All About the Diagnosis of Psoriasis
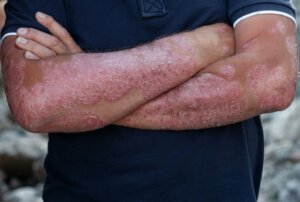
Psoriasis is an autoimmune disease that manifests itself through breakouts on the surface of the skin. It’s considered a chronic disorder that can go through periods of remission over the years. Only a professional can make a diagnosis of psoriasis, as it can be confused with other skin or infectious diseases.
Despite advances in research surrounding this condition, there’s no unified diagnosis for psoriasis. Due to this, the specialist has to resort to the recognition of a series of patterns, the review of the patient’s clinical history, and the consideration of the risk groups for the disease.
Although the symptoms of psoriasis may be very obvious to the naked eye, it’s actually a very difficult disorder for non-specialists to diagnose. For this reason, you should always go to an expert if you suspect that you’re suffering from it, and avoid premature self-medication at all costs.
Diagnosis of psoriasis by physical examination

Unlike other autoimmune disorders, psoriasis can’t be diagnosed through 100 percent effective blood tests or imaging studies. Its diagnosis varies depending on the type or variant of the disease, among which vulgaris, nail, guttate and pustular psoriasis stand out as the most frequent.
The method most used by dermatologists to diagnose psoriasis is through a physical exam. It’s very common for the specialist to use a dermatoscope, an instrument that has proven to be very useful for this task. Considering that between 80% and 90% of the disease occurs through the vulgaris variant, the following will need to be present:
- Plates delimited with silver scales.
- Red or pearly-colored skin surface.
- Inflammation and burning in the affected area.
- Desquamation in peripheral or central areas.
- Excoriation in the epidermis.
The dermatologist will carefully review these symptoms in the area indicated by the patient as well as in others such as the scalp, the folds, behind the ears and in the joints and extremities. They will also assess the thickness, color, and growth of the nails, a clear symptom of nail psoriasis.
Along with this physical examination, they will consider the patient’s family history. Psoriasis is known to have a high genetic predisposition, and so a history of the disease in parents or grandparents can help confirm it. A review of the patient’s medical history for skin lesions, infections, or immune disorders can also be used to support the diagnosis.
Finally, the specialist doctor will consider the risk factors for psoriasis and its comorbidities. For example, physical inactivity, heavy smoking, alcoholism, obesity, and suffering from heart conditions, diabetes, or metabolic syndrome increase the chances of developing it.
Diagnosis of psoriasis by laboratory tests
In most cases, the diagnosis of psoriasis is carried out through a physical evaluation, but, in certain contexts, it’s necessary to perform a biopsy of the skin surface. This procedure is rare and is used only when there are doubts about a possible differential diagnosis.
Evidence indicates that it is very useful in some variants, such as nail psoriasis. This can be easily mistaken for fungal infections, even by qualified professionals. In this way, a biopsy is a support tool to make a more accurate psoriasis diagnosis.
It’s performed through a minimally invasive puncture that removes a tissue sample which is then evaluated under a special microscope. While waiting for the results, the doctor may prescribe a preventive treatment to deal with the disease for the time being.
PASI classification in psoriasis
When making the diagnosis of psoriasis, the specialist will proceed to classify the disease according to its severity.
There are many rating scales. The three most used are the National Psoriasis Foundation Psoriasis Score (NPF-PS), the Physician’s Global Assessment (PGA) and the Psoriasis Area Severity Index (PASI). The latter is by far the most used for its practicality.
This scale divides the body into four sections: trunk, upper limbs, lower limbs and head, and the following values are taken into account:
- Percentage of affected skin: From 0% to 100% in degrees ranging from 1 to 6.
- Desquamation: On a scale from 0 to 4.
- Itching: On a scale from 0 to 4.
- Erythema: On a scale from 0 to 4.
- Induration: Determined on a scale of 0 to 4.
Finally, all the values are combined and extrapolated on a scale ranging from 0 (absence of disease) to 72 (maximum disease). The tests are usually repeated from time to time to evaluate the improvement of the condition and possible changes in treatment in case the current treatment isn’t working.
Differential diagnosis of psoriasis

One of the reasons why self-diagnosis of patients isn’t recommended is the possible differential causes of breakouts on the skin. There are at least a dozen diseases with symptoms that are very similar to those of psoriasis, and so the mediation of a specialist is irreplaceable.
The most common differential diagnoses of psoriasis are as follows:
- Saborrheic dermatitis: Very common differential diagnosis in psoriasis vulgaris, especially when the outbreaks are located on the scalp and its surroundings.
