
The oral cavity is made up of the teeth and all the tissues that support them, also known as the periodontium. One of the main supporting tissues are the gums, which is why they can be affected by many different pathologies. Among the diseases that affect these tissues, inflammation of the gums or gingivitis stands out.
This is one of the most frequent gingival diseases worldwide, with a prevalence of between 20 and 50% depending on the population studied. This pathology can be accompanied by an infection of the tissue and can affect other deeper structures, thus being the first stage of periodontal disease.
There are many different degrees of this disease, although, in general terms, it begins with a slight bleeding from the gums when brushing. In the most severe cases, inflammation can affect the periodontal ligaments and bone tissue, causing their destruction, so timely treatment is essential.
Causes of gingivitis

One of the main causes of this disease is the chronic effect of dental plaque resulting from poor or inadequate oral hygiene. The mouth contains a large number of bacteria, which combine with mucus and food debris to form a substance called plaque, which will coat the tooth.
Dental plaque must be removed every day with proper brushing, otherwise conditions such as cavities or halitosis will appear. When plaque isn’t removed, it tends to accumulate at the base of the tooth, harden, and form a hard deposit called tartar.
This plaque and tartar cause inflammation of the gums and, consequently, gingivitis. Both factors, together with inadequate hygiene, favor the accumulation of germs in the tissue. All of these microorganisms produce toxins, which greatly worsens the disease.
Risk factor’s
Despite the high frequency of the disease, multiple investigations have managed to determine some risk factors that favor its application.
These factors are related to the weakness of the immune system and anatomical alterations of the mouth, among which the following stand out:
- Pregnancy
- Old age
- Misaligned teeth that irritate the gums
- Stress
- Some medications such as phenytoin or heavy metals
- Poorly fitting dentures
- Uncontrolled diabetes mellitus
Gingivitis symptoms
The symptoms of gingivitis are very subtle and can be difficult to notice with the naked eye as they’re not particularly bothersome. In this sense, it’s important to be familiar with the normal appearance of the gums in order to be able to identify the pathology. Normal gums are a pale pink tissue, moist, not painful on palpation, and firmly attached to the teeth.
One of the main symptoms of this disease is gingivorrhagia or bleeding gums, especially after brushing. The expelled blood is usually scarce and bright red. It’s often seen in the foam produced by toothpaste in small droplets or with a pink tint.
On the other hand, the gums may show changes in their appearance as a result of inflammation and the action of bacteria. In this sense, it’s possible to notice any of the following symptoms:
- Enlarged gums
- Reddish color in the oral mucosa, similar to irritated tissue
- Bad breath
- Receding gums
- Pain or discomfort when touching the gums
- Bright appearance of the gums
- Mouth ulcers in the most severe cases
Diagnosis
The diagnosis of this gingival pathology is very simple and is based on a quick examination by the dentist. He will inspect the patient’s mouth to verify the condition of the gums and verify the existence of the disease.
The dentist may touch the gums with his fingers and stimulate them to check for tenderness and bleeding. They may also ask you pertinent questions in order to identify the existence of any of the risk factors described above.
For their part, dentists usually measure the depth of the space between the gum and the tooth to check the risk of suffering from gingivitis, this space must be less than 3 millimeters.
A dental X-ray is necessary, especially in the most severe cases. This is done in order to determine if there’s a decrease in bone mass, which would indicate the presence of periodontitis, one of the most frequent complications of the disease.
Gingivitis treatment

The treatment of gingivitis is aimed at reducing inflammation and eliminating the infection from the tissue. On the other hand, it’s necessary to eliminate the direct cause of the disease, so the dental implant must be removed and adjusted when the irritation is the result of a defect in it.
Gingivitis is reversible as long as both plaque and tartar are removed from the teeth. In this sense, the dentist must use various instruments to remove solid deposits and perform a proper clean.
Some specialists recommend the use of antiseptic rinses the days before cleaning to reduce inflammation.
Once the tartar and plaque are removed, the gum inflammation usually goes away on its own within a few days. Gingivitis is a disease that tends to recur, so good oral hygiene and continuous dental check-ups are essential.
How to prevent its appearance?
The best method to prevent the appearance of any dental or gum disease is proper oral hygiene and proper tooth care. Plaque removal is very important, which is why many dentists recommend brushing at least two times a day with a suitable brush.
Some research claims that electric brushes are better at removing plaque and calculus, however, a good brushing technique is also essential. In this sense, it’s necessary to try to cover all the teeth with the bristles of the brush, without forgetting the attached structures such as the tongue.
Proper tooth brushing should be accompanied by flossing at least once a day, as it’s the most effective way to remove plaque lodged between the teeth. The use of mouthwash is also highly recommended, since it helps to eliminate germs found in the mouth and, in turn, to improve breath.
Timely treatment is essential
Gingivitis is a periodontal disease characterized by bleeding and inflammation of the gums. It’s caused by multiple factors, although it’s closely related to inadequate oral hygiene. In this sense, the best way to prevent and treat it is through the removal of tartar and proper tooth brushing.
Although it may not seem so serious, gingivitis can progress and turn into periodontitis, which is a disease that can lead to the destruction of bone tissue in the mouth. Early diagnosis and care are of great importance, which is why a specialist should be consulted in the event of any suspicious symptoms.
- Matesanz-Pérez P, Matos-Cruz R, Bascones-Martínez A. Enfermedades gingivales: una revisión de la literatura. Av Periodon Implantol. 2008; 20(1): 11-25.
- Azcona Barbed L. Gingivitis. Farmacia Profesional. 2010; 24(2): 66-68.
- Tur Feijón E. Gingivitis: características y prevención. Enfermería Dermatológica. 2011; (12): 13-17.
- Trombelli L, Farina R, Silva CO, Tatakis DN. Plaque-induced gingivitis: Case definition and diagnostic considerations. J Periodontol. 2018;89 Suppl 1:S46-S73.
- Dufty J, Gkranias N, Donos N. Necrotising Ulcerative Gingivitis: A Literature Review. Oral Health Prev Dent. 2017;15(4):321-327.
- He T, Qu L, Chang J, Wang J. Gingivitis Models – Relevant Approaches to Assess Oral Hygiene Products. J Clin Dent. 2018;29(2):45-51.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







