What Is Pseudotumor Cerebri?
An increase in intracranial pressure without an apparent trigger is known as pseudotumor cerebri. It is also known as idiopathic intracranial hypertension, which is a more appropriate term when we see the symptoms it can produce in the body.
The most serious problems are eye problems, which can even lead to blindness if not treated properly.
Despite its generic name, and although all the symptoms seem to point to it, the development of the condition doesn’t imply the presence of a tumor. In this case, the cerebrospinal fluid can’t circulate as it should due to the increasing hypertension. According to some indications, its incidence rate is 1-5 cases per 100,000 inhabitants.
Symptoms of pseudotumor cerebri

Evidence suggests that 48% of patients with pseudotumor cerebri are asymptomatic. This value is worryingly high, as this means that nearly half of those who suffer from it won’t know they have it until the condition progresses to a more serious level. Experts have identified four ways it can manifest. They are as follows:
- With isolated symptoms of intracranial hypertension: Here, headaches (with up to 75% incidence), nausea, vomiting, double vision or diplopia and others stand out.
- With isolated symptoms in the ocular area: This may be decreased visual acuity, blurred vision, eye fatigue, visual darkening and others. This may lead the patient to believe that it’s a benign condition.
- With the coexistence of intracranial and ocular symptoms: This generally occurs when intracranial hypertension is very high or hasn’t been treated properly.
- With isolated papilledema: This is less common than the others, and the condition can also manifest itself solely through a papilledema. This is usually found in a routine eye exam.
Symptoms can be made worse by making sudden movements and by changes in position such as getting up or sitting down. In rare cases, symptoms such as cognitive impairment, facial paralysis, lack of coordination (in walking, for example), pain in the lumbar area, and brachial plexopathy may occur. Ringing in the ears (tinnitus) may also occur.
Causes of pseudotumor cerebri
The causes of pseudotumor cerebri haven’t yet been determined. Studies in this regard suggest dividing the condition into two groups: idiopathic or primary pseudotumor cerebri (the cause of which is unknown) and secondary pseudotumor cerebri (which develops due to an underlying condition in the body). The following have been identified as possible causes:
Use of some medications
The controlled or uncontrolled intake of some groups of drugs has led to intracranial pressure. For example, research and studies have suggested the relationship between growth hormone treatment and this condition. Hormone therapy has even been shown to develop after several years.
There also appears to be a relationship, supported by evidence, between tetracycline and pseudotumor cerebri. On the other hand, there’s evidence that it can be induced by minocillin and isotretinoin, the latter being one of the most effective acne treatments.
Depending on the recurrence of the treatment, the dosage, and the age of the patient, experts suggest that there should be regular eye check-ups to try to prevent this derived complication.
Various health problems
Although the association is rare, there’s also enough evidence to link this condition with the development of certain health problems. This can be triggered both with treatment and without it. There are investigations and studies that show that pseudotumor cerebri can be responsible for patients developing anemia.
Its incidence in lupus patients has also been reported. Evidence indicates that sleep disorders can trigger episodes of this type, especially in conditions like sleep apnea. Other conditions that have been linked with it include blood clotting disorders, underactive parathyroid glands, polycystic ovary syndrome, and kidney disease.
Obesity
The most direct relationship that has been established between the condition and other conditions is obesity. To be more precise, obesity in conjunction with women of childbearing age.
The evidence indicates that a considerable percentage of cases occur in this part of the population. The reason isn’t yet clear, although it’s believed that the combination of active adipose tissue and female hormones may be the cause.
As a complement to these triggers, and despite the absence of relevant research during the last decade, it has also been found that excessive intake of vitamin A can cause increased intracranial pressure.