- Lichen simplex chronicus – Usually develops on the groin, extremities, neck, and genitals.
- Ringworm of the body: Very common in uncovered areas, it’s characterized by microvesicles on the edges. Diagnosed by culture and KOH (potassium hydroxide).
- Onychomycosis: Nail fungal infections can be confused with nail psoriasis.
- Atopic dermatitis: More common in children, eczema represents a more conservative diagnosis than psoriasis.
- Lupus: Also of autoimmune origin, lupus usually presents other symptoms such as fever, fatigue and damage to the heart, lungs, liver and kidneys.
- Skin cancer: Squamous cell carcinoma develops on the surface of the skin that is exposed to the sun. It is distinguished by very firm and delimited nodules, sores or patches.
These are just a few examples of differential diagnoses, although there may be many others such as leishmaniasis, reactive arthritis, or pityriasis rosea.
Due to all this, it’s very important to consult a specialist, preferably a dermatologist, as soon as you observe changes on the surface of the skin. A misdiagnosis is counterproductive for the treatment and improvement of symptoms, and even more so if you proceed with self-medication.
Although the disease has no cure, a series of therapies and drugs can be applied that can improve the quality of life of patients. All of this, in principle, will combine to make a correct diagnosis of psoriasis to proceed with the best treatment option.
Psoriasis is an autoimmune disease that manifests itself through breakouts on the surface of the skin. It’s considered a chronic disorder that can go through periods of remission over the years. Only a professional can make a diagnosis of psoriasis, as it can be confused with other skin or infectious diseases.
Despite advances in research surrounding this condition, there’s no unified diagnosis for psoriasis. Due to this, the specialist has to resort to the recognition of a series of patterns, the review of the patient’s clinical history, and the consideration of the risk groups for the disease.
Although the symptoms of psoriasis may be very obvious to the naked eye, it’s actually a very difficult disorder for non-specialists to diagnose. For this reason, you should always go to an expert if you suspect that you’re suffering from it, and avoid premature self-medication at all costs.
Diagnosis of psoriasis by physical examination

Unlike other autoimmune disorders, psoriasis can’t be diagnosed through 100 percent effective blood tests or imaging studies. Its diagnosis varies depending on the type or variant of the disease, among which vulgaris, nail, guttate and pustular psoriasis stand out as the most frequent.
The method most used by dermatologists to diagnose psoriasis is through a physical exam. It’s very common for the specialist to use a dermatoscope, an instrument that has proven to be very useful for this task. Considering that between 80% and 90% of the disease occurs through the vulgaris variant, the following will need to be present:
- Plates delimited with silver scales.
- Red or pearly-colored skin surface.
- Inflammation and burning in the affected area.
- Desquamation in peripheral or central areas.
- Excoriation in the epidermis.
The dermatologist will carefully review these symptoms in the area indicated by the patient as well as in others such as the scalp, the folds, behind the ears and in the joints and extremities. They will also assess the thickness, color, and growth of the nails, a clear symptom of nail psoriasis.
Along with this physical examination, they will consider the patient’s family history. Psoriasis is known to have a high genetic predisposition, and so a history of the disease in parents or grandparents can help confirm it. A review of the patient’s medical history for skin lesions, infections, or immune disorders can also be used to support the diagnosis.
Finally, the specialist doctor will consider the risk factors for psoriasis and its comorbidities. For example, physical inactivity, heavy smoking, alcoholism, obesity, and suffering from heart conditions, diabetes, or metabolic syndrome increase the chances of developing it.
Diagnosis of psoriasis by laboratory tests
In most cases, the diagnosis of psoriasis is carried out through a physical evaluation, but, in certain contexts, it’s necessary to perform a biopsy of the skin surface. This procedure is rare and is used only when there are doubts about a possible differential diagnosis.
Evidence indicates that it is very useful in some variants, such as nail psoriasis. This can be easily mistaken for fungal infections, even by qualified professionals. In this way, a biopsy is a support tool to make a more accurate psoriasis diagnosis.
It’s performed through a minimally invasive puncture that removes a tissue sample which is then evaluated under a special microscope. While waiting for the results, the doctor may prescribe a preventive treatment to deal with the disease for the time being.
PASI classification in psoriasis
When making the diagnosis of psoriasis, the specialist will proceed to classify the disease according to its severity.
There are many rating scales. The three most used are the National Psoriasis Foundation Psoriasis Score (NPF-PS), the Physician’s Global Assessment (PGA) and the Psoriasis Area Severity Index (PASI). The latter is by far the most used for its practicality.