Diagnosis and treatment of pseudotumor cerebri
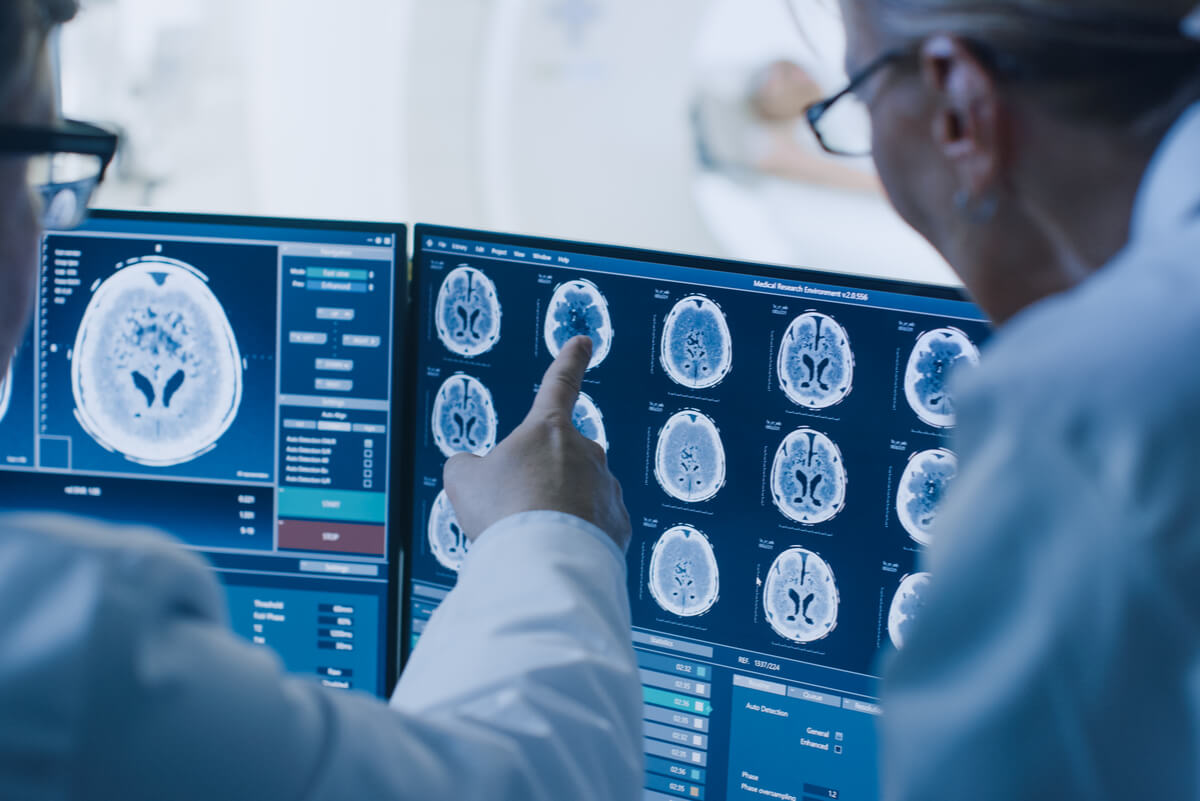
There are many ways to diagnose pseudotumor cerebri. A neurologist or ophthalmologist usually carries it out. They’ll perform several tests on the patient, such as a test of visual acuity, visual field, color, and eye muscles, among others.
Advances in understanding the disease and in technology have meant that it can also be diagnosed through imaging tests. Using these tests, experts have found delimited changes in the flattening of the eyeball, enhancement of the optic nerve head and an increase in tortuosity and empty sella turcica, among other things.
For this reason, the specialist can also perform an MRI venography and CT scans. As a complement, blood tests and even a lumbar puncture can be performed; in part to rule out any other conditions. The doctor must follow a diagnostic protocol as the symptoms are very general.
As soon as the presence of pseudotumor cerebri has been confirmed, treatment will begin. This varies depending on the severity of the condition, the collateral effects it has generated and the possible causes that have generated it. Evidence indicates that conservative treatment often works, including weight loss and improved diet.
If there’s a mild loss in vision, or at least a high probability of it, the doctor may prescribe acetazolamide, furosemide, or corticosteroids. If the loss is severe, or there’s a risk of progression, surgical interventions are sometimes necessary. This, fortunately, only happens in very few cases. Don’t hesitate to seek medical assistance if you have any of the symptoms.
An increase in intracranial pressure without an apparent trigger is known as pseudotumor cerebri. It is also known as idiopathic intracranial hypertension, which is a more appropriate term when we see the symptoms it can produce in the body.
The most serious problems are eye problems, which can even lead to blindness if not treated properly.
Despite its generic name, and although all the symptoms seem to point to it, the development of the condition doesn’t imply the presence of a tumor. In this case, the cerebrospinal fluid can’t circulate as it should due to the increasing hypertension. According to some indications, its incidence rate is 1-5 cases per 100,000 inhabitants.
Symptoms of pseudotumor cerebri

Evidence suggests that 48% of patients with pseudotumor cerebri are asymptomatic. This value is worryingly high, as this means that nearly half of those who suffer from it won’t know they have it until the condition progresses to a more serious level. Experts have identified four ways it can manifest. They are as follows:
- With isolated symptoms of intracranial hypertension: Here, headaches (with up to 75% incidence), nausea, vomiting, double vision or diplopia and others stand out.
- With isolated symptoms in the ocular area: This may be decreased visual acuity, blurred vision, eye fatigue, visual darkening and others. This may lead the patient to believe that it’s a benign condition.
- With the coexistence of intracranial and ocular symptoms: This generally occurs when intracranial hypertension is very high or hasn’t been treated properly.
- With isolated papilledema: This is less common than the others, and the condition can also manifest itself solely through a papilledema. This is usually found in a routine eye exam.
Symptoms can be made worse by making sudden movements and by changes in position such as getting up or sitting down. In rare cases, symptoms such as cognitive impairment, facial paralysis, lack of coordination (in walking, for example), pain in the lumbar area, and brachial plexopathy may occur. Ringing in the ears (tinnitus) may also occur.
Causes of pseudotumor cerebri
The causes of pseudotumor cerebri haven’t yet been determined. Studies in this regard suggest dividing the condition into two groups: idiopathic or primary pseudotumor cerebri (the cause of which is unknown) and secondary pseudotumor cerebri (which develops due to an underlying condition in the body). The following have been identified as possible causes:
Use of some medications
The controlled or uncontrolled intake of some groups of drugs has led to intracranial pressure. For example, research and studies have suggested the relationship between growth hormone treatment and this condition. Hormone therapy has even been shown to develop after several years.
There also appears to be a relationship, supported by evidence, between tetracycline and pseudotumor cerebri. On the other hand, there’s evidence that it can be induced by minocillin and isotretinoin, the latter being one of the most effective acne treatments.
Depending on the recurrence of the treatment, the dosage, and the age of the patient, experts suggest that there should be regular eye check-ups to try to prevent this derived complication.
Various health problems
Although the association is rare, there’s also enough evidence to link this condition with the development of certain health problems. This can be triggered both with treatment and without it. There are investigations and studies that show that pseudotumor cerebri can be responsible for patients developing anemia.
Its incidence in lupus patients has also been reported. Evidence indicates that sleep disorders can trigger episodes of this type, especially in conditions like sleep apnea. Other conditions that have been linked with it include blood clotting disorders, underactive parathyroid glands, polycystic ovary syndrome, and kidney disease.
Obesity
The most direct relationship that has been established between the condition and other conditions is obesity. To be more precise, obesity in conjunction with women of childbearing age.
The evidence indicates that a considerable percentage of cases occur in this part of the population. The reason isn’t yet clear, although it’s believed that the combination of active adipose tissue and female hormones may be the cause.
As a complement to these triggers, and despite the absence of relevant research during the last decade, it has also been found that excessive intake of vitamin A can cause increased intracranial pressure.
Diagnosis and treatment of pseudotumor cerebri

There are many ways to diagnose pseudotumor cerebri. A neurologist or ophthalmologist usually carries it out. They’ll perform several tests on the patient, such as a test of visual acuity, visual field, color, and eye muscles, among others.
Advances in understanding the disease and in technology have meant that it can also be diagnosed through imaging tests. Using these tests, experts have found delimited changes in the flattening of the eyeball, enhancement of the optic nerve head and an increase in tortuosity and empty sella turcica, among other things.
For this reason, the specialist can also perform an MRI venography and CT scans. As a complement, blood tests and even a lumbar puncture can be performed; in part to rule out any other conditions. The doctor must follow a diagnostic protocol as the symptoms are very general.
As soon as the presence of pseudotumor cerebri has been confirmed, treatment will begin. This varies depending on the severity of the condition, the collateral effects it has generated and the possible causes that have generated it. Evidence indicates that conservative treatment often works, including weight loss and improved diet.
If there’s a mild loss in vision, or at least a high probability of it, the doctor may prescribe acetazolamide, furosemide, or corticosteroids. If the loss is severe, or there’s a risk of progression, surgical interventions are sometimes necessary. This, fortunately, only happens in very few cases. Don’t hesitate to seek medical assistance if you have any of the symptoms.