This scale divides the body into four sections: trunk, upper limbs, lower limbs and head, and the following values are taken into account:
- Percentage of affected skin: From 0% to 100% in degrees ranging from 1 to 6.
- Desquamation: On a scale from 0 to 4.
- Itching: On a scale from 0 to 4.
- Erythema: On a scale from 0 to 4.
- Induration: Determined on a scale of 0 to 4.
Finally, all the values are combined and extrapolated on a scale ranging from 0 (absence of disease) to 72 (maximum disease). The tests are usually repeated from time to time to evaluate the improvement of the condition and possible changes in treatment in case the current treatment isn’t working.
Differential diagnosis of psoriasis

One of the reasons why self-diagnosis of patients isn’t recommended is the possible differential causes of breakouts on the skin. There are at least a dozen diseases with symptoms that are very similar to those of psoriasis, and so the mediation of a specialist is irreplaceable.
The most common differential diagnoses of psoriasis are as follows:
- Saborrheic dermatitis: Very common differential diagnosis in psoriasis vulgaris, especially when the outbreaks are located on the scalp and its surroundings.
- Lichen simplex chronicus – Usually develops on the groin, extremities, neck, and genitals.
- Ringworm of the body: Very common in uncovered areas, it’s characterized by microvesicles on the edges. Diagnosed by culture and KOH (potassium hydroxide).
- Onychomycosis: Nail fungal infections can be confused with nail psoriasis.
- Atopic dermatitis: More common in children, eczema represents a more conservative diagnosis than psoriasis.
- Lupus: Also of autoimmune origin, lupus usually presents other symptoms such as fever, fatigue and damage to the heart, lungs, liver and kidneys.
- Skin cancer: Squamous cell carcinoma develops on the surface of the skin that is exposed to the sun. It is distinguished by very firm and delimited nodules, sores or patches.
These are just a few examples of differential diagnoses, although there may be many others such as leishmaniasis, reactive arthritis, or pityriasis rosea.
Due to all this, it’s very important to consult a specialist, preferably a dermatologist, as soon as you observe changes on the surface of the skin. A misdiagnosis is counterproductive for the treatment and improvement of symptoms, and even more so if you proceed with self-medication.
Although the disease has no cure, a series of therapies and drugs can be applied that can improve the quality of life of patients. All of this, in principle, will combine to make a correct diagnosis of psoriasis to proceed with the best treatment option.
- Cassinelli, M. F. V. Diagnóstico diferencial de la Psoriasis.
- Gottlieb, A. B., Chaudhari, U., Baker, D. G., Perate, M., & Dooley, L. T. The National Psoriasis Foundation Psoriasis Score (NPF-PS) system versus the Psoriasis Area Severity Index (PASI) and Physician’s Global Assessment (PGA): a comparison. Journal of drugs in dermatology: JDD. 2003; 2(3): 260-266.
- Grover, C., Reddy, B. S. N., & Uma Chaturvedi, K. Diagnosis of nail psoriasis: importance of biopsy and histopathology. British Journal of Dermatology. 2005; 153(6): 1153-1158.
- Johnson, M. A. N., & Armstrong, A. W. Clinical and histologic diagnostic guidelines for psoriasis: a critical review. Clinical reviews in allergy & immunology. 2013; 44(2): 166-172.
- Kim, W. B., Jerome, D., & Yeung, J. Diagnosis and management of psoriasis. Canadian Family Physician. 2017; 63(4): 278-285.
- Lallas, A., Kyrgidis, A., Tzellos, T. G., Apalla, Z., Karakyriou, E., Karatolias, A., … & Zalaudek, I. Accuracy of dermoscopic criteria for the diagnosis of psoriasis, dermatitis, lichen planus and pityriasis rosea. British Journal of Dermatology. 2012; 166(6): 1198-1205.
- Montalvo Alvarez, A. M., Blanco González, O., Capó de Paz, V., Fraga Nodarse, J., & Monzote Fidalgo, L. ¿Leishmaniasis o psoriasis? Diagnóstico diferencial. Revista Cubana de Medicina Tropical. 2014; 66(2): 305-311.
- Raychaudhuri, S. K., Maverakis, E., & Raychaudhuri, S. P. Diagnosis and classification of psoriasis. Autoimmunity reviews. 2014; 13(4-5): 490-495.
- Valdimarsson, H. The genetic basis of psoriasis. Clinics in dermatology. 2007; 25(6): 563-567.
Este texto se ofrece únicamente con propósitos informativos y no reemplaza la consulta con un profesional. Ante dudas, consulta a tu especialista.