- Asensio-Sanchez, V. M., Merino-Angulo, J., Martínez-Calvo, S., Calvo, M. J., & Rodríguez, R. Epidemiología del pseudotumor cerebral. Archivos de la Sociedad Española de Oftalmología. 2007; 82(4): 219-221.
- Degnan, A. J., & Levy, L. M. Pseudotumor cerebri: brief review of clinical syndrome and imaging findings. American journal of neuroradiology. 2011; 32(11): 1986-1993.
- Friedman, D. I. (2004). Pseudotumor cerebri. Neurologic clinics. 2004; 22(1): 99-131.
- Friedman, D. I., Liu, G. T., & Digre, K. B. Revised diagnostic criteria for the pseudotumor cerebri syndrome in adults and children. Neurology. 2013; 81(13): 1159-1165.
- González Gili, L. O., Buffone, I. R., Carrara, L. E., Coto, M. B., Fortunatti, E. A., Dejtera, M., … & Romano, M. (2016). Pseudotumor cerebral secundario al consumo de minociclina en un paciente pediátrico. Archivos argentinos de pediatría. 2016; 114(2): 2-3.
- Jeng, M. R., Rieman, M., Bhakta, M., Helton, K., & Wang, W. C. (2002). Pseudotumor cerebri in two adolescents with acquired aplastic anemia. Journal of pediatric hematology/oncology. 2002; 24(9): 765-768.
- Kesler, A., Goldhammer, Y., Hadayer, A., & Pianka, P. (2004). The outcome of pseudotumor cerebri induced by tetracycline therapy. Acta neurologica scandinavica. 2004; 110(6): 408-411.
- Malozowski, S., Tanner, L. A., Wysowski, D. K., Fleming, G. A., & Stadel, B. V. Benign intracranial hypertension in children with growth hormone deficiency treated with growth hormone. The Journal of pediatrics. 1995; 126(6): 996-999.
- Marcus, D. M., Lynn, J., Miller, J. J., Chaudhary, O., Thomas, D., & Chaudhary, B. Sleep disorders: a risk factor for pseudotumor cerebri?. Journal of neuro-ophthalmology. 2001; 21(2): 121-123.
- Morrice, G., Havener, W. H., & Kapetansky, F. Vitamin A intoxication as a cause of pseudotumor cerebri. Jama. 1960; 173(16): 1802-1805.
- McGeeney, B. E., & Friedman, D. Pseudotumor cerebri pathophysiology. Headache: The Journal of Head and Face Pain. 2014; 54(3): 445-458.
- Nazir, S. A., & Siatkowski, R. M. Pseudotumor cerebri in idiopathic aplastic anemia. Journal of AAPOS: the official publication of the American Association for Pediatric Ophthalmology and Strabismus. 2003; 7(1): 71-74.
- Rodríguez Pupo, J. M., Díaz Rojas, Y. V., Rojas Rodríguez, Y., Núñez Arias, E., & García Gómez, A. Hipertensión intracraneal idiopática: principales aspectos neurofisiológicos, diagnósticos y terapéuticos. Correo Científico Médico. 2015; 19(2): 282-299.
- Ramos, L. O., Mattos, P. C., Akel, P. B. de M., Peixoto, I. L., & Blos, F. L. Pseudotumor Cerebri Associated With The Use Of Isotretinoin. Journal of the Portuguese Society of Dermatology and Venereology. 2014; 72(3): 407-409.
- Rogers, A. H., Rogers, G. L., Bremer, D. L., & McGregor, M. L. Pseudotumor cerebri in children receiving recombinant human growth hormone. Ophthalmology. 1999; 106(6): 1186-1190.
- Thurtell, M. J., & Wall, M. Idiopathic intracranial hypertension (pseudotumor cerebri): recognition, treatment, and ongoing management. Current treatment options in neurology. 2013; 15(1): 1-12.
- Vischi, A., Guerriero, S., Giancipoli, G., Lorusso, V., & Sborgia, G. Delayed onset of pseudotumor cerebri syndrome 7 years after starting human recombinant growth hormone treatment. 2006: 178-180.
- Yoo, W. H., Park, J. H., Kim, H. K., Park, T. S., & Baek, H. S. Recurrent pseudotumor cerebri in systemic lupus erythematosus: a case report. Journal of Korean medical science. 2001; 16(6): 805.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







